Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Case Report Open Access
Multi-Focal Endometriosis in a Young Woman with Adnexal Para-Mesonephric Cyst: Role of MRI in Surgical Planning
| Albarello F1*, Deriu G1, Zagatti Y1, Goletti S2 and Campioni P1 | |
| 1Department of Radiology, University of Ferrara, Ferrara, Italy | |
| 2Department of Radiology, CTO A Alesini Hospital, Rome, Italy | |
| Corresponding Author : | Albarello F Department of Radiology University of Ferrara, Ferrara, Italy Tel: +393928529110 E-mail: fabrizioalbarello@yahoo.it |
| Received: Septemebr 16, 2015; Accepted: October 08, 2015; Published: October 15, 2015 | |
| Citation: Albarello F, Deriu G, Zagatti Y, Goletti S, Campioni P (2015) Multi-Focal Endometriosis in a Young Woman with Adnexal Para-Mesonephric Cyst: Role of MRI in Surgical Planning. J Preg Child Health 2:202. doi:10.4172/2376-127X.1000202 | |
| Copyright: © 2015 Albarello F, et al.. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
We present a case of a young woman with several cystic lesions of different origin in both ovaries. The MRI played a crucial role for the pre-operative characterization of the lesions helping to define the possible malformative origin of one of those then confirmed by the laparoscopy as hydatid of Morgagni in a multifocal endometriosis patient. A discussion of the MR imaging findings is provided as follow.
| Keywords |
| Hydatid of morgagni; Magnetic resonace; Endometriosis; Pelvis; Ovarian cysts |
| Case Presentation |
| In September 2011, a 22-year-old woman went to the emergency room of our hospital referring abdominal pain; she was nullipara, with no history of weight or appetite change. She was afebrile, with a normal blood leukocyte count; her menarca was at 12 years. Trans-vaginal ultrasonography (TVUS) showed left ovarian increased in volume, with dysomogeneous structure, ectasic right tube (8 mm) and two disomogeneous right ovarian cysts, suspicious for endometriomas. |
| A nodule of about 1.5 cm was found in the recto-vaginal septum, which confirmed the palpatory finding of the gynecological examination. |
| The patient has been therefore submitted to pelvic MRI after the clinical and ultrasonographic suspect of endometriosis. |
| MRI of the pelvis was performed at 1.5 T (Signa General Electric, Milwaukee, USA), using a 16-channel pelvic phased array surface coil. |
| MRI analysis was performed with T1 and T2-weighted Spin Echo, Fast Spin Echo and Fast Recovery Fast Spin Echo sequences, with axial, coronal and sagittal planes, with and without fat saturation, without gadolinium injection; the patient was prepared with a water-based gel (ultrasonography gel) in the rectum. |
| MRI protocol for the suspicion of endometriosis includes axial T1-weighted SE, T2-weighted FSE, T1-weighted FSE fat-sat and T2- weighted FSE fat-sat sequences in the axial plane and T2-weighted FSE fat-sat sequences in the coronal plane. To complete the study, T2- weighted FSE fat-sat sequences were acquired in the sagittal plane. |
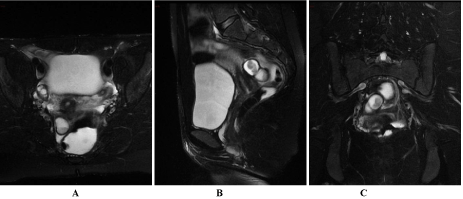
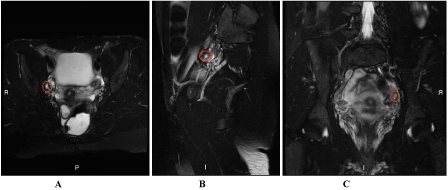
| MRI confirmed the presence of a bilobate, ovalar formation, on the right side of the recto-vaginal septum, hyper-intense on both T1 and T2-weighted images, with hypo-intense peripheral crest-wreath, compatible with endometriotic lesion (Figure 1); MRI also emphasize the presence of a cystic formation, with axial diameter of about 6 mm, tightly adherent to the terminal tract of the right fallopian tube and set to the ovary compatible with a non enodometriosic adnexal cyst probable due to malformative origin also campatible with hydatid of Morgagni (Figure 2). |
| Another cystic pluriconcamerate formation, of about 1.3 cm, was found also near the distal tract of the right tube, in posterior-medial position, compatible with another endometriotic lesion which caused structural distortion of the tube morphology, that appared ectasic (8 mm) and spread along an area of about 2 cm (Figure 3). |
| MRI finally confirmed, in comparison with the examinations previously performed, the bilateral ovarian functional cystic aspects and the normal uterine morphology. |
| The patient has been, therefore, submitted to laparoscopy that confirmed the aforesaid findings. |
| Discussion |
| Endometriosis is defined as the presence of functional endometrial glands and stroma outside the uterine cavity, which responds to hormonal stimulation with various degrees of cyclic hemorrhage. Deep endometriosis is the sub peritoneal invasion by endometriotic lesion that exceeds 5 mm in depth. It can affect the rectovaginal septum and uterosacral ligaments, as well as the vagina, the urinary and the alimentary tract [1,2]. The etio-pathogenesis of endometriosis is still unclear and probably multifactorial. Three theories of histopathogenesis have been proposed: |
