Case Report Open Access
Mucinous Appendiceal Adenocarcinoma Presenting as Sister Mary Joseph Nodule: Case Report and Brief Review of Literature
Amareshwar Podugu, Alicia Alvarez, Ronnie Pimentel and Andrew Ukleja*
Digestive Disease Institute, Cleveland Clinic Florida, Weston, Florida, USA
- *Corresponding Author:
- Dr. Andrew Ukleja, MD
Department of Gastroenterology
2950 Cleveland Clinic Blvd, Weston
Florida 33331, USA
Tel: 954659-5646
E-mail: UKLEJAA@ccf.org
Received date: August 14, 2015 Accepted date: Sepember 14, 2015 Published date: Sepember 21, 2015
Citation: Podugu A, Alvarez A, Pimentel R, Ukleja A (2015) Mucinous Appendiceal Adenocarcinoma Presenting as Sister Mary Joseph Nodule: Case Report and Brief Review of Literature . J Gastrointest Dig Syst 5:339. doi:10.4172/2161-069X.1000339
Copyright: © 2015 Podugu A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Sister Mary Joseph nodule is a rare form of umbilical metastasis. Often, this is the only initial presenting sign for an underlying internal malignancy and is usually associated with poor prognosis. Although the gastrointestinal tract is the most common primary site, the majority of these metastases are from gastric and colorectal sites. We report a case of Sister Mary Joseph nodule in a patient with no GI complaints. Further evaluation led to the diagnosis of primary mucinous adenocarcinoma of the appendix. Primary mucinous adenocarcinoma of the appendix is a very rare tumor type that can give rise to umbilical metastases. To the best of our knowledge, only 3 cases of adenocarcinoma of the appendix metastasizing to the umbilicus have been reported in the medical literature.
Keywords
Umbilicus; Metastasis; Sister Mary Joseph’s nodule; Adenocarcinoma; Vermiform Appendix; Mucinous neoplasm
Introduction
The frequency of cutaneous metastasis from internal malignancies ranges from 5-9% [1-4]. However, umbilical metastases from visceral malignancies described as Sister Mary Joseph nodule (SMJN) is rare and represents only 10% of all cutaneous metastases [3,5,6]. Its presence can signify recurrence of tumor or an extensive spread of the underlying cancer. Approximately 1-3% of abdominopelvic tumors likely metastasize to the umbilicus [4,5,7]. SMJN is well described with over 400 cases reported in medical literature as sign of internal malignancies. A substantial number of cases involve intra-abdominal malignancies from the gastrointestinal and female genital tract. It has been estimated that SMJN with unknown primary ranges between 15% and 30% [8-10]. A meta-analysis of reports of umbilical metastasis by Dubreuil et al and a case series of 77 patients with umbilical metastases revealed that women were more commonly affected than men [4,11] Isolated cases from other sites like gallbladder, liver, breast, lung, prostate, penis, peritoneum, lymphoma, bladder, kidney, endometrium, cervix, vagina, vulva, and fallopian tube and other organ systems have been reported. Irrespective of the primary disease, the presence of umbilical metastases is worrisome and is usually associated with poor prognosis. Although the gastrointestinal tract is the most common primary site, the majority of these metastases are from stomach and colorectal sites. Very few case reports demonstrated an association between appendiceal adenocarcinoma and SMJN. The first case report was described from Taiwan in 2008 [12]. 2 more cases of appendiceal neoplasm with low malignant potential and mucinous adenocarcinoma of the appendix were reported in series of 77 umbilical malignancies [11]. We report a case of SMJN resulting from primary mucinous adenocarcinoma of the appendix.
Case Report
A 68 year-old Female with h/o quiescent ulcerative colitis, hypertension and hyperparathyroidism seen in the gastroenterology department for the evaluation of umbilical discharge for five months. Patient developed small painless immobile lump underneath the umbilicus, which initially measured 1-2 cm associated with clear nonpurulent discharge followed by protruded umbilicus and 10 lb weight loss. Patient denied any abdominal pain, nausea, vomiting, fever and changes in bowel habits. She denied any menstrual bleeding or spotting’s. No significant family history for GI malignancy. On exam she was noted to have a non-tender soft umbilical mass of 6 cm with mucinous discharge and palpable subcutaneous mass in the supraumbilical area (Figure 1). Her findings were consistent with SMJN. CT scan abdomen/pelvis showed a right adenexal mass measuring 7.6 x 11.3 x 9.4 cm associated with multiple metastases to ometum, retroperitoneum, umbilicus and liver. CBC was with in normal limits. CEA, CA 19-9 and CA 125 were elevated. Umbilical biopsy was performed and was positive for malignant cells consistent with adenocarcinoma.
