Research Article Open Access
Patient Characteristics and Clinical Features of Acute Hepatitis E Infection in the South of the Netherlands
Moniek van Heijst, Assi Cabbolet*, Dennis van der Lee, Robbert Eichhorn, Ulrike de Wit and Robert Laheij
Department of Gastroenterology and Hepatology, Elisabeth-TweeSteden Hospital, Netherlands
- *Corresponding Author:
- Assi Cabbolet
Department of Gastroenterology and Hepatology
Elisabeth-TweeSteden Hospital, Hilvarenbeekseweg 60
Tilburg, 5022 GC, Netherlands
Tel: +31 653453889
E-mail: mailto:a.cabbolet@elisabeth.nl
Received date: March 8, 2016; Accepted date: June 15, 2016; Published date: June 22, 2016
Citation: van Heijst M, Cabbolet A, van der Lee D, Eichhorn R, de Wit U, et al. (2016) Patient Characteristics and Clinical Features of Acute Hepatitis E Infection in the South of the Netherlands. J Gastrointest Dig Syst 6:440. doi:10.4172/2161-069X.1000440
Copyright: © 2016 van Heijst M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License; which permits unrestricted use; distribution; and reproduction in any medium; provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: Evidence suggests that the incidence of hepatitis E infection increases in the developed world, and that the infection is not always travel related. The details of acute infections in developed countries have not yet been fully elucidated. Objectives: The aim of this study was to evaluate clinical features of acute viral hepatitis E infections in the developed world. Study design: All patients with a positive result on hepatitis E serology testing in the previous 5 years were evaluated. Retrospectively, the files of patients with an acute infection were analyzed. Results: Overall, 332 patients were tested. In 34 patients there was an acute infection. None of the patients had travelled to a developing country. Three patients were asymptomatic. In the other patients, main symptoms were malaise, fatigue and nausea and/or vomiting. Jaundice was seen in 8 patients. Liver tests were increased in almost all patients, but ranges varied considerably. The infection was self-limiting in all cases; normalization of liver tests occurred after two months. Conclusions: Clinical features of acute hepatitis E infection are nonspecific and cannot be recognized at presentation. In patients with acute onset of malaise and elevation of liver tests, hepatitis E should be considered.
Keywords
Acute infection; Clinical characteristics; Developed country; Hepatitis E; Netherlands
Background
Hepatitis E virus is a major cause of non-A, non-B hepatitis in many developing countries in Africa and Asia. It is endemic and typically causes explosive outbreaks of acute hepatitis. In these countries, hepatitis E infection is associated with poor sanitation due to faecal contamination of the water supply. Symptoms are generally mild, but pregnant women can suffer significant morbidity and mortality [1-3].
In developed and non-endemic countries, occurrence of hepatitis E infection has been associated with travellers returning from endemic countries [1]. During the past decade, sporadic cases of hepatitis E infection have been reported in many industrialized countries, in patients with no travel history [4-13]. The number of these autochthonous cases has increased dramatically, and evidence for animal reservoirs and zoonotic transmission has been revealed. Most episodes of zoonotic transmission are foodborne and have been linked to ingestion of raw or undercooked meat of wild and domestic animals [1,14-16].
In The Netherlands, hepatitis E RNA has been detected in more than 50% of the pig farms, and hepatitis E-specific antibodies were detected in approximately 70% of the slaughter pigs [14]. In 2013, The Netherlands counted over 12 million pigs [17]. This indicates the amount of people that could be at risk of developing hepatitis E infection, and emphasizes the need for more research in this area.
In general, hepatitis E virus causes a self-limiting infection. However, recent observations indicate that hepatitis E infection can become chronic in transplant and immunocompromised patients. This increases the complexity of the disease and, especially in these individuals, certainly makes it an emerging and significant clinical problem [1].
Most research, especially on clinical features, has been performed in the endemic areas [18,19]. The detailed clinical characteristics of acute infections in developed countries have not yet been fully elucidated.
Increasing numbers of reported sporadic cases of hepatitis E in these areas, as noted above, call for the need to identify the infection at presentation.
