Case Report Open Access
Physical Therapy Following a Hip Resurfacing Procedure
| Steve Karas1* and Keelan Enseki2,3 | |
| 1Assistant Professor, Chatham University Physical Therapy, Pittsburgh, PA, USA | |
| 2Orthopedic Physical Therapy Residency Program Director, Centers for Rehab Services/University of Pittsburgh Medical Center: Center for Sports Medicine, USA | |
| 3Adjunct Instructor, University of Pittsburgh, USA | |
| Corresponding Author : | Steve Karas Chatham University Woodland Road Pittsburgh PA 15232, USA E-mail: skaras@chatham.edu |
| Received May 16, 2013; Accepted June 12, 2013; Published June 14, 2013 | |
| Citation: Karas S, Enseki K (2013) Physical Therapy Following a Hip Resurfacing Procedure. J Nov Physiother 3:157. doi:10.4172/2165-7025.1000157 | |
| Copyright: © 2013 Karas S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Background and purpose: Hip resurfacing has emerged as an option for relatively younger, active individuals with end stage hip osteoarthritis. Rehabilitation protocols for these individuals have not been well disseminated in the literature. This case report describes the interventions for anactive individual following a hip resurfacing procedure.
Methods/Case description: The patient was a 44-year-old male referred to physical therapy following a hip resurfacing procedure. He was experiencing progressive hip pain and functional limitations over a ten year period prior to surgery.
Findings/Interventions: The patient received a course of home physical therapy. Gait training, passive range of motion (PROM), active range-of-motion (PROM) and lower extremity strengthening were initiated. One month after surgery, outpatient rehabilitation was initiated and progressed to include hip joint mobilization, weight-bearing strength, balance exercises and a functional activity progression.
Clinical relevance/Outcomes: Eleven months after surgery the patient reported no pain and returned to full activity, including playing tennis twice weekly, jogging up to 40 minutes, and coaching lacrosse. Slight AROM limitations remained.
Discussion/Conclusion: This case demonstrates the rehabilitation of a patient undergoing a hip resurfacing procedure. Techniques not commonly used after traditional hip arthroplasty are described, including aggressive range of motion, and joint mobilization.
| Keywords |
| Birmingham hip; Osteoarthritis; Rehabilitation |
| Introduction |
| Traditionally, the surgical treatment of choice for advanced hip osteoarthritis (OA) is total hip arthroplasty (THA). However, relatively younger patients with hip OA who attempt to participate in higher level sporting activity after THA face the possibility of implant failure, joint-bearing surface wear, implant loosening, dislocation, and instability [1,2]. Despite the expectations of the minimal incision surgical technique for THA, younger patients seeking to return to a high level of activity historically have been presented with limited choices [2,3]. In 2006 the Food and Drug Administration (FDA) approved the Birmingham Hip Resurfacing (BHR) System for use in the United States, ten years after the system was developed in the United Kingdom and implanted in nearly 60,000 patients. (According to a letter from The Food and Drug Administration in May, 2006) This device has been used extensively in Europe to allow for return to sporting activities in younger patients with hip OA and while potentially avoiding the negative complications associated with traditional THA procedures. |
| Outcomes data for individuals who undergo hip resurfacing (HR) procedures is limited. In one study of 384 patients under the age of 55, 87%were able to return to leisure time sporting activity in an eight year follow up after HR when the rehabilitation progression was “carefully planned in a graded manner” [4]. Favorable results were also noted in patients’ postoperative responses showing they were able to increase sporting function, activity, intensity and frequency [5]. While the short term results appear favorable to allow return to sport after HR, there is no evidence that patients return to normal ADL’s at a faster rate than patients undergoing traditional THA procedures [6] and long term results have not yet appeared in the literature [7]. |
| Specific rehabilitation guidelines have not been clearly identified in the physical therapy literature. However, there has been research suggesting that postoperative HR rehabilitation that “failed to meet the different demands” of a younger population may adversely affect HR results [8]. One case study has been published detailing objective improvements in PROM and function after rehabilitation which included joint mobilization techniques [9]. |
| Surgical options for young individuals with debilitating hip OA may include total hip arthroplasty, hip resurfacing, and in rare cases arthroscopic hip techniques. The choices are reviewed in table 1. Authors have advised against THA for patients under 30,45 or 50 years old respectively [8-10]. Younger patients who choose THA procedures may have to modify their high level of activity or risk premature failure of their hip components. Often, THA patients are unable to improve on their preoperative activity level [11,12]. |
