Rehabilitation Tool for Gastroparesis by the Analysis of Interstitial Cells of Cajal (The External Gastric Pacmaker with a Feedback of Gastric Potential)
Received: 20-Mar-2018 / Accepted Date: 27-Mar-2018 / Published Date: 05-Apr-2018 DOI: 10.4172/2161-069X.1000557
Abstract
Gastric diseases are the third most fatal to world’s population which causes substantial mortality and morbidity (nearly 60-70 million people were affected). For example: Hernia, Chronic constipation, Gastro Esophageal Reflux Disease, colorectal cancer, gastroparesis, peptic and gastric ulcers, ulcerative colitis, crohn’s disease etc. Gastroparesis (GP) is the one such disease defined as the paralysis of stomach results in delayed gastric emptying which lacks the peristaltic action of stomach that breaks down the bolus into smaller particles makes it suitable for entering into the duodenum. Gastroparesis is a condition which cannot be cured by drugs or any other therapies rather it needs a life supporting tool which grasps our attention of making innovativeness in the existing system. The reliable therapy for gastroparesis is Gastric Electrical Stimulation through enterra system. The innovation made with the our enterra system is to induce the stimulation with the feedback information from the Electrogastrograph (EGG) module that enables the pacemaker to work on synchronous mode rather than the existing enterra system that induce the stimulation with the help of timing and clock circuit or activated by the patients. The EGG that extracts the functional information of stomach is solely being the appropriate and effective method to study motility parameter to establish gastric pacing activity. The best solution for this most intolerable disease can be provided by the gastric electrical stimulation of the Interstitial Cells of Cajal (ICC) called pacemaker.
Keywords: Gastroparesis; Enterra system; Electrogastrograph; Interstitial cells
Introduction
The proposal of this revolutionary project begins with improving the accuracy of the non-invasive gastric diagnostic tool (EGG) [1], which serves as the only method suitable for diagnosing gastroparesis. Ceased gastric motility has been observed by analyzing its electrical activity through EGG. The therapy for gastroparesis is the gastric electrical stimulation which is induced by the feedback from the EGG when detecting the delayed gastric emptying. The treatment can be provided permanently by the activation or stimulation of gastric muscles to overrule the gastric dysfunction. The automation of gastric pacing can be done through controlling the stimulator with EGG which enables the synchronous mode of operation rather than activating manually. The “rehabilitation tool for gastroparesis by the analysis of interstitial cells of cajal” is a therapeutic device which improves the patient condition through intelligent stimulation by analyzing the electrical activity of the stomach.
Etiology of Gastroparesis
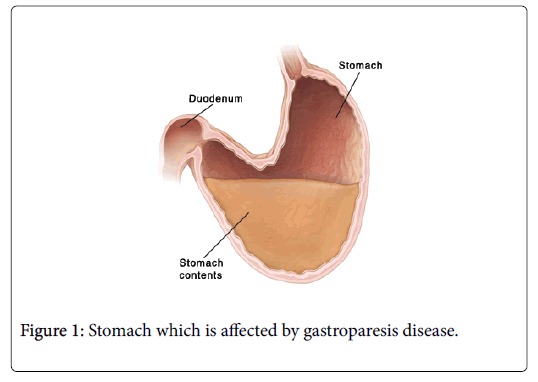
The Gastroparesis is a disease that causes delayed gastric emptying. The stomach gradually becomes unresponsive for the stimulus from the interstitial cells of cajal. Due to improper stimuli from ICC, the stomach wall tends to paralyzed. The paralyzed stomach will not give good digestion, so the food contents starts staying inside the stomach and results poor digestion (Figure 1). The disease is quite difficult to tolerate and also cannot be cured completely [2]. The disease can either be controlled or the symptoms are reduced by the gastric external stimulation. The stimulation is the most effective method that overrules the gastric dysfunction and regulates its mobility [3]. This method is also not effective, if it provides asynchronous stimulation. Rather retaining the original gastric activity this unregulated stimulation will cause saturation and the stomach muscles will develop an irreversible unresponsiveness. This complicates the disease to the extent of death. Thus, this proposed methodology will offer a revolutionary solution for gastroparesis with fewer complications [4].
