Review Article Open Access
Spleen-Preserving Distal Pancreatectomy that also Preserves Splenic Vessels
Wataru Kimura*The First Department of Surgery, Yamagata University Faculty of Medicine, Japan
- *Corresponding Author:
- Wataru Kimura
Vice President, Professor and Chairman
The First Department of Surgery
Yamagata University, 2-2-2 Iida-Nishi Yamagata City
Yamagata, 990-9585, Japan
Tel: +8123-628-5334
E-mail: wkimura@med.id.yamagata-u.ac.jp
Received date: May 12, 2014; Accepted date: June 20, 2014; Published date: June 26, 2014
Citation: Kimura W (2014) Spleen-Preserving Distal Pancreatectomy that also Preserves Splenic Vessels. J Gastroint Dig Syst 4:191 doi:10.4172/2161-069X.1000191
Copyright: © 2014 Kimura W, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Spleen-preserving distal pancreatectomy is a common resection of the pancreas. Compared to distal pancreatectomy and splenrctomy Spleen Preserving procedure a limited resection. Recent advances in endoscopic surgery have resulted in more facilities offering laparoscopies SPDP.
Keywords
Spleen-preserving distal pancreatectomy; Splenic vessel preservation; Kimura method
Introduction
Spleen-preserving distal pancreatectomy (SPDP) is steadily becoming more common as a means of performing limited resection of the pancreas. Spleen preserving procedure a limited resection as compared to the distal pancreatectomy and splenrctomy, which procedure is very usuallry done. This surgical procedure is considered significant because it may prevent postoperative infection and pneumonia, while also blocking platelet count elevation. Kimura et al. [1,2] reported on “SPDP that also preserved splenic vessels,” deeming it as a safe and reliable surgical procedure. Since then, there have been several reports of cases in which this procedure was successfully performed.
Surgical procedures that preserve blood flow to the pancreas include the Kimura method [1,3], which preserves splenic vessels, and the Warshaw method [4], which resects splenic vessels and preserves short gastric vessels. When performing the Warshaw method, caution is required because of the significant possibility of postoperative splenic infarction, abscess, or gastric varix [5]. To reliably preserve the spleen, preserving splenic vessels is important [1]. In Japan, after a certain period of debate and gaining of experience, the trend of using this procedure is growing stronger. As the present report focuses on limited resection of the pancreas, it appears that greater preservation is offered by the Kimura method, which preserves splenic vessels, than the Warshaw method, which does not.
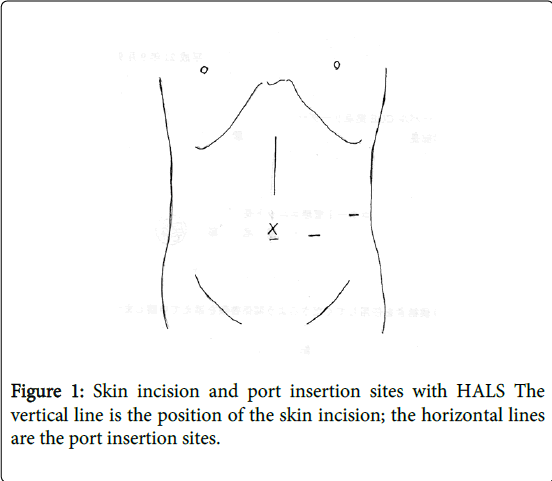
Furthermore, recent advances in endoscopic surgery have resulted in more facilities offering laparoscopic SPDP. Emphasizing safety and reliability, hand-assisted laparoscopic surgery (HALS) (Figure 1) is employed to ensure an optimal visual field until moving the pancreatic body and tail and detaching the splenic vessel under direction vision through the small incision of the laparotomy wound [6–8]. The number of facilities capable of performing a Kimura resection via HALS is gradually increasing.
Significance of spleen preservation
Spleen preservation is more highly evaluated in Western countries than in Japan. Spleen preservation reduces the onset of infections (e.g., pneumonia and septicemia) brought into the body, while inhibiting hematological abnormalities such as elevated platelet count [9–11]. Furthermore, it is believed to offer tumor immunity [12]. This study discusses a safe technique of splenic vessel preservation and SPDP for lesions in the pancreatic body and tail region.