Objectives
The aim of this study was to evaluate clinical characteristics of acute viral hepatitis E in the south of the Netherlands, and establish whether hepatitis E can be recognised at primary presentation.
Study Design
Epidemiology
Retrospectively, we identified all patients tested for hepatitis E infection in the two general hospitals in Tilburg, The Netherlands. These two hospitals serve a population of approximately 300,000 people. Positive results on serology testing or PCR (polymerase chain reaction) for hepatitis E of the previous 5 years, January 2009 to August 2014, were retrieved. After identifying patients with an acute infection, the patient files were evaluated retrospectively. We collected data about the patient’s characteristics and clinical features, in particular presenting symptoms, physical examination, laboratory findings and abdominal ultrasounds results. This data was entered in an electronic database for analysis.
Laboratory studies
Serology tests were performed using enzyme-linked immunosorbent assay (ELISA) to identify anti-hepatitis E virusimmunoglobulin M (IgM) and immunoglobulin G (IgG), and PCR to detect serum hepatitis E virus ribonucleic acid (RNA). Patients with a positive result on either IgM antibodies or RNA, were considered to have had an acute infection, and were included into the study. In almost all patients, other viral causes of hepatitis were excluded: serologic tests were conducted for hepatitis A virus, hepatitis B virus, hepatitis C virus, Epstein-Bar virus and cytomegalovirus.
Statistics
For statistical analysis the electronic database organized in the Statistical Package for Social Science (SPSS) for Windows (version 19) was used. The results are presented as absolute numbers, mean, range of values and percentage.
Results
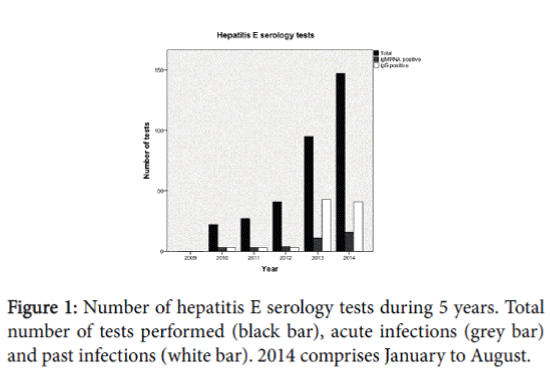
A total of 332 patients were tested for hepatitis E infection in the previous 5 year. In the past five years, serology tests were increasingly performed (Figure 1). In 34 out of the 332 patients (10.2%) there was an acute infection.
The mean age of the patients with an acute infection was 52 years (range 20-79 years); 68% were males. There was no clustering of infections in certain areas. Patients with an acute infection were living in small but also large towns.
No patients reported to have travelled to endemic countries prior to the period of hepatitis E infection. Apart from one patient who received chemotherapy during treatment of breast cancer, all patients were immunocompetent. Three patients were asymptomatic and tested for a hepatitis infection because of pathologic blood tests. Main symptoms were malaise, fatigue and nausea and/or vomiting. Jaundice was the least frequent symptom (Table 1). Two patients presented with decompensation of liver cirrhosis (aetiology: alcoholic and chronic viral hepatitis B) caused by acute hepatitis E infection.
| Symptom | Number of patients | Frequency (%) |
|---|---|---|
| Fatigue/malaise | 26 | 77 |
| Nausea/vomiting | 19 | 56 |
| Reduced appetite | 16 | 47 |
| Myalgia/arthralgia | 14 | 41 |
| Abdominal pain | 14 | 41 |
| Fever | 9 | 27 |
| Jaundice | 8 | 24 |
Table 1: Frequency of reported symptoms in acute hepatitis E at presentation.
