Opinion Article Open Access
Prevalence of Anxiety Symptoms and it Impact in People with Osteoarthritis: An Update
Ray Marks*
Departments of Health, Physical Education & Gerontological Studies and Services, City University of New York, York College and Health and Behavior Studies, Columbia University, Teachers College, New York, USA
- *Corresponding Author:
- Ray Marks
Professor, Departments of Health, Physical Education
& Gerontological Studies and Services
City University of New York, York College and
Health and Behavior Studies, Columbia University
Teachers College, New York, USA
Tel: 1-212-678-3445
Fax: 1-212-678-8259
E-mail: rm226@columbia.edu
Received date: January 04, 2016; Accepted date: February 22, 2016; Published date: March 17, 2016
Citation: Marks R (2016) Prevalence of Anxiety Symptoms and it Impact in People with Osteoarthritis: An Update. J Ost Arth 1:110.
Copyright: © 2016 Marks R. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Osteoarthritis
Abstract
Anxiety, a very common psychological syndrome in the aging population, is a potential moderating factor in the context of disabling osteoarthritis, the most common joint disorder affecting the older population. This narrative review examines the extent to which anxiety may preside among adults with a diagnosis of osteoarthritis, regardless of site, and its linkage to the disabling process. Drawn largely from English language peer reviewed publications over the last 35 years, articles that discussed the topic of anxiety among cases with osteoarthritis were examined to demonstrate that this correlate is very important to evaluate and is amenable to treatment. Although not well represented in the vast body of literature, ample evidence implies untreated anxiety is likely to produce excess pain, and less optimal outcomes than that which is treated. It is concluded that more attention to this correlate in the clinical realm is highly desirable to offset the deleterious outcomes associated with one or more forms of anxiety, regardless of joint site, or disease duration.
Keywords
Anxiety; Disability; Osteoarthritis; Outcomes; Surgery; Treatment
Introduction
Anxiety, a state of apprehension and distress occurring in different forms, including pre-existing trait anxiety, generalized anxiety disorder, and state anxiety is widespread among adults in general, as well as adults with a variety of health conditions [1-4]. Commonly affecting the individual’s physical, functional, and social well-being, as well as their overall health status and life quality significantly and adversely [5], it is our view that the presence of this condition is often overlooked in general among the aging adult population. Moreover, we believe this mental correlate does not receive the same attention as those physical correlates that accompany the disabling long-term health condition known as osteoarthritis, an irreversible chronically painful destructive musculoskeletal condition of one or more joints (Table 1 and Table 2). This brief was designed to update the extent to which anxiety has been observed to prevail in cases diagnosed as having osteoarthritis, the impact of anxiety in the context of osteoarthritis, and the implications of this information in the context of optimizing outcomes for adults with osteoarthritis, and for reducing the immense overall burden associated with osteoarthritis.
| S.No | Sites that can be affected by osteoarthritis |
|---|---|
| 1 | Neck |
| 2 | Low back |
| 3 | Knee |
| 4 | Hip |
| 5 | Hands |
| 6 | Ankles |
| 7 | Knee + hip |
| 8 | Knee + hand |
| 9 | Hip + hand |
| 10 | Knee + hip + hand |
| 11 | Acromioclavicular joint |
| 12 | Shoulder |
| 13 | Elbow |
| 14 | Wrist |
| 15 | Thumb |
| 16 | Jaw |
Table 1: Sites that can be affected by osteoarthritis.
| S.No | Symptoms |
|---|---|
| 1 | Anxiety |
| 2 | Body image distortions |
| 3 | Bone crepitus on movement |
| 4 | Depression |
| 5 | Functional Limitations |
| 6 | Impaired joint Range of Motion |
| 7 | Inflammation |
| 8 | Joint deformity |
| 9 | Joint hypertrophy |
| 10 | Joint laxity |
| 11 | Muscle atrophy |
| 12 | Muscle weakness |
| 13 | Obesity |
| 14 | Pain, aching and/or swelling |
| 15 | Poor proprioception |
| 16 | Poor self-efficacy |
| 17 | Postural problems |
| 18 | Reduced fitness |
| 19 | Sleep problems |
| 20 | Social functioning impaired |
| 21 | Stiffness |
| 22 | Work Disability |
Table 2: Typical symptoms experienced by adults with osteoarthritis, a chronic disabling musculoskeletal health condition.