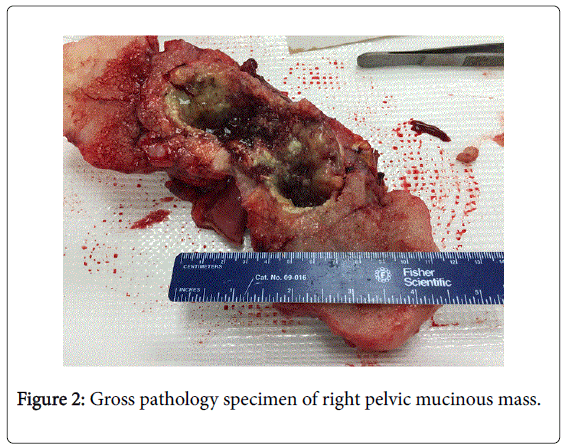
Subsequently underwent abdominal surgery, which revealed a 5 cm umbilical tumor eroding through the umbilicus, omentum partially replaced with multiple tumor nodules and a 12 x 8 x 7.5 cm right pelvic mucinous mass (Figure 2) involving and replacing the right tube, right ovary, distal appendix and a loop of ileum. Surgical pathology showed poorly differentiated mucinous adenocarcinoma arising in the appendix. Diagnosis of pT4bNn/aM1a metastatic mucinous adenocarcinoma of the appendix was established.
Discussion
Sister Mary Joseph’s Nodule (SMJN) refers to a nodule or mass that can be either seen or felt in the peri-umbilical region and usually corresponds to umbilical metastasis. Sister Mary Joseph (1856-1939), the nursing superintendent and surgical assistant of Dr. William Mayo at St Mary’s Hospital (now Mayo Clinic) in Rochester, Minnesota was the first one who illustrated an association between umbilical nodule and intra-abdominal malignancies [6]. The first case of umbilical metastasis was first described in 1864 by Storer even before the origin of the term SMJN [13]. However, it was only in 1949, Sir Hamilton Bailey coined the term ‘Sister Mary Joseph’s Nodule’ in his book ‘Demonstration of Physical Signs in Clinical Surgery’ to describe this entity [14,15]. SMJN constitutes 83-85% of all malignant umbilical tumors, being much more common than primary malignant umbilical tumors [5,7,11,16]. Among these the most prominent histological type is adenocarcinoma (75%) with other histological variants like squamous cell carcinoma, undifferentiated tumors, carcinoid, sarcoma, mesothelioma, melanoma, and lymphoma being extremely rare [17-20]. Rich lymphatic and vascular supply of umbilicus, along with its association with embryologic remnants makes it a potential site for metastasis of neoplastic cells [21-23]. In addition, direct extension from a contiguous tumor and direct implantation following laparoscopy may contribute to the spread of tumors to the umbilicus [24]. The clinical features of SMJN from different primary lesions cannot be visually distinguished. Its presentation can vary from painless firm irregular small nodule to sometimes painful ulcerated mass with exudate like pus, blood, mucinous or serous fluid. Sometimes it can present as a diffuse subcutaneous induration with indistinct borders. As in our case, often it could represent the initial presenting symptom/ sign for an underlying internal malignancy [4]. Benign conditions like endometriosis [25], hernia, myxoma, epithelial inclusion cysts [26], omphalithiasis [27] abscesses [4] can mimic SMJN.
Imaging modalities like ultrasonography (US), computed tomography (CT), magnetic resonance imaging (MRI), and positron emission tomography (PET) provide assistance to establish the diagnosis. Tissue diagnosis by biopsy, either excisional or fine needle aspiration (FNA), helps identifying the possible primary site [28-30]. Immunohistochemical marker studies and ultrastructural examination have been utilized in identifying origin of anaplastic tumors. In approximately 72% of the cases of unknown primary tumor, immunohistochemical analysis helped to determine the cellular origin [31]. In addition the use of electron microscopy and cytogenetic analysis enhances the diagnostic sensitivity and specificity. Establishing the diagnosis of SMJN is ominous indicating an advanced stage of cancer with a grave prognosis. Long term survival of patients is uncommon [4,6,32-34].
