Case Report Open Access
Physical Therapy Management of a Patient with Anterior Canalithiasis using the Deep Head Hanging Maneuver
| Amer Al Saif1 and Eric G. Johnson2* | |
| 1Department of Physical Therapy, King Abdulaziz University, Jeddah, KSA | |
| 2Department of Physical Therapy, Loma Linda University, Loma Linda, CA, USA | |
| Corresponding Author : | Eric Johnson Loma Linda University, 24951 North Circle Drive Nichol Hall 1900, Loma Linda, CA 92350, USA Tel: (909) 558-4632 ext. 47471 Fax: (909) 558-0459 E-mail: ejohnson@llu.edu |
| Received June 04, 2012; Accepted July 09, 2012; Published July 13, 2012 | |
| Citation: Al Saif A, Johnson EG (2012) Physical Therapy Management of a Patient with Anterior Canalithiasis using the Deep Head Hanging Maneuver. J Nov Physiother 2:117. doi: 10.4172/2165-7025.1000117 | |
| Copyright: © 2012 Al Saif A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
A 61-year-old female patient presented with a chief complaint of chronic vertigo that started suddenly four months ago. Her symptoms included intermittent nausea and position related vertigo. The left Hallpike-Dix test produced the patient’s vertigo and nausea. Weak left torsional downbeat nystagmus of approximately 10 seconds duration was also observed. The straight head hanging (HH) test was subsequently performed and it produced multiple beats of robust left torsional downbeat nystagmus of approximately 30 seconds duration. The patient was diagnosed with left anterior canalithiasis, which is a type of benign paroxysmal positional vertigo (BPPV). The deep head hanging maneuver (DHM) was performed and the patient reported feeling better immediately afterward. The HH test was performed again within a couple of minutes and the patient reported 80% resolution of both her vertigo and nausea. The patient was seen the following day and reported 100% resolution of symptoms. Her symptoms remained resolved at a 1 week follow-up. Based on the limited research concerning the examination and intervention methods described in this single subject case report, further research including controlled clinical trials are needed.
| Keywords |
| Vestibular rehabilitation; Benign paroxysmal positional vertigo; Physical therapy; Straight head hanging test; Deep head hanging maneuver |
| Introduction |
| Benign paroxysmal positional vertigo (BPPV) is one of the most common diagnoses made in primary care and neuro-otology clinics [1]. Within the labyrinth of the inner ear lie collections of calcium crystals called otoconia [2]. For a variety of reasons, in patients with BPPV, the otoconia are dislodged from their usual position within the utricle and travel through the endolymphatic fluid into one of the three semicircular canals (SCC) of the inner ear [2]. After angular position changes, the involved SCC sends the brain inaccurate signals that the stationary head is still moving [3]. It has been reported that 80-90% of all BPPV cases are the result of otoconia being trapped in the posterior SCC (PSC) and 10-12% in the horizontal SCC (HSC) [4,5]. There is much more debate concerning the anterior SCC (ASC) and reports vary from 2-21% [6]. Symptoms of BPPV include brief attacks of dizziness (vertigo) associated with nystagmus, lightheadedness, imbalance, and nausea that are provoked by angular position changes such as bending forward, sitting up, and rolling over in bed [2]. These symptoms can last from days to months and may be recurrent over many years. BPPV is often idiopathic; however, in older people the most common cause is degeneration of the utricular gelatinous matrix that supports the otoconia [7]. |
| Diagnosing BPPV is made on the basis of a characteristic history including positional vertigo that can be induced by the Hallpike-Dix test [2]. The addition of using infrared goggles with the Hallpike-Dix test improves the accuracy of the test. During the Hallpike-Dix test, the patient long-sits on an examination table with their head rotated approximately 45 degrees to one side. The clinician then assists the patient into a supine position with their head and neck extended slightly below the level of the table while maintaining the rotated head position [3,8,9]. Symptoms typically begin a few seconds after assuming this position due to the gravitational impact that moves the otoconia within the SCC’s. This increases the internal pull on the endolymphatic fluid of the SCC producing a more vigorous bending of the cilia within the ampulla of the SCC [3]. The end result of the Hallpike-Dix test, in the presence of BPPV, is torsional jerk nystagmus in the vertical plane (anterior and posterior SCC’s) of typically short duration suggesting a specific type of BPPV called canalithiasis. The clinician can determine the SCC involved by observing the directionality of the eye movements provoked [3]. ASC canalithiasis is characterized by paroxysmal downbeating nystagmus lasting less than 60 seconds [10,11]. The most common clinical intervention for canalithiasis is the canalith repositioning maneuver (CRM), also known as the Epley maneuver [12]. The CRM is widely considered the primary treatment for vertical SCC canalithiasis. |
