Case Report Open Access
Prenatal Diagnosis of a True Knot of the Umbilical Cord in Twins Pregnancy
| Eran Ashwal, Ron Bardin, Amir Aviram, Yoav Peled, Yariv Yogev and Liran Hiersch* | |
| Department of Obstetrics and Gynecology, Helen Schneider Hospital for Women, Rabin Medical Center, Tel Aviv University, Israel | |
| Corresponding Author : | Liran Hiersch Department of Obstetrics and Gynecology Helen Schneider Hospital for Women Rabin Medical Center Tel Aviv University, Israel Tel: +972-3-9377400 Fax: +972-3-9377409 E-mail: lirhir@gmail.com |
| Received: October 09, 2015; Accepted: October 26, 2015; Published: November 02, 2015 | |
| Citation: Ashwal E, Bardin R, Aviram A, Peled Y, Yogev Y, et al. (2015) Prenatal Diagnosis of a True Knot of the Umbilical Cord in Twins Pregnancy. J Preg Child Health 2:198. doi:10.4172/2376-127X.1000198 | |
| Copyright: © 2015 Ashwal E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Background: True knot of the umbilical cord is an uncommon finding, which is difficult to diagnose antenatally. The appropriate management of patients with a sonographically identified true knot is yet to be determined.
Case: We present a twin pregnancy, in which antenatal diagnosis of a true knot of the umbilical cord was made at 33 weeks’ gestation. Fetal Doppler examination showed an absence of end diastolic flow in the umbilical artery of the second twin.
Conclusion: The appropriate management of patients with a true knot identified prenatally is unclear. Once diagnosis is suspected, further fetal surveillance is warranted.
| Keywords |
| Twin pregnancy; Umbilical cord; Diabetes mellitus; Doppler ultrasound imaging |
| Introduction |
| The reported incidence of true knots in the umbilical cord ranges from 0.3 to 2.1% of all deliveries and is associated with approximately 6% of all cases of perinatal mortality [1]. Known predisposing factors for the formation of a true knot include elongated umbilical cord, small fetus, polyhyramnios, monoamniotic twin pregnancy, male gender, diabetes mellitus, and multiparity [2]. |
| Although most true knots are loose, do not have clinical significance and present as an incidental finding at delivery, true cord knots are well known to be associated with intrauterine death [3]. |
| Even though antenatal diagnosis of a true umbilical cord knot is possible, such a diagnosis may be difficult, even with the employment of color Doppler flow imaging [4]. |
| We present a case of a twin pregnancy, in which the antenatal diagnosis of a true knot of the umbilical cord was made using grayscale and Doppler ultrasound imaging. |
| Case Report |
| A 33-year-old woman was referred at 33+1 weeks of gestation of her second pregnancy, a dichorionic diamniotic twin pregnancy, to our perinatal center with suspected fetal growth restriction of the first twin. The patient presented no past medical history except for the occasional use of Lorazepam (lorivan) and was a nonsmoker. She had a previous normal pregnancy followed by normal vaginal delivery. The current pregnancy was complicated by premature contractions and the patient had been previously treated with several tocolytics agents including nifedipine, indomethacin and atosiban. |
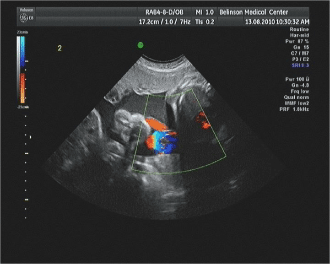
| On admission, the patient was asymptomatic, and her vital signs and physical examinations were unremarkable. Cardiotocography (CTG) demonstrated normal fetal heart rate tracings for both fetuses with no uterine contractions. On sonographic examination, weight estimations were 1769 g (34th percentile according to our national reference growth charts [5]) and 1831 g (42th percentile) for the first and second twin, respectively. There was a normal amount of amniotic fluid in both sacs and the biophysical score was 8 of 8 for both fetuses. While assessing the Doppler flow in the umbilical artery of the second twin, a focal bulging located several centimeters distal to the abdominal cord insertion of the second twin was revealed (Figure 1). On color Doppler this finding demonstrated a circular like pattern. Proximal and distal to this finding, the umbilical cord looked regular in appearance. Pulsed-wave Doppler examination revealed an intermittent absence end diastolic flow pattern in the umbilical artery of the second twin. |
| Because of the early gestational age and the evidence of fetal wellbeing, expectant management was chosen, and the patient was admitted for the purpose of antenatal corticosteroid therapy administration along with frequent fetal monitoring with CTG and sonographic evaluation. According to our departmental protocols, surveillance included biophysical profile, amniotic fluid index and non-stress test twice a day along with Doppler flow assessment (for umbilical artery and middle cerebral artery) every other day. |
| Subsequent evaluations revealed significant deterioration in the form of persistent absent end diastolic flow in the umbilical artery for the second twin (Figure 2). Following these findings, the abnormal flow patterns and the abnormal segment of the umbilical cord suspected to be true knot, cesarean delivery was conducted three days from admission. |
| Two live and vital male infants were delivered. Fetal weights were 1790 g (37th percentile) 1860 g (46th percentile) for the first and second twins, respectively. There was a true knot on the umbilical cord of the second twin. One-minute and 5-minutes Apgar scores were of 7 and 8 for both fetuses, respectively. Both neonates were discharged healthy from the hospital 3 days following delivery. |
