Suicide Rates between Methamphetamine Users who inject versus Non-Injectors
Received: 20-Mar-2018 / Accepted Date: 11-Apr-2018 / Published Date: 18-Apr-2018 DOI: 10.4172/2155-6105.1000359
Abstract
Methamphetamine abuse has created a continuous wave of destruction and disparity throughout communities as its widespread usage increases on a momentary basis. With such proliferated abuse comes an invasion of poverty, crime, addiction, prostitution, venereal diseases and death; many of which occur by suicide. Whether its overdose, self-inflicted wounds or mere tragedy, death seems to be synonymous with methamphetamine abuse. Although somewhat limited, the previous research on methamphetamine has primarily focused on the physiological, neurological and social aspects of abuse. Furthermore, despite methamphetamine’s growing popularity, researchers have failed to develop a clear understanding of the inherent differences between users who inject versus noninjectors. Therefore, this study chose to explore the differences in suicide attempts between methamphetamine users who inject versus non-injecting users, while also examining additional demographic variables. The results of this study suggest intravenous methamphetamine use and suicide are strongly related; however, they have a peculiar relationship in the sense that intravenous users, who attempted suicide, were likely to make their first suicide attempt prior to their initial injection.
Keywords: Methamphetamine abuse; Suicide attempts; Injectors and non-injectors
Abbreviations
METH: Methamphetamine; IV: Intravenous, VIDUS: Vancouver Injection Drug Users Study
Introduction
Along with America’s plush and prodigious history comes the desolate devastation of its illicit infatuation with drug use. Over the last few decades, this infatuation has turned to methamphetamine (meth) use and has spread throughout the United States like wildfire [1]. In the 1960’s, California was considered to be the country’s center for methamphetamine production [2]; however, use of the drug has created problems in areas ranging from Hawaii [3,4], to the Southwest, Midwest and even some East Coast cities [5,6]. Meth use has become so prevalent outside the United States; it is now considered to be a global health problem and will likely remain so for years to come [7].
It is estimated approximately 11 million Americans have used meth on at least one occasion, with nearly 1.3 million Americans using meth in the last year and roughly 0.2-0.3% of the population using meth on a regular basis (using meth in the past month) [8]. Further research conducted by the National Survey on Drug Use and Health (NSDUH) indicated in 2012 there were “133,000 new meth users,” with the average age of new users being 19.7 years old (Substance Abuse and Mental Health Services Administration [9]. These numbers are alarming to say the least and as they continue to rise, so should societal concern.
Given these high and growing rates of meth, it is important to examine the impact of this drug on mental health. Research has clearly demonstrated deleterious effects of substance use on an individual’s mental health (e.g. dementia, depression, overall cognitive decline). Individuals who abuse illicit substances have been found to have increased rates of depression, anxiety, inpatient treatment and other cognitive deficits as compared to the general population [10,11]. Specifically, this study examined the relationship between routes of administration (injecting versus non-injecting) of meth and suicidality.
Meth use and suicide
Although research has failed to examine differences in the frequency of suicide attempts between meth users based on modes of administration, there has been some research which has highlighted the increased risk of suicide within the methamphetamine using population [12,13]. For example, studies on meth withdrawal have highlighted the increased risk of suicide attempts amongst users in their first 30 to 90 days of treatment [14]. Other researchers have found individuals addicted to meth were more likely to report depressive symptoms, psychotic processes and suicidal ideation than individuals denying dependence [15].
Marshall et al. [13] managed to examine individual differences between the participants in the Vancouver Injection Drug Users Study (VIDUS) who reported a suicide attempt. These researchers concluded 8% of participants reported a suicide attempt, resulting in an incident rate of 2.51 attempts per 100 participants. Based on this research, Marshall et al. were able to determine users who attempted suicide tended to be younger (median age: 35 vs. 40), were more likely to use intravenously, reported fewer years injecting (median number of years: 17 vs. 19) and were more likely to be female (48.3% vs. 35.1%). These researchers also found that when compared to periods of no meth injection, “infrequent meth injection was a predictor of attempting suicide, while frequent meth injection was associated with the greatest risk of attempting suicide”. Overall, Marshall et al. found intravenous meth users to be at the greatest risk for suicide, with an 80% higher likelihood of attempting suicide than other users. These researchers attributed this to “a combination of neurobiological, social and structural mechanisms”; while concluding meth injection should be regarded as a strong predictor for attempting suicide and treatment centers should conduct thorough risk assessments for such users.
Similar to the VIDUS study, Callor et al. [14] examined toxicology reports and the medical records of 442 individuals who committed suicide between 1996 and 2002 in Utah. These researchers found methamphetamine to be the most common substance in the blood and/or urine of suicide completers; thus, raising the possibility of an unrecognized correlation existing between meth use and suicide. When searching for an explanation, Callor et al. [14] concluded “among boys, the leading risk factor is a previous attempt, followed by depression, disruptive behavior and substance abuse”. The researchers believe meth use in these teenagers with suicidal ideations served as a catapult toward completing the act, once the decision had been made.
The research would lead one to assume intravenous meth users have a higher propensity of suicide, especially since they appear to suffer more physical, social and psychological difficulties. It also appears as if meth injectors face considerably more penuries than non-injecting users. IV-users appear to be ostracized, even within the drug using population, which may contribute to these individuals being the last to receive treatment, accommodations or any social services which may be available. Research suggests intravenous meth users are more likely to present with comorbid psychological difficulties, which may also contribute to suicidal and self-harming behaviours [14,15].
Summary and hypothesis/research questions
Methamphetamine abuse has significant harmful effects from neurological, behavioral and physical standpoints. Based on the literature surrounding this topic, there has been limited exploration into the suicidal tendencies of meth users based on modes of administration within the United States. From the research available, it appears intravenous drug user’s face more difficulties; however, only one study was found in which differences in suicide attempts between injectors and non-injectors was compared. Further exploration into this question is needed. Therefore, this study examined the relationship between meth use and factors pertaining to suicide.
Secondarily to the main objective of examining the relationship of injecting methamphetamine and suicidality, this study also examined demographic and individual history variables to determine if additional correlations between meth use and suicide exist. Such other variables included substance use history, mental health history, criminal justice system involvement, etc.
Methods
Participants
In order to obtain the desired information, this study was conducted at various drug treatment centers located throughout the Midwestern United States. Inclusion criteria involved having a history of methamphetamine use and being English speaking. Participants did not receive any form of compensation