| While the effectiveness of the CRM for PSC canalithiasis has been established in the literature, this is not the case for ASC canalithiasis [10,11]. Yacovino et al. [13] suggest using the Deep Head Hanging maneuver (DHM) as the primary treatment for ASC canalithiasis. The DHM is performed on an examination table in a similar manner to the CRM. Because the ASC has a different trajectory than the PSC, maneuvers targeting ASC canalithiasis differ geometrically from those described by Epley for PSC canalithiasis [10]. The DHM is intended to invert the ASC and allow debris to fall to the “top” of the ASC, and then, upon sitting, allow it to further migrate into the common crus and then the utricle [10]. The DHM has the advantage that the clinician does not need to know the affected side [13]. According to Casani et al. [11], the ASC is much nearer to the sagittal plane than the PSC so keeping the head in a neutral non-rotated position is more beneficial in mobilizing the particles in the ASC compared to rotary movements. Casani et al. [11] contend that rotation of the head by 45 degrees toward one side, such as during the CRM, may prevent the amount of dependent position required to successfully move the otoconia through the ASC. The purpose of this case report is to provide anecdotal evidence for successful resolution of ASC canalithiasis using the DHM. |
| Case Summary |
| A 61-year-old Saudi female elementary school teacher presented with a chief complaint of chronic vertigo that started suddenly four months ago. Symptoms include nausea and positional related vertigo. She was referred by an ear, nose and throat (ENT) physician with a diagnosis of positional vertigo. The patient denied a previous diagnosis of positional vertigo or any recent history of trauma or infection that may have predisposed her to developing positional vertigo. Her familial and social history was unremarkable and she reported that she was not taking any medications. The subjective examination revealed intermittent position-provoked vertigo lasting 20 to 30 seconds after gross angular position changes and nausea. Primary provocative position changes were right head/neck rotation and head/neck extension. The physical examination included screening tests for cervical instability, cervical positional tolerance, and videonystagmography (VNG). The VNG provides objective assessment of the occulomotor and vestibular systems and assists in determining central versus peripheral involvement. Once it was determined that there was no central-mediated problem, cervical instability, or cervical positional intolerance, a right Hallpike-Dix test was performed using the VNG and it was negative. The patient was returned to the long-sitting position and after a brief rest, a left Hallpike- Dix test was performed. This test produced the patient’s vertigo and nausea and weak left torsional downbeat nystagmus of approximately 10 seconds duration was observed. At this time, the straight head-hanging (HH) test was performed to establish ASC involvement. During the HH test, the patient long-sits on an examination table with their head in neutral. The clinician then assists the patient into a supine position with their head extended as far as possible so that their head hangs over edge at 30 degrees below horizontal. The patient is instructed to look straight ahead and the clinician observes for nystagmus. In the present case, the HH test produced multiple beats of robust left torsional downbeat nystagmus of approximately 30 seconds duration. The patient was diagnosed with left ASC canalithiasis. A CRM was performed and the patient was returned to a sitting position. The patient was agreeable to a second HH test within a couple of minutes, which again produced her nausea, vertigo, and multiple beats of robust left torsional down-beat nystagmus of approximately 30 seconds duration. At that time, the decision was made to perform the DHM. The patient reported that she felt better immediately after the DHM was performed. The HH test was performed within a couple of minutes and the patient reported 80% resolution of both her vertigo and nausea during and immediately after the test was completed. The patient was instructed