Methods
To provide a comprehensive understanding of this topic, we focused on retrieving all relevant papers published between 1980 and Jan 2016 in the major data bases. To explore to what degree anxiety is likely to prevail in osteoarthritis, we specifically sought clinical studies that addressed this question in some way, regardless of instrument used. To ascertain the possible impact of anxiety on health status and/or health outcomes among people with osteoarthritis we examined correlational or prospective studies that embedded some related details in this respect.
To this end, we sought and utilized reports embedded in the Academic Search Complete, PubMed, Scopus, Web of Science, Science Citation Index, and PsychInfo data bases using the key words, anxiety and osteoarthritis.
Only English language peer reviewed publications were deemed acceptable and all selected papers had to focus on osteoarthritis patients, rather than other forms of rheumatic disease. The key findings were categorized into three key topics: those examining the presence of anxiety in the context of osteoarthritis, the impact of anxiety on osteoarthritis disability, and the implications of these findings. No meta-analyses were conducted due to the limited number of publications in this realm, and papers retrieved were not constrained to any stage of the disease process, such as pre or postsurgical anxiety observations. All research articles that addressed one or more of the topics of interest were first carefully examined, and only included in a related narrative if they provided information on prevalence, disease severity, and/or treatment implications.
Results
Over the course of time, when utilizing the key words anxiety and osteoarthritis, the numbers of studies located in: Academic Search Complete were 139, CINAHL-117, PsychInfo had 137 articles listed, Science Citation Index cited 308 items, Web of Science listed 371 items, Scopus listed 851 items, and numbers in PubMed as of Jan 30, 2016 were 348 [equal to only 5 % of all osteoarthritis publications]. Types of studies included: cross-sectional clinical studies, presurgical, postsurgical treatment, and rehabilitation studies. Joints studied included the hip, knee, hand, and temporomandibular joints, but many papers on osteoarthritis were not related in any way to the present topic. The Hospital Anxiety and Depressions [HAD-A] and Spielberger Anxiety Scales were most commonly used, even though these do not prove anxiety is clinically present.
Prevalence Findings
In terms of identifying whether anxiety in any form is a consistent correlate among people suffering with definitive osteoarthritis, we found no major study has specifically sought to estimate anxiety in a large cohort of well-defined osteoarthritis sufferers. Most studies that have attempted to provide information on this correlate were limited in size and the primary purpose was generally to examine osteoarthritis in general, or anxiety as a correlate of pain or function. Despite the paucity of studies on this present topic, when compared to studies on depression, and especially to other commonly measured osteoarthritis correlates such as obesity [see Box 2] one can potentially expect approximately one quarter of adults with painful osteoarthritis to present with some form of anxiety, as outlined by Castano et al. [5] and Stubbs et al. [6]. This former group found anxiety to occur at high rates of 24.7% among a cohort of 1258 cases, and the latter group indicated that almost 20% of cases with osteoarthritis have anxiety symptoms. In an earlier study, Axelrod et al. [7] found that among 54 patients with osteoarthritis, the majority of whom were women, the prevalence of clinically significant anxiety and/or depression was 40.7%. Marks [8] showed approximately nine percent (92 cases) of 1000 disabled hip osteoarthritis cases awaiting surgery had a prior mental health disorder, and among these patients, 5.5% (44 cases) reported trait anxiety histories, alone or in combination with trait depression. Among the 112 cases reporting either the presence of trait and/or state anxiety, nine cases reported both knee osteoarthritis of these conditions and a further nine with depression histories reported state anxiety. However, most of the 90 cases experiencing state anxiety had no prior anxiety history. Memel et al. [9] found 24.4% of patients with osteoarthritis exhibited anxiety in some form, which the general practitioner did not always recognize, and more recently Wong et al. [10] found a high prevalence of psychiatric morbidity, including anxiety among cases with knee osteoarthritis visiting an orthopedic clinic. Most of these data concur with findings of Perrot et al. [11] who observed many patients with either hip or knee osteoarthritis had mild anxiety as recorded using the HADS.
