Spontaneous Coronary Artery Dissection of the Multiple Coronary Arteries Rare Case Report
Received: 06-Jan-2016 / Accepted Date: 06-Feb-2016 / Published Date: 13-Feb-2016
Abstract
Spontaneous coronary artery dissection is a rare and unusual cause of acute myocardial infarction and sudden cardiac death. A 46-year-old man with history of Hypertension and smoking since from past 15 years, presented with angina. He had a positive Cardiac Troponin levels, and coronary angiography showed dissection of all major coronary vessels. Spontaneous coronary artery dissection (SCAD) is a rare cause of myocardial infarction (MI) and sudden cardiac death. Women, especially in the postpartum period, appear to be more commonly affected than men. The most common mode of presentation is that of sudden onset myocardial ischemia in the absence of any previous history of heart disease. The present rare case reports a middle aged man who presented with anginal chest pain and coronary angiography showed coronary dissection of all major coronary vessels.
Keywords: Angina; Angiography; Coronary artery; Dissection; Spontaneous coronary dissection
77836Introduction
Spontaneous coronary artery dissection (SCAD) is a rare entity, the overall incidence on coronary angiographies is around 0.2% [1-4]. The mean age of presentation is 42 years, with three-quarters of cases reported in women, of which 30% are peripartum [5]. Coronary atherosclerosis and the peripartum period are most commonly associated with the development of SCAD [6]. Other predisposing factors that have been reported include connective tissue disorders (Marfan’s syndrome, Ehlers-Danlos syndrome), vasculitis (for example, polyarteritis nodosa, systemic lupus erythematosus and eosinophilic arteritis), antiphospholipid antibody syndrome and inflammatory bowel disease [6]. Conditions associated with coronary shear, such as severe systolic hypertension, cocaine use are also the causes of SCAD. The clinical presentation of SCAD depends largely on the degree of compromise of myocardial blood flow, with most patients presenting with an acute coronary syndrome [5]. Undiagnosed or untreated cases may present in extremis with tamponade, cardiogenic shock or even sudden cardiac death [5].
Etiology And Pathogenesis
The precise etiology of SCAD is multifactorial, complex, and largely unknown. Dissection during pregnancy may be due to changes in the media due to increasing hormone levels, in addition to the shear stress present during labor. In addition to damage to the media, the hormonally induced changes in pregnancy have included fragmentation of reticulin fibers, the loosening of ground substance, and the hypertrophy of smooth muscle, which in combination may significantly increase the risk of dissection. Due to these factors, multiparous women appear to be at greater risk of developing SCAD. Vasculitis has been noted in several cases. The presence of eosinophilic infiltrates, periarteritis-like adventitial changes, tissue-damaging granule components, and the close interaction between eosinophils and degraded collagen have been well documented. Coronary artery dissection can occur secondary to atherosclerosis after rupture of a plaque or vasa vasorum. Nevertheless, some authors have suggested that atherosclerosis itself may prevent SCAD via a stenting effect, whereby scarring and atrophy of the media prevents extension of the dissection and may be associated with improved collateral circulation. Other conditions associated with SCAD include the following: systemic lupus erythematosis, hypersensitivity angiitis, blunt chest trauma, intense physical exercise, sarcoidosis, mitral stenosis secondary to rheumatic coronary arteritis, fibromuscular dysplasia, cocaine use, old age with and without CAD, cardiopulmonary resuscitation, copper deficiency causes, apical hypertrophic cardiomyopathy and cryoglobulinemia associated with hepatitis C virus, and hypertension. We illustrate below the rare case of a 46-yearold man with history of hypertension presented with angina secondary to SCAD involving multiple coronary arteries.