The SPDP technique
Skin incision
An upper abdominal median incision is made up to 3 cm above the navel, and a transverse incision to the left is made at this same height, thereby creating an L-shaped incision. Alternatively, HALS can be used to gain a good visual field until moving the pancreatic body [13-17] (Figure 1).
Exposure of the anterior surface of the pancreas
The omentum is resected at the beginning of the transverse colon and the omental foramen is cut open to expose the anterior surface of the pancreas. This is continued down to the lower curve of the spleen, and the peritoneum around the outside of the spleen is resected.
Detachment of the pancreatic body and tail region from the retroperitoneum and moving the spleen
The peritoneum between the transverse mesocolon anterior lobe and the pancreatic capsule is resected transversely in line with the lower margin of the pancreas, and the retroperitoneum is opened up. The caudal pancreatic region is then separated from the retroperitoneum, after which the spleen is also separated from the retroperitoneum. As the pancreatic tail and splenic hilum are often quite deep, the splenorenal ligament is resected, and the spleen is moved from the retroperitoneum and brought to the front of the field of vision. If using HALS, the pancreatic tail and body region and spleen are brought outside the abdominal wall from the median small opening.
In small-bodied and slender patients, where a relatively good visual field is possible without moving the spleen, this procedure can be performed by resecting the pancreas first without moving the spleen. However, the authors generally move the spleen for this procedure. Moving the pancreatic body and tail region and splenic hilum to a shallow operative field allows for a good view of the back of the pancreatic body and tail region and a more reliable operation on the splenic vein. Furthermore, because the surgical site can be grasped with the left hand, surgery can be performed easily and safely.
Identifying the splenic vein
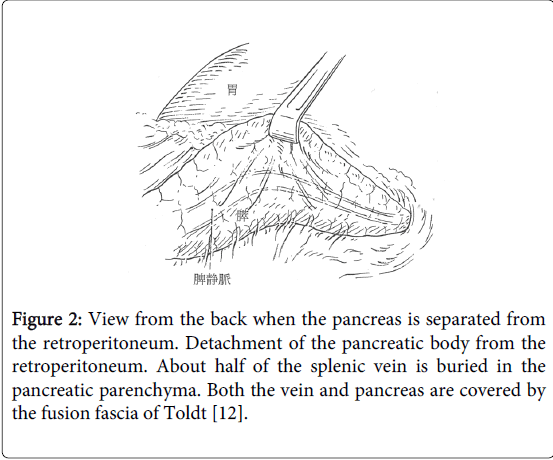
The splenic body and tail region are flipped over on the side of the pancreatic head, and the splenic vein, which is inside the loose connective tissue on the back of the pancreas, is identified. The splenic vein runs transversely through the back and middle of the pancreas and is found in the loose connective tissue membrane that covers the entire rear surface of the pancreas. At this juncture, the back of the splenic vein is visible on the abdominal side of Toldt’s fascia (Figure 2). As the splenic vein enters the pancreatic tail, it becomes covered in pancreatic parenchyma and may completely disappear from sight.
Dissection of Toldt’s fascia and exposure of the splenic vein
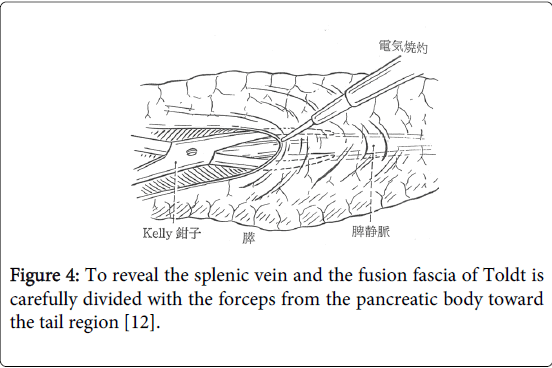
Kelly forceps are inserted between Toldt’s fascia and the surface of the splenic vein, which are gently separated from each other (Figure 3). Toldt’s fascia is dissected along the long axis of the splenic vein, thereby exposing the veins rear surface [1]. This procedure is then repeated until the pancreatic tail, exposing a long length of the splenic vein (Figure 4).