Unsurprisingly, Duivenvoorden et al. [12] who examined a sub-set of total hip or knee arthroplasty patients found high anxiety prevalence preoperatively. Moreover, those with preoperative anxiety had worse patient reported outcomes at 3 and 12 months after surgery and these patients were less satisfied than those with no anxiety. Thus, even though anxiety prevalence may vary, depending on nature of sample, the instrument used to assess this, the type of anxiety present, and the overall osteoarthritis disease and health status, most available studies exemplify the negative role anxiety might play in the disabling process of osteoarthritis. For example, in a study of osteoarthritis cases, even though Hayashi et al. [13] found a low rate of anxiety in their cohort study, anxiety was a negative disease correlate. Rates were also low in the study by Hsieh et al, [14] although as outlined by this group, pain is generally associated with increased psychological distress. Many, if not the majority of published studies on the clinical presentation of the adult with osteoarthritis have not measured or reported on anxiety however, or if they have, they have measured this alongside depression and reported this as a mental health variable, the samples have often been highly heterogeneous, the measurement tools inconsistent, not all joints have been studied, and hence the data and their results are clearly limited in their generalizability, at present. They may also be underestimates of the presence of anxiety in osteoarthritis in general, as most surgical studies until recently did not examine this correlate. Most studies too are only indicators of anxiety symptoms, and are not based on confirmatory clinical diagnoses.
Impact
The fact that anxiety may be more common than not among cases with osteoarthritis is important to consider given that anxiety has been observed to be associated with more severe pain and less than optimal functional assessments [15-18]. Hayishi et al. [13] too noted anxiety related responses to pain were significant correlating factors for gait speeds, in patients with osteoarthritis of lower limbs, while Ozcetin et al. [19] found anxiety impacted overall function among knee osteoarthritis cases.
Blackburn et al. [20] in examining the influence of preoperative anxiety on satisfaction after total knee replacement similarly found a positive correlation between preoperative anxiety and levels of knee disability, as did Summers et al. [21] who examined cases of primary hip or knee osteoarthritis using outpatient department computer lists. Similarly, a more recent paper by Wise et al. [22] revealed a strong association between worsened measures of mental health and pain and risk of pain flares.
Likewise, McHugh et al. [23] who examined predictors of outcomes of recovery following total hip replacement surgery found anxiety was a significant factor influencing the degree of recovery.
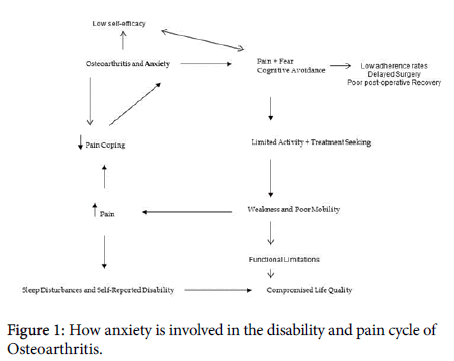
As outlined above, the presence of anxiety, while not always assessed or considered as a component of osteoarthritis disability, is a potentially highly important independent determinant of the disease severity and outcomes such as pain, function, and life quality [24], as well as functional declines [25] (Table 3 and Figure 1).
| Authors | Study approach | Key results |
|---|---|---|
| Axford et al. [7] | 54 cases with lower limb OA were studied | Anxiety is common in OA and is related to pain and disability |
| Badel et al. [26] | 16 patients with temporo mandibular joint OA 20 controls | Patients with chronic pain had high anxiety levels before treatment |
| Badura-Brzoza et al. [27] | Longitudinal study of 103 cases undergoing hip replacement surgery for primary OA | Total hip replacement outcomes are influenced by trait anxiety |
| Blackburn et al.[20] | 40 knee arthroplasty patients | The severity of preoperative anxiety and depression was associated with higher levels of knee disability (coefficient = 0.409; p = 0.009). |
| Chen et al. [28] | Cross sectional study of 192 out patients | Key predictors of sleep were high anxiety levels |
| Creamer et al. [29] | Cross-sectional study of 69 knee OA cases | Disability was associated with anxiety |
| Eliis et al. [30] | 154 indigent patients undergoing total knee | 11% has pre surgical anxiety arthroplasty Anxious patients reported lower patient perceived outcome scores at 1 year |
| Ferreira et al. [24] | 40 women with knee OA; 25 controls | Women with OA have higher anxiety rates than women with no OA |
| French et al. [18] | 1010 hip OA cases after treatment | Anxiety was predictive of a positive outcome at 9 weeks |
| Fujita et al. [31] | Qualitative report related to hip surgery for OA | Some patients expressed anxiety over limited mobility, body image and prosthesis |
