Rare Case Report of Primary Osteosarcoma of the Posterior Skull Base with Lung Metastases in 14 Years Old Female
Received: 10-Oct-2017 / Accepted Date: 27-Oct-2017 / Published Date: 31-Oct-2017 DOI: 10.4172/2167-7964.1000279
Abstract
Osteosarcoma arising from skull base are very rare. We report the case of a 14-year-old female patient who presented with a swelling in the right postauricular region for 6 months, which proved to be a high-grade osteosarcoma. On Chest screening, we found two lung nodules which most likely represent metastases. We describe pre-and post-operative findings on Computed Tomography (CT) and Magnetic Resonance Imaging (MRI). We review the literature of reported cases of primary osteogenic sarcomas of the skull to discuss the common clinical presentation, evaluation methods, and recommended treatment plans.
Keywords: Osteosarcoma; CT scan; MRI; Metastases
Introduction
Osteosarcoma is the most common primary osseous malignancy excluding malignant neoplasms of marrow origin (myeloma, lymphoma and leukemia). However, only 5-10% are located in the craniofacial bones and most common locations are maxilla & mandible [1-8]. Cranial vault osteosarcoma is very rare with occurrence of less than 1% [1-6]. The most common radiological findings of osteosarcoma are ill defined osteolytic lesion with wide zone of transition, cortical bone destruction, an aggressive periosteal reaction (speculated, laminated type or Codman’s triangle), a soft tissue mass, and a tumor matrix in the destructive lesion. Most osteosarcomas are purely osteolytic however few lesions appear as sclerotic or mixed [1-8]. Here we represent a rare case of posterior skull base osteosarcoma with possible two lung metastases.