| It is generally accepted that there are several theoretical advantages to HR including greater bone preservation, higher post operative activity levels, the ability to return to sporting activity, and ease of future revision procedures [13]. It has also been shown that individuals can improve their level of activity postoperatively [14]. There have been several complications reported such as limited range of motion [15-17], failed femoral components [18], femoral fracture [19], avascular necrosis [20], ion excretion [21,22] and tissue Synovitis [23,24]. These appear to be the result of a surgical learning curve as well as the need to modify the initial implant design [25]. |
| Several surgical approaches have been described in regard to performing hip resurfacing procedures [26]. The current standard of component fixation is cemented fixation of the femoral component combined with a cementless acetabular component fixation [27]. Numerous approaches including: anterior, posterior, lateral, or other variations have been described. Universal agreement in regard to an ideal approach does not exist [28]. In comparison to traditional THA procedures, where the entire femoral head and neck are removed and replaced with a prosthetic component, the HR procedure involves placement of a cap (via stem) onto the reshaped femoral head. The femoral neck and part of the femoral head are preserved ( Figure 1). A cup is inserted into the prepared acetabulum. Both components are composed of high carbon, as-cast, cobalt chrome (CoCr) alloy. This “metal-on-metal” design has been noted as concern in regard to potential complications that may result in higher ion concentration in the blood [5]. |
| One year following HR procedures, patients have shown range of motion and strength measurements lower than normative age related data and assistive devices used in 75% of the patients [29]. Two years following surgery, HR has produced similar results when compared to THA in young patients when considering Harris hip scores, pain, and activity levels. It was reported that HR patients had greater ROM at this time when compared to similar patients who received THA [30]. Results of three year follow-up evaluation using functional outcome measures such as the Harris Hip score have yielded very satisfactory results with excellent return to function [31]. |
| Five year postoperative follow-up research using Harris and Oxford Hip scores as well as UCLA activity level scores allowed the authors to conclude that hip resurfacing “produces an excellent outcome in the younger patient who requires surgical intervention for hip disease” [32]. Similar findings were revealed in a five year postoperative follow-up showing superior results in patients with HR versus THA [33]. In studies with a similar time frame, conclusions supporting HR in younger patients were published and it was noted that HR and THA have similar survivorship rates [34]. |
| Hip arthroscopy is becoming a more popular option for individuals with hip pain originating from various conditions. This procedure is typically reserved for the younger, relatively active population. Conditions amendable to arthroscopy include but are not limited to: acetabularlabral tears, femoral acetabular impingement, capsular laxity, and the presence of loose bodies within the joint [35]. While use of arthroscopy for chondral lesions has been described, advanced arthritis is typically considered a contraindication to the procedure [36]. Existing evidence suggests poor outcomes after patients with advanced arthritis were treated with arthroscopy [37]. Though the individual described in this case study was relatively younger and active, the degree of arthritic changes present in his hip joint would typically disqualify him as an ideal candidate to undergo an arthroscopic procedure. This patient’s advanced arthritic changes would more likely place them in the group of individuals who are ideal for a hip resurfacing procedure. |
| Case Description |
| The patient was a 45 year-old self-employed consultant who coached a college lacrosse team. Over the course of a three-year period progressive pain prevented him from participating in athletic/ recreational activities and eventually began to affect his ADL’s. The patient decided to consult with an orthopedic surgeon and was diagnosed with severe OA of the hip joint. Prior to the limitations secondary to hip joint OA he was active playing pick-up lacrosse, weight training, cycling, and jogging. After failure to improve with conservative treatment, the patient was presented with and accepted the option of undergoing a hip resurfacing procedure utilizing the Birmingham Hip Resurfacing system. |
| Findings or Interventions |
