Case Report Open Access
Primary Cutaneous Squamous Cell Carcinoma of Thigh A Case Report and Review of Literature
Vishwas D. Pai1*, Sushma V. Pai2, Vidhya Manohar3, Suvarna Ravindranath3 and Mahantesh. K. Math4
1Department of Surgical Oncology, Kerudi Cancer Hospital and Research Centre, Bagalkot 587101, Karnataka, India
2Department of Anesthesiology and Critical care, Kerudi Cancer Hospital and Research Centre, Bagalkot 587101, Karnataka, India
3Department of Pathology, SRL Diagnostics, Banagalore 560076, Karnataka, India
4Department of Plastic Surgery, Kerudi Cancer Hospital and Research Centre, Bagalkot 587101, Karnataka, India
- *Corresponding Author:
- Vishwas. D. Pai
Department of Surgical Oncology
Kerudi Cancer Hospital and Research Centre
Bagalkot 587101, Karnataka, India
Tel: +91-9449333502
E-mail: vishpai88@gmail.com
Received Date: January 20, 2016; Accepted Date: February 04, 2016; Published Date: February 12, 2016
Citation: Pai VD, Pai SV, Manohar V, Ravindranath S, Math MK (2016) Primary Cutaneous Squamous Cell Carcinoma of Thigh – A Case Report and Review of Literature. J Orthop Oncol 2:106. doi:10.4172/2472-016X.1000106
Copyright: © 2016 Pai VD, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Orthopedic Oncology
Abstract
Squamous cell carcinomas (SCC) are second most common cutaneous malignancy. Exposure to ultraviolet rays remains the single most important etiological factor. Although SCC can arise in unexposed areas these are typically associated with long standing ulcers and sinuses or immunosuppression. There are no randomized controlled trials on primary cutaneous SCC in general and in these rare subsites in particular. There is no consensus on the management of these tumours particularly the role of prophylactic lymph node dissection and role of adjuvant radiotherapy. The purpose of reporting this case is to critically review the literature for the current evidence for the management of primary cutaneous squamous cell carcinoma.
Keywords
Squamous cell carcinoma; Skin malignancies; Non melanoma skin cancer
Introduction
Squamous cell carcinoma (SCC) is the second most common cutaneous malignancy [1,2]. Its occurrence is related to the exposure of ultraviolet radiation and hence is more common in fair individuals and on those parts of the body which are exposed to sunlight [3]. SCC can also arise within burns, scars, chronic ulcers or sinus tracts and from pre-existing lesions such as Bowen’s disease as well in those with compromised immune status [4-6]. Squamous cell carcinoma occurring on the intact skin in non sun exposed area in immunocompetent individuals is considered extremely rare. There is no consensus on the management or prognosis of these subgroups of tumours owing to their rarity.
Case Report
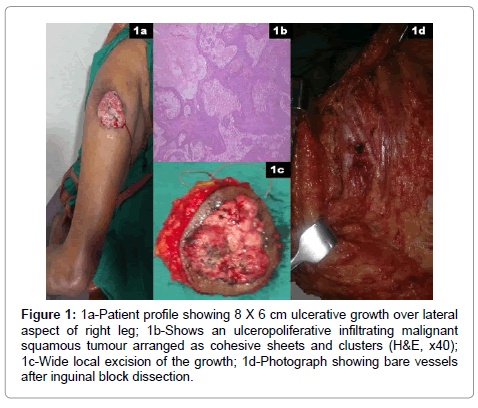
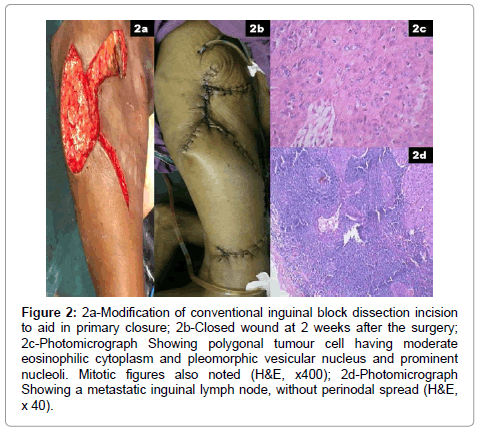
A 78 year old lady presented with history of an ulcer over right thigh of 6 months duration. She had no prior history of trauma or burns or long standing ulcer over the affected area. On examination, she had an ulcer with everted edges of size 8 × 6 cm lateral aspect of upper portion of right thigh (Figure 1a). She also had multiple, hard nodes in right inguinal area, largest being 2 × 1cm in size. Biopsy of the growth confirmed it as squamous cell carcinoma (Figure 1b). FNAC of the groin nodes demonstrated metastatic deposits of squamous cell carcinoma. Contrast enhanced computed tomography (CECT) of the pelvis demonstrated enlarged inguinal nodes but no pelvic lymphadenopathy. Metastatic work up confirmed absence of distant metastasis. Wide