Case Report
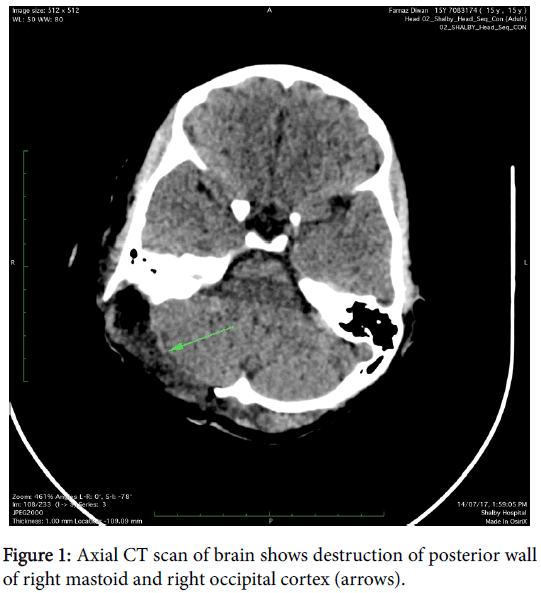
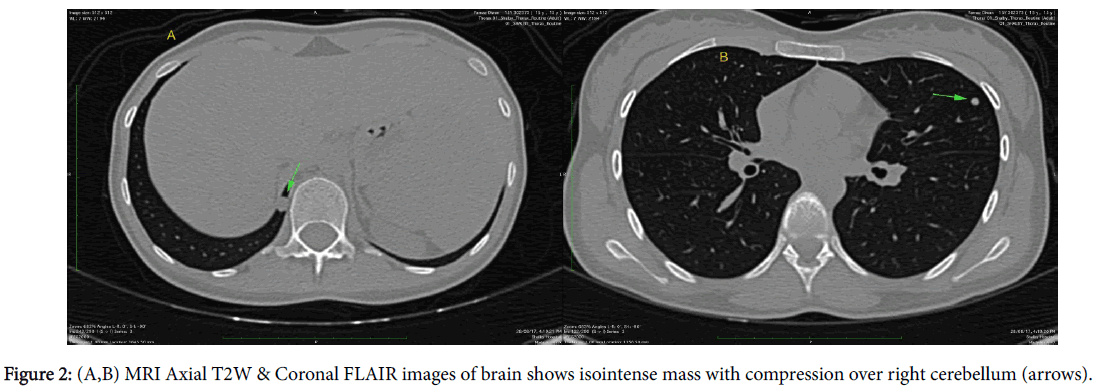
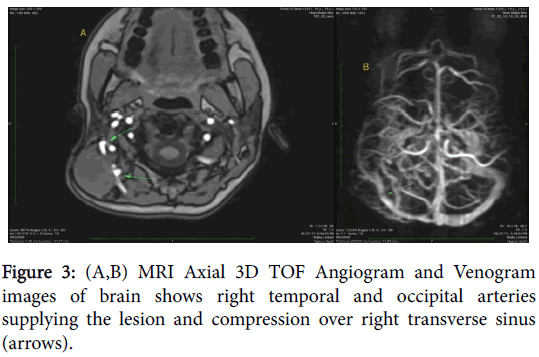
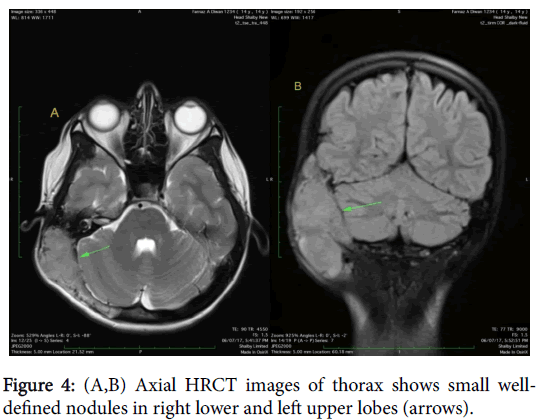
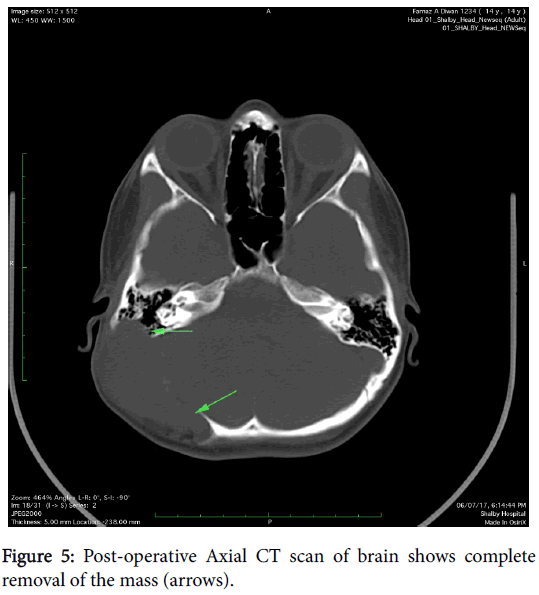
A 14-year-old female patient presented with a swelling at postauricular region since for six months. The swelling was slow growing. Patient gave history of trauma as well at same region so clinically hematoma was considered as a main possibility. CT scan was carried out which showed presence of large expansile soft tissue density mass involving right occipitotemporal and parietal skull vault with areas of destruction of inner & outer table and also of posterior wall of right mastoid (Figure 1). On MRI study, the mass was seen as isointense on T1 weighted, T2 weighted and FLAIR images with compression over right cerebellum (Figure 2) and area of hemorrhage within which was seen as hyperintense area on T1W images & corresponding loss of signal on susceptibility weighted images. The lesion also causes mild compression over right transverse sinus and is supplied by right occipital and temporal arteries (Figure 3). Screening of thorax and abdomen was also done to rule out metastases. High resolution computed tomography (HRCT) of thorax showed presence of two well-defined nodules in left upper and right lower lobes (Figure 4), which were proved to be metastases. Biopsy was taken from the lesion and was proven to be a high grade osteoblastic osteosarcoma. Therefore, the lesion was completely removed and post-surgical CT scan was also done which showed complete resection of the mass (Figure 5).
