Commentary Open Access
Re-Examinations-A High Cost Affair Commentary on "Music Does Not Alter Anxiety in Patients with Suspected Lung Cancer Undergoing Bronchoscopy: A Randomised Controlled Trial" European Clinical Respiratory Journal
Elisabeth Jeppesen RN1*, Carsten M Pedersen RN2, Klaus R Larsen1and Vibeke Backer11Department of Respiratory Medicine, Bispebjerg Hospital, Copenhagen, Denmark
2Department of Thoracic Anaesthesiology, Rigshospitalet, Copenhagen, Denmark
- *Corresponding Author:
- Elisabeth Jeppesen
Department of Respiratory Medicine
Bispebjerg Hospital, Copenhagen, Denmark
E-mail: Elisabeth.Margrethe.Langvall.Jeppesen@regionh.dk
Received Date: January 13, 2017; Accepted Date: January 30, 2017; Published Date: February 06, 2017
Citation: Jeppesen ERN, Pedersen CMRN, Larsen KR, Backer V (2017) Re-Examinations - A High Cost Affair. Cancer Surg 2: 106.
Copyright: © 2017 Jeppesen ERN, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License; which permits unrestricted use; distribution; and reproduction in any medium; provided the original author and source are credited.
Visit for more related articles at Cancer Surgery
Commentary
Within the field of diagnosing lung cancer it is essential to use the newest technology and as fast as possible to diagnose and direct patients to correct treatment. And, importantly, this should be done gently. Most patients experience fear when facing the possibility of suffering from lung cancer, but also the thought of undergoing bronchoscopy may provoke fear. Prior to the current study, music has been investigated in relation to bronchoscopy with different outcomes and with contradictory findings [1-4]. Music is a low-cost and a lowrisk intervention. We hypothesized that MusiCure would reduce anxiety and that as a result of reduced anxiety, patients undergoing bronchoscopy would lie more still, and so it would be easier to get the necessary material, and fewer reexaminations would be needed. “MusiCure-music as medicine” is music composed by the Danish composer Niels Eje and his aim is to compose music that is relaxing and soothing.
We found no significant differences between the groups on anxiety measured with STAI (Spielberger´s State-Trait Anxiety Inventory) when corrected for gender and baseline anxiety (Table 1). Neither did we find any significant differences between the groups in head, body, leg or arm movement, measured by Actigraphs (GT3X+), which were attached to the patient’s head, hip, ankles and wrists. In the current study, the staff attending the bronchoscopy, who actively held the patient’s hands and head to calm the patient, could confound measurement of movement. In addition, the sensor on the head was found to easily fall off.
| b | SEB | β | p | |
|---|---|---|---|---|
| Model 1 | ||||
| Constant | 41.26 | 1.67 | P<0.0001* | |
| (37.95 to 44.56) | ||||
| Group | -5.31 | 2.34 | -0.19 | P=0.025* |
| (-9.94 to -0.68) | ||||
| Model 2 | ||||
| Constant | 0.81 | 2.16 | P=0.706 | |
| (-3.45 to 5.08) | ||||
| Group | -1.17 | 0.98 | -0.04 | P=0.234 |
| (-3.09 to 0.76) | ||||
| STAI State at arrival | 0.87 | 0.05 | 0.8 | P<0.0001* |
| (0.77 to 0.96) | ||||
| STAI Trait at arrival | 0.17 | 0.05 | 0.13 | P=0.001* |
| (0.07 to 0.28) | ||||
| Gender | -2.38 | 1.03 | -0.09 | P=0.022* |
| (-4.41 to -0.35) | ||||
Table 1: Linear model of predictors of STAI state immediately before bronchoscopy, with 95% bias corrected and accelerated confidence intervals reported in parentheses.
