Pkd-Tsc Syndrome and Renal Cell Carcinoma: A Case Report
Received: 18-Mar-2014 / Accepted Date: 17-Apr-2014 / Published Date: 19-Apr-2014 DOI: 10.4172/2161-0681.1000170
Abstract
Introduction: In this work we report a clinical case of PKD-TSC syndrome, with a review of current literature.
Case report: In August 2013 we admitted in our clinic a patient with an history of Tuberous Sclerosis Complex (TSC) who had a CT finding of right renal tumor in a kidney with multiple cists. After performing a right radical nephrectomy, a genetic investigation assessed that the patient was affected by “PKD-TSC syndrome”, with a deletion on chromosome 16p 13.3.
Discussion: Genomic findings demonstrated that PKD-TSC syndrome is due to large deletions in chromosome 16 that results in deletion of part or all of both the TSC2 and the PKD1 gene, giving both aspects of Polycystic Kidney Disease and Tuberous Sclerosis Syndrome.
Conclusion: Our report is emblematic of this rare disease that has a genetic pathogenesis that needs further studies to be totally understood.
Keywords: Pkd-tsc syndrome; Renal cell carcinoma; Surgery; Genetic disorders
313912Introduction
Autosomal Dominant Polycystic Kidney Disease (AD-PKD) and Tuberous Sclerosis Complex (TSC) are two well described genetic disorders. However, in Literature [1] it’s documented an uncommon condition, due to a deletion on chromosome 16p13.3, who involves both PKD1 and TSC2 genes, called “PKD-TSC syndrome”. Little more than 30 cases are described in literature, with none specific relation to age [2]. We report a case of a 42-years-old man with Polycystic Kidney Disease and Tuberous Sclerosis Complex who presented with a Computed Tomography (CT) finding of a 25 mm upper pole right renal neoplasm, associated with a 20 mm angiomyolipoma, inside a cystic formation with Antero-Posterior (AP) diameter 62 mm, Latero-Lateral (LL) 55 mm and Cranio-Caudal (CC) 53 mm. The patient underwent a right radical nephrectomy and was discharged six days after.
Case Report
In August 2013, a 42-years-old man came to our attention sent by his family physician, with a report of impaired renal function associated with right renal colics and pyelonephritis.
This patient was already affected by tuberous sclerosis that causes him recurrent convulsive crisis, for which he was in therapy with Carbamazepine since 2010.
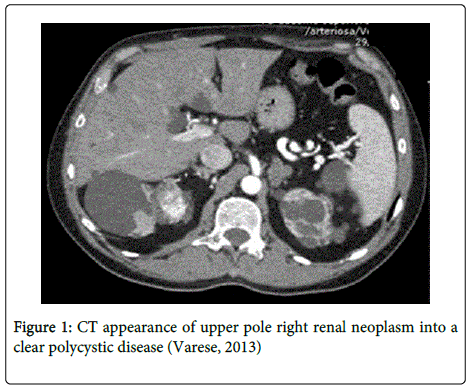
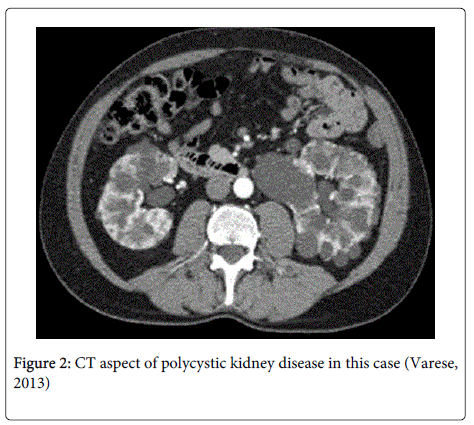
Admitted in Our department, we assessed medical antibiotic therapy and we performed a Computed Tomography (CT), who showed an image of bilateral renal enlargement due to a polycystic disease (Figures 1 and 2). The patient hadn’t any previous familiar history for Polycystic Kidney Disease. At the superior third of right kidney, an exophytic cyst of 62×55×53 mm presented on its posterior-medial wall a solid 20 mm formation (Figure1). Nearby, there was a roundish 25 mm solid formation, which showed a disomogeneous density value with rapid contrast enhancement, dubious of neoplastic disease. Contemporary, a hepatic asymptomatic cystic disease was assessed. The indication was surgical and we opted for a right radical nephrectomy, as renal function was already impaired and the patient was candidate to dialysis.
The intervention was performed in October 2013, delayed as he had a convulsive episode on August, studied with a basal EEG and neurological evaluation after the regression of acute infective disease. The day of surgery, the patient had a near-syncope with bradycardia, so the intervention was delayed of two days. Surgical access was a mono-lateral right subcostal incision and we performed a radical nephrectomy of a 15×8×7,5 cm kidney; total operating time was 2,20 hours. The first post-operative days were characterized by a temporary amylases increase, stabilized after few days. Ultrasound and radiological verifications didn’t noticed any early surgical complication.
The Pathologist report was of a 22 mm nodule of clear cell renal cell carcinoma pT1a, pNx, G2, associated with a 20 mm angiomyolipoma in an adult renal multicystic disease. The patient was discharged in good general conditions and also postoperative follow up at three and six months didn’t show any early neoplastic recurrence. As Tuberous Sclerosis Complex was coexisting with a condition of multicystic renal disease, our pathology division carried out a genomic evaluation of the case, discovering the deletion of TSC2 and PKD1 region on chromosome 16p13.3, pathognomonic of “PKD-TSC syndrome”.
