Research Article Open Access
Rectal, Axillary or Skin Temperature in Newborns?
| Giulia Placidi*, Ilaria Merusi and Luigi Gagliardi | |
| Woman and Child Health Department, Pediatrics and Neonatology Division, Italy | |
| Corresponding Author : | Giulia Placidi Woman and Child Health Department Pediatrics and Neonatology Division Ospedale Versilia Via Aurelia 335, I - 55043 - Lido di Camaiore (LU), Italy Tel: 3905846057113 Fax: 3905846059764 E-mail: giulia.placidi@gmail.com |
| Received July 17, 2014; Accepted December 03, 2014; Published December 08, 2014 | |
| Citation: Placidi G, Merusi I, Gagliardi L (2014) Rectal, Axillary or Skin Temperature in Newborns? J Preg Child Health 1:123. doi: 10.4172/2376-127X.1000123 | |
| Copyright: © 2014 Placidi G, et al.This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Pregnancy and Child Health
Abstract
Background: Hypothermia in newborns is strongly associated with increased morbidity. Despite its importance, where and how temperature should be measured is not still clearly defined.
Aim: To compare sites and instruments for measuring temperature in newborns to estimate differences and limits of agreement.
Patients: Sample: 107 healthy term newborns. The temperature was measured in three different body sites (forehaed, axilla and rectum), using three different thermomethers.
Results: Mean ± DS rectal temperature was 36.9 ± 0.4°C, mean axillary temperature was 36.5 ± 0.4°C, mean skin temperature was 36.1 ± 0.4°C. The mean rectal-axillary temperature difference was 0.3 °C (limits of agreement -0.30 to 0.92); the mean axillary-skin difference was 0.35°C (limits of agreement -0.45 to 1.17); the rectal-skin difference was 0.67°C (limits of agreement -0.05 to 1.40). All the differences between methods are statistically significant. Infants born after a cesarean section had a slightly lower temperature than after vaginal delivery.
Conclusions: Observed values of temperature depend on site and type of thermometer used. Since the measure in different sites produces different results, it seems necessary to define an objective way to assess it. The core-peripheral temperature difference may detect a thermal stress.
| Keywords |
| Newborn; Temperature; Cold stress; Reproducibility of results; Skin |
| Introduction |
| An association between neonatal hypothermia and increased morbidity both in healthy neonates and in low birth weight infants has been known since several years [1,2]. Despite its importance, several controversies exist regarding body temperature in neonates. Firstly, the normal temperature range in newborn is not clearly defined, and depends on where and how it is measured. The World Health Organization (WHO) reports the normal “core” temperature to be above 36.5°C, while temperatures of 36 to 36.4°C are labeled as mild hypothermia, those 32 to 35.9°C as moderate and those <32°C as severe hypothermia. According to the WHO, axillary temperature is better than the rectal temperature because of hygiene, safety and ease [3]. In newborns, the presence and degree of hypothermia is an item in assessment of disease severity in several scores such as Clinical Risk Index for Babies II (CRIB) [4] and Score of Neonatal Acute Physiology Perinatal Extension II (SNAPPE) [5], and an item recorded also by the Vermont Oxford Network (VON), but surprisingly its detection method and site are not specified. Although the measurement of rectal temperature was widely considered to be the gold standard for the newborn [6,7], it is slower and more invasive than other alternatives, and because of its risks and drawbacks, the American Academy of Pediatrics (AAP), the National Institute for Health and Clinical Excellence (NICE) and the Italian Pediatric Society (SIP) recommend avoiding rectal temperature and recommend the axillary site instead [8-10]. |
| Because of the recent recall of mercury thermometers [11], companies have increased the range of equipment commercially available for the clinician, specifically reserved for different body site (rectal, skin, axillary), including less invasive methods. Few and conflicting data are available on the performance of thermometers in neonates, and on the exchangeability of temperatures obtained in different sites [12-16]. New Italian guidelines from the Ministry of Health [17] recommend to monitor newborn’s temperature immediately after birth, but axillary thermometer could interfere with mother-infant bonding and breastfeeding, while infrared forehead measurement would not, because of its lack of body contact. Given all these uncertainties, the aim of the study was to compare different instruments for measuring temperature in different sites of the body in a sample of newborns at birth, to estimate differences and limits of agreement. |