Physiology of Stomach
The physiology of the stomach and the electrical properties are important in assessing about the health.
Interstitial cells of cajal–natural gastric pacemaker
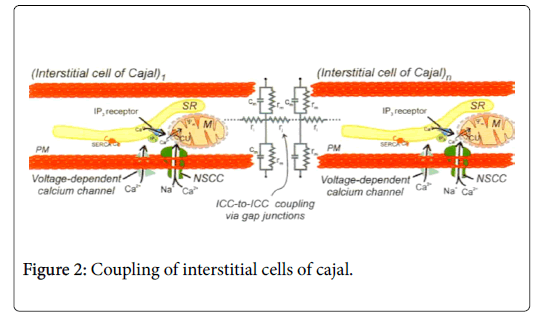
The entire stomach wall is interiorly coated by interstitial cells of Cajal (ICC). The ICCs are the pacemaker cells, the cells that spontaneously depolarize and repolarize and set the myoelectrical rhythmicity of the stomach and other areas of the gastrointestinal tract. The interstitial cells are electrically coupled with the circular muscle cells (Figure 2).
Low-amplitude rhythmic circular contractions occur at the pacemaker rhythm. Rhythmicity and contractility of the circular muscle layer are modulated by ongoing activity excitatory and inhibitory of myenteric neurons that synapse with the interstitial cells [5].
Electrical activity of the stomach
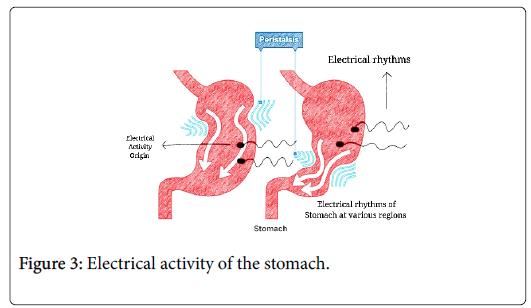
The electrical activity of the stomach that is initiated by the ICC is the essential component in the gastric functions. This can be captured and reconstructed into useful diagnostic functional information. The electrogastrogram is a function of intensity of the gastric actions per unit time. It varies depending upon the area which is considered based on its activity. Figure 3 shows the electrical activity at different regions of the stomach [5].
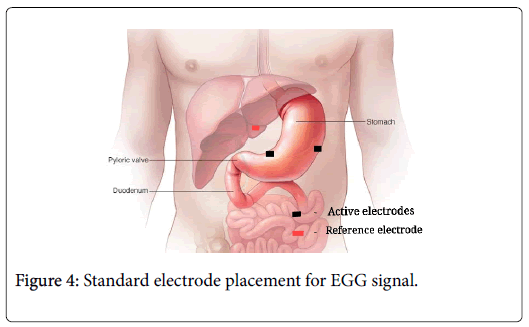
These gastric potentials are very sensitive. To get a good quality signal, one active electrode should be placed approximately 10 cm from the umbilicus and 6 cm to the patient's left. The second active electrode should be placed approximately 4 cm above the umbilicus on the midline of the abdomen.
The reference electrode is placed 10 to 15 cm to the right of the midline electrode, usually along the mid clavicular line and 2 to 3 below the lowest anterior rib on the right side (Figure 4) [5].
Signal acquisition
The electrodes placed on the abdomen captures the electrical signal and provide the functional information of the GI tract. The signal acquired will be feedback to the PIC microcontroller which serves as the reference for gastric stimulator [6-8].
Responsiveness of the Stomach
The Stomach will produce a movement in response to the stimulus from the ICC. This gastric motility is the important in the phase of digestion. The delayed gastric emptying has been a resultant from many causes such as from an accidental damage to vagus nerve and some idiopathic causes. The diabetic and Parkinson’s patients can also be a victim.
Thus, developing the gradual unresponsiveness and causing several symptoms such as chronic nausea, vomiting (especially of undigested food), abdominal pain, Gastroesophageal reflux (GERD), heartburn, lack of appetite, spasms of the stomach wall, constipation or infrequent bowel movements, weight loss and malnutrition. The gastric electrical stimulation can provide treatment for gastroparesis which controls the condition and help in reducing the progression of complications.