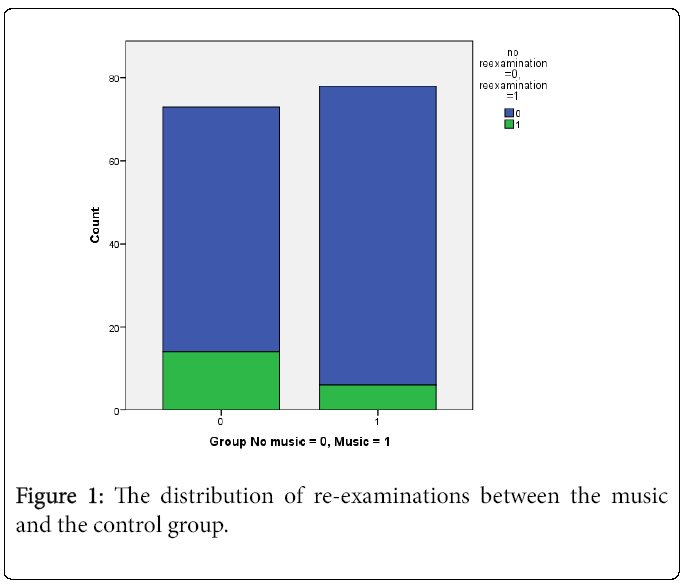
Surprisingly, we found a significant difference in number of reexaminations. Significantly more patients required re-examination in the control group without music compared to the music group (19.2% (14 of 73) and 7.7% (6 of 78), respectively; p<0.032), with a 2.49 times higher odds ratio of reexamination among those in the no-music group (Figure 1).
This was surprising because there was no significant difference in the duration of the bronchoscopies between the groups, or between the physicians who performed neither the bronchoscopy, nor the diagnostic procedures performed during bronchoscopy. There was though an uneven count of earlier bronchoscopies between the groups, but no significant difference. The earlier bronchoscopies had been performed before the study period, and some dating several years back. In the music group 11 had had a bronchoscopy performed before vs. 67 who had not, but in the control group five had had a history with an earlier bronchoscopy vs. 68 who had not. This could possibly confound the result. The follow-up period was 14 days, in this study, and most patients would be reexamined within 14 days, but some might not. This could also have confounded the result.
Dubois et al. [1] reported less coughing when patients listened to music while undergoing bronchoscopy. Less coughing can make it easier to get relevant and sufficient biopsies. We had no sensors on the thorax. Less coughing could be the cause of fewer re-examinations.
These thoughts, amongst others, have led to a follow-up study where we have added an exclusion criterion, so to participate in the study there must be no earlier history of bronchoscopy. In the follow-up study there is a sensor on the thorax, but no sensors elsewhere. We have also added a third study group with self-selected music. In addition the period for following up on re-examinations has been extended. In the ongoing study it has been extended to 28 days. The data collection period is expected to terminate by the end of 2017.
A re-examination is a high-cost affair both as regards the expenses incurred in performing one more investigation, but also a high-cost affair for the patient awaiting the diagnosis, as the period of uncertainty is extended. Furthermore, re-examinations also extend the period before the final diagnosis, which is crucial in cancer diagnostics. It is therefore of interest both to the healthcare system and to the patient to minimize the number of re-examinations and if music is a solution it is a low-risk and a low-cost intervention.
References
- Dubois JM, Bartter T, Pratter MR (1997) Music improves patient comfort level during outpatient bronchoscopy. J Bronchology Interv Pulmonol 4: 83.
- Colt HG, Powers A, Shanks TG (1999) Effect of music on state anxiety scores in patients undergoing fiberoptic bronchoscopy. Chest 116: 819-824.
- Triller N, Erzen D, Duh S, Petrinec Primozic M, Kosnik M (2006) Music during bronchoscopic examination: the physiological effects. A randomized trial. Respiration 73: 95-99.
- Tam WW, Lo KK, Hui DS (2016) The effect of music during bronchoscopy: A meta-analysis. Heart Lung 45: 86-94.
Relevant Topics
- Breast Cancer Surgery
- Colon Cancer Surgery
- Dermatologic Surgery
- Kidney Cancer Surgery
- Leukemia Surgery
- Lung Cancer Surgery
- Lymphoma Surgery
- Oesophageal Cancer Surgery
- Pancreatic Cancer Surgery
- Prostate Cancer Surgery
- Radiation Therapy
- Skin Cancer Surgery
- Stomach Cancer Surgery
- Throat Cancer Surgery
- Thyroid Cancer Surgery
Recommended Journals
Article Tools
Article Usage
- Total views: 3396
- [From(publication date):
March-2017 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 2514
- PDF downloads : 882