| Hernandez et al. [32] | Systematic review of 37 studies | Anxiety influences post op. pain |
| Hirshman et al. [33] | 104 knee OA cases undergoing surgery were studied | Patients with higher state and trait anxiety had worse function before and after surgery |
| Jacobs et al. [34] | 1020 knee OA surgeries followed for 2 years | 41.9% of less severe cases, reported anxiety, and were more dissatisfied than more severe cases |
| McHugh et al. [23] | 206 patients awaiting hip arthroplasty | Anxiety influenced recovery at 6m |
| Montin et al. [35] | Longitudinal study hip OA cases before + after surgery | Pre-operative trait anxiety predicted health quality of life before and after surgery |
| Pinto et al. [17] | 92 total hip and knee arthroplasty patients | Anxiety at 4-6 months was a predictor of persistent post-surgical pain |
| Salmon et al. [36] | Longitudinal study of 102 cases undergoing hip replacement surgery | Recovery at follow-up was slower in those with greater anxiety |
| Scopaz et al. [37] | 182 cases with knee OA | Higher anxiety scores rates were associated with worse function scores |
| Sinikallio et al. [38] | Examined 111 cases of OA, 35-75 years with knee OA | Negative emotions impact pain and disability |
| Smith and Zautra, [39] | 88 cases of women with OA | Anxiety was related to elevations in current and future pain at twice the rate for depression |
| Wong et al. [10] | 115 knee OA cases | Anxiety was found in 24% cases |
Table 3: Selected findings in the available literature linking anxiety to adverse clinical and surgical outcomes over the past 15 years; OA: Osteoarthritis.
Discussion and Conclusion
As outlined above, people with osteoarthritis may exhibit various degrees of anxiety, an important mental health symptom, at all stages of the disease process. Moreover, the presence of anxiety in any form clearly heightens pain and disability levels, while retarding short term and long term outcomes, including optimal recovery rates after conservative, as well as surgical interventions. Pain and disability in turn, may invoke anxiety, increased fear, and a spiral of adverse functional outcomes. Not surprisingly, Davis et al. [40] who examined the associations of various health indicators and the psychological well-being of adults with and without radiographic knee osteoarthritis found self-reported knee pain correlated significantly with the presence of psychological distress, rather than visible joint destruction. Similarly Van Baar et al. [41] found that after controlling for other characteristics, the psychological characteristics of patients with osteoarthritis, such as anxiety, contributed as much as the more traditional kinesiological measures to the patient’s disability. A related prospective study by Dieppe et al. [42] found adults with osteoarthritis examined over an eight year period generally had a poor outcome with high levels of physical disability, as well as anxiety, especially if they had knee osteoarthritis. In addition, anxiety can clearly heighten osteoarthritis disability, while lowering quality of life [19,43,44], and can slow the post-operative recovery process [17] quite considerably.
Consequently, efforts to routinely examine both the physical as well as the mental health status of this patient group followed by tailored and targeted interventions with periodic follow-up visits to re-examine levels of anxiety are strongly indicated for decreasing the osteoarthritis burden as outlined by Montin et al. [35]. That is, despite the problems in the reported literature, and lack of depth, the possibility that anxiety is an important element in the disease process should not be ignored and appears highly worthy of attention in the clinic and surgical setting to offset the adverse impact of anxiety on health status and intervention efforts [45].
Among those who recognize this imperative, Vrizekolk et al. [46] stress the importance of examining and diagnosing the presence of an anxiety related syndrome among cases with osteoarthritis, as well as among the general primary care population of adults. Hill et al. [47] too emphasized that physicians need to recognize as well as address the significant additional negative impact anxiety can render on the patients’ physical well-being, while Dorr and Chao [48] advocated for appropriate pre-operative education to allay any unwarranted negative impact attributable to anxiety. For Ferreira et al. [24] the treatment of patients with osteoarthritis should thus include a combination of pharmacotherapy, psychotherapy, counselling and family support, given the high percentage of people with osteoarthritis who may be experiencing anxiety symptoms [6].