Proposed Methodology
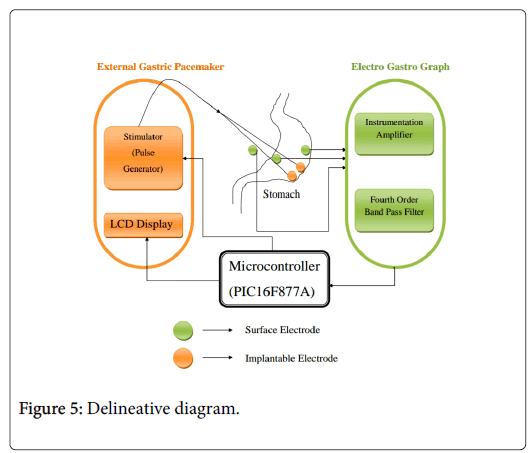
Biofeedback is a technique used here to treat the gastroparesis disease, where the gastric stimulation is given to the patient with the feedback from gastric potential via electrogastrograph. The unique objective is to provide an effective treatment for gastroparesis by the help of their own Gastric Signals rather than asynchronous stimulation with the help of timers. The PIC microcontroller is used to integrate the electrogastrograph and the gastric stimulator.
The delineative diagram (Figure 5) describes the integration of those sub systems i.e., electrogastrograph and external gastric pacemaker and an interface.
Electrogastrograph
Electrogastrograph can provide a real-time diagnosis helps in improving the treatment through the Stimulator by using it as a biofeedback. The electrogastrogram replicates the stomach activity at every instance which is recorded and used to provide synchronous and regulated stimulation.
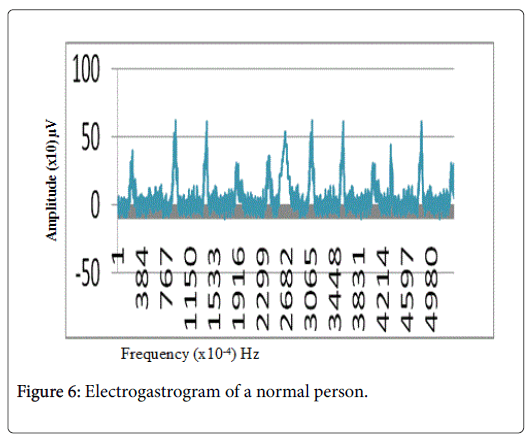
EGG is an integral unit of electrodes, amplifier, filter unit and a processor to record the electrical activity of the gastric cells. This is the only method that exactly reproduces the functional information of the gastro-intestinal organs which can help in diagnosing the gastric diseases. The Figure 6 shows the electrogastrogram of a normal person.
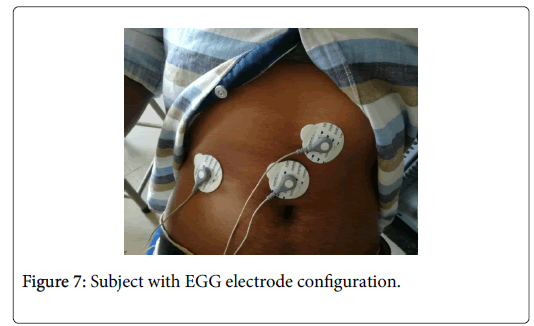
Surface Electrodes: High-quality, fresh and disposable electrodes such as those used for electrocardiogram (EGG) recording are recommended. To minimize artifacts in the EGG recording caused by the movement, it is best to use electrodes that adhere very well to the skin (Figure 7).
Instrumentation Amplifier: A high-quality recording system is needed to amplify and process the 100 to 500 micro volts EGG signal that ranges from 1.0 to 15.0 cpm.