Case Presentation
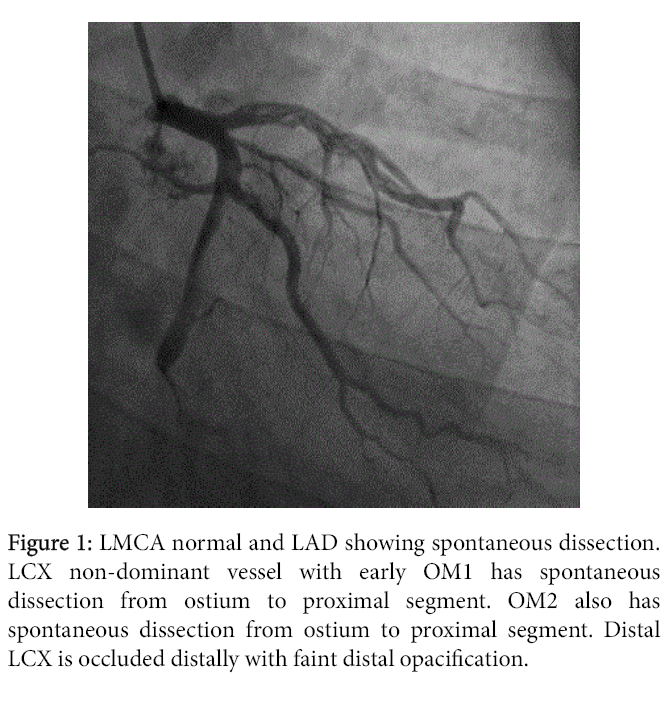
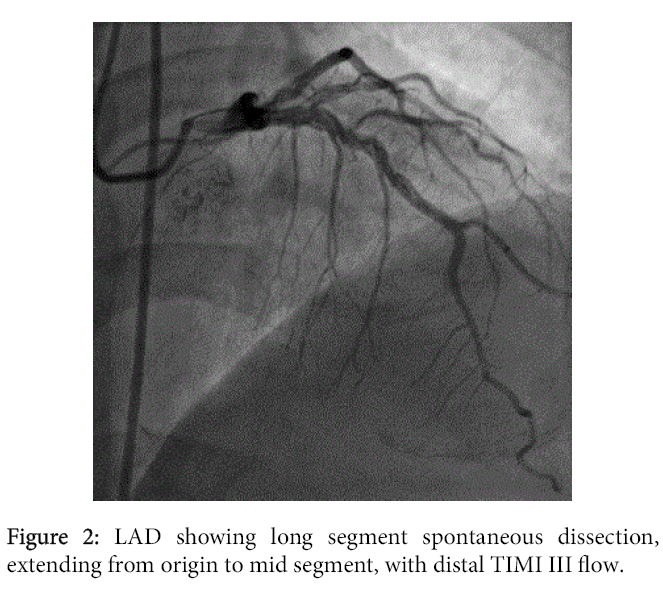
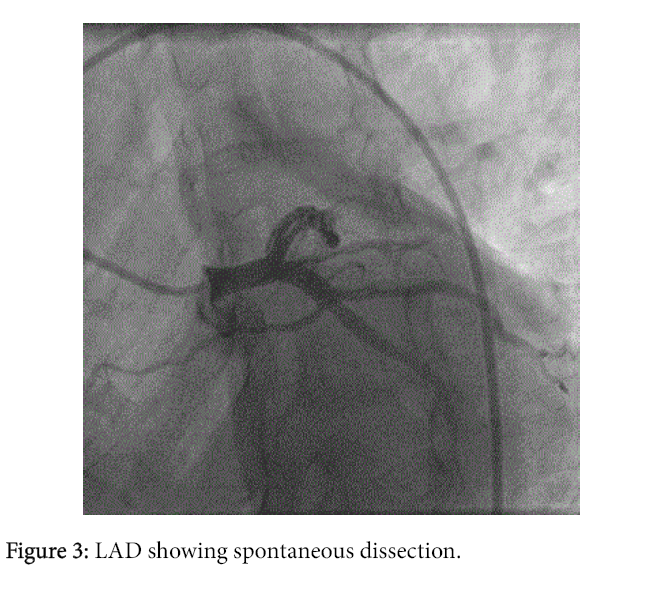
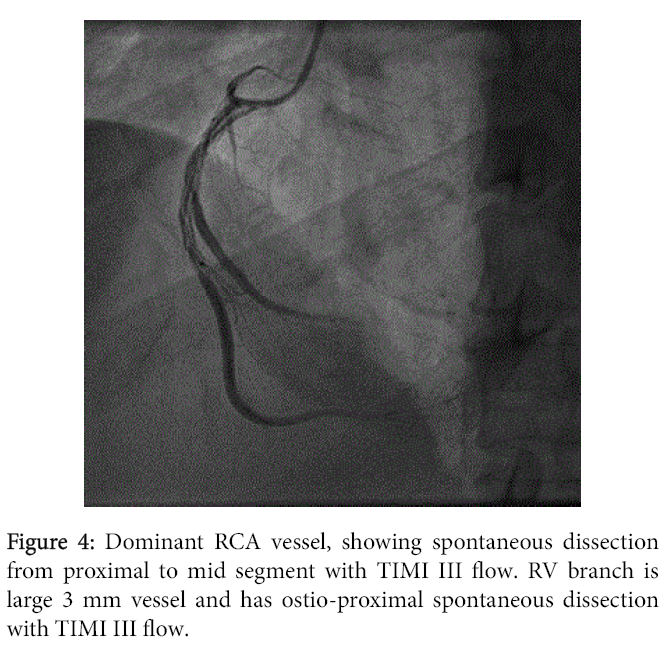
A 46-years-old man with history of Hypertension and smoking with no family history of heart disease presented to emergency department with retrosternal chest pain. An initial electrocardiogram was normal (Figure 1), with a troponin T levels of 2.01 ng/ml. He was treated with aspirin, clopidogrel, statin, heparin, beta blockade and statin. His symptoms relieved after the medications. Cardiac catheterization was performed, the angiogram showed the following lesions showing in the (Figures 2-4) LMCA was normal, LAD: Type 3, 3.5 mm vessel, has long segment Spontenous dissection extending from origin to Mid segment, with distal TIMI 3 flow. LCX: Non-dominant, Early OM1 is 1.5 mm vessel and has Spontenous dissection from Ostium to Proximal segment. OM2 is large sized vessel of 2.75 mm vessel and has Spontenous dissection from the ostium to proximal segment with TIMI 3 flow. Distal LCX continues as OM3 and occluded distally with faint distal opacification. RCA: Dominant and has Spontenous dissection from proximal to mid segment with TIMI 3 flow. RV branch is large 3 mm vessel, and has Ostio-proximal spontenous dissection with TIMI 3 flow (CAD-TVD, With Spontenous Dissection of LAD, OM1, OM2, RCA, RV Branch).
Discussion
SCAD is a rare cause of ischemic heart disease. In the majority of cases the diagnosis is established angiographically during or after an episode of acute coronary syndrome [7-10]. Coronary dissection can be associated with atherosclerotic coronary artery disease, aortic root dissection or it may be a secondary injury produced by blunt chest trauma. Other reported associations include cystic medial necrosis and Ehlers-Danlos syndrome, and in some cases it is idiopathic. The pathology is that of an intramural hematoma that expands and produces an acute coronary syndrome. Reports of SCAD simultaneously involving all three coronary arteries are exceptional and limited to very few case reports [11-17].