| The metastatic theory of Sampson: this is the most widely accepted theory at present. According to this theory, endometriosis results from the metastatic implantation of endometrial tissue from retrograde menstruation that is due to endometrial tissue refluxes through the fallopian tube during menstruation and is then deposited on the peritoneal surface or pelvic organs. Other possible means of metastatic spread includes the transport of endometrial cells to distant sites from the pelvis via the bloodstream or lymphatic channels and iatrogenic spread during needle biopsy or surgery [3]. Favoring factors of this theory are both uterine mullerian anomalies (according to the classification of the American Fertility Society) and dismenorrhea, considered as a symptom of illness but also a risk factor: it would be related to vigorous uterine contractions, indeed, that would cause an obstacle to the normal menstrual flow with consequent retrograde flow. |
| The metaplastic theory of Meyer: it’s related to metaplastic differentiation of serous surface (coelomatic epithelium) or the remnants of mullerian tissue into endometrium-like tissue under the influence of estrogen. The strongest evidence for this theory is the demonstration of endometriosis in women who lack of functional ectopic endometrium (including those with Turner syndrome, gonadal dysgenesis, etc.), as well as in men. |
| The induction theory: it combines the first two proposed mechanism and suggests that shed endometrium releases substances that induce undifferentiated mesenchyme to form endometriotic tissue [4]. |
| The persistence of residual of para-mesonephric ducts or more rarely of the mesonephric ducts causes the formation of paraovarian or paratubal cysts (5-20% of the adnexal masses) [5]. Such formations result constituted by totipotent epithelium celomatic cells. Among these structures derived from mullerian remnants, we can enumerate the hydatid cyst of Morgagni [6,7], which is the most common benign non-inflammatory adnexal condition. Characteristically, it appears as a simple cyst (maximum axial diameter less than 2 cm) containing serous material, pedunculate, which typically locates next to the fimbria [8]. |
| The hydatid cyst of Morgagni is the most common benign noninflammatory tubaric condition and it usually appears as a simple cyst generally with an axial diameter smaller than 2 cm, containing serous material, pedunculate, typically located next to the fimbria. It originates from mullerian remnants [9] and it is usually found accidentally during laparoscopy or laparotomy, because it cannot be always visualized during transvaginal sonography. The presence of this formation, according to the data found in literature could constitute a substratum of coelomatic tissue that, under the estrogen stimulation, could differentiate, through metaplastic mechanism, in functioning endometrium-like tissue, tucked to the serous tubal surface (Meyer’s theory). This theory is supported by the presence of a voluminous endometriotic lesion in the recto-vaginal septum of the patient [10], which is interlinked with mullerian remnants right in this site that could become endometrium-like tissue under the estrogenic stimulation after the menarca [11]. |
| It’s important to keep in mind that in young patients with endometriosis, the concomitant presence of cystic ovarian lesions <1 cm has to raise the diagnostic doubt between further endometriotic lesion, functional cysts or hydatid cyst of Morgagni. The distortion of tubal morphology could be partly the result of the chronic inflammatory condition caused by the endometriosis, partly due to the possible alterations of the ciliary motility of the tubal epithelium induced by the paramesonephric cysts. Consequently, it results in tubal adherences that could contribute to tubal ectasia and also to the possible reflux of menstrual blood, which can be a concausa of the distal peritubal endometriotic implants as described in the Sampson’s theory. MRI allows discriminating between these lesions on the base of theirs different signal features [12]. |
| Both simple cysts and hydatid Morgagni cysts are hypointense on T1-weighted images and hyperintense on T2-weighted images; their different spatial position allows to discriminate them: the first ones are in the context of the ovary, instead the other ones appear as pedunculate appendixes of the fimbria and they can lean against the ovary and compress it, giving the characteristic “beak sign” [13] . |
| Endometriotic cysts, instead, have variable signal on MRI [14] depending on the time between menstrual bleeding and the execution of MRI exam because, as we know, the paramagnetic properties of hemoglobin catabolites change according to the degradation phase [15]. |
| Conclusion |
| MRI, due to higher spatial resolution, allowed us to identify endometriotic implants and incidental findings too small to be seen with USTV. Furthermore, an optimal tissue characterization was possible through the MRI in order to differentiate in the pre-operative phase the ovarian cystic formations. According to our preliminary experiences, with the limitations of a case report MRI showed to be more helpful than the US, in the pre-operative planning. MRI played a crucial role in distinguishing the multiple endometriotic lesions from the malformative cysts, giving important informations to the surgeon in the pre-operative planning. |
References
- Del Frate C, Girometti R, Pittino M, Del Frate G, Bazzocchi M, et al. (2006) Deep retroperitoneal pelvic endometriosis: MR imaging appearance with laparoscopic correlation. Radiographics 26: 1705-1718.