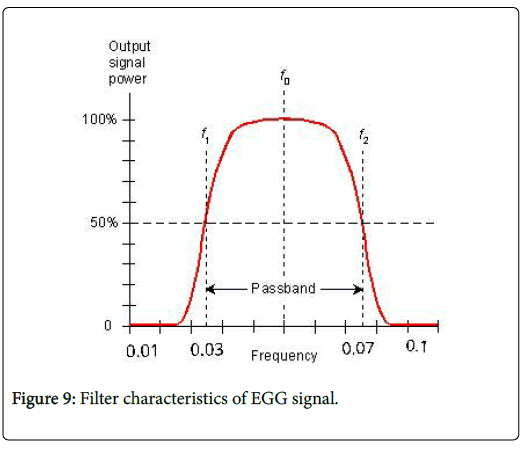
Band Pass Filter: The desired frequency range of normal gastric signal is 0.05-0.11 Hz, in order to eliminate the contamination of the signals fourth order band pass filter with appropriate cut-off frequencies is used.
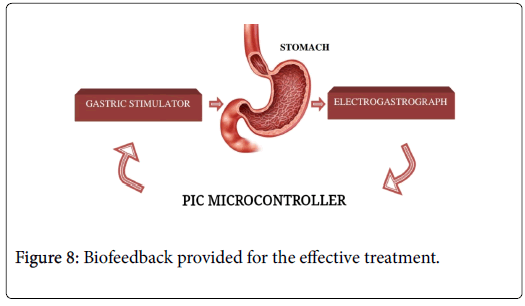
PIC microcontroller
It is used to integrate the electrogastrograph and gastric pacemaker. It uses PIC star plus software to detect the peaks in gastric potential for appropriate stimulation (Figure 8).
Gastric Pacemaker
Gastric electrical stimulation (GES)
Gastric electrical stimulation is the only method to treat gastroparesis effectively. It improves the stomach activity and partially retains the actual function of the stomach from gastroparesis [9]. The electrogastrogram of a normal person has 3 to 3.5 cpm rather gastroparesis patient has an EGG with reduced frequency that is less than 2 cpm due to delayed gastric emptying (Figure 9). GES is provided with a high frequency i.e. 12 cpm and a pulse width of 300 microseconds [10]. Gastric pacemaker is like a cardiac pacemaker in size and also implanted through laparoscopy surgery. The procedure takes 2 to 3 hours under general anesthesia. There are two intramuscular lead wired electrodes are associated with stimulator to provide mild electrical stimulation.
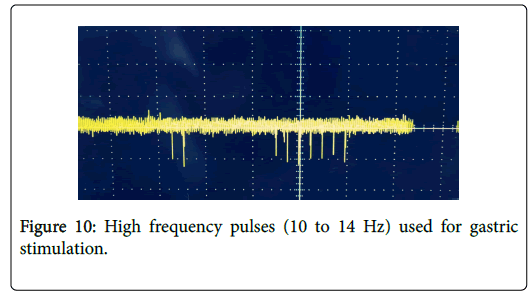
Figure 10 shows the pulses that are delivered to the stomach which is affected by gastroparesis.
Gastric Pacemaker
It will provide the gastric electrical stimulation to the gastric muscles via the feedback from electrogastrograph [11].
Stimulator (Pulse Generator): Gastric pacemaker is solely works with the help of pulse generator, which is programmed to deliver different frequencies depends on the patient risk. Generally, gastroparesis patient needs 10 to 14 Hz frequency for gastric muscle stimulation.
LCD Display: LCDs are available to display the frequency which is delivered to the patient when the trigger is ON. It is interfaced with PIC microcontroller to get the trigger pulse from the pulse generator.
Integration
The electrogastrograph will record the gastric potential using normal surface electrode on the abdomen. The output from EGG will fed to PIC microcontroller for peak detection process; where gastric stimulator is already connected to controller to deliver the high frequency. If the desired condition is satisfied with the input signal from the EGG, then the stimulation will be provided to patient. The general condition is three peaks, if it’s achieved; stimulation is not given to patient. If the patient input gastric signal holds less than two peaks, then stimulation of 14 Hz is given to patient. These Conditions are preloaded to PIC Controller using appropriate coding [12,13].
Electrode configuration of stimulator
The electrode configuration of a stimulator is difficult to test practically. The EGG requires the placement of electrodes noninvasively hence the determination for the best configuration can be assessed by the trial and error method rather the stimulator requires the placement of electrodes internally hence the configuration cannot be regulated. So, the ideal configuration and practical configuration are explained below.