Berger in 1882, first described primary appendicular neoplasm [35]. Primary appendiceal cancer is rare accounting for 0.4-1.0% of all gastrointestinal tumors [36] Three histological variants of the primary appendicular adenocarcinoma have been illustrated, including mucinous adenocarcinoma, intestinal type (goblet and colonic) and signet ring cell cancers [37]. Patients with appendiceal malignancies generally present with the symptoms suggestive of acute appendicitis or as a palpable abdominal mass [38]. However, our patient lacked any symptoms and signs of acute appendicitis. Liu etal reported a case similar to our case of appendiceal carcinoma presenting with only initial sign of SMJN [12]. The sex distribution is usually equal [39]. Right hemicolectomy has been the standard of care, especially if the tumor is confined to the appendix. Several clinical studies have established better survival rate after the right hemicolectomy in comparison with appendectomy [40-44]. Overall 5-year survival is 44% for appendicular mucinous tumors, 52% and 20% for the colonic subtype and for the signet ring cell subtype, respectively [37,45]. When associated with intraperitoneal dissemination and accumulation of mucinous implants, the prognosis is similar to that of peritoneal carcinomatosis with 5-year survival being less than 10% [37].
Conclusion
Physicians must exercise caution while dealing with umbilical lesions that do not exactly fit to the diagnosis of hernia and meticulously evaluate for an underlying malignancy.
References
- Brownstein MH, Helwig EB (1973) Spread of tumors to the skin.Arch Dermatol 107: 80-86.
- Spencer PS, Helm TN (1987) Skin metastases in cancer patients.Cutis 39: 119-121.
- Lookingbill DP, Spangler N, Sexton FM (1990) Skin involvement as the presenting sign of internal carcinoma. A retrospective study of 7316 cancer patients.J Am AcadDermatol 22: 19-26.
- Dubreuil A, Dompmartin A, Barjot P, Louvet S, Leroy D (1998) Umbilical metastasis or Sister Mary Joseph's nodule.Int J Dermatol 37: 7-13.
- Steck WD, Helwig EB (1965) Tumors of The Umbilicus.Cancer 18: 907-915.
- Al-Mashat F, Sibiany AM (2010) Sister Mary Joseph's nodule of the umbilicus: is it always of gastric origin? A review of eight cases at different sites of origin.Indian J Cancer 47: 65-69.
- Barrow MV (1966) Metastatic tumors of the umbilicus.J Chronic Dis 19: 1113-1117.
- Falchi M, Cecchini G, Derchi LE (1999) [Umbilical metastasis as first sign of cecal carcinoma in a cirrhotic patient (Sister Mary Joseph nodule). Report of a case].Radiol Med 98: 94-96.
- Galvañ VG (1998) Sister Mary Joseph's nodule.Ann Intern Med 128: 410.
- Gabriele R, Borghese M, Conte M, Basso L (2004) Sister Mary Joseph's nodule as a first sign of cancer of the cecum: report of a case.Dis Colon Rectum 47: 115-117.
- Papalas JA, Selim MA (2011) Metastatic vs. primary malignant neoplasms affecting the umbilicus: clinicopathologic features of 77 tumors. Annals of diagnostic pathology 15: 237-242.
- Liu H, Yuan SS, Lin KJ, Huang CK, Hung CM, et al. (2008) Unusual Presentation of Appendiceal Adenocarcinoma: Report of a Case. Formosan Journal of Surgery 41:217-220.
- Storer HR (1864) Cases illustrative of obstetric disease. The Boston Medical and Surgical Journal 70:69-74.
- Bailey H (1949) Demonstrations of Physical Signs in clinical Surgery Williams and Wilkins. New York 227.
- Key JD, Shephard DA, Walters W (1976) Sister Mary Joseph's nodule and its relationship to diagnosis of carcinoma of the umbilicus.Minn Med 59: 561-566.
- Khan AJ, Cook B (1997) Metastatic carcinoma of umbilicus: "Sister Mary Joseph's nodule".Cutis 60: 297-298.
- Shetty MR (1990) Metastatic tumors of the umbilicus: a review 1830-1989.J SurgOncol 45: 212-215.
- Panaro F, Andorno E, Di Domenico S, Morelli N, Bottino G, et al. (2005) Sister Joseph's nodule in a liver transplant recipient: Case report and mini-review of literature.World J SurgOncol 3: 4.
- Tam C, Turner H, Hicks RJ, Seymour JF (2002) Diffuse large B-cell non-Hodgkin's lymphoma presenting as Sister Joseph's nodule.Leuk Lymphoma 43: 2055-2057.
- Bank H, Liberman SI (1971) Sistr Joseph's nodule and malignant ascites in multiple myeloma.N Engl J Med 284: 676-677.
- Powell FC, Cooper AJ, Massa MC, Goellner JR, Su WP (1984) Sister Mary Joseph's nodule: a clinical and histologic study.J Am AcadDermatol 10: 610-615.
- Goodheart RS, Cooke CT, Tan E, Matz LR (1986) Sister Mary Joseph's nodule.Med J Aust 145: 477-478.
