Our Experience with Internal Fixation of Unstable Charcot Foot with Intramedullary Nail and Plate
Received: 13-Apr-2018 / Accepted Date: 08-May-2018 / Published Date: 15-May-2018 DOI: 10.4172/2329-910X.1000268
Abstract
Background: Charcot neuroarthropathy is potentially a limb-threatening disease, most commonly associated with diabetes mellitus. Early diagnosis is a key factor in the management and plays a central role in the prevention of severe deformity. Conservative treatment remains the gold standard for most patients with acute stage of the Charcot neuroarthropathy. Surgery is usually reserved for patients with severe or unstable deformities that are refractory to conservative treatment. The aim of this article is to provide a brief overview of the Charcot neuroarthropathy and to present our experience in surgical treatment of patients with this condition.
Methods: 14 patients with Charcot neuroarthropathy and clinically unstable foot with a major dislocation in Lisfranc joint, stadius Eichenholz II, treated from January 2016 to September 2017 at University Medical Centre Ljubljana, were included in the study. Primary they were treated conservatively, until the acute edema, increased local temperature and redness were gone. All patients underwent an open reduction and internal fixation with plates or with intramedullary nails and plates.
Results: Successful recovery was obtained in all 14 cases, achieving stable foot. No postoperative complications were observed during the follow-ups.
Conclusion: Successful surgical treatment with internal fixation with plates or with intramedullary nail or plate, improved our patients quality of life. Based on our experience delayed open reduction and internal fixation of acute unstable Charcot foot is good and appropriate technique especially for patients without coexisting infections or macroangiopathy.
Keywords: Charcot foot; Intramedullary fixation; Internal fixation; Surgery
Introduction
Charcot neuroarthropathy (CN) is a progressive, non-infectious disorder in patients with peripheral neuropathy, affecting the bones, joints and soft tissues of the foot and ankle. It can result in fracture, severe instability and permanent deformity with subsequent plantar ulceration or even limb loss [1-3]. The most common etiology of Charcot neuroarthropathy is currently diabetes mellitus but it can be also associated with neurosyphilis, syringomyelia, leprosy, HIV, poliomyelitis, congenital neuropathy, toxic exposure, rheumatoid arthritis, multiple sclerosis, autonomic neuroarthropathy, traumatic injury and metabolic abnormalities [1,4,5]. The main underlying cause in diabetes is neuropathy, caused by chronic hyperglycemia and microvascular disease, leading to nerve injury via osmotic changes and ischemia [4]. The loss of protective sensation increases the likelihood of micro trauma, while autonomic neuropathy results in increased blood flow to the limb, causing tissue swelling and local osteoporosis [2]. Early diagnosis is a key factor in the management and plays a central role in the prevention of severe deformity [6]. Treatment depends on many factors and can be conservative, surgical or combined [1]. The most important surgical indications in chronic CN are recurring or non-healing ulcers, joint instability, pain, prominent exostosis and associated malalignment. Surgical interventions include exostectomy, Achilles tendon lengthening and arthrodesis [1]. Patients without any indication for surgery can be treated non-surgically with offloading of the involved foot, treating the bone disease and preventing further fractures and dislocations. Total contact casting (TCC) is believed to be the gold standard of the conservative treatment [1,7].
The aim of present analysis was to evaluate our experience with internal fixation of unstable Charcot foot and to compare the results with similar studies.
Materials and Methods
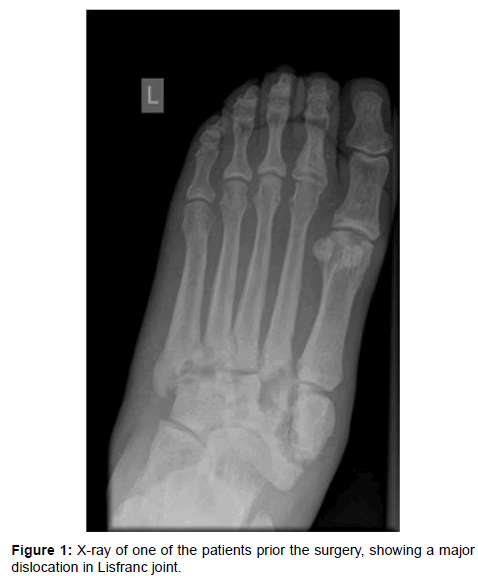
We reviewed 14 patients (11 male, 3 female) with CN with high degree of instability of the foot and dislocation in Lisfranc joint who were treated surgically from January 2016 to September 2017 at University Medical Centre Ljubljana (UMCL). The criteria for surgical treatment included deformed or unstable foot, sufficient peripheral circulation based on the result of angiography and patient’s willingness to cooperate in a rehabilitation process. We excluded patients with a peripheral arterial occlusive disease or insufficient peripheral circulation and patients with inflammatory ulcers or osteitis. In patients who met all inclusion criteria we primary decided to perform a surgery after transitional conservative treatment. The mean age of female patients was 38.00 ± 31.24 (range 28 to 56) years, the mean age of male patients was 55.91 ± 13.92 (range 45 to 61) years. At the time of diagnosis all patients had unstable foot with a major dislocation in Lisfranc joint, stadius Eichenholz II (Figure 1).