Ideal configuration
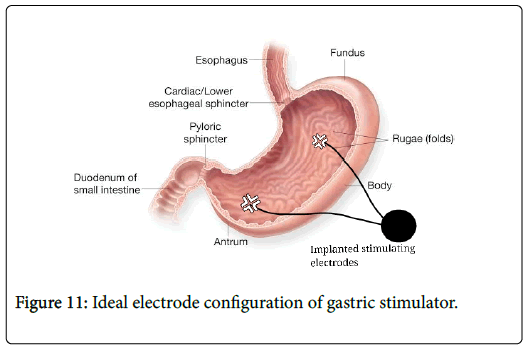
Three bipolar electrodes were implanted: one in the fundus, one in the anterior antrum, and one in the posterior antrum (Figure 10 for electrode configuration). Each electrode was made of an 18 mm long, 0.5 mm diameter platinum-iridium coil coated with titanium nitride. In the clinical trial the electrodes were connected to the implantable device, which performed both the detection and the stimulation tasks. The device was implanted subcutaneously on the left side of the abdomen (Figure 11). This implantation procedure is done by normal laparoscopic surgery of 2 to 3 hours [14].
Proposed configuration
Invasive implantation of electrode i.e., stimulating electrode is done through laparoscopy and so the testing cannot be performed. Here, it uses two electrodes. One is an active electrode and another is a reference electrode. The stimulation should be provided over the corpus and antrum regions of the stomach [15].
Work Flow
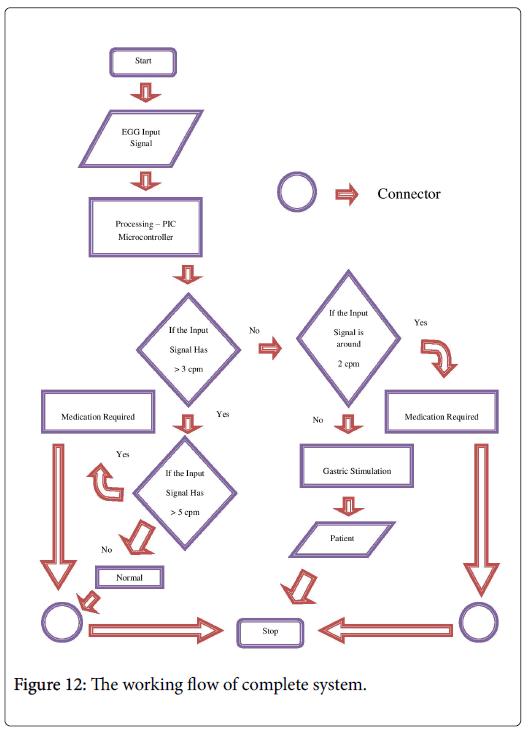
The flowchart shown in Figure 12 depicts the work flow of the complete system and the detailed explanation is as follows:
• The patients who suffer from gastric problems are provided with the diagnostic setup which examines by acquiring the gastric electrical signals (EGG).
• The signal is then assessed for any physiological changes by a processor (PIC16F877A).
Condition 1: The signal with the number of cycles in a minute greater than 3 is declared as normal.
• The signal which satisfies this will be proceeded to further evaluation (Conditional check 2) and the signal that fails in this check will be declared as abnormal and proceeded to make a decision (Conditional check 3) of which kind of treatment is advisable to the patient.
Condition 2: The signal is checked here for the normal gastric rate (should be less than 3 cpm) and also examines whether there is any kind of hyper-actions.
• The signal that falls under the former condition will be declared as completely normal and the latter will be declared as abnormal and they are advised to take up a medical examination.
Condition 3: The signal is checked here to make a decision between which kind of treatment is recommended to the patient.
• The patient with mild effect (i.e., who have around 2 cpm) will be advised to take up a doctor’s advice and who have severe effect (i.e., who have less than 1 cpm) will be advised to take up a treatment through our gastric stimulator.
Result
The outcome of the proposed methodology provides the synchronous stimulation to the stomach. Thus the device provides an effective treatment for gastroparesis with fewer complications. The Figure 13 shows the typical working prototype of our proposed device.