local excision of the ulcer with right sided complete ilio inguinal block dissection was performed after informed, written consent from the patient (Figure 1c and 1d). Incision was modified so that both primary tumour as well as the nodal dissection can be performed through the same incision while avoiding local or free flaps for reconstruction (Figure 2a and 2b). Her intra and post-operative course was uneventful. Final histopathological examination confirmed the primary tumour as squamous cell carcinoma (Figure 2c). All the resection margins including the base were free with lateral margin being closest (0.8 cm from the tumour). Four nodes in the groin showed metastatic deposits of squamous cell carcinoma however without perinodal extension (Figure 2d). Post operatively she received adjuvant radiotherapy.
Figure 1: 1a-Patient profile showing 8 X 6 cm ulcerative growth over lateral aspect of right leg; 1b-Shows an ulceropoliferative infiltrating malignant squamous tumour arranged as cohesive sheets and clusters (H&E, x40); 1c-Wide local excision of the growth; 1d-Photograph showing bare vessels after inguinal block dissection.
Figure 2: 2a-Modification of conventional inguinal block dissection incision to aid in primary closure; 2b-Closed wound at 2 weeks after the surgery; 2c-Photomicrograph Showing polygonal tumour cell having moderate eosinophilic cytoplasm and pleomorphic vesicular nucleus and prominent nucleoli. Mitotic figures also noted (H&E, x400); 2d-Photomicrograph Showing a metastatic inguinal lymph node, without perinodal spread (H&E, x 40).
Discussion
Primary cutaneous SCC is a malignant tumour which arises from the keratinizing cells of the epidermis or its appendages. It is the 2nd most common skin malignancy accounting for 25% of cutaneous cancer related deaths annually worldwide [1,2]. Incidence of SCC is rising in many countries across the globe [7]. Chronic exposure to ultra violet light remains the single most important risk factor for development of these malignancies. Hence individuals with fair skin, those with inherited disorders like albinism and Xeroderma pigmentosum particularly at higher risk for developing cutaneous SCC [3]. SCC can also arise within long standing ulcers , sinuses, burns as well as scars [4,5]. Bowen’s disease is considered to be a precursor for the development of SCC. Individuals with impaired immunity as well as those on chronic immunosuppressive drugs at particularly high risk for the development of SCC [6]. SCC developing on intact skin in the absence of any of the above mentioned risk factors is considered extremely rare.
SCC presents as a non-healing ulcer or as an indurated, nodular, keratinizing tumour. SCC typically spreads first to regional lymph nodes prior to the development of distant metastases. Diagnosis is established by an incisional biopsy. Metastatic work up includes Ultrasound examination of the regional nodal basin and chest radiograph to rule out metastasis to lungs.
Prognostic factors of SCC include anatomical site, size, tumour thickness, level of invasion, rate of growth, etiology, degree of histological differentiation and host immunosuppression [7–10]. SCC arising from the lip, non sun exposed areas such as heels, perineum and those arising from chronic ulcers are considered as high risk lesions whereas the rest of the subsites are considered as low risk lesions [7]. Tumours diameter greater than 2 cm, thickness more than 4 mm, extension into subcutaneous fat and poorly differentiated histology are considered as high risk features associated with risk of recurrence [8-10].