- Koninckx PR, Ussia A, Adamyan L, Wattiez A, Donnez J (2012) Deep endometriosis: definition, diagnosis, and treatment. FertilSteril 98: 564-571.
- Zhu L, Lang J, Wang H, Liu Z, Sun D, et al. (2009) Presentation and management of perineal endometriosis. Int J GynaecolObstet 105: 230-232.
- Coutinho A Jr, Bittencourt LK, Pires CE, Junqueira F, Lima CM, et al. (2011) MR imaging in deep pelvic endometriosis: a pictorial essay. Radiographics 31: 549-567.
- Savelli L (2006) Paraovarian/paratubal cysts: comparison of transvaginalsonographic and pathological findings to establish diagnostic criteria Ultrasound ObstetGynecol 28: 330-334.
- Cebesoy FB, Kutlar I, Dikensoy E, Yazicioglu C, Kalayci H (2010) Morgagnihydatids: a new factor in infertility? Arch GynecolObstet 281: 1015-1017.
- Kiseli M, Caglar GS, Cengiz SD, Karadag D, Yılmaz MB (2012) Clinical diagnosis and complications of paratubal cysts: review of the literature and report of uncommon presentations. Arch GynecolObstet 285: 1563-1569.
- Merlini L, Anooshiravani M, Vunda A, Borzani I, Napolitano M, et al. (2008) Noninflammatory fallopian tube pathology in children. PediatrRadiol 38: 1330-1337.
- Perlman S, Hertweck P, Fallat ME (2005) Paratubal and tubal abnormalities. SeminPediatrSurg 14: 124-134.
- Hoogeveen M, Dörr PJ, Puylaert JB (2003) Endometriosis of the rectovaginal septum: endovaginal US and MRI findings in two cases. Abdom Imaging 28: 897-901.
- Abrao MS, RM Neme, M Averbach (2003) Rectovaginal septum endometriosis: a disease with specific diagnosis and treatment. ArqGastroenterol 40: 192-197.
- Bazot M, Darai E, Hourani R, Thomassin I, Cortez A, et al. (2004) Deep pelvic endometriosis: MR imaging for diagnosis and prediction of extension of disease. Radiology 232: 379-389.
- Kishimoto K, Ito K, Awaya H, Matsunaga N, Outwater EK, et al. (2002) Paraovarian cyst: MR imaging features. Abdom Imaging 27: 685-689.
- Marcal L, Nothaft MA, Coelho F, Choi H (2010) Deep pelvic endometriosis: MR imaging. Abdom Imaging 35: 708-715.
- Kinkel K, Chapron C, Balleyguier C, Fritel X, Dubuisson JB, et al. (1999) Magnetic resonance imaging characteristics of deep endometriosis. Hum Reprod 14: 1080-1086.
Figures at a glance
 |
 |
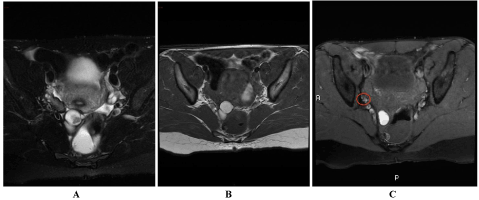 |
| Figure 1 | Figure 2 | Figure 3 |
Post your comment
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 11152
- [From(publication date):
December-2015 - Jul 30, 2025] - Breakdown by view type
- HTML page views : 10224
- PDF downloads : 928