The treatment of acute MI subsequent to coronary dissection is controversial. Because thrombolysis can expand the intramural hematoma and extend the dissection, it can be catastrophic. After the initial management of the acute condition, subsequent treatment options are also controversial. There are several reports [18] of CABG in patients with spontaneous coronary dissection, particularly in those with left main stem involvement or multivessel dissections. It is important to note that literature suggests that CABG in SCAD patients may be hazardous because of the chance of dissection progression through the venous and arterial conduits or into the distal part of the grafted vessels. Many reports recommend that this type of revascularization should be reserved for patients in whom aggressive medical treatment fails. Longheval, et al. [19] report a good prognosis following healing of dissections, so there is a scope for medical treatment. Several recent studies have reported stent placement for the treatment of SCAD [20]. The results were good, with reportedly low rates of restenosis; however, this treatment should be reserved for localized dissection.
The present case poses problems when the type of revascularization is considered. Because of the widespread nature of the dissection, both CABG and the positioning of coronary stents would be difficult. So patient was considered for optimal medical management. The present case was reported because of the presentation and unique angiographic images.
Conclusion
SCAD is a rare, multifactorial and complex disease which occurs predominantly in young, otherwise healthy subjects. Its presentation may vary from unstable angina to sudden cardiac death. In the acute phase primary PCI remains the reperfusion strategy of choice; however, in small and medium-sized arteries with normalised TIMI flow conservative treatment is defendable. While in-hospital mortality is low regardless of initial treatment, PCI is associated with high rates of complication. Spontaneous coronary artery dissection should be considered in any young woman with no risk factors for coronary artery disease and acute myocardial infarction. Given the propensity for extension of dissection with or without mechanical revascularization, and documentation of spontaneous healing, medical therapy remains a rational approach. Depending upon hemodynamic stability, however, it is recognized that therapy must be individualized.