Surgical excision is the mainstay of treatment for the majority of cutaneous SCC. Tumour free margin of 4-mm is appropriate for clinically well-defined, low risk tumours less than 2 cm in diameter. A wider margin (6 mm or more) is essential for tumours more than 2 cm in diameter, tumours with moderately, poorly differentiated histology and tumours extending into the subcutaneous tissue [11]. Mohs’ micrographic surgery is an attractive alternative particularly in high risk cases as it allows histological confirmation of complete resection of the tumour with minimal loss of normal tissue [12,13].
Management of regional nodes in cases of cutaneous SCC is a topic of debate at present. Therapeutic lymph node dissection is indicated whenever patient presents with metastatic nodes. However, role of elective prophylactic lymph node dissection is considered controversial. It has been observed that SCC typically spreads first to regional lymph nodes [14,15]. In addition, for patients who develop nodal metastases prognosis is poor with an expected 5-year survival of 26- 34% [7,16]. This underlines the need for early detection and treatment of regional nodes in these cases. Some studies do recommend prophylactic lymph node dissection for cutaneous SCC greater than 8 mm in depth [17,18]. However strength of these recommendations is too week considering the morbidity associated with the lymph node dissection. To overcome this problem there has been recent interest in the application of sentinel lymph node biopsy in the management of high risk SCC [19,20]. Hypothetically, the procedure is feasible and may avoid unnecessary lymph node dissection. However, due to higher false negativity in the published series and lack of large, prospective studies it remains an investigational tool [21].
Adjuvant radiotherapy is indicated in presence of extensive perineural invasion or when margins are involved or when regional nodes show metastatic deposits [22,23]. Majority of the recurrences develop within first 2 years. Hence it is reasonable to follow up these patients for atleast 2 years and ideally upto 5 years [7,10]. Present patient was an immunocompetent elderly lady who developed SCC de novo on lateral aspect of right thigh (No exposure to sunlight) and had no history of trauma or chronic wounds. SCC developing on intact skin in the absence of any of the risk factors is rarely reported in literature.
Conclusion
The purpose of reporting this case is to highlight the rarity of the location for primary cutaneous squamous cell carcinoma and to critically review the literature for the current evidence in the management of these rare malignancies.
References
- Thompson AK, Kelley BF, Prokop LJ, Murad MH, Baum CL (2016) Risk Factors for Cutaneous Squamous Cell Carcinoma Recurrence, Metastasis, and Disease-Specific Death: A Systematic Review and Meta-analysis. JAMA Dermatol.
- Alam M, Ratner D (2001) Cutaneous squamous-cell carcinoma. N Engl J Med 344: 975-983.
- Karagas MR, Stannard VA, Mott LA, Slattery MJ, Spencer SK, et al. (2002) Use of tanning devices and risk of basal cell and squamous cell skin cancers. J Natl Cancer Inst 94: 224-226.
- Baldursson B, Sigurgeirsson B, Lindelöf B (1993) Leg ulcers and squamous cell carcinoma. An epidemiological study and a review of the literature. Acta Derm Venereol 73: 171-174.
- Chowdri NA, Darzi MA (1996) Postburn scar carcinomas in Kashmiris. Burns 22: 477-482.
- Moloney FJ, Comber H, O'Lorcain P, O'Kelly P, Conlon PJ, et al. (2006) A population-based study of skin cancer incidence and prevalence in renal transplant recipients. Br J Dermatol 154: 498-504.
- Rowe DE, Carroll RJ, Day CL Jr (1992) Prognostic factors for local recurrence, metastasis, and survival rates in squamous cell carcinoma of the skin, ear, and lip. Implications for treatment modality selection. J Am Acad Dermatol 26: 976-990.
- Friedman HI, Cooper PH, Wanebo HJ (1985) Prognostic and therapeutic use of microstaging of cutaneous squamous cell carcinoma of the trunk and extremities. Cancer 56: 1099-1105.