Rather the gastric electrical stimulation which provides it as asynchronous, this rehabilitation tool can provide it in synchronous mode without competing with the natural stimulus. Thus, the tool helps in restoring back the gastric function by overcoming the stomach’s uncertainty.
The overall performance of the prototype is evaluated using the pulse generator that is connected to the prototype.
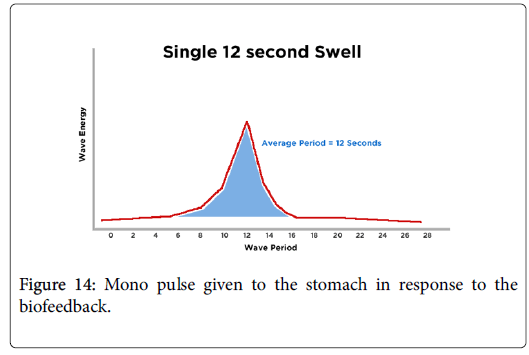
The device delivers the single mono pulse for the period of 20 Seconds (Figure 14). This recovers back the actual electrical characteristics of the stomach of gastroparesis patient. After delivering the processed EGG to the PIC microcontroller, the coding that is uploaded in the controller examines the peaks on the input signal. The recognized peaks are evaluated and cross verified with the conditions that we declared with respect to the physiology and functional topology of the stomach [16,17].
The appropriate stimulation with the appropriate period will be provided based on the assessment made from the diagnosis. The controller serves as a regulator that decides the functioning of the stimulator. It switches the stimulator between two states either ON or OFF. If the stimulator is decided to be ON, it delivers the frequency of 14 Hz i.e., high frequency stimulation is provided via the stimulating electrodes implanted on the stomach. The stimulation status is displayed on the LCD screen and the stimulation pulses can be viewed through the digital oscilloscope (Figure 10) if the appropriate terminal is connected to it. The following Figures 15 and 16 show the type of stimulation provided according to the status of the microcontroller. This helps in keeping the stimulator as ON or OFF.
The stimulator is kept OFF by the PIC microcontroller, if the gastric motility is normal when examining through the electrogastrograph. The stimulator remains intact and leaves the natural functions undisturbed rather providing unwanted stimulation and resulting in an irreversible damage.
The stimulator is kept ON and provides appropriate stimulation, if gastric delayed emptying is detected when examining through the electrogastrograph. The stimulation can be provided with the current of frequency of 14 Hz through the stimulating electrode for that instance of a particular period of 1 minute [18,19]. The high frequency stimulation offers the stimulus to the stomach when the natural stimulus is not so effective for the proper functioning of the stomach. The competitive stimulation is completely eliminated with the help of the feedback by the analysis of the electrical activity of the interstitial cells of cajal with respect to the responsiveness of the stomach at every instant in real time [20].
Inference
The plot in the Figure 6 is an electrogastrogram in the digital values showing the recording over a period of 4 minutes and 15 seconds.
The stimulator provides the stimulation of 14 Hz with an onset of the trigger from EGG module. The Stimulation is not produced when the diagnostic module finds the normal gastric actions i.e., the electrogastrogram obtained is having more than 2 cpm. This is depicted in Figure 15. The stimulation is produced only when the diagnostic module finds it necessary.
The stimulation can be provided with the current of frequency of 14 Hz through the stimulating electrode at that particular period of 1 minute. This is depicted in Figure 16.
Conclusion
The Project provides an effective treatment to the Gastroparesis. The Gastric Electrical Stimulation is a method that compensates the effect of the disease by providing a high frequency over the surface of the stomach through the implanted electrodes. Gastroparesis is a disease which paralyzes the stomach; the sufferers cannot digest the food properly due to the delayed gastric emptying. The stimulation can only be provided when the Gastric emptying is required which promotes synchronous stimulation. Rather the existing stimulator provides continuous stimulation once it’s triggered after a bolus feedback that can stress the gastric muscles over its regular contraction.