- Majmudar B, Wiskind AK, Croft BN, Dudley AG (1991) The Sister (Mary) Joseph nodule: its significance in gynecology.GynecolOncol 40: 152-159.
- Yusuf M, Azhar R (2004) Umbilical metastasis from oesophageal squamous cell carcinoma: a case report. The Internet Journal of Gastroenterology.
- Albrecht LE, Tron V, Rivers JK (1995) Cutaneous endometriosis.Int J Dermatol 34: 261-262.
- López J, Rodil MA (1998) Fine needle aspiration cytology of an umbilical cyst mimicking Sister Mary Joseph's nodule.ActaCytol 42: 1069-1070.
- Amaro R, Goldstein JA, Cely CM, Rogers AI (1999) Pseudo Sister Mary Joseph's nodule.Am J Gastroenterol 94: 1949-1950.
- Gupta RK, Naran S, McHutchison AG, Lallu S, Fauck RJ (1994) Diagnosis of umbilical metastasis (Sister Mary Joseph's nodule) by fine-needle aspiration: an immunocytochemical study.DiagnCytopathol 10: 126-129.
- ScudelerD, Wakely PE Jr (2006) Fine needle aspiration biopsy of gastrointestinal stromal tumor presenting as an umbilical mass (Sister Mary Joseph's Nodule).Ann DiagnPathol 10: 100-103.
- Mallya MV, Mandrekar S, Nadkarni NS, Menezes S (1995) Sister Mary Joseph's nodule--diagnosis of umbilical metastases by fine needle aspiration.Indian J PatholMicrobiol 38: 95-98.
- Schneider V, Smyczek B (1990) Sister Mary Joseph's nodule. Diagnosis of umbilical metastases by fine needle aspiration.ActaCytol 34: 555-558.
- Touraud J, Lentz N, Dutronc Y, Mercier E, Sagot P, et al. (2000) [Umbilical cutaneous metastasis (or Sister Mary Joseph's nodule) disclosing an ovarian adenocarcinoma]. Gynecologie, obstetrique&fertilite 28:719-721.
- Gabriele R, Conte M, Egidi F, Borghese M (2005) Umbilical metastases: current viewpoint.World J SurgOncol 3: 13.
- Kurt S, Camuzcuoglu H, Camuzcuoglu A, Dicle N, Tinar S (2009) Umbilical metastasis of serous component as a first sign of mixed type epithelial ovarian cancer.Eur J GynaecolOncol 30: 455-457.
- Hananel N, Powsner E, Wolloch Y (1998) Adenocarcinoma of the appendix: an unusual disease.Eur J Surg 164: 859-862.
- Vanags A, Strumfa I, Abolins A, Brikuns A, Simtniece Z, et al. (2011) Primary Adenocarcinoma of the Appendix. ActaChirurgicaLatviensis 11:151-153.
- Pai RK, Longacre TA (2005) Appendiceal mucinous tumors and pseudomyxomaperitonei: histologic features, diagnostic problems, and proposed classification. Advances in anatomic pathology 12:291-311.
- Ito H, Osteen RT, Bleday R, Zinner MJ, Ashley SW, et al. (2004) Appendiceal adenocarcinoma: long-term outcomes after surgical therapy.Dis Colon Rectum 47: 474-480.
- Iwuagwu OC, Jameel JK, Drew PJ, Hartley JE, Monson JR (2005) Primary carcinoma of the appendix - Hull series.Dig Surg 22: 163-167.
- Nitecki SS, Wolff BG, Schlinkert R, Sarr MG (1994) The natural history of surgically treated primary adenocarcinoma of the appendix.Ann Surg 219: 51-57.
- Cortina R, McCormick J, Kolm P, Perry RR (1995) Management and prognosis of adenocarcinoma of the appendix.Dis Colon Rectum 38: 848-852.
- Cirocco WC (2005) Right hemicolectomy remains the treatment of choice for adenocarcinoma of the appendix.GastrointestEndosc 61: 791.
- Hesketh KT (1963) The management of primary adenocarcinoma of the vermiform appendix.Gut 4: 158-168.
- Hopkins GB, Tullis RH, Kristensen KA (1973) Primary adenocarcinoma of the vermiform appendix: report of seven cases and review of the literature.Dis Colon Rectum 16: 140-144.
- McCusker ME, Coté TR, Clegg LX, Sobin LH (2002) Primary malignant neoplasms of the appendix: a population-based study from the surveillance, epidemiology and end-results program, 1973-1998.Cancer 94: 3307-3312.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 17167
- [From(publication date):
October-2015 - Aug 23, 2025] - Breakdown by view type
- HTML page views : 12503
- PDF downloads : 4664