- Clayman GL, Lee JJ, Holsinger FC, Zhou X, Duvic M, et al. (2005) Mortality risk from squamous cell skin cancer. J Clin Oncol 23: 759-765.
- Breuninger H (1998) Diagnostic and therapeutic standards in interdisciplinary dermatologic oncology. Published by the German Cancer Society
- Brodland DG, Zitelli JA (1992) Surgical margins for excision of primary cutaneous squamous cell carcinoma. J Am Acad Dermatol 27: 241-248.
- Mohs FE, Snow SN (1985) Microscopically controlled surgical treatment for squamous cell carcinoma of the lower lip. Surg Gynecol Obstet 160: 37-41.
- MOHS FE (1947) Chemosurgical treatment of cancer of the ear; a microscopically controlled method of excision. Surgery 21: 605-622.
- Garcia-Zuazaga J, Olbricht SM (2008) Cutaneous squamous cell carcinoma. Adv Dermatol 24: 33-57.
- Martinez JC, Cook JL (2007) High-risk cutaneous squamous cell carcinoma without palpable lymphadenopathy: is there a therapeutic role for elective neck dissection? Dermatol Surg 33: 410-420.
- Reschly MJ, Messina JL, Zaulyanov LL, Cruse W, Fenske NA (2003) Utility of sentinel lymphadenectomy in the management of patients with high-risk cutaneous squamous cell carcinoma. Dermatol Surg 29: 135-140.
- Friedman NR (1993) Prognostic factors for local recurrence, metastases, and survival rates in squamous cell carcinoma of the skin, ear, and lip. J Am Acad Dermatol 28: 281-282.
- Afzelius LE, Gunnarsson M, Nordgren H (1980) Guidelines for prophylactic radical lymph node dissection in cases of carcinoma of the external ear. Head Neck Surg 2: 361-365.
- Tartaglione G, Potenza C, Caggiati A, Gabrielli F, Russo A, et al. (2003) [Sentinel node radiolocalisation and predictive value in lip squamous cell carcinoma]. Radiol Med 106: 256-261.
- Hatta N, Morita R, Yamada M, Takehara K, Ichiyanagi K, et al. (2005) Implications of popliteal lymph node detected by sentinel lymph node biopsy. Dermatol Surg 31: 327-330.
- Kwon S, Dong ZM, Wu PC (2011) Sentinel lymph node biopsy for high-risk cutaneous squamous cell carcinoma: clinical experience and review of literature. World J SurgOncol 9: 80.
- Mendenhall WM, Amdur RJ, Hinerman RW, Cognetta AB, Mendenhall NP (2009) Radiotherapy for cutaneous squamous and basal cell carcinomas of the head and neck. Laryngoscope 119: 1994-1999.
- Han A, Ratner D (2007) What is the role of adjuvant radiotherapy in the treatment of cutaneous squamous cell carcinoma with perineural invasion? Cancer 109: 1053-1059.
Relevant Topics
- 3D Printing in Limb-Sparing Surgery
- Adamantinoma
- Aneurysmal Bone Cysts
- Chondrosarcoma
- Chordomas
- Cryosurgery
- Enchondroma
- Ewing’s Sarcoma
- Fibrous Dysplasia
- Giant Cell Tumor of Bone
- Immunotherapy for Osteosarcoma
- Liquid Biopsy in Orthopedic Oncology
- Malignant Osteoid
- Metastatic Bone Cancer
- Molecular Profiling of Bone Tumors
- Multilobular Tumour of Bone
- Orthopaedic Oncology
- Osteocartilaginous Exostosis
- Osteochondrodysplasia
- Osteoma
- Osteonecrosis
- Osteosarcoma
- Primary Bone Tumors
- Sarcoma
- Secondary Bone Tumours
- Targeted Therapy in Bone Sarcomas
- Tumours of Bone
Recommended Journals
Article Tools
Article Usage
- Total views: 18804
- [From(publication date):
March-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 17826
- PDF downloads : 978