Discussion
Osteosarcoma is the most common solid primary malignancy of bone. However, primary osteosarcoma of the skull base is rare, about 150 cases reported since 1945 [1-9].
Common clinical symptoms are slow growing swelling, pain and a soft tissue mass, which is tender to palpation [2,4,7,9]. CT scan and MRI are the preferred radiological investigations. MRI is superior to CT for defining soft tissue extension and marrow involvement, and the presence of skip lesions. Most common radiological features are an illdefined osteolytic lesion with wide zone of transition, cortical bone destruction, an aggressive periosteal reaction (speculated, laminated type or Codman’s triangle), a soft tissue mass, and a tumor matrix in the destructive lesion [1-8].
Metastasis of craniofacial osteosarcoma is uncommon with lungs as most common locations for metastases. CT scans are best suited to evaluate the thorax for metastatic disease.
Radionuclide bone scanning with technetium is the preferred method for evaluating the entire skeleton for the presence of multiple lesions. The current survival rate for children with localized osteosarcoma is approximately 65%, compared with 25% for patients with metastatic disease [7,9,10].
Biopsy should be performed after complete history, clinical examination and imaging. Percutaneous core needle biopsy has now been established as safe and accurate method for diagnosing of bone tumors. It is done under radiological imaging guidance such as CT scan, MRI or ultrasonography. The biopsy tract needs to be planned in consultation with the orthopedic oncosurgeon [9,10].
The final diagnosis of Osteosarcoma was only established by the histological studies. Most common treatment option is complete removal of the tumour by surgery followed by chemotherapy or radiotherapy [8-10].
References
- Ashkan K, Pollock J, D’Arrigo C, Kitchen ND (1998) Intracranial osteosarcomas: report of four cases and review of the literature. J Neurooncol 40: 87-96.
- Benson JE, Goske M, Han JS, Brodkey JS, Yoon YS (1984) Primary osteogenic sarcoma of the calvaria. AJNR Am J Neuroradiol 5: 810-813.
- Bose B (2002) Primary osteogenic sarcoma of the skull. Surg Neurol 58: 234-240.
- Gadwal SR, Gannon FH, Fanburg-Smith JC, Becoskie EM, Thompson LD (2001) Primary osteosarcoma of the head and neck in pediatric patients. Cancer 91: 598-605.
- Gangadhar K, Santhosh D (2012) Radiopathological evaluation of primary malignant skull tumors: a review. Clin Neurol Neurosurg 114: 833-839.
- Garland LH (1945) Osteogenic sarcoma of the skull. Radiology 45: 45-48.
- Mascarenhas L, Peteiro A, Ribeiro CA, Magalhães Z, Romão H, et al. (2004) Skull osteosarcoma: illustrated review. Acta Neurochir 146: 1235-1239.
- Fukunaga M (2005) Low-grade central osteosarcoma of the skull. Pathol Res Pract 201: 131-135.
- Chander B, Ralte AM, Dahiya S, Sharma MC (2003) Primary osteosarcoma of the skull. A report of 3 cases. J Neurosurg Sci 47: 177-181.
- Patel AJ, Rao VY, Fox BD, Suki D, Wildrick DM, et al. (2011) Radiation-induced osteosarcomas of the calvarium and skull base. Cancer 117: 2120-2126.
Citation: Solanki S, Dave K (2017) Rare Case Report of Primary Osteosarcoma of the Posterior Skull Base with Lung Metastases in 14 Years Old Female. OMICS J Radiol 6: 279. DOI: 10.4172/2167-7964.1000279
Copyright: © 2017 Solanki S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Tools
Article Usage
- Total views: 6314
- [From(publication date): 0-2017 - Oct 19, 2025]
- Breakdown by view type
- HTML page views: 5420
- PDF downloads: 894