| The patient presented to physical therapy two days status post right HR. He was utilizing crutches with atouch-down weight bearing (TDWB) statusand ambulated with a slow, painful gait. Due to his inability to drive, the surgeon referred the patient to home care physical therapy. After establishing that the patient had normal distal sensation and circulation by evaluating light touch and palpating distal pulses, gait training was completed to ensure proper use of crutches and weight bearing status.Traditional THA precautions for a posterior lateral approach (no hip flexion beyond 90 degrees, no adduction across the midline, and no internal rotation) were reviewed and demonstrated, as instructed by the surgeon. Painfree therapeutic exercise was initiated and included 2-3 sets of 8-12 repetitions of supine isometric quadriceps setting, gluteal isometric setting, ankle AROM and heel slide activities. |
| During the first week after surgery, the patient wasseen by a home care physical therapist three times and treated with pain-free AROM, AAROM, and isometric lower extremity exercise. The initial goal was to slowly progress ROM, minimize pain, and avoid loss of strength due to inactivity. This program included 2-3 sets of 10 -15 repetitions of supine ankle AROM, isometric quadriceps setting, heel slide exercises, short arc quadriceps extension, and hip abduction activities. Gentle therapist-assisted AAROM exercise within traditional posterior lateral THA motion restrictions were performed for 3-5 minutes prior to and following the therapeutic exercise. Flexion, abduction, and rotation with the hip flexed to 90 degrees were performed in supine and extension was performed in the prone position. The exercise program, minus the AAROM, was conducted three times per day as pain allowed. The treatment and visit frequency was continued through week two as the patient progressed up to 3 sets of 20 repetitions for each exercise. |
| Three weeks after surgery the surgeon cleared the patient to begin progressive stretching of the hip musculature. The surgeon removed the traditional THA precautions at this point. Initially, the patient had difficulty moving the hip without compensatory pelvic motion. Hip flexion was achieved with posterior pelvic rotation, hip extension through anterior pelvic rotation, and abduction with a lateral lean and a hip hiking motion.At this point, single knee to chest activities were introduced for 5 reps of 20-30 seconds holding time. Seated flexion was also utilized to gain hip flexion motion. 4-way hip AROM standing in flexion, extension, abduction, and adduction was initiated using a mirror for feedback to assist in obtaining the motion from the hip and maintaining a relatively level pelvis. PRE’s were updated as well to include standing mini-squats and NWB hip flexion, extension, adduction, and adduction leg raises with an emphasis on hip motion. |
| During weeks three through five of the patient’s rehabilitation visit frequency was two to three times per week and emphasis was placed on proper gait pattern using visual feedback and education from clinician observation.AROM of the hip without compensation from the pelvis was emphasized. Feedback included verbal cues from the physical therapist, visual feedback using a mirror, pelvic stabilization from the therapist as the patient moved his hip, and therapist-assisted stretching and PROM. Specific stretching included NWB contractrelax and hold-relax techniques at end range flexion, extension, adduction, abduction, internal rotation and external rotation. The physical therapist asked the patient to maneuver his leg to the end of the appropriate range while providing a gentle counterforce to the pelvis. For hold-relax activities, the therapist instructed the patient to gently contract the muscle to be stretched for 15 - 20 seconds. When the patient relaxed, the therapist moved the hip further into the range of interest. Using contract-relax the therapist instructed the patient to contract the agonist muscle for 15 - 20 seconds, and when relaxed the therapist would move the hip into the increased available range. These stretches were performed a maximum of 3-5 times or until ROM gains plateaued. The stationary bike was utilized both as a light aerobic exercise and to facilitate motion. The seat of the stationary bike could be adjusted to provide greater movement into flexion as tolerated. |
| A consistentproblem that was noted involved the patient standing with his knee flexed and entire leg in external rotation. Additionally, he ambulated with a limp that resulted in a hip hiking motion in the frontal plane. The home care therapistpostulated that the patient had a trueleg length discrepancy after performing a long sit test. The authors acknowledge the lack of specificity and validity associated with this test [38]. No specific measures of leg length were performed at this time since further information regarding this issue would not have significantly impacted the rehabilitation process. It was also noted the patient had a flexion contracture of the right knee (approximately 4 degrees). In discussions with the patient and his family, it was reported that his limp was a long-standing gait pattern issue of approximately 15 years. When PROM was initiated a hard end feel was noted at the end of passive hip flexion and the patient noted that the hip “felt stuck.” |