to minimize angular head movements, avoid sleeping on the affected side, and use an extra pillow for a slightly elevated position that night. Her follow-up examination was scheduled the next day. The patient returned the following day and reported 100% resolution of both her vertigo and nausea. The HH test was negative as nystagmus was not observed and there were no reports of vertigo or nausea. The patient returned for a third appointment one week later and she continued to report 100% resolution of all symptoms. The patient was discharged at this time and instructed to return to the clinic if she had any recurrence of symptoms. No other home interventions were given. This patient outcome was expected given the examination findings and there were no unanticipated effects of the patient management process. |
| Discussion |
| The mechanism driving BPPV is otoconia pathologically located in one of the three SCC’s of the inner ear. Because otoconia have mass, angular position changes impact the involved SCC as the otoconia move within the endolymphatic fluid [2,3]. This movement results in an increased neural firing rate of the involved inner ear and a sensory mismatch between the systems responsible for position-sense and balance [3]. The symptomatic consequence includes nausea and vertigo lasting seconds to minutes [1,3]. Medical management aimed at resolving BPPV includes the CRM or liberatory maneuvers depending upon the specific BPPV type [1,2]. The purpose of these interventions is to physically remove the otoconia from the SCC and relocate it back into the utricle using gravity via a systematic progression of head position changes. |
| In the case presented above, the patient reported chronic positional vertigo and nausea for approximately 4 months. Both the left Hallpike- Dix and HH tests were positive for ASC canalithiasis and symptoms were much clearer and stronger with the HH test. During the HH test, multiple beats of robust torsional downbeat nystagmus of approximately 30 seconds duration were observed suggesting anterior canalithiasis [10,11]. During the HH test, the head reaches a more dependent position compared to the Hallpike-Dix test by about 20 degrees. This is important for maximally provoking ASC canalithiasis [10]. Bertholon et al. [14] suggest that the HH test is the best way to trigger ASC canalithiasis. In the present case, the DHM for ASC canalithiasis was implemented successfully. Our findings are consistent with those reported by Yacovino et al. [13] and Casani et al. [11]. Yacovino et al. [13] reported resolution of symptoms in all 13 subjects treated for ASC canalithiasis using the DHM. The authors reported that most patients required a single DHM and over-all, 1.23 DHM’s were required for symptom resolution. Similarly, Casani et al. [11] reported resolution of ASC canalithiasis symptoms after 1 or 2 treatment sessions using the DHM in 15 of 18 patients. A third treatment session was required for 2 patients and one patient did not respond to the intervention. Although Casani et al. [11] reported a semicircular canal switch in several patients; we did not observe this occurrence in the patient described in this case report. |
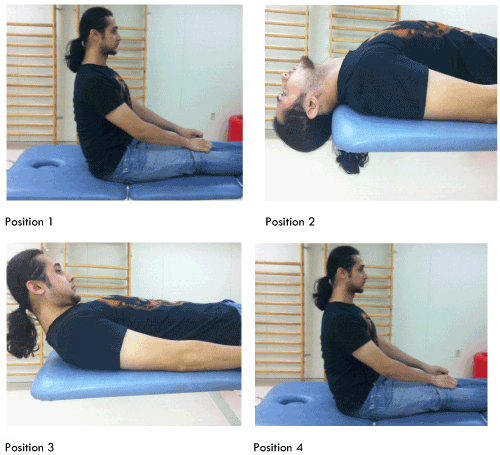
| The DHM consists of 4 steps with intervals of at least 30 seconds (Figure 1) [10]. The patient is assisted from a long-sitting position into a supine position with their head extended backwards by 30 degrees. Next, the supine position is maintained while their head is flexed forward 45 degrees above the horizontal plane. Finally, the patient is returned to the sitting position. In position 1, the otoconia lie near the ASC ampulla. In position 2 (head-hanging position), both ASC’s are inverted with their ampullas superior and their non-ampullary endings medial and inferior. Otoconia migrate due to their weight towards the apex of the ASC. In position 3 (chin to chest), gravity facilitates further migration towards the common crus [10]. Finally, in position 4, the patient sits up with head tucked in [10]. This last step allows otoconia to move through the common crus and into the utricle [10,11]. |
| In this case report we described the clinical management of a patient presenting with ASC canalithiasis. The HH test was performed to make the clinical diagnosis and the DHM was used to successfully treat the patient condition. Based on the limited research concerning the examination and intervention methods described in this single subject case report, further research including controlled clinical trials are needed. |
References
- Bronstein AM (2003) Vestibular reflexes and positional maneuvers. J Neurol Neurosurg Psychiatry 74: 289��?293.