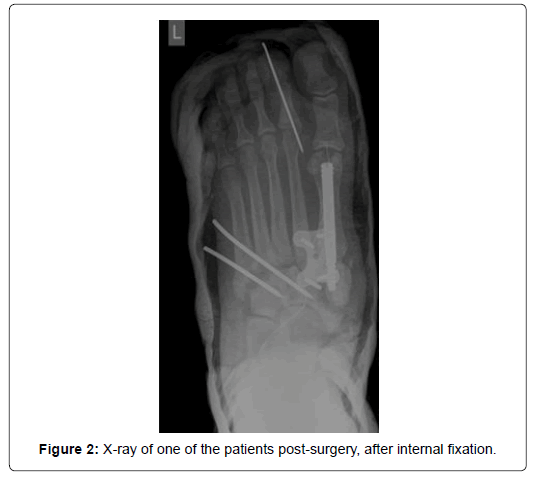
Instability was determined based on clinical and radiographic signs (X-ray, CT scanning). Two patients had concurrent dislocation of a metatarsophalangeal (MTP) joint including one female patient with dislocated first MTP joint and one male patient with dislocated second MTP joint. All patients were diabetics, two female patients (28 and 30 years old) had Type I diabetes and everyone else had Type II diabetes. None of the patients had any previous ulcers, Charcot episodes or other foot deformities. Because of the swelling in the acute stage of Charcot neuroarthropathy all patients were temporarily treated with TCC until the acute edema, increased local temperature and redness were gone. The mean duration of the conservative treatment prior surgery was 18.86 ± 5.81 (range 14 to 23) days. After the acute phase was clinically and radiographically over all patients underwent an open reduction and internal fixation. Type of fixation depended on Type of diabetes. In two patients with Type I diabetes fixation was made with plates and in patients with Type II diabetes fixation was made with an intramedullary nail and plates. During the surgery Esmarch bandage was used to minimize the bleeding. All patients received prophylactic antibiotic therapy during surgical procedure and anticoagulation therapy while immobilized. The wound dressing was changed every two to three days. All patients were dismissed from the hospital one week after the surgery. Postoperatively we applied a below-knee non-weight bearing cast for 8 weeks. During this period patients were walking with the help of the crutches. All patients had regular clinical check-ups 6 months after the surgery. In the first month they had a check-up every week and in the second and third month every two weeks. After 8 weeks non-weight bearing cast was replaced with a vacuum walker boot and after 10 weeks patients began with rehabilitation program in one of Slovenian thermal spas or health resorts. After 3 months patients started walking without the walker brace. Between fourth and sixth months after the surgery patients had check-ups once a month. During every check-up X-ray of the foot were taken to review patient’s condition and bone healing (Figure 2). After 6 months follow up period patients continued with regular diabetes check-ups in one of the general hospitals. Once a year they were still followed at our surgical clinic.
Results
All 14 cases with inclusion criteria healed successfully, without any intraoperative or postoperative complication. Stable foot was achieved in all patients. We did not observe any immediate postoperative complication. None of the patients had any evidence of superficial or deep infection. They were all able to replace a below-knee non-weight bearing cast with a vacuum stabilization boot after 8 weeks and began with full weight bearing walking without the walker brace after 3 months. All patients had their diabetes mellitus under control and none of them reported development of ulcers, as well as no deformation of the foot morphology was observed during any of the follow-ups. One male patient developed a gangrene of a big toe on the operated foot 25 months after the surgery because of the occurrence of peripheral arterial occlusive disease. His gangrene was surgically treated with an amputation of the big toe.