Other available treatment options include guided imagery [35] the application of video technology [49] pharmacologic interventions [50] well designed pre-operative education [51] anxiety management approaches [52] social rehabilitation [53] Cognitive Behavioral Therapy [54] and a patient-centered approach [45]. Those with trait anxiety histories who may also experience state anxiety [46], those who are overweight, those with excessively high anxiety levels [55] as well as those with multiple morbidities, and those living within an indigent population [30] should be specially assessed to minimize adverse outcomes. These include, but are not limited to: a slower recovery rate after surgery [36] high current and future pain levels [35,39,56], disability scores [57] slower walking speeds [13], distress over body image following surgery [31] post-operative pain and lower perceived self-efficacy [58] and life quality [59] reduced patient satisfaction after total hip or knee replacement surgery [33,60] and revision surgery [61] and distress in general [45]. Screening as a routine practice, followed by carefully tailored and targeted interventions that take into account the diagnostic category of anxiety, as well as the overall coping mechanisms of the patient, plus the degree of distress exhibited is hence of key importance in clinical and surgical settings in efforts to offset the complex adverse associations depicted in figure 1. Accordingly, Rolfson et al. [60] stated surgeons need to be aware of the ramifications of mental health concerns that may influence post-operative pain and outcomes after arthroplasty surgery. In agreement, Ellis advocate patients awaiting surgery be routinely assessed and the impact of any observed anxiety or distress and its negative effect on surgical outcomes should be discussed with patient prior to surgery [30].
As well, since anxiety may complicate the post-operative recovery process, patients exhibiting anxiety during hospitalization might benefit from appropriate treatment and follow-up [62]. Possible instruments that have been used successfully to assess the presence of anxiety in people with osteoarthritis are the: Hospital Anxiety and Depression Scale [HADS] [16-18,63,64]; Pain Anxiety Symptoms Scale [PASS] [64,65]; Beck Anxiety Inventory [19,66].
The State Trait anxiety Inventory [67] and integrated service delivery efforts to detect and treat Anxiety in this group may provide more timely and efficacious osteoarthritis outcomes, rather than adverse outcomes and prognoses of this widespread disabling condition [68].
References
- Fava GA, Porcelli P, Rafanelli C, Mangelli L, Grandi S (2010) The spectrum of anxiety disorders in the medically ill. J Clin Psychiatry 71: 910-914.
- Sareen J, Jacobi F, Cox BJ, Belik SL, Clara I, et al. (2006) Disability and poor quality of life associated with comorbid anxiety disorders and physical conditions. Arch Intern Med 166: 2109-2116.
- Scott KM, Bruffaerts R, Tsang A, Ormel J, Alonso J, et al. (2007) Depression-anxiety relationships with chronic physical conditions: results from the World Mental Health Surveys. J Affect Disord 103: 113-120.
- Burns MN, Siddique J, Fokuo JK, Mohr DC (2010) Comorbid anxiety disorders and treatment of depression in people with multiple sclerosis. RehabilPsychol 55: 255-262.
- CastañoCarou A, Pita Fernández S, PértegaDíaz S, de Toro Santos FJ4 (2015) Clinical profile, level of affection and therapeutic management of patients with osteoarthritis in primary care: The Spanish multicenter study EVALÚA. ReumatolClin 11: 353-360.
- Stubbs B, Aluko Y, Myint PK, Smith TO4 (2016) Prevalence of depressive symptoms and anxiety in osteoarthritis: a systematic review and meta-analysis. Age Ageing 45: 228-235.
- Axford J, Butt A, Heron C, Hammond J, Morgan J, et al. (2010) Prevalence of anxiety and depression in osteoarthritis: use of the Hospital Anxiety and Depression Scale as a screening tool. ClinRheumatol 29: 1277-1283.
- Marks R1 (2009) Comorbid depression and anxiety impact hip osteoarthritis disability. Disabil Health J 2: 27-35.
- Memel DS, Kirwan JR, Sharp DJ, Hehir M (2000) General practitioners miss disability and anxiety as well as depression in their patients with osteoarthritis. Br J Gen Pract 15: 645-648.
- Wong LY, Yiu RL, Chiu CK, Lee WK, Lee YL, et al. (2015) Prevalence of Psychiatric Morbidity in Chinese Subjects with Knee Osteoarthritis in a Hong Kong Orthopaedic Clinic. East Asian Arch Psychiatry 25: 150-158.
- Perrot S, Rozenberg S, Moyse D, Legout V, Marty M; cercled'étude de douleur en rhumatologie (CEDR) (2011) Comparison of daily, weekly or monthly pain assessments in hip and knee osteoarthritis. A 29-day prospective study. Joint Bone Spine 78: 510-515.