Abnormalities in physical examination were seen in 15 patients: 8 patients (24%) had tenderness of the (upper) abdomen, 4 patients (12%) had an objectified fever, and 8 patients (24%) were icteric. An increase of alanine aminotransferase was seen in almost all patients (97%), gamma glutamyltranspeptidase and alkaline phosphatase were raised in 32 and 28 patients (94% and 82%), respectively; ranges varied considerably (Table 2). Total bilirubin was raised in twenty-one patients (62%), and also varied strongly. The inflammatory parameters were predominantly normal. Twenty-nine patients (85%) underwent hepatobiliary ultrasound or CT (computed tomography) imaging. Hepatic steatosis was seen in only 10 patients (29%), which was preexisting in two patients.
| Parameter | Mean | Range | Normal value |
|---|---|---|---|
| Total bilirubin | 47 | 4-168 | 0-17 µmol L-1 |
| ALP | 234 | 40-627 | 43-115 U L-1 |
| GGTP | 333 | 21-1390 | 0 -55 U L-1 |
| ALT | 1370 | 42 – 6226 | 0-45 U L-1 |
| C-reactive protein | 19 | 0-96 | 0-10 mg L-1 |
| Leukocytes | 7.3 | 3.2-14.4 | 4.0-10.0 10E9 L-1 |
Table 2: Values of laboratory parameters in acute hepatitis E at presentation. ALP: Alkaline Phosphatase, GGTP: Gamma Glutamyltranspeptidase, ALT: Alanine Aminotransferase.
In general, clinical course of the disease was mild to moderate. Half of the patients required hospital admission. The mean length of hospital stay was 6 days (range 1-13 days). No patients developed hepatic encephalopathy, portal hypertension or hepatorenal syndrome. Viral hepatitis E infection was self-limiting in almost all cases; there was no follow up in three patients. The mean time of normalization of liver biochemical and function tests was two months (range 1-5 months). The overall mortality rate was 0%.
Discussion
The present study describes the clinical aspects of acute hepatitis E infection in a developed country, the Netherlands. We found that acute hepatitis E infection in the south of the Netherlands is still a rare infection. It presents as a self-limiting, mild infection with general symptoms. Most patients experienced fatigue and half had nausea or vomiting. Jaundice was only seen in a few patients. Physical examination was normal in more than half of the patients. Liver enzymes and bilirubin vary considerably between patients.
Concerning social-demographic data of our patients, we found that males were more commonly affected than females. Mean age of presentation was 52 years, with a wide range. Similar investigations regarding to case study with acute hepatitis E infection from other European countries also revealed that the infection rate among the middle-aged male population was significantly higher [7,8,10,20]. Patients in our study presented mostly with fatigue, malaise, nausea and vomiting, which are non-specific symptoms, and occur commonly with other forms of acute hepatitis. Other comparable studies report reduced appetite and jaundice as most commonly presenting symptoms [7,10,20]. This shows that symptoms are non-specific, and can vary in populations.
None of the patients in this study report to have travelled to an endemic country. This emphasizes the presence of an autochthonous hepatitis E virus in the Netherlands. The misconception that hepatitis E only affects travelers into endemic areas could generally have resulted in neglecting diagnosis of hepatitis E in a former period. The more recent increasing awareness of indigenous infection has led to an increasing number of cases diagnosed. There is likely to be an even larger group of patients with either asymptomatic or milder selflimiting hepatitis E infection, who do not present for medical attention, as suggested by the high seroprevalence rates reported in Europe and the United States Course of acute hepatitis E infection was self-limiting in all patients, as reported in previous research [1,21]. Chronic hepatitis E infection has only been reported among immunosuppressed patients. Especially in solid organ transplant patient, but also in patients with HIV or haematological disease who received chemotherapy and/or stem cell transplantation [21,22].
A major limitation of our study is its retrospective design. Whether patients had travelled to endemic countries was not specifically mentioned in all patient files. In some patients, laboratory tests were not complete. Nevertheless, we do not believe that this had an influence on the results and overall clinical picture [23-29].
Secondly, the study has a small sample size. This can be explained by the previous unawareness of hepatitis E infection in developed countries, and non-specific symptoms that not always result in seeking medical attention [20,30].