- Fife TD, Iverson DJ, Lempert T, Furman JM, Baloh RW, et al. (2008) Practice parameter: therapies for benign paroxysmal positional vertigo (an evidence-based review): report of the Quality Standards subcommittee of the American Academy of Neurology. Neurology 70: 2067-2074.
- Herdman SJ, Tusa RJ (2007) Physical therapy management of benign positional vertigo, in Herdman S (Ed) Vestibular Rehabilitation. (3rd edn), F. A. Davis, Philadelphia.
- Jackson LE, Morgan B, Fletcher JC Jr, Krueger WW (2007) Anterior canal benign paroxysmal vertigo: an underappreciated entity. Otol Neurotol 28: 218- 222.
- Parnes LS, Agrawal SK, Atlas J (2003) Diagnosis and management of benign paroxysmal positional vertigo (BPPV). CMAJ 169: 681-693.
- Korres S, Balatsouras DG, Kaberos A, Economou C, Kandiloros D, et al. (2002) Occurrence of semicircular canal involvement in benign paroxysmal positional vertigo. Otol Neurotol 23: 926-932.
- Parnes LS, McClure JA (1992) Free-floating endolymph particles: a new operative finding during posterior semicircular canal occlusion. Laryngoscope 102: 988-992.
- Furman JM, Cass SP (1999) Benign paroxysmal positional vertigo. N Engl J Med 341:1590��?1596.
- Epley JM (2001) Human experience with canalith repositioning maneuvers. Ann N Y Acad Sci 942:179��?191.
- Kim YK, Shin JE, Chung JW (2005) The effect of canalith repositioning for anterior semicircular canal canalithiasis. ORL J Otorhinolaryngol Relat Spec67: 56-60.
- Casani AP, Cerchiai N, Dallan I, Sellari-Franceschini S (2011) Anterior canal lithiasis: diagnosis and treatment. Otolaryngol Head Neck Surg 144: 412-418.
- Epley JM (1992) The canalith repositioning procedure: for treatment of benign paroxysmal positional vertigo. Otolaryngol Head Neck Surg 107: 399-404.
- Yacovino DA, Hain TC,Gualtieri F(2009) New therapeutic maneuver for anterior canal benign paroxysmal positional vertigo. J Neurol 256: 1851-1855.
- Bertholon P, Bronstein AM, Davies RA, Rudge P, Thilo KV (2002) Positional down beating nystagmus in 50 patients: cerebellar disorders and possible anterior semicircular canalithiasis. J Neurol Neurosurg Psychiatry 72: 366372.
Figures at a glance
 |
| Figure 1 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 10145
- [From(publication date):
October-2012 - Aug 25, 2025] - Breakdown by view type
- HTML page views : 5455
- PDF downloads : 4690