- Duivenvoorden T, Vissers MM, Verhaar JA, Busschbach JJ, Gosens T, et al. (2013) Anxiety and depressive symptoms before and after total hip and knee arthroplasty: a prospective multicentre study. Osteoarthritis Cartilage 21: 1834-1840.
- Hayashi K, Kako M, Suzuki K, Hattori K, Fukuyasu S, et al. (2015) Gait Speeds Associated with Anxiety Responses to Pain in Osteoarthritis Patients. Pain Med .
- Hsieh RL, Lee WC, Lo MT, Liao WC (2013) Postural stability in patients with knee osteoarthritis: comparison with controls and evaluation of relationships between postural stability scores and International Classification of Functioning, Disability and Health components. Arch Phys Med Rehabil 94: 340-346.
- Zambon S, Siviero P, Denkinger M, Limongi F, Castell MV, et al. (2015) Osteoarthritis, comorbidity and pain: Their role in determining functional limitations in older populations (European project on Osteoarthritis). Arthritis Care Res (Hoboken).
- Hanusch BC, O'Connor DB, Ions P, Scott A, Gregg PJ (2014) Effects of psychological distress and perceptions of illness on recovery from total knee replacement. Bone Joint J 96-96B: 210-6.
- Pinto PR, McIntyre T, Ferrero R, Almeida A, Araújo-Soares V (2013) Risk factors for moderate and severe persistent pain in patients undergoing total knee and hip arthroplasty: a prospective predictive study. PLoS One 8: e73917.
- French HP, Galvin R, Cusack T, McCarthy GM (2014) Predictors of short-term outcome to exercise and manual therapy for people with hip osteoarthritis. PhysTher 94: 31-39.
- Ozcetin A, Ataoglu S, Kocer E, Yazici S, Yildiz O, et al. (2007) Effects of depression and anxiety on quality of life of patients with rheumatoid arthritis, knee osteoarthritis and fibromyalgia syndrome. West Indian Med J 56: 122-129.
- Blackburn J, Qureshi A, Amirfeyz R, Bannister G (2012) Does preoperative anxiety and depression predict satisfaction after total knee replacement? Knee 19: 522-524.
- Summers MN, Haley WE, Reveille JD, Alarcón GS (1988) Radiographic assessment and psychologic variables as predictors of pain and functional impairment in osteoarthritis of the knee or hip. Arthritis Rheum 31: 204-209.
- Wise BL, Niu J, Zhang Y, Wang N, Jordan JM, et al. (2010) Psychological factors and their relation to osteoarthritis pain. Osteoarthritis Cartilage 18: 883-887.
- McHugh GA, Campbell M, Luker KA (2013) Predictors of outcomes of recovery following total hip replacement surgery: A prospective study. Bone Joint Res 2: 248-254.
- Ferreira AH, Godoy PB, Oliveira NR, Diniz RA, Diniz RE, et al. (2015) Investigation of depression, anxiety and quality of life in patients with knee osteoarthritis: a comparative study. Rev Bras Reumatol 55: 434-438.
- Dekker J, van Dijk GM, Veenhof C (2009) Risk factors for functional decline in osteoarthritis of the hip or knee. CurrOpinRheumatol 21: 520-524.
- Badel T, Lovko SK, Podoreski D, Pavcin IS, Kern J (2011) Anxiety, splint treatment and clinical characteristics of patients with osteoarthritis of temporomandibular joint and dental students-a pilot study. Med Glas (Zenica) 8: 60-63.
- Badura-Brzoza K, Zajac P, Brzoza Z, Kasperska-Zajac A, Matysiakiewicz J, et al. (2009) Psychological and psychiatric factors related to health-related quality of life after total hip replacement-preliminary report. European Psychiatry 24: 119-124.
- Chen CJ, McHugh G, Campbell M, Luker K (2014) Subjective and Objective Sleep Quality in Individuals with Osteoarthritis in Taiwan. Musculoskeletal Care.
- Creamer P, Lethbridge-Cejku M, Hochberg MC (2000) Factors associated with functional impairment in symptomatic knee osteoarthritis. Rheumatology (Oxford) 39: 490-496.