| Discussion |
| It has been shown that true umbilical cord knots may be responsible for fetal compromise due to cord blood flow alternations. Constriction of the umbilical cord by a true knot may lead to obstruction of the fetal circulation with subsequent intrauterine growth restriction or fetal death [2]. However, in most cases, Wharton’s jelly cushions umbilical blood vessels, thus preventing disruption of flow due to compression or bending of the umbilical cord. |
| Failure to identify umbilical cord knots prenatally may be attributed to several factors. First, the umbilical cord is a complex vascular structure with different patterns of twisting and displays an erratic spatial configuration within the amniotic cavity. Second, even though early observations suggested that cord knots are formed early in gestation when the fetus is extremely mobile and there is enough amniotic fluid surrounding it, later observations suggest that the majority of knots are formed during labor [6], and thus antepartum diagnosis is not possible. |
| Various sonographic patterns have been described as characteristic of true knots, including ‘cloverleaf’ pattern [7], ‘four-leaf clover’ [4] or ‘hanging noose’ [8]. However, none of these signs is specific, and other cord complications can generate a sonographic image that can be indistinguishable from a true knot, including false knots, the presence of multiple loops of cord a small pocket of fluid, and situations in which two or more segments of the cord are in close apposition to each other [9]. In addition, the sensitivity of these findings is limited. The case described above had neither of these patterns. Recently, 3-dimensional Doppler sonography had been suggested to be helpful in the diagnosis true knots, especially in second trimester [10]. |
| In the current case, the diagnosis was made at 33 weeks’ gestation. The presence of a true knot was suspected by the presence of a bulging of an umbilical cord segment anterior to the fetal abdomen. Color Doppler sonography assisted in making the diagnosis by providing additional information on the direction of blood flow and was essential for the accurate diagnosis of the knot. The deterioration in the diastolic flow in the umbilical artery – from intermittent to persistent absence of diastolic flow - could be attributed to some degree of tightening of the true knot. Unfortunately, the placentas in our case were not sent for a pathological evaluation so other factors associated with abnormal flows were not ruled out. |
| The appropriate management of patients with a suspected true knot in the umbilical cord identified by ultrasonography during the antepartum period is unclear. Once the prenatal diagnosis of a true knot is suspected, further fetal surveillance is required, including Doppler flow velocity and fetal CTG. The optimal management of cases of true knot of the umbilical cord and abnormal flows which are diagnosed earlier during gestation is a true dilemma and should be tailored to each patient following proper patient counseling. |
| Nevertheless, our ability to diagnose antepartum problems continues to outstrip our ability to treat them. Although frustrating, it should be viewed merely as a necessary step in the evolution of diagnostic testing. |
References
- Spellacy WN, Gravem H, Fisch RO (1966) The umbilical cord complications of true knots, nuchal coils, and cords around the body. Report from the collaborative study of cerebral palsy. Am J ObstetGynecol 94: 1136-1142.
- Airas U, Heinonen S (2002) Clinical significance of true umbilical knots: a population-based analysis. Am J Perinatol 19: 127-132.
- Sherer DM, Dalloul M, Zigalo A, Bitton C, Dabiri L, et al. (2005) Power Doppler and 3-dimensional sonographic diagnosis of multiple separate true knots of the umbilical cord. J Ultrasound Med 24: 1321-1323.
- Sepulveda W, Shennan AH, Bower S, Nicolaidis P, Fisk NM (1995) True knot of the umbilical cord: a difficult prenatal ultrasonographic diagnosis. Ultrasound ObstetGynecol 5: 106-108.
- Dollberg S, Haklai Z, Mimouni FB, Gorfein I, Gordon ES (2005) Birth weight standards in the live-born population in Israel. Isr Med Assoc J 7: 311-314.
- Blickstein I, Shoham-Schwartz Z, Lancet M (1987) Predisposing factors in the formation of true knots of the umbilical cord--analysis of morphometric and perinatal data. Int J GynaecolObstet 25: 395-398.
- Collins JH (1991) First report: prenatal diagnosis of a true knot. Am J ObstetGynecol 165: 1898.
- Ramón Y Cajal CL, Martínez RO (2004) Prenatal diagnosis of true knot of the umbilical cord. Ultrasound ObstetGynecol 23: 99-100.
- Hertzberg BS, Bowie JD, Bradford WD, Bolick D (1988) False knot of the umbilical cord: sonographic appearance and differential diagnosis. J Clin Ultrasound 16: 599-602.
- Hasbun J, Alcalde JL, Sepulveda W (2007) Three-dimensional power Doppler sonography in the prenatal diagnosis of a true knot of the umbilical cord: value and limitations. J Ultrasound Med 26: 1215-1220.
Figures at a glance
 |
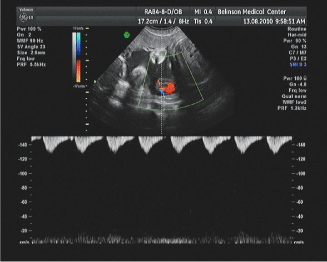 |
| Figure 1 | Figure 2 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 11848
- [From(publication date):
December-2015 - Sep 03, 2025] - Breakdown by view type
- HTML page views : 10882
- PDF downloads : 966