References
- Verma PK, Sandhu MS, Mittal BR, Aggarwal N, Kumar A, et al. (2004) Large spontaneous coronary artery dissections – a study of three cases, literature review, and possible therapeutic strategies. Angiology 55: 309-318.
- Mohamed HA, Eshawesh A, Habib N (2002) Spontaneous coronary artery dissection – a case report and review of the literature. Angiology 53: 205-211.
- Bac DJ, Lotgering FK, Verkaaik AP, Deckers JW (1995) Spontaneous coronary artery dissection during pregnancy and post partum. Eur Heart J 16: 136-8.
- Almahmeed WA, Haykowski M, Boone J, Ling H, Allard M, et al. (1996) Spontaneous coronary artery dissection in young women. Cathet Cardiovasc Diagn 37: 201-205.
- Sabatine MS, Jaffer FA, Staats PN, Stone JR (2010) Case records of the Massachusetts General Hospital. Case 28–2010. A 32-year-old woman, 3 weeks postpartum, with substernal chest pain. N Engl J Med 363: 1164–1173.
- Kamran M, Guptan A, Bogal M (2008) Spontaneous coronary artery dissection: case series and review. J Invasive Cardiol 20: 553–559.
- Verma PK, Sandhu MS, Mittal BR, Aggarwal N, Kumar A, et al. (2004) Large spontaneous coronary artery dissections – a study of three cases, literature review, and possible therapeutic strategies. Angiology 55: 309-318.
- Mohamed HA, Eshawesh A, Habib N (2002) Spontaneous coronary artery dissection – a case report and review of the literature. Angiology 53: 205-211.
- Bac DJ, Lotgering FK, Verkaaik AP, Deckers JW (1995) Spontaneous coronary artery dissection during pregnancy and postpartum. Eur Heart J 16: 136-138.
- Almahmeed WA, Haykowski M, Boone J (1996) Spontaneous coronary artery dissection in young women. Cathet Cardiovasc Diagn 37: 201-205
- Conraads VM, Vorlat A, Colpaert CG, Rodrigus IE, De Paep RJ, et al. (1999) Spontaneous dissection of three major coronary arteries subsequent to cystic medial necrosis. Chest 116: 1473-1475.
- Rensing BJ, Kofflard M, Van den Brand MJ, Foley DP (1999) Spontaneous dissection of all three coronary arteries in a 33-week-pregnant woman. Catheter Cardiovasc Interv 48: 207-210.
- Maresta A, Varani E, Balducelli M, Vecchi G (2002) Spontaneous coronary dissection of all three coronary arteries: A case description with medium-term angiographic follow-up. Ital Heart J 3: 747-751.
- Antoniucci D, Magi Diligenti L (1990) Spontaneous dissection of the three major coronary arteries. Eur Heart J 11: 1130-1134.
- Shroff G, Rajani R (2003) Spontaneous coronary artery dissection: An uncommon problem with a common presentation. Indian Heart J 55: 655-657.
- Rovner A, Thanigaraj S, Rogers JG, Moazami N, Lasala JM, et al. (2004) Spontaneous multivessel coronary artery dissection in a young asymptomatic patient. J Interv Cardiol 17: 123-127.
- Choi JW, Davidson CJ (2002) Spontaneous multivessel coronary artery dissection in a long-distance runner successfully treated with oral antiplatelet therapy. J Invasive Cardiol 14: 675-678.
- Yoshida K, Mori S, Tomari S (2000) Coronary artery bypass grafting for spontaneous coronary artery dissection: A case report and a review of the literature. Ann Thorac Cardiovasc Surg 6: 57-60.
- Longheval G, Badot V, Cosyns B, Najioullah S (1999) Spontaneous coronary artery dissection: Favorable outcome illustrated by angiograph data. Clin Cardio 22: 374-375.
- Verma PK, Sandhu MS, Mittal BR, Aggarwal N, Kumar A, et al. (2004) Large spontaneous coronary artery dissections – a study of three cases, literature review, and possible therapeutic strategies. Angiology 55: 309-318.
Citation: Madhu KJ, Subramani KSR, Prasad NM, Manjunath CN (2016) Spontaneous Coronary Artery Dissection of the Multiple Coronary Arteries – Rare Case Report. Cardiovasc Ther 1: 104.
Copyright: © 2016 Madhu KJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Usage
- Total views: 12783
- [From(publication date): 2-2016 - Jul 03, 2025]
- Breakdown by view type
- HTML page views: 11839
- PDF downloads: 944