- Ellis HB, Howard KJ, Khaleel MA, Bucholz R (2012) Effect of psychopathology on patient-perceived outcomes of total knee arthroplasty within an indigent population. J Bone Joint Surg Am 94: e84.
- Fujita K, Makimoto K, Hotokebuchi T (2006) Qualitative study of osteoarthritis patients' experience before and after total hip arthroplasty in Japan. Nurs Health Sci 8: 81-87.
- Hernández C, Díaz-Heredia J, Berraquero ML, Crespo P, Loza E, et al. (2015) Pre-operative Predictive Factors of Post-operative Pain in Patients With Hip or Knee Arthroplasty: A Systematic Review. ReumatolClin 11: 361-380.
- Hirschmann MT, Testa E, Amsler F, Friederich NF (2013) The unhappy total knee arthroplasty (TKA) patient: higher WOMAC and lower KSS in depressed patients prior and after TKA. Knee Surg Sports TraumatolArthrosc 21: 2405-2411.
- Jacobs CA, Christensen CP, Karthikeyan T (2015) Chronic non-orthopedic conditions more common in patients with less severe degenerative changes that have elected to undergo total knee arthroplasty. J Arthroplasty 30:1146-9.
- Montin L, Leino-Kilpi H, Katajisto J, Lepistö J, Kettunen J, et al. (2007) Anxiety and health-related quality of life of patients undergoing total hip arthroplasty for osteoarthritis. Chronic Illn 3: 219-227.
- Salmon P, Hall GM, Peerbhoy D (2001) Influence of the emotional response to surgery on functional recovery during 6 months after hip arthroplasty. J Behav Med 24: 489-502.
- Scopaz KA, Piva SR, Wisniewski S, Fitzgerald GK (2009) Relationships of fear, anxiety, and depression with physical function in patients with knee osteoarthritis. Arch Phys Med Rehabil 90: 1866-1873.
- SinikallioSH, Helminen EE, Valjakka AL, Väisänen-Rouvali RH, Arokoski JP (2014) Multiple psychological factors are associated with poorer functioning in a sample of community-dwelling knee osteoarthritis patients. J ClinRheumatol 20: 261-267.
- Smith BW, Zautra AJ (2008) The effects of anxiety and depression on weekly pain in women with arthritis. Pain 138: 354-361.
- Davis MA, Ettinger WH, Neuhaus JM, Barclay JD, Segal MR (1992) Correlates of knee pain among US adults with and without radiographic knee osteoarthritis. J Rheumatol 19: 1943-1949.
- van Baar ME, Dekker J, Lemmens JA, Oostendorp RA, Bijlsma JW (1998) Pain and disability in patients with osteoarthritis of hip or knee: the relationship with articular, kinesiological, and psychological characteristics. J Rheumatol 25: 125-133.
- Dieppe P, Cushnaghan J, Tucker M, Browning S, Shepstone L (2000) The Bristol 'OA500 study': progression and impact of the disease after 8 years. Osteoarthritis Cartilage 8: 63-68.
- Liu R, Damman W, Beaart-van de Voorde L, Kaptein AA, Rosendaal FR, et al. (2015) Aesthetic dissatisfaction in patients with hand osteoarthritis and its impact on daily life. Scand J Rheumatol .
- Wang J, Howard K, McAdams W, Bucholz R (2014) Evaluating the effects of anxiety disorder on physical and psychosocial measures for indigent patients with severe lower extremity osteoarthritis. Current Orthopaedic Practice 25: 158-163.
- Tallon D, Chard J, Dieppe P (2000) Exploring the priorities of patients with osteoarthritis of the knee. Arthritis Care Res 13: 312-319.
- Vriezekol J, Eijsbouts A, Evers A, Stenger A, Van Den Hoogen F, et al. (2010) Poor psychological health status among patients with inflammatory rheumatic diseases and osteoarthritis in multidisciplinary rehabilitation: need for a routine psychological assessment. DisabilRehabil 32: 836-844.
- Hill CL, Gill T, Taylor AW, Daly A, Grande ED, et al. (2007) Psychological factors and quality of life in arthritis: a population-based study. ClinRheumatol 26: 1049-1054.
- Dorr LD, Chao L (2007) The emotional state of the patient after total hip and knee arthroplasty. ClinOrthopRelat Res 463: 7-12.