| Patients |
| We studied a sample of 107 healthy (i.e not requiring any special care) term newborns. All these newborns had an uneventful delivery, and followed the usual routine of care of our hospital: for the first two hours after delivery, mother and baby were transferred in a post-delivery room with a controlled temperature of 24°C. During this observation period, the babies stayed with their mothers, covered with clothes after being bathed and dried. After this time mothers and infants were transferred to the ward, where we carried out the measurements. |
| Methods |
| For each infant, the temperature was measured by the same nurse in three different body sites (forehaed, axilla and rectum), using three different thermometers specifically designed for each site, at two hours of life. Rectal temperature was assessed by digital thermometer Chicco Artsana; axillary temperature by electronic themometer Kendall Filac 3000, and forehead skin temperature by infrared thermometer Thermofocus 01500 Tecnimed. For the purpose of this study, we defined hypothermia following WHO defintions [3]. Data are expressed as means (SD). For each infant, we calculated the difference between temperature recordings (rectal-axillary; rectal-forehead; axillary-forehead); paired data Student t test was used for betweengroup comparisons. The limits of agreement between methods were calculated according to Bland and Altman as the mean (± 2 SD) of the differences between the three measurements [18]. All calculations were carried out with the statistical package Stata 11. |
| Results |
| Mean birthweight was 3321 g (SD 452 g, range 2210- 4440 g), mean gestational age 38 (SD 1,38 weeks, range 37-41 weeks); 22 infants (20%) were delivered by cesarean section (CS). Mean (DS) rectal temperature was 36.9°C (0.4), (range 35.9- 37.6); mean axillary temperature was 36.5°C (0.4) (range 35.1-37.5); mean forehead skin temperature was 36.1°C (0.4), range 35.4-37.2). Depending on the method and site of measurements, the number of neonates deemed hypothermic was different (Table 1). The comparison between techniques in individual infants are reported in Figure 1; the mean difference between rectal and axillary temperature was 0.31°C (limits of agreement -0.30 to 0.92); the mean difference between axillary and forehead temperature was 0.35°C (limits of agreement -0.45 to 1.17); and that between rectal and skin temperature was 0.67°C (limits of agreement -0.05 to 1.40). All the differences between methods were statistically significant (P<0,001). We never observed a difference between rectal and axillary/forehead temperature greater than 2°C, which could indicate ‘cold stress’ [20]. Temperatures depended on birth weight for all methods (p <0.003, by correlation analysis), a kilogram of weight being associated with about 0.3 degrees increase for rectal and axillary temperature, and about 0.15 degrees for skin temperature. Temperature was different by mode of delivery, as measured by all methods: rectal mean temperature in cesarean sections (CS) was 36.6°C (0.3) , in vaginal deliveries was 36.9°C (0.3); axillary mean temperature in CS was 36.2°C (0.4) vs 36.6°C (0.3); skin mean temperature was 36.0°C (0.3) in CS, vs.36.2°C (0.3) in vaginal deliveries. (P<0.05 for all comparisons). Frequency different degrees of hypothermia according to mode of delivery is shown in Table 1. No adverse events were observed and all the thermometers were judged safe and easy to use by nurses. |
| Discussion |
| We found that the observed values of temperature depend on site of measurement and related type of thermometer used. |
| In the past, rectal temperature was considered the gold standard to measure core temperature, but due to its drawbacks it is not presently recommended as the routine method of assessing this parameter by scientific societies [8,9,10]. |