Despite the limitations, this study is one of the first on clinical characteristics of non-traveller acute hepatitis E infection performed in the Netherlands. Previous research involved only few sporadic cases [5,31] or immunocompromised patients [21]. Understanding the clinical presentation of acute hepatitis E infection is important for the recognition of the disease. In immunocompetent patients, the detection could expand our understanding about the route of transmission and the relation with the zoonotic origin. In addition, it could be the cause of previously unresolved hepatitis. Therefore, besides creating an increasing awareness for non-travel associated hepatitis E among clinicians and medical microbiologists, diagnostics should be routinely incorporated into standard patients care. Moreover, in patients with acute on chronic liver failure, hepatitis E diagnostics should be implemented in the work-up.
In conclusion, this study confirms the existence of non-travel related hepatitis E infection in developed countries. Unfortunately, the identification of patients with an acute hepatitis E infection is difficult, as clinical features are non-specific. In patients presenting with acute onset of malaise and elevation of liver tests, and in patients with acute on chronic liver failure, hepatitis E should be considered and serological testing or PCR should be conducted.
References
- Mirazo S, Ramos N, Mainardi V, Gerona S, Arbiza J (2014) Transmission, diagnosis, and management of hepatitis E: an update. See comment in PubMed Commons below Hepat Med 6: 45-59.
- Banait VS, Sandur V, Parikh F, Murugesh M, Ranka P, et al. (2007) Outcome of acute liver failure due to acute hepatitis E in pregnant women. See comment in PubMed Commons below Indian J Gastroenterol 26: 6-10.
- Pelosi E, Clarke I (2008) Hepatitis E: a complex and global disease. See comment in PubMed Commons below Emerg Health Threats J 1: e8.
- Preiss JC, Plentz A, Engelmann E (2006) Autochthonous hepatitis E virus infection in Germany with sequence similarities to other European isolates. Infection 34:173-175.
- Widdowson MA, Jaspers WJ, van der Poel WH, Verschoor F, de Roda Husman AM, et al. (2003) Cluster of cases of acute hepatitis associated with hepatitis E virus infection acquired in the Netherlands. See comment in PubMed Commons below Clin Infect Dis 36: 29-33.
- Worm HC, Wurzer H, Frösner G (1998) Sporadic hepatitis E in Austria. See comment in PubMed Commons below N Engl J Med 339: 1554-1555.
- Mansuy JM, Peron JM, Abravanel F, Poirson H, Dubois M, et al. (2004) Hepatitis E in the south west of France in individuals who have never visited an endemic area. See comment in PubMed Commons below J Med Virol 74: 419-424.
- Ijaz S, Arnold E, Banks M (2005) Non-travel-associated hepatitis E in England and Wales: demographic, clinical, and molecular epidemiological characteristics. J Infect Dis 192: 1166-1172.
- Amon JJ, Drobeniuc J, Bower WA, Magaña JC, Escobedo MA, et al. (2006) Locally acquired hepatitis E virus infection, El Paso, Texas. See comment in PubMed Commons below J Med Virol 78: 741-746.
- Dalton HR, Thurairajah PH, Fellows HJ, Hussaini HS, Mitchell J, et al. (2007) Autochthonous hepatitis E in southwest England. See comment in PubMed Commons below J Viral Hepat 14: 304-309.
- Buti M, Clemente-Casares P, Jardi R, Formiga-Cruz M, Schaper M, et al. (2004) Sporadic cases of acute autochthonous hepatitis E in Spain. See comment in PubMed Commons below J Hepatol 41: 126-131.
- Tsang TH, Denison EK, Williams HV, Venczel LV, Ginsberg MM, et al. (2000) Acute hepatitis E infection acquired in California. See comment in PubMed Commons below Clin Infect Dis 30: 618-619.
- Chapman BA, Burt MJ, Wilkinson ID, Schousboe MI (1993) Community acquired viral hepatitis in New Zealand: a case of sporadic hepatitis E virus infection. See comment in PubMed Commons below Aust N Z J Med 23: 722-723.
- Rutjes SA, Bouwknegt M, van der Giessen JW, de Roda Husman AM, Reusken CB (2014) Seroprevalence of hepatitis E virus in pigs from different farming systems in The Netherlands. See comment in PubMed Commons below J Food Prot 77: 640-642.