| Six weeks after surgery, the patient was referred to outpatient physical therapy.The patient attended physical therapy sessions twice weekly. The patient was full weight bearing at this point, and continued to ambulate asymmetrically with decreased terminal extension of the involved hip during the stance phase of gait. General tightness of hip musculature was noted (hamstrings, adductors, rectus femoris, and iliopsoas complex). Strength was rated at 4/5 for all planes (compared to 5/5 on the non-surgical extremity). Selected AROM and pain measurements can be found in table 2. The patient described a consistent low-grade aching discomfort. Treatment at this point included manual stretching of all tight muscle structures and anterior tibial-femoral mobilization in an attempt to increase knee extension motion. All stretching activities were performed for 3 repetitions and held 30 seconds each. The joint mobilization technique was performed at a grade III level, held for 1 minute, and repeated 3 times. 4-way hip strengthening was progressed in standing using resistive tubing so that the involved side first moved the tubing, then was required to be the stance leg. These activities were later replicated on a 4-way hip resistance machine. |
| Weight bearing activities were progressed as tolerated, and included: wall squat exercises, multidirectional lunges (later progressed with handheld weights), and the leg press machine. Strengthening activities emphasizing motion in the transverse plane were also emphasized. An example of such an activity would include standing on one leg with the pelvis help parallel to the ground; followed by rotation of the pelvis on the fixed lower extremity. All strengthening exercises were initially prescribed for 3 sets of 10 repetitions, and then progressed up to 20 repetitions or to exhaustion. Progressive lumbopelvic stabilization activities were utilized as tolerated. Initially the patient performed various activities with upper and lower extremity movement while maintaining the lumbar spine and pelvis in a stable position. These activities were progressed by using a physioball to provide a less stable exercise surface. |
| Balance exercises were utilized as well. The patient was asked to maintain balance standing on both legs with a progressive decrease in base of support (placing the feet closer together and eventually in tandem). Balance activities would initially be performed for 3 trials, attempting to maintain position for 30 seconds per trial. Trial times were increased up to 60 seconds as tolerated by the patient. An attempt to optimize the patient’s gait pattern was made. The treating therapist provided feedback regarding gait symmetry and allowed for practice to correct the identified issues. The most notable issues were the previously described hip hike tendency in gait and lack of terminal knee extension secondary to the patient’s knee flexion contracture. The potential for these issues as long-term complications was recognized. |
| Endurance training was mainly accompanied through a progression of time and resistance on the stationary bike. The patient was able to progress up to 45 minutes on the stationary bike with variable levels of resistance. |
| Twelve weeks after surgery the patient did show improvement in ROM and pain variables (Table 1). The clinician observed that during gait he had a slight decrease in stance time on the involved leg and a slight decrease in stride length. Pain was not noted with ambulation for community distances with a maximum distance of approximately five city blocks. |
| The patient did note minor to moderate low back discomfort and stiffness that did not limit his normal activities. Additional treatment included long axis distraction, caudal glide, and posterior femoral glide mobilization techniques in an attempt to increase flexion. Long axis distraction was performed in supine with the hip at 30 degrees of flexion, 30 degrees of abduction, and slight external rotation. The therapist grasped the patient’s leg just proximal to the ankle and performed progressive distraction based on the interpretation of joint restriction. The caudal glide technique was performed with the patient in supine and the hip flexed to 90 degrees. The therapist grasped the proximal femur and directed movement of the femur in a caudal direction. Posterior femoral glide activities were performed in supine as well. The patient’s hip was placed just short of end-range flexion. The therapist then applied a force to the proximal femur in a posterior direction. All mobilization techniques were performed up to a grade III level, and maintained for 2 to 3 sets of 1-minute applications. |
| Resisted lateral movements such as resisted side-stepping with elastic tubing and lateral slides were performed in each direction. Balance activities were progressed from bilateral, to unilateral stance initially with eyes open, and then closed when the patient could maintain balance and a level pelvis. The patient was asked to balance on a stable surface, and then less stable surfaces were introduced (rocker-board or air-filled disc) along with progressively more aggressive levels of manually applied perturbation forces. |