Discussion
It has been reported that currently there is not enough evidence supporting internal and/or external fixation for the treatment of Charcot neuroarthropathy [5,8-11]. Frykberg claims the choice should be made based on the quality of the bone, which is usually poor in CN. Therefore in his opinion external fixation provides better compression with fewer fixation failures. He prefers to utilize circular (Ilizarov) external fixation for most of charcot foot reconstructions [6]. Although its use clearly has advantages in fixation rigidity, external fixation is not without complications. Different studies showed a pin tract infection rate between 31% and 45% [8,12]. On the contrary we believe that delayed open reduction and internal fixation is a good solution for patients with unstable charcot foot. We prefer stabilization with circular external fixator just in case of coexisting ulcers, wounds or osteitis. Any kind of osteosynthesis is an option only in patients with sufficient peripheral circulation. In patients with badly damaged macrocirculation we use conservative treatment and smaller surgical interventions, including vascular surgery, if necessary.
The optimal timing of surgical stabilization is debated. Typically, surgical treatment was delayed until after completion of consolidation or Eichenholtz stage III [13]. In addition, some studies reported that surgery should be avoided during the active inflammation [1,3,7]. The demineralization, soft bone, and swelling in stage I may increase technical difficulty and surgical complications, such as infection and loss of fixation [13-15]. Also at our clinic we prefer delayed surgery after acute edema, increased local temperature and redness are gone. The main reason is the fact that diabetic patients are very susceptible to postoperative complications, especially in the acute phase of Charcot neuroarthropathy. On the other hand, several researches suggested early surgical intervention to prevent the deformity from progressing [1,16-19]. Sundararajan et al. tested the hypothesis that earlier intervention with stable internal fixation in patients with Eichenholtz stage I severe neuropathic arthropathy is better option than later intervention. However, they reported that after a follow-up period ranging from 1 to 7 years, the mean hindfoot scale scores, clinical evaluation category, and complication rates did not differ significantly among the patients in the three Eichenholtz stages [20].
None of our patients had any postoperative complications and none of them reported any ulceration after the surgery. One patient developed a gangrene of big toe because of the occurrence of peripheral arterial occlusive disease 25 months after the surgery. Also a study made by Simon et al. showed similar results. They operated on 14 patients with Eichenholtz stage I diabetic neuropathy and all arthrodesis procedures were successful without any immediate or long-term postoperative complications [16]. Comparable results were published in German study made on 22 patients with 26 affected feet treated primary surgically for Charcot neuroarthropathy. Researchers did not observe any recurrence of ulceration or manifestation of new ulcers but they reported other complications in nine patients, five of them had perioperative hematoma and four instability of the foot [3]. Also the analysis of Indian study [20] made on 33 patients reported healing of all 20 preoperative ulcers without recurrence but revealed some other complications. Twenty three patients had no complications, two had implant failure but achieved union, three had nonunion but the foot was salvaged, two had infection controlled and the foot salvaged, and three patients required foot amputation. The major complication in their study was a 15 % infection rate (5/33 patients).
Poor long-term glycemic control has been associated with an increased risk of surgical site infection. Peripheral neuropathy and a hemoglobin A1c concentration of >8 % have been independently associated with surgical site infection [21]. The fact that all of our patients had their diabetes mellitus under control probably contributed to none of them getting an infection.
One of the limitations of this study is that there was no control group with which to compare the results. We could not include the control group because we believe that all patients with fulfilled criteria for surgery should be primary treated surgically. Another limitation is a small and heterogeneous group of patients, which makes generalizations more difficult.
Conclusion
Although conservative treatment is believed to be a gold standard for Charcot neuroarthropathy, surgical treatment is essential when nonoperative treatment fails. It is reserved for recurring or non-healing ulcers, joint instability, pain, prominent exostosis and acute fractures or dislocations. Surgical interventions include exostectomy, Achilles tendon lengthening and arthrodesis. Arthrodesis can be performed with internal or external fixation. Also, additional osteotomies may be used. Therefore based on our experience delayed open reduction and internal fixation of acute unstable charcot foot is good and appropriate technique especially for patients without coexisting infections or macroangiopathy.
References
- Guven MF, Karabiber A, Kaynak G, Ogut T (2013) Conservative and surgical treatment of the chronic Charcot foot and ankle. Diabetic Foot Ankle 4: 21177.
