Case Report Open Access
Posterior Vaginal Wall Cyst Mimicking Rectocele
Hediye Dagdeviren, Caglar Helvacioglu, Ammar Kanawati, Cihan Kaya* and Huseyin CengizDepartment of Obstetrics and Gynaecology, Bakirkoy Dr. Sadi Konuk Teaching and Research Hospital, Istanbul, Turkey
- *Corresponding Author:
- Cihan Kaya
Department of Obstetrics and Gynaecology
Bakirkoy Dr. Sadi Konuk Teaching and Research Hospital
Istanbul, Turkey
Tel: +905536161385
E-mail: drcihankaya@gmail.com
Received date: March 10, 2017; Accepted date: March 13, 2017; Published date: March 18, 2017
Citation: Dagdeviren H, Helvacioglu C, Kanawati A, Kaya C, Cengiz H (2017) Posterior Vaginal Wall Cyst Mimicking Rectocele. J Preg Child Health 4:306. doi:10.4172/2376-127X.1000306
Copyright: © 2017 Dagdeviren H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Vaginal wall cysts occur rarely and can cause a variety of symptoms. A 35-year-old woman presented with history of mass bulging from vagina for a-year. Pelvic examination revealed a reducible non-tender mass protruding from the vagina and diagnosed as rectocele. Physical examination is important for the detection and characterization of vaginal cysts but may be inadequate for appropriate diagnosis.
Keywords
Mullerian cyst; Rectocele; Vagina.
Introduction
Benign cystic lesions of the vagina are uncommon. Mesonephric (Gartner’s duct) cysts, Bartholin gland cysts, Mullerian cysts and squamous inclusion cysts are the most type of vaginal cystic lesions [1]. This paper presents a rare case of large posterior vaginal wall cyst of Mullerian origin mimicking as rectocele.
Case
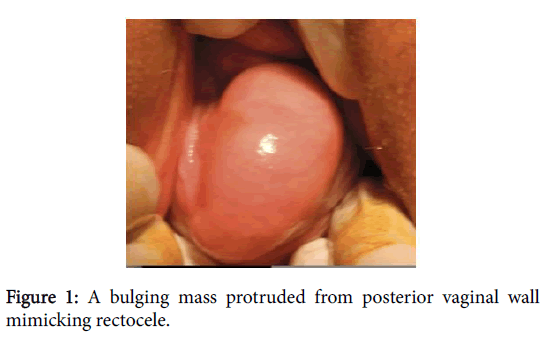
A 35 year old multiparous woman was admitted to our gynaecology clinic with a complaint of reducible non-tender mass protruding from the vagina noted for about one year. The mass bulged from her vagina intermittently, especially during coughing, squatting or having bowel movements. Also she had discomfort during defecation. On her pelvic examination, a bulging mass protruded from posterior vaginal wall (Figure 1). The mass was soft and could be compressed manually easily. The mass appeared to be a rectocele and a colpography posterior operation was planned. Informed consent included permission for documentation of the case was taken from the patient before the operation. After dissection of the posterior vaginal wall there was a 5 cm diameter cyst lying deep of the posterior vaginal wall.
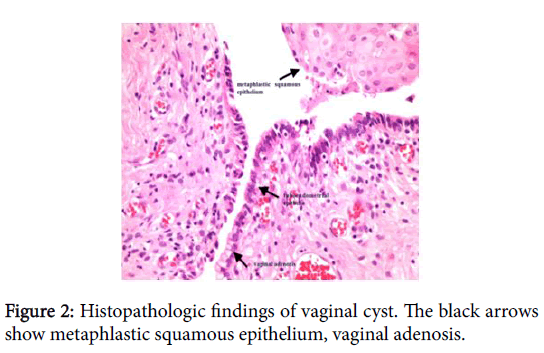
Cyst was dissected completely from the rectum and posterior vaginal wall. The final pathologic report was a cyst derived from müllerian epithelium arise from patches of vaginal adenosis and are lined by tuboendometrial- or mucinous-type epithelia and metaplastic squamous epithelium (Figure 2). Her follow-up and long-term recovery period was uneventful.
Discussion
Mullerian duct cysts are remnants of the embryological paramesonephric ducts [2]. Usually they are single and they have been reported to be located typically anterolateral vaginal wall [3,4]. Controversely in our case cyst was located at the posterior vaginal wall. Most of them are asymptomatic but, rarely an abscess can develop in a Mullerian cyst presenting with chronic pelvic pain and deep dyspareunia [5]. Also, adenocarcinoma arising from a vaginal Mullerian cyst had been reported previously [3].
Vaginal wall cysts are usually discovered incidentally on physical examination. In some patients cysts may cause as mild discomfort, feeling of vaginal pressure and fullness. Also, posterior cysts may cause constipation and painful defecation. Our case was presented with complaints of a mass protruding through the vagina for a year which was increasing in size but there were no associated urinary or bowel symptoms.
In most cases, the appropriate diagnosis can be made on history and examination. Prolapse of pelvic organs such as a cystocele or rectocele, can mimic a vaginal cyst, so they should be ruled out in differential diagnosis [5,6]. As in our case, the mass protruding from the vagina appeared to be a rectocele, first. Magnetic resonance imaging may be useful in differential diagnosis of vaginal masses and ruling out vaginal prolapse [4,7]. Techniques such as reducing the prolapse while the patient performs the Valsalva manoeuvre, changing her position may be useful to rule out prolapse [5].
References
- Pradhan S, Tobon H (1986) Vaginal cysts: A clinicopathological study of 41 cases. Int J Gynecol Pathol 5: 35-46.
- Kresowik J, Kennedy CM, Wing S (2007) Prolapsing vaginal cyst: A case report. J Reprod Med 5552: 852-854.
- Hwang JH, Jeong MO, Lee NW (2009) Multiple Mullerian cyst: A case report and review of literature. Arch Gynecol Obstet 280: 137-139.
- Wai CY, Corton MM, Miller M (2004) Multiple vaginal wall cysts: Diagnosis and surgical management. Obstet Gynaecol 103: 1099-1102.
- Montella JM (2005) Vaginal Mu¨llerian cyst presenting as a cystocele. Obstet Gynecol 105: 1182-1184.
- Lucente V, Benson JT (1990) Vaginal M u¨ llerian cyst presenting as an anterior enterocele: A case report. Obstet Gynecol 76: 906-908.
- Cil AP, Basar MM, Kara SA (2008) Diagnosis and management of vaginal mullerian cyst in a virgin patient. Int Urogynecol J 19: 735-737.
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 27100
- [From(publication date):
April-2017 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 26052
- PDF downloads : 1048