Discussion
PKD and TSC are both genetic disorders that, on the surface, may not appear to be closely related. One disorder (TSC) is associated with the development of benign tumors in many organs and often results in seizures, epilepsy, sebaceous adenomas of the skin [3], kidney diseases like angiomyolipomas, that are found in approximately 45-80% of patients affected and mental retardation, whereas PKD is generally thought of as a disease of the kidneys that develops a high amount of cists, with a fast decrease of renal function although cystic and non-cystic lesions in other organs are common, together with vascular and cardiac malformations like cerebral aneurysms or aortic root dilatation. However, both diseases are associated with cysts in the kidney. Furthermore, since the identification of genes for these disorders in the mid-90s, there have been suggestions of a linked pathogenesis. Clinical manifestations of TSC are the result of a mutation of two tumor suppressor genes, TSC1 and TSC2, giving a systemic disease [4]. Tuberin, the TSC2 protein, plays a role in localizing polycystin-1 (the PKD1 protein) to the cell surface, regulating cell cycle. Related signaling pathways may be involved in both disorders. The mTOR pathway, a regulator of cell proliferation, is centrally important in TSC and may also be involved in PKD.
Recently findings in genetics, determined that TSC loci are in chromosome 9q34 (TSC1) and 16p13.3 (TSC2). The major gene for ADPKD (PKD1) has also been identified and mapped on chromosome 16p13.3, adjacent to the TSC2 locus [5]. Recent works [6,7] determined that the first pathogenetic factor in this disease is a deletion of TSC2 and PKD1 region, giving both aspects of Polycystic Kidney Disease and Tuberous Sclerosis Syndrome. The typical finding that underlines PKD-TSC syndrome is an angiomyolipoma in pathologic specimen of patients with history of Polycystic Kidney Disease. Even if the most common finding in this disease is multiple hamartomas in different organs like brain, skin, kidney, liver, lung and heart, it’s also possible to develop malignant tumors, mainly renal or brain [8]. In PKD-TSC syndrome Renal Cell Carcinoma (RCC) develops within dysplastic epithelial cysts, and mean age of diagnosis for people with PKD-TSC-associated RCC is 25 years lower than common population.
Conclusion
Our clinical case is emblematic of PKD-TSC syndrome, with a phenotype clearly due to this disease. Surgical resection of the tumor is clearly the best option to adopt in this case, aiming to oncological radicality. The patient didn’t present any early recidivism during his follow-up examinations at three and six months. PKD-TSC syndrome is a genetic disease that carries both manifestations of AD-PKD and TSC, due to large deletions in chromosome 16 that results in deletion of part or all of both the TSC2 and the PKD1 gene.
References
- Boehm D, Bacher J, Neumann HP (2007) Gross genomic rearrangement involving the TSC2-PKD1 contiguous deletion syndrome: characterization of the deletion event by quantitative polymerase chain reaction deletion assay. Am J Kidney Dis 49: e11-21.
- Laass MW, Spiegel M, Jauch A, Hahn G, Rupprecht E, et al. (2004) Tuberous sclerosis and polycystic kidney disease in a 3-month-old infant. PediatrNephrol 19: 602-608.
- Kacerovska D, Vrtel R, Michal M, Vanecek T, Vodicka R, et al. (2009) TSC2/PKD1 contiguous gene syndrome: a report of 2 cases with emphasis on dermatopathologic findings. Am J Dermatopathol 31: 532-541.
- Neumann HP, Schwarzkopf G, Henske EP (1998) Renal angiomyolipomas, cysts, and cancer in tuberous sclerosis complex. SeminPediatrNeurol 5: 269-275.
- Martignoni G, Bonetti F, Pea M, Tardanico R, Brunelli M, et al. (2002) Renal disease in adults with TSC2/PKD1 contiguous gene syndrome. Am J SurgPathol 26: 198-205.
- Torra R, Badenas C, Darnell A, Camacho JA, Aspinwall R, et al. (1998) Facilitated diagnosis of the contiguous gene syndrome: tuberous sclerosis and polycystic kidneys by means of haplotype studies. Am J Kidney Dis 31: 1038-1043.
- Sampson JR, Maheshwar MM, Aspinwall R, Thompson P, Cheadle JP, et al. (1997) Renal cystic disease in tuberous sclerosis: role of the polycystic kidney disease 1 gene. Am J Hum Genet 61: 843-851.
- Martignoni G, Bonetti F, Pea M, Tardanico R, Brunelli M, et al. (2002) Renal disease in adults with TSC2/PKD1 contiguous gene syndrome. Am J SurgPathol 26: 198-205.
Citation: Pirola GM, Saredi G, Pacchetti A, Marconi AM (2014) Pkd-Tsc Syndrome and Renal Cell Carcinoma: A Case Report. J Clin Exp Pathol 4:170. DOI: 10.4172/2161-0681.1000170
Copyright: © 2014 Pirola GM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16501
- [From(publication date): 6-2014 - Aug 31, 2025]
- Breakdown by view type
- HTML page views: 11833
- PDF downloads: 4668