- Sponer P, Kucera T, Brtkova J, Srot J (2013) The management of charcot midfoot deformities in diabetic patients. Acta Medica 56: 3-8.
- Mittlmeier T, Klaue K, Haar P, Beck M (2010) Should one consider primary surgical reconstruction in charcot arthropathy of the feet? Clin Orthop Relat Res 468: 1002-1011.
- Papanas N, Maltezos E (2013) Etiology, pathophysiology and classifications of the diabetic charcot foot. Diabetic Foot Ankle 4: 20872.
- Shamsi B, Hossain J, Mendez G (2012) Delayed diagnosis of charcot and successful utilization of internal and external fixation: A Case Report. Foot Ankle Online J 5: 1-8.
- Frykberg RG, Rogers LC (2018) The diabetic charcot foot: A primer on conservative and surgical management. J Diabetic Foot Complications 1: 19-25.
- Sommer TC, Lee TH (2001) Charcot Foot: The diagnostic dilemma. Am Fam Physician 64: 1591-1598.
- Hegewald KW, Wilder ML, Chappell TM, Hutchinson BL (2016) Combined internal and external fixation for diabetic charcot reconstruction: A retrospective case series. J Foot Ankle Surg 55: 619-627.
- Wukich DK, Sung W (2009) Charcot arthropathy of the foot and ankle: modern concepts and management review. J Diabetes Complications 23: 409-426.
- Hong CC, Jin Tan K, Lahiri A, Nather A (2015) Use of a definitive cement spacer for simultaneous bony and soft tissue reconstruction of mid and hindfoot diabetic neuroarthropathy: A case report. J Foot Ankle Surg 54: 120-125.
- Nasser EM, LaPorta GA, Trott K (2015) Medial column arthrodesis using an anatomic distal fibular locking plate. J Foot Ankle Surg 54: 671-676.
- Rogers LC, Frykberg RG, Armstrong DG, Boulton AJ, Edmonds M et al. (2011) The charcot foot in diabetes. Diabetes Care 34: 2123-2129.
- Johnson JE (1999) Operative treatment of neuropathic arthropathy of the foot and ankle. Instr Course Lect. 48: 269-267.
- Scott RT, DeCarbo WT, Hyer CF (2015) Osteotomies for the management of charcot neuroarthropathy of the foot and ankle. Clin Podiatr Med Surg 32: 406-418.
- Trepman E, Nihal A, Pinzur MS (2005) Current topics review: Charcot neuroarthropathy of the foot and ankle. Foot Ankle Int 26: 26-46.
- Simon SR, Tejwani SG, Wilson DL, Santner TJ, Denniston NL (2000) Arthrodesis as an early alternative to nonoperative management of charcot arthropathy of the diabetic foot. J Bone Joint Surg Am 82: 939-950.
- Bono JV, Roger DJ, Jacobs RL (1993) Surgical arthrodesis of the neuropathic foot: A salvage procedure. Clin Orthop Relat Res 296: 14-20.
- Schon LC, Easley ME, Seinfeld SB (1998) Charcot neuroarthropathy of the foot and ankle. Clin Orthop 349: 116-131.
- Caravaggi CM, Sganzaroli AB, Galenda P, Balaudo M, Gherardi P, et al. (2012) Long-term follow up of tibiocalcaneal arthrodesis in diabetic patients with early chronic Charcot osteoarthropathy. J Foot Ankle Surg 51: 408-411.
- Sundararajan SR, Srikanth KP, Nagaraja HS, Rajasekaran S (2017) Effectiveness of hindfoot arthrodesis by stable internal fixation in various eichenholtz stages of neuropathic ankle arthropathy. J Foot Ankle Surg 56: 282-286.
- Wukich DK, Crim BE, Frykberg RG, Rosario BL (2014) Neuropathy and poorly controlled diabetes increase the rate of surgical site infection after foot and ankle surgery. J Bone Joint Surg Am 96: 832-839.
Citation: Frangez I, Klar H, Nizic-Kos T (2018) Our Experience with Internal Fixation of Unstable Charcot Foot with Intramedullary Nail and Plate. Clin Res Foot Ankle 6: 268. DOI: 10.4172/2329-910X.1000268
Copyright: © 2018 Frangez I, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 5390
- [From(publication date): 0-2018 - Dec 08, 2025]
- Breakdown by view type
- HTML page views: 4494
- PDF downloads: 896