| Twelve weeks after surgery the patient showed improved hip strength (4/5 for flexion and abduction, 5/5 for internal rotation, external rotation, and extension). Hip flexibility was notably improved, though tightness of the hamstring muscle group persisted and was observed bilaterally. The patient did note times of no discomfort (Table 2). When asked to rate his overall level of functioning as a percentage of what the patient considered optimal, he estimated being 80% of the optimal level. Gentle force attenuation and landing activities were added. Activities included: stepping off boxes of various sizes and landing in a predetermined position (landing on both legs, then progressing to single leg landing). In addition, loaded rotation and pivoting activities as well as acceleration/deceleration activities in multiple planes of movement were initiated. |
| Outcomes |
| The final outpatient physical therapy visit occurred 15 weeks following surgery. ROM and pain improved (Table 2). Strength was rated at 5/5 for all planes, except abduction, which was still rated at 4/5. His gait was observed and the PT noted “relatively normal” gait with no pain. When asked to rate his overall level of functioning as a percentage of what the patient considered optimal, he estimated being 87% of the optimal level. |
| Approximately 10 months after the procedure a follow-up visit was made with the patient for an interview and to determine his status. The patient reported pain free ability participating in lacrosse practice for periods up to two hours, jogging on sidewalks and trails for distances up to three miles, stationary cycling for up to sixty minutes, cycling on level trails for up to two hours, using the elliptical trainer for up to thirty minutes, and playing tennis recreationally. He was unable to perform any of these activities prior to surgery without significant pain. The patient continued to partake in a general strength and aerobic activity program as part of an overall active lifestyle. The therapist found the patient to have minor limitations bilaterally in the FABER test position, no Trendeleburg Sign, and a loss of 5 degrees of knee extension on the involved side. Subjectively the patient was pleased with the outcome. |
| Discussion |
| The purpose of this case report was to describe the rehabilitation following a relatively new procedure. Research on the specific interventions following this procedure is limited; with only one case study of a bilateral resurfacing existing in the physical therapy literature [39]. The patient achieved increases in flexion, extension, and abduction AROM measurements consistent with normal ranges of motion. His reported pain scale consistently decreased until a painfree level of function was achieved. |
| Limitation in our initial rehabilitation occurred due to a lack of familiarity with the procedure and what activities have been shown to be safe in the rehabilitation process. Traditional limitations of the case study model were also present. If we had access to established rehabilitation guidelines for this procedure, we may have been more aggressive in initially attempting to regain range of motion. However, specific guidelines do not exist. The surgeon initially utilized a traditional model of rehabilitation for THA. The patient’s initial compensation to hip motion was continually addressed in therapy and was a large part of our intervention. Perhaps, if we could have isolated all hip motions initially through manual therapy and followed those motions with a clear home program, this may have been reduced. This patient was a unique example because he had a long-standing gait abnormality that may have been associated with his progressing hip pain or a congenital leg length discrepancy. The authors could not confirm either hypothesis secondary to not evaluating the patient preoperatively. |
| Inthis case, HR was treated by accelerated/aggressive rehabilitation resulted in improvements in hip strength and motion, self-reported function, and no adverse events.HR appears to be a reasonable choice for young, active patients with hip OA. Our experience leads us to believe in the importance of emphasizing the need for the early restoration of properly isolated hip AROM through the use ofhip stretching and mobilization that are outside the traditional postoperative rehabilitation of THA procedures. Traditional THA precautions such as limitations in range of motion do not appear to be warranted with the HR patient. Safe higher-level activities, such as landing drills, loaded rotation and pivoting activities were initiated in this case by12 weeks post operatively. Although this patient was able to return to sports, whether HR will allow a return to competitive athletics is still unknown. In addition, the long-term results, greater than 10 years post operatively, have not been fully investigated. The treatment program introduced in this case study resulted in the safe and effective treatment of an active 45-year old that underwent a HR procedure. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
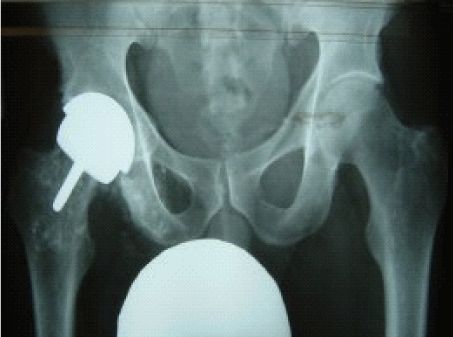 |
| Figure 1 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 16472
- [From(publication date):
May-2013 - Sep 03, 2025] - Breakdown by view type
- HTML page views : 11778
- PDF downloads : 4694