- Ayral X, Gicquere C, Duhalde A, Boucheny D, Dougados M (2002) Effects of video information on preoperative anxiety level and tolerability of joint lavage in knee osteoarthritis. Arthritis Rheum 47: 380-382.
- Wu LR, Parkerson GR Jr, Doraiswamy PM (2002) Health perception, pain, and disability as correlates of anxiety and depression symptoms in primary care patients. J Am Board FamPract 15: 183-190.
- Giraudet-Le Quintrec JS, Coste J, Vastel L, Pacault V, Jeanne L, et al. (2003) Positive effect of patient education for hip surgery: a randomized trial. ClinOrthopRelat Res : 112-120.
- Feeney SL (2004) The relationship between pain and negative affect in older adults: anxiety as a predictor of pain. J Anxiety Disord 18: 733-744.
- Badura-Brzoza K. Zajac P, Kasperska-Zajac A, Brzoza Z, Matysiakiewicz J, et al. (2008) Anxiety and depression and their influence on the quality of life after total hip replacement: preliminary report. Int J Psychiatry ClinPract 12: 280-284.
- Davis L, Barlow DH, Smith L (2010) Comorbidity and the treatment of principal anxiety disorders in a naturalistic sample. BehavTher 41: 296-305.
- Daltroy LH, Morlino CI, Eaton HM, Poss R, Liang MH (1998) Preoperative education for total hip and knee replacement patients. Arthritis Care Res 11: 469-478.
- Wesseling J, Welsing PM, Bierma-Zeinstra SM, Dekker J, Gorter KJ, et al. (2013) Impact of self-reported comorbidity on physical and mental health status in early symptomatic osteoarthritis: the CHECK (Cohort Hip and Cohort Knee) study. Rheumatology (Oxford) 52: 180-188.
- Salaffi F, Cavalieri F, Nolli M, Ferraccioli G (1991) Analysis of disability in knee osteoarthritis. Relationship with age and psychological variables but not with radiographic score. J Rheumatol 18: 1581-1586.
- Wylde V, Dixon S, Blom AW (2012) The role of preoperative self-efficacy in predicting outcome after total knee replacement. Musculoskeletal Care 10: 110-118.
- Qi A, Lin C, Zhou A, Du J, Jia X, et al. (2016) Negative emotions affect postoperative scores for evaluating functional knee recovery and quality of life after total knee replacement. Brazilian Journal of Medical and Biological Research 49: e4616.
- Rolfson O, Dahlberg LE, Nilsson JA, Malchau H, Garellick G (2009) Variables determining outcome in total hip replacement surgery. J Bone Joint Surg Br 91: 157-161.
- Liddle AD, Judge A, Pandit H, Murray DW4 (2014) Determinants of revision and functional outcome following unicompartmental knee replacement. Osteoarthritis Cartilage 22: 1241-1250.
- Sveinsdóttir H, Skúladóttir H (2012) Postoperative psychological distress in patients having total hip or knee replacements: an exploratory panel study. OrthopNurs 31: 302-311.
- Rivard V, Cappeliez P (2007) Perceived control and coping in women faced with activity restriction due to osteoarthritis: relations to anxious and depressive symptoms. Can J Aging 26: 241-254.
- Ayob S, Ryan CG, Cormac G, Martin DJ (2013) The role of pain related anxiety in the functioning of patients white knee osteoarthritis in Malaysia. Journal of the Physiotherapy Pain Association 34: 25-29.
- Lavernia CJ, Alcerro JC, Rossi MD (2010) Fear in arthroplasty surgery: the role of race. ClinOrthopRelat Res 468: 547-554.
- Fitzgerald G, White D, Piva S (2012) Associations for change in physical and psychological factors and treatment response following exercise in knee osteoarthritis: An exploratory study. Arthritis Care Res (Hoboken) 64: 1673-1680.
- Finan P, Buenaver L, Smith M, et al. (2013) Discordance between pain and radiographic severity in knee osteoarthritis: Findings from quantitative sensory testing of central sensitization. Arthritis Rheum 65: 363-372.
- Tan V, Jinks C, Chew-Graham C, Healey EL, Mallen C (2015) The triple whammy anxiety depression and osteoarthritis in long-term conditions. BMC FamPract 16: 163.
--
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 12783
- [From(publication date):
August-2016 - Sep 03, 2025] - Breakdown by view type
- HTML page views : 11899
- PDF downloads : 884