| For each couple of measurements, we plotted the difference vs. the mean value (so called Bland-Altman plot) [18]. This technique is generally used to assess the agreement between methods purported to measure the same thing. In this case however, the differences are due to two different sources of variability: that between sites, and that between thermometers, specifically designed for a site. Thus, the limits of agreement are inflated by a systematic difference that probably reflects a biologic phenomenon (e.g., that the forehead is really colder than the rectum). In this study a clear gradient of temperature was observed between rectal, axillary and skin temperature. The difference between axillary and rectal temperature is in agreement with the results of a metaanalysis carried out some years ago comparing sites of measurement, [19] and with traditional wisdom in Italy, that suggests “half a degree” difference between rectal and axillary values, and with some [13,14] but not all [16] studies. As for the difference between forehead and rectal temperature, the same discrepancies occur [15,16]. There are few data on this issue regarding neonates. Unlike Uslu et al. [16], De Curtis et al. [15] found no difference between rectal and infrared skin temperature, in stable preterm and term neonates, at mean age of 15.7 days. The agreement between the two methods could be due to the thermo-neutral environment where preterm infants were maintained. It has been found that preterm infants have a smaller core-surface temperature gradient because of their relative lack of thermal insulation by body fat [13,20]. It is of interest that we found that infants born after a cesarean section had a slight but persistent lower temperature that those after vaginal delivery. The lower temperature in cesarean section is probably due to several causes, including temperature in the operating theatre, and, for elective cesarean sections, the absence of labor, that leads to a reduction in non-shivering thermogenesis in brown adipose tissue [21]. Effects of anaesthetics on the mother’s body temperature were also considered to be responsible [22], but all our CS were carried out in epidural, not general anaesthesia. In conclusion, since the measure of temperature in different body sites produces different results, it is necessary to define a standard way to assess it and to define which is the optimal temperature range in newborns. For an early detection of hypothermia and the related risks, a dual site (axillary-skin) measurement could be useful. A growing concern about Sudden Unexpected Postnatal Collapse (SUPC) requests even more attention on the early post natal period, including temperature measurement in the first hours immediatly after birth. Infrared forehead temperature measurement is a non invasive method which does not interfere with infant-mother bonding and breastfeeding, therefore offering a clear advantage over other methods while maintaining a precision comparable to other methods, once the ‘baseline’ difference between methods is taken into account. |
| Author Contributions |
| GP wrote the first draft of the manuscript. IM and LG conributed to manuscript preparation. GP and LG carried out statistical analyses and prepared tables and figure. All Authors contributed to the overall project design, instrument preparation, acquisition of data, interpretation of the results, and critically revised the paper, and have seen and approved the submission of this version of the manuscript. |
References
- Silverman WA, Fertig JW, Berger AP (1958) The influence of the thermal environment upon the survival of newly born premature infants. Pediatrics 22: 876-886.
- McCall EM, Alderdice FA, Halliday HL, Jenkins JG, Vohra S (2010). Interventions to prevent hypothermia at birth in preterm and/or low birthweight infants. Cochrane Database of SustematyReviews , Issue 3. Art. No.: CD004210. DOI:10.1002/14651858.CD004210.pub4.
- Thermal protection of the newborn: a practical guide. WHO, RHT/MSM/97.2 [online] 1997 [cited 2006 June 15]. WHO reference number: WS 420 97TH
- Parry G, Tucker J, Tarnow-Mordi W; UK Neonatal Staffing Study Collaborative Group (2003) CRIB II: an update of the clinical risk index for babies score. Lancet 361: 1789-1791.
- Richardson DK, Corcoran JD, Escobar GJ, Lee SK (2001) SNAP-II and SNAPPE-II: Simplified newborn illness severity and mortality risk scores. J Pediatr 138: 92-100.
- Bailey J, Rose P (2001) Axillary and tympanic membrane temperature recording in the preterm neonate: a comparative study. J AdvNurs 34: 465-474.
- Martin SA, Kline AM (2004) Can there be a standard for temperature measurement in the pediatric intensive care unit? AACN Clin Issues. 15(2): 254-266.
- American Academy of Pediatrics Committee on Fetus and Newborn. Hospital Stay for Healthy Term Newborns (2004) Pediatrics 113;1434.
- National Collaborating Centre for Women's and Children's Health (UK) (2007) Feverish illness in children: assessment and initial management in children younger than 5 years. NICE Clinical Guidelines no. 47. RCOG Press 2007.
- SocietàItaliana di pediatria 2011 Gestione del segno/sintomofebbre in pediatria. LineeGuidadellaSocietàItaliana di Pediatria.