Tips for avoiding splenic vein damage (prevention)
The splenic vein is detached in the direction of the spleen from the planned pancreatic dissection line (Kimura method). It is difficult to detach the splenic vein going the other way (from the splenic end of the pancreatic tail toward the pancreatic body) because performing the operation in this direction can compromise conservation of the spleen. Negative consequences may occur because it is relatively difficult to distinguish fat tissue and pancreatic parenchyma in the splenic hilum. Moreover, in this area, the splenic vein has already divided into multiple branches that may be damaged or accidentally ligated/resected [1,2]. If this occurs, the main trunk of the splenic vein in the splenic hilum will become thinner, limiting venous perfusion. This lack of venous perfusion to the spleens periphery may cause splenic infarction, making it impossible to conserve the spleen.
Although SPDP had been used as a surgical procedure in the past, it had not attracted much attention. SPDP’s popularity showed a marked rise after our 1996 report outlining this surgical approach, whereby the splenic vein is separated from the duodenum to the spleen. Thus, this procedure, including the present method, has come to be called the Kimura method.
Dissection of splenic vein branches (prevention)
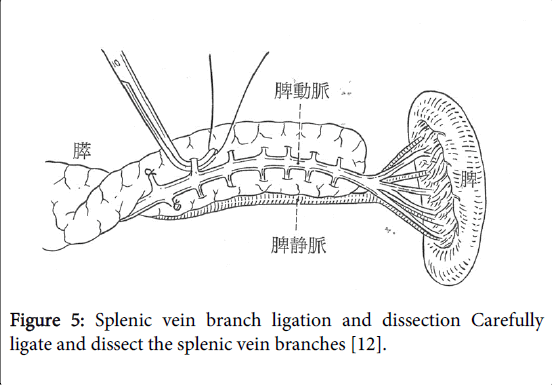
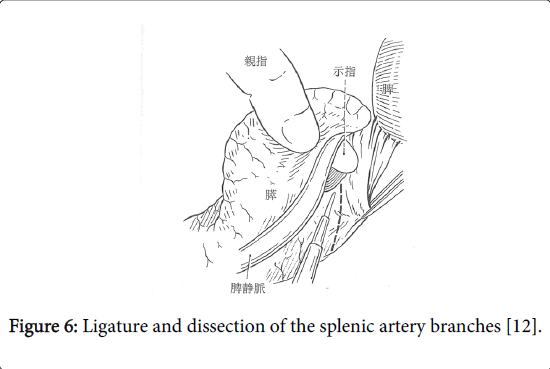
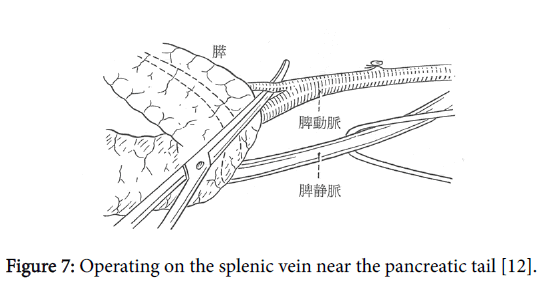
The splenic vein branches are carefully ligated and dissected (Figure 5). Most of the front half of the splenic vein is embedded in the pancreatic parenchyma, and many branches extend above and below at right angles. While carefully ligating and dissecting these branches one by one, the splenic vein is separated from the pancreatic parenchyma toward the splenic hilum (Figures 6 and 7). In a normal pancreas with no inflammation, it is easy to expose these branches by a few millimeters or more from the main splenic vein trunk.
This part of the procedure must be performed very carefully when strong or chronic inflammation is present.
How to respond to splenic vein damage
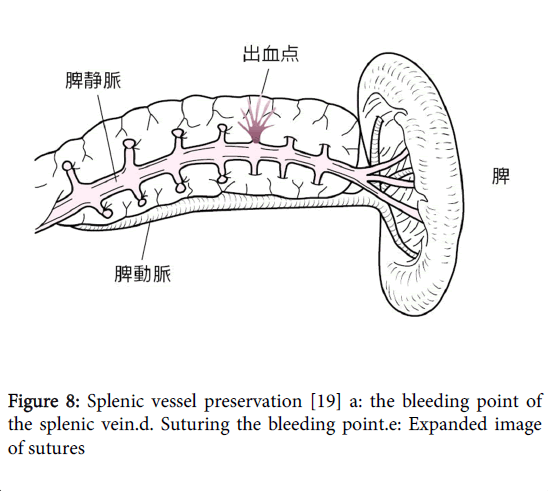
If the vein root is damaged, one must either perform astriction or apply fibrin glue to the area and take a wait-and-see approach (Figure 8). The surgeon must not attempt to immediately stop the bleeding by suturing the vein. The vein may be repaired after stopping the bleeding with one of the aforementioned methods.