- Christensen PB, Engle RE, Hjort C, Homburg KM, Vach W, et al. (2008) Time trend of the prevalence of hepatitis E antibodies among farmers and blood donors: a potential zoonosis in Denmark. See comment in PubMed Commons below Clin Infect Dis 47: 1026-1031.
- Yugo DM, Meng XJ (2013) Hepatitis E virus: foodborne, waterborne and zoonotic transmission. See comment in PubMed Commons below Int J Environ Res Public Health 10: 4507-4533.
- Centraal Bureau voor de Statistiek, Den Haag/Heerlen.
- Goumba AI, Konamna X, Komas NP (2011) Clinical and epidemiological aspects of a hepatitis E outbreak in Bangui, Central African Republic. See comment in PubMed Commons below BMC Infect Dis 11: 93.
- Aggarwal R, Krawczynski K (2000) Hepatitis E: an overview and recent advances in clinical and laboratory research. See comment in PubMed Commons below J Gastroenterol Hepatol 15: 9-20.
- Terzic D, Dupanovic B, Mugosa B, Draskovic N, Svirtlih N (2009) Acute hepatitis E in Montenegro: epidemiology, clinical and laboratory features. See comment in PubMed Commons below Ann Hepatol 8: 203-206.
- Riezebos-Brilman A, Verschuuren EA, van Son WJ, van Imhoff GW, Brügemann J, et al. (2013) The clinical course of hepatitis E virus infection in patients of a tertiary Dutch hospital over a 5-year period. See comment in PubMed Commons below J Clin Virol 58: 509-514.
- Kamar N, Izopet J, Rostaing L (2013) Hepatitis E virus infection. See comment in PubMed Commons below Curr Opin Gastroenterol 29: 271-278.
- Hogema BM, Molier M, Slot E, Zaaijer HL (2014) Past and present of hepatitis E in the Netherlands. See comment in PubMed Commons below Transfusion 54: 3092-3096.
- Dalton HR, Stableforth W, Thurairajah P (2008) Autochthonous hepatitis E in Southwest England: natural history, complications and seasonal variation, and hepatitis E virus IgG seroprevalence in blood donors, the elderly and patients with chronic liver disease. Eur J Gastroenterol Hepatol 20: 784-790.
- Mansuy JM, Legrand-Abravanel F, Calot JP, Peron JM, Alric L, et al. (2008) High prevalence of anti-hepatitis E virus antibodies in blood donors from South West France. See comment in PubMed Commons below J Med Virol 80: 289-293.
- Meng XJ, Wiseman B, Elvinger F, Guenette DK, Toth TE, et al. (2002) Prevalence of antibodies to hepatitis E virus in veterinarians working with swine and in normal blood donors in the United States and other countries. See comment in PubMed Commons below J Clin Microbiol 40: 117-122.
- Bouwknegt M, Engel B, Herremans MM (2008) Bayesian estimation of hepatitis E virus seroprevalence for populations with different exposure levels to swine in the Netherlands. Epidemiol Infect 136: 567-576
- Kaufmann A, Kenfak-Foguena A, André C, Canellini G, Bürgisser P, et al. (2011) Hepatitis E virus seroprevalence among blood donors in southwest Switzerland. See comment in PubMed Commons below PLoS One 6: e21150.
- Slot E, Hogema BM, Riezebos-Brilman A, Kok TM, Molier M, et al. (2013) Silent hepatitis E virus infection in Dutch blood donors, 2011 to 2012. See comment in PubMed Commons below Euro Surveill 18.
- Mansuy JM, Abravanel F, Miedouge M, Mengelle C, Merviel C, et al. (2009) Acute hepatitis E in south-west France over a 5-year period. See comment in PubMed Commons below J Clin Virol 44: 74-77.
- Melenhorst WB, Gu YL, Jaspers WJ, Verhage AH (2007) Locally acquired hepatitis E in the Netherlands: associated with the consumption of raw pig meat? See comment in PubMed Commons below Scand J Infect Dis 39: 454-456.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 11392
- [From(publication date):
June-2016 - Sep 03, 2025] - Breakdown by view type
- HTML page views : 10482
- PDF downloads : 910