Case Report Open Access
Rapunzel Syndrome: A Case Report with Literature Review
Rajesh Godara*, Bansal AR, Sandhya, Jaikaran, Tamaknand V and Tripura R
Department of Surgical Gastroenterology and Surgery, Post Graduate Institute of Medical Sciences Rohtak, India
- *Corresponding Author:
- Dr Rajesh Godara
Department of Gastrointestinal Surgery
Post Graduate Institute of Medical Sciences
Rohtak, Haryana, India
Tel: 919812343765
E-mail: drrajeshgodara@yahoo.co.uk
Received date: April 15, 2015; Accepted date: May 26, 2015; Published date: May 30, 2015
Citation: Godara R, Bansal AR, Sandhya, Jaikaran, Tamaknand V, et al. (2015) Rapunzel Syndrome: A Case Report with Literature Review. J Gastrointest Dig Syst 5:291. doi:10.4172/2161-069X.1000291
Copyright: © 2015 Godara R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: Bezoar is a conglomeration of foreign material in the intestinal tract. Trichobezoar (accumulation of hair in the gastric chamber, secondary to impulsive pulling and intake) and Rapunzel syndrome (accumulation of hair in the small intestine) usually occur in children and adolescents with trichotillomania, trichophagia and gastric dysmotility disorder.The usual symptomatology includes vomiting and abdominal pain.
Case presentation: 18 year old female presented with complaints of dull aching epigastric pain, vomiting, loss of appetite and weight loss of 18 months duration. On examination she was emaciated having a palpable lump in epigastrium. Further examination and imaging showed a large trichobezoar. She underwent gastrotomy and extraction of hair ball. Post operative course was uneventful.
Conclusion: Early diagnosis and treatment of the Rapunzel syndrome is of eminent importance in order to avoid later fatal complications such as gastric perforation, intestinal obstruction and necrosis. Complete removal of trichobezoar and psychiatric consultation, coupled with long-term follow-up, are essential to prevent recurrence.
Keywords
Rapunzel syndrome; Trichobezoar
Introduction
Most bezoars are of indigestible organic matter such as hair-trichobezoars; or vegetable and fruit- phytobezoars; or a combination of both but other rare substances have also been been described in literature. Trichobezoars, commonly occur in patients with psychiatric disturbances but only 50% will have history of trichophagia. Trichobezoars are commonest type of bezoars comprise 55% of all.
Hair strands are retained in the folds of the gastric mucosa, peristalsis causes these to become enmeshed until a ball is formed that is too large to leave the stomach, resulting in gastric atony due to the large size of the trichobezoar.
These hair become matted together and assumes the shape of stomach; usually as a single mass. Very rarely they might invade through the small intestine and lead to intestinal obstruction, which is known as Rapunzel syndrome [1,2]. Untreated patients may either manifest as gastric outlet obstruction, GI bleed and very rarely with gastric necrosis and perforation.
Case Report
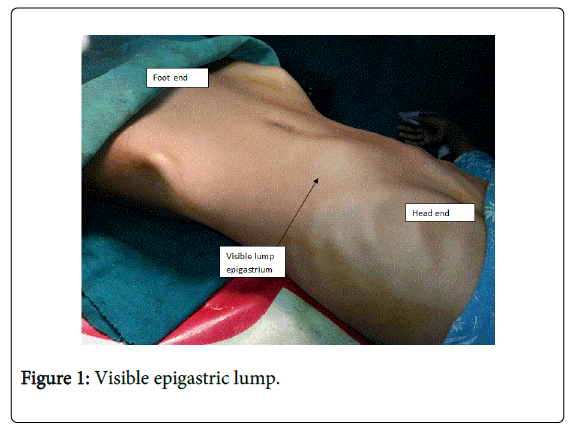
An 18 year old female presented to outdoor clinic with complaints of dull aching epigastric pain, non-bilious vomiting, decreased appetite and weight loss of 18 months duration. Clinical examination revealed an oblong,mobile well-defined mass occupying the upper half of the abdomen. The mass was non tender and firm in consistency (Figure 1).