If any splenic vein branch is pulled out and damaged, the situation is slightly more serious. If this occurs, the first choice for treatment is astriction to try to stop the bleeding, although this is not always successful. If astriction fails, bulldog forceps are applied to both sides of the damaged part of the splenic vein to stop the bleeding, and the area is then closed with a running suture using PROLENE sutures.
Treating the splenic hilum
Whereas splenic vessels are split into numerous branches in the splenic hilum, the pancreatic tail can be easily separated from the splenic hilum if the aforementioned procedure is performed in keeping with the relationship between the pancreatic parenchyma and splenic vein, with minimal risk to the multiple branches. With respect to the relationship between the splenic hilum and pancreatic tail, pancreatic tail is found in the center of the splenic hilum in 50% cases, in the head in 8% cases, and in the tail region in approximately 42% cases.
Separation of the splenic artery and pancreas
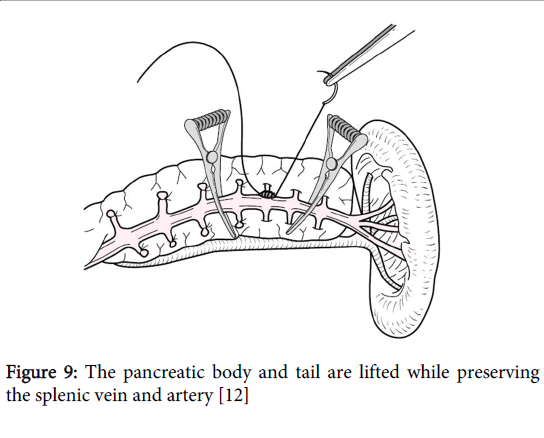
After separating the pancreatic parenchyma from the splenic vein up until the splenic end of the pancreas, the splenic artery is separated from the pancreas from this area toward the duodenum side (Figure 9). Even when drawing near the root of the splenic artery, there are a few artery branches to the pancreas that only extend toward the tail side, making it much easier to separate these branches than those of the splenic vein. If these branches are properly taken care of, the splenic artery is easy to separate because the rest of it is only lightly attached to the pancreas via loose connective tissue.
Dissection of the pancreas
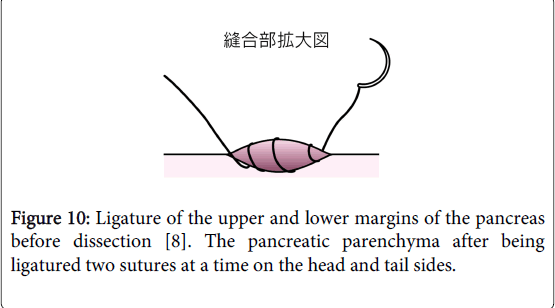
Before dissecting the pancreas, double ligature of the transverse pancreatic artery and superior transverse pancreatic artery, along with the pancreatic parenchyma, can minimize arterial bleeding during pancreatic dissection (Figure 10).
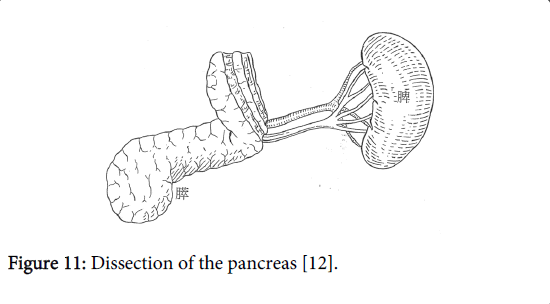
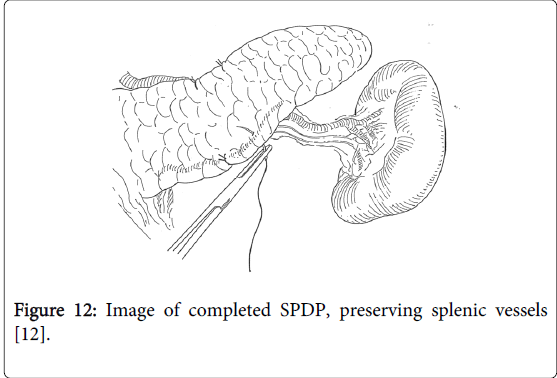
The pancreas is dissected perpendicularly to the long axis (Figure 11), and the pancreatic duct is identified. The pancreatic duct is securely ligated, and the pancreatic stump is closed with knotted sutures (Figure 12).