The ceased gastric contraction retains the intake food in the stomach that cannot be able to propel down to the intestine. The patient with GP can’t even able to digest a small amount of food and result in vomiting. They may suffer from several severe symptoms and lack of nutrition. They can be provided with different kind of treatment methods based on the severity but the ultimate and effective method is the gastric electrical stimulation by the analysis of interstitial cells of cajal. The inclusion of diagnostic module can provide synchronous stimulation which eliminates the further worsening of the disease (i.e., may cause fatigueless). Thus the intelligent stimulation can be provided by assessing the electrogastrogram and takes the decision between the different treatment methods to be suggested (i.e., medication based on the doctor’s advice or gastric electrical stimulation).
References
- Gopu G, Neelaveni R, Porkumaran K (2010) Non-invasive technique for acquiring and analysis of electrogastrogram. IJCA 2: 73-76.
- Jing Ma, Christopher K (2009) Diabetic gastroparesis: Diagnosis and management. Drugs 69: 971-986.
- Kenneth LK, Stern RN (2004) Handbook of electrogastrography. Oxford University Press. Oxford, New York.
- Haddab S, Laghrouche M (2009) Microcontroller: Based system for electrogastrography monitoring through wireless transmission. Meas Sci Rev 9: 122-126.
- Rossi Z, Forlini G, Fenderico P, Cipolla R, Nasoni S (2005) Electrogastrography. Eur Rev Med Pharmacol Sci 9: 29-35.
- Parkman HP, Hasler HL, Barnett L, Eaker EY (2003) Electrogastrography: A document prepared by the gastric section of the American Motility society clinical GI motility testing task force. Neurogastroenterol Motil 15: 89-102.
- Aljarallah BM (2011) Management of diabetic gastroparesis. Saudi J Gastroenterol 17: 97-104.
- Altintop CG, Latifoglu F, Celikzencir E, Sezgin GC, Yurc A (2017) Determining of gastroparesis disease from electrogastrogram signals using cramer-rao lower bound and power spectral density. IU-JEEE 17: 3061-3067.
- Chen J (1992) A computerized data analysis system for electrogastrogram. Comput Biol Med 22: 45-57.
- Bortolotti M (2011) Gastric electrical stimulation for gastroparesis: A goal greatly pursued, but not yet attained. World J Gastroenterol 17: 273-282.
- McCallum RW, Chen JD, Lin Z, Bruce D (1998) Gastric pacing improves emptying and symptoms in patients with gastroparesis. Gastroenterol 114: 456-461.
- Soffer E, Abell T, Lin Z, Lorinczs A, Mccallum R, et al. (2009) Gastric electrical stimulation for gastroparesis: Physiological foundations, technical aspects and clinical implications. Aliment Pharmacol Ther 30: 681-694.
- Gopu G, Geethadevasena MS (2016) Electrogastrogram recovery for correction of gastric disorders using gastric stimulator. Circuits and Systems 7: 179-186.
- Mason RJ, Lipham J, Eckerling G, Schwartz A, DeMeester TR (2005) Gastric electrical stimulation: An alternative surgical therapy for patients with gastroparesis. Arch Surg 140: 841-846.
- Health Quality Ontario (2006) Gastric electrical stimulation: An evidence-based analysis. Ont Health Technol Assess Ser 6: 1-79.
- Soffer E (2012) Gastric electrical stimulation for gastroparesis. J Neurogastroenterol Motil 18: 131-137.
- Pasricha PJ, Camilleri M, Hasler WL, Parkman HP (2017) Gastroparesis: Clinical and regulatory insights for clinical trials. Clin Gastroenterol Hepatol 15: 1184-1190.
Citation: Gokul M, Durgadevi N, Bhuvaneshwari R, Vadivu VRS, Kumar CR (2018) Rehabilitation Tool for Gastroparesis by the Analysis of Interstitial Cells of Cajal (The External Gastric Pacmaker with a Feedback of Gastric Potential). J Gastrointest Dig Syst 8: 557. DOI: 10.4172/2161-069X.1000557
Copyright: © 2018 Gokul M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 10291
- [From(publication date): 0-2018 - Dec 09, 2025]
- Breakdown by view type
- HTML page views: 9235
- PDF downloads: 1056