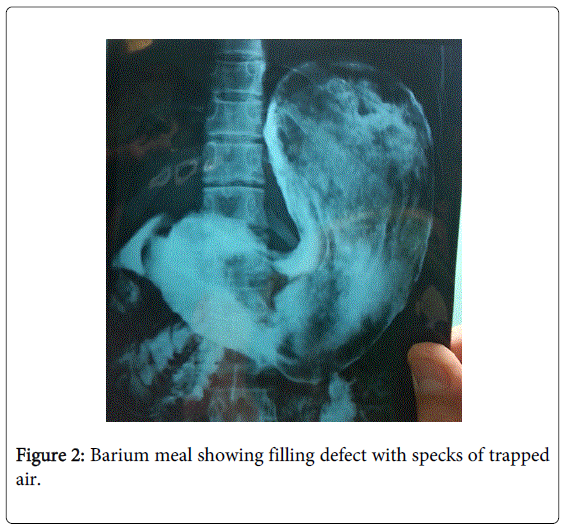
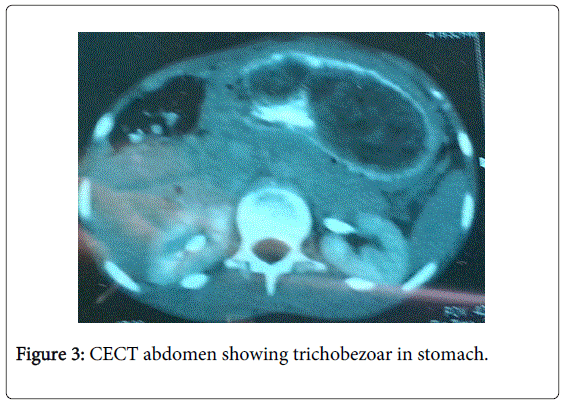
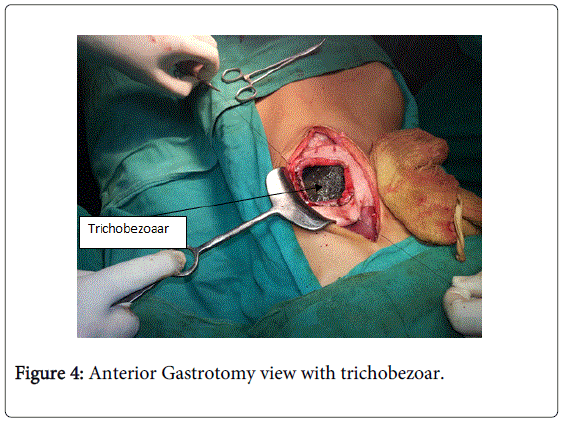
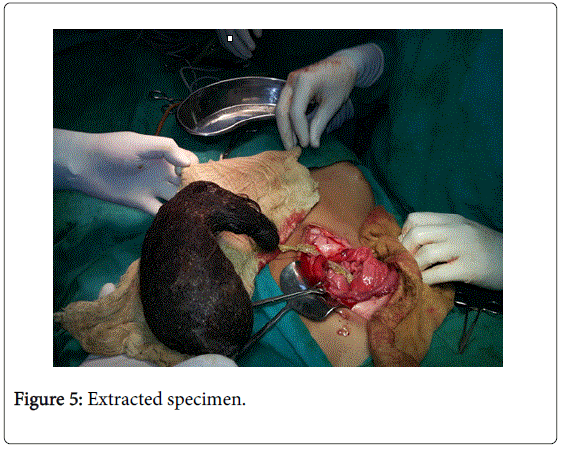
Laboratory tests revealed hypochromic microcytic anemia. Imaging in form of barium meal and CECT abdomen showed a large trichobezoar extending upto to the small bowel (Figures 2 and 3). She underwent laparotomy after fluid and electrolyte deficit correction. On exploration there was a huge trichobezoar ball filling the entire stomach cavity and extending into the duodenum and jejunum (Figure 4). The trichobezoar mass was removed via anterior gastrotomy (Figure 5). Abdominal cavity was closed after two layered closure of gastrotomy.
The patient had an uneventful postoperative course and was discharged after five days. She is currently being followed up as an outpatient both by surgical and psychiatric teams.
Discussion
Trichotillomania is characterized by recurrent and impulsive pulling of one's hair for pleasure, gratification, or relief of tension. Children and women <30 years of age are the ones who most frequently suffer from this type of disorder. Bezoars are concretions in the gastrointestinal tract that increase in size by continuous accumulation of non-absorbable food or fibers. Most bezoars in children are trichobezoars from swallowed hair from the head, dolls, or brushes. Trichobezoars formed by hair follicles are collected in mucosal folds and grow increasingly longer. Only 50% will have history of trichophagia. Trichobezoars have been described in literature and they comprise 55% of all bezoars [3]. As the proteins of the follicles denature, they discolour, turning black or brown, and an unpleasant odour seems to be emitted [4]. The common presentation of trichobezoar is in young females usually with an underlying psychiatric disorder causing symptoms, which could mimic gastrointestinal infections and infestation especially in endemic areas.