Drain placement
Two PHYCON water seal drains are placed facing the splenic hilum from the pancreatic stump. The PHYCON drains are of the water seal, closed type.
Conclusion
The most serious complication of SPDP was the possibility of pancreatic juice leakage from the pancreatic stump melting the exposed splenic vessel walls (the venous wall in particular) and causing massive hemorrhage. However, this did not occur in any of our cases, even in those that developed pancreatic fistulae. We also considered the risk of torsion of splenic vessels; however, because we are always careful to position the spleen back in its exact original position, we have never experienced a case where this occurred. SPDP that preserves splenic vessels is a simple surgical procedure that can be performed safely and reliably. We believe the procedure described will come to be more commonly selected and widely used.
References
- Kimura W, Inoue T, Futakawa N, Shinkai H, Han I, et al. (1996) Spleen-preserving distal pancreatectomy with conservation of the splenic artery and vein. Surgery 120: 885-890.
- Kimura W, Mitsuhiro Yano, Shuichiro Sugawara, Shinji Okazaki, Tamie Sato, et al. (2010) (Spleen-preserving distal pancreatectomy for benign lesions of the pancreatic body and tail region. Shujutua 17: 813-823.
- Kimura W (2009) Splenic vessel and spleen-preserving distal pancreatectomy (the Kimura’s method), important points and blind spots in surgery of the pancreas and spleen, Kimura W (ed.), 2nd edition, Bunkodo, Tokyo.
- WarshawAL (1988) Conservation of the spleen with distal pancreatectomy. Arch Surg 123:550-553.
- Miura F, Takada T, Asano T, Ochiai T, et al. (2005) Hemodynamic changes of splenomegaric circulation after spleen-preserving pancreatectomy with excision of splenic artery and vein.Surgery 138:518-522.
- Kimura W (2009) The significance of spleen-preserving distal pancreatectomy. Rinshou-Geka 64: 437–440.
- Tezuka K(2010) Distal pancreatectomy (spleen-preserving). Shujutu 64: 617–622.
- Kimura W (2008) Pancreatectomy for IPMN. Spleen-preserving caudal pancreatectomy. Shoukaki-Geka 31:1081-1091.
- Malangoni MA, Dillon LD, Klamer TW, Condon RE (1984) Factors influencing the risk of early and late serious infection in adults after splenectomy for trauma. Surgery 96: 775-783.
- Kimura W, Yano M, Sugawara S, Okazaki S, Sato T, et al. (2010) Spleen-preserving distal pancreatectomy with conservation of the splenic artery and vein: techniques and its significance. J HepatobiliaryPancreatSci 17: 813-823.
- Tezuka K, Kimura W, Hirai I, Moriya T, Watanabe T, et al. (2012) Postoperative hematological changes after spleen-preserving distal pancreatectomy with preservation of the splenic artery and vein. Dig Surg 29: 157-164.
- Sugimachi K, Kodama Y, Kumashiro R, Kanematsu T, Noda S, et al. (1980) Critical evaluation of prophylactic splenectomy in total gastrectomy for the stomach cancer. Gann 71: 704-709.
- Kimura W (2007). Spleen-preserving caudal pancreatectomy: indications and techniques, Surgery 61: 879–885.
- Kimura W (2003) Spleen-preserving distal pancreatectomy: indications and techniques. Surgery 65: 1676-1681.
- Kimura W (2008) Surgical treatment for pancreatic endocrine tumors. Journal of the Japan Pancreas Society 23: 703-709.
- Moriya T (2007) Surgical indications and treatment outcomes for cystic pancreatic lesions other than IPMN. The Journal of the Japan Surgical Association 62: 1665-1669.
- Kimura W (2012) Splenic vein damage during sple en-preserving distal pancreatectomy. The Journal of the Japan Surgical Association 67: 224-229.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 16562
- [From(publication date):
June-2014 - Sep 01, 2025] - Breakdown by view type
- HTML page views : 11839
- PDF downloads : 4723