- Directive 2007/51/EC of the European Parliament and of the Council of 25 September 2007 amending Council Directive 76/769/EEC relating to restrictions on the marketing of certain measuring devices containing mercury.
- Trevisanuto D, Martellan B, Zanconato S, Cavallin F, Zanardo V (2011) Accuracy of infrared skin thermometers in children. Arch Dis Child 96: 785-786.
- Roll C, Horsch S, Husing J et al. (2000) Small premature infant do not tolerate axillary temperature measurement any better than rectal measurement. Study of the effect of axillary and rectal temperature measurement on vital parameters and cerebral hemodynamics and oxygenation. Z GeburtshilfeNeonatol 204(5): 193-197.
- Hissink Muller PC, van Berkel LH, de Beaufort AJ (2008) Axillary and rectal temperature measurements poorly agree in newborn infants. Neonatology 94: 31-34.
- De Curtis M,Calzolari F, Marciano A, Cardilli V, Barba G (2008) Comparison between rectal and infrared skin temperature in the newborn. Arch Dis Child Fetal Neonatal Ed 93: F55-57.
- Uslu S,Ozdemir H, Bulbul A, Comert S, Bolat F, et al. (2011) A comparison of different methods of temperature measurements in sick newborns. J Trop Pediatr 57: 418-423.
- MinisterodellaSalute.Raccomandazione per la prevenzionedellamorte o disabilitàpermanente in neonatosano di peso>2500 grammi non correlata amalattiacongenita. Roma 2014.
- Bland JM, Altman DG (1986) Statistical methods for assessing agreement between two methods of clinical measurement. Lancet 1: 307-310.
- Craig JV, Lancaster GA, Williamson PR, Smyth RL (2000) Temperature measured at the axilla compared with rectum in children and young people: systematic review. BMJ 320: 1174-1178.
- Lyon AJ, Freer Y (2011) Goals and options in keeping preterm babies warm. Arch Dis Child Fetal Neonatal Ed 96: F71-74.
- Clarke L, Heasman L, Firth K, Symonds ME (1997) Influence of route of delivery and ambient temperature on thermoregulation in newborn lambs. Am J Physiol 272: R1931-1939.
- Christensson K, Siles C, Cabrera T, Belaustequi A, de la Fuente P, et al. (1993) Lower body temperatures in infants delivered by caesarean section than in vaginally delivered infants. ActaPaediatr 82: 128-131.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
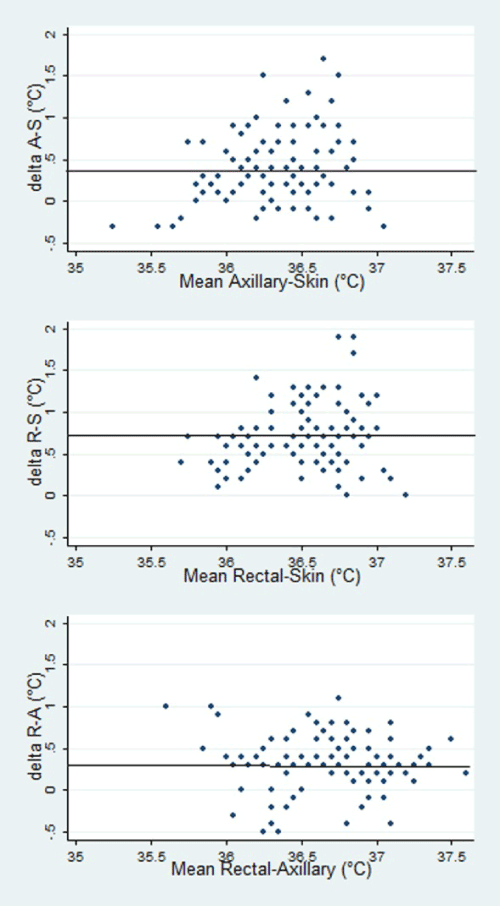 |
| Figure 1 |
Relevant Topics
Recommended Journals
Article Tools
Article Usage
- Total views: 16083
- [From(publication date):
December-2014 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 11449
- PDF downloads : 4634