Rapunzel syndrome is a rare form of trichobezoar named after a fairy tale written in 1812 by the Brothers Grimm about a young maiden, Rapunzel, with long tresses who lowered her hair to the ground from her prison tower to permit her young prince to climb up to her window and rescue her [5]. Patient with Trichotillomania (a psychological condition that involves strong urges to pull hair), around 30% will engage in trichophagia, and of these, only 1% will go on to eat their hair to the extent requiring surgical removal. Various criteria have been used to diagnose the syndrome; however, the essential features are a trichobezoar, and a tail extending to the bowel or symptoms suggestive of bowel obstruction [6]. The clinical presentation can be variable. Patients may present with abdominal pain (37%), nausea and vomiting (33%), abdominal distension, diarrhoea or constipation, anorexia, weight loss (7%), or abdominal mass. Complications of trichobezoars include gastrointestinal obstruction (26%), bleeding (10%), perforation, malabsorption, and nutritional deficiencies.
Rapunzel syndrome associated with gastric perforation is a very rare entity and only few cases have been reported in the literature [7]. If bezoars are left without treatment, the mortality rate can reach 30% because of the associated complications [8]. Endoscopic removal is an option for small trichobezoar. Enzymatic dissolution, Nd-YaG laser and extracorporeal shock wave fragmentation are novel approaches to be further evaluated [9]. Regarding optimal surgical management of these cases, new reports on the use of video laparoscopy are encouraging. However, sample sizes have so far been small and, for this reason, the role of this technique in the treatment of the Rapunzel syndrome remains to be defined. Fragmentation carries the risk of small bowel obstruction, protein losing enteropathy, pancreatitis, steatorrhoea and perforation. The standard treatment remains surgical intervention for large, symptomatic and complicated trichobezoar like Rapunzel syndrome. Antidepressant treatment help control the obsession while behavioral therapy and family involvement provides the means for habit-reversal training.
Conclusion
Delayed treatment can leads to catastrophic complication like gastric perforation which is an extremely rare complication of Rapunzel syndrome. In such an event, treatment should follow the general lines of managing a perforated viscus with removal of bezoar with an anterior gastrotomy with subsequent psychiatric counselling to avoid recurrences.
References
- Phillips MR, Zaheer S, Drugas GT (1998) Gastric trichobezoar: case report and literature review. See comment in PubMed Commons below Mayo Clin Proc 73: 653-656.
- Koç O, Yildiz FD, Narci A, Sen TA (2009) An unusual cause of gastric perforation in childhood: trichobezoar (Rapunzel syndrome). A case report. See comment in PubMed Commons below Eur J Pediatr 168: 495-497.
- Al Wadan AH, Al Kaff H, Al Senabani J, Al Saadi AS (2008) 'Rapunzel syndrome' trichobezoar in a 7-year-old girl: a case report. See comment in PubMed Commons below Cases J 1: 205.
- Chintamani, Durkhure R, Singh JP, Singhal V (2003) Cotton Bezoar--a rare cause of intestinal obstruction: case report. See comment in PubMed Commons below BMC Surg 3: 5.
- Al-Wadan AH, Al-Absi M, Al-Saadi AS, Abdoulgafour M (2006) Rapunzel syndrome. See comment in PubMed Commons below Saudi Med J 27: 1912-1914.
- Frey AS, McKee M, King RA, Martin A (2005) Hair apparent: Rapunzel syndrome. See comment in PubMed Commons below Am J Psychiatry 162: 242-248.
- Naik S, Gupta V, Naik S, Rangole A, Chaudhary AK, et al. (2007) Rapunzel syndrome reviewed and redefined. See comment in PubMed Commons below Dig Surg 24: 157-161.
- Williams RS (1986) The fascinating history of bezoars. See comment in PubMed Commons below Med J Aust 145: 613-614.
- Coulter R, Antony MT, Bhuta P, Memon MA (2005) Large gastric trichobezoar in a normal healthy woman: case report and review of pertinent literature. See comment in PubMed Commons below South Med J 98: 1042-1044.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 17138
- [From(publication date):
June-2015 - Aug 28, 2025] - Breakdown by view type
- HTML page views : 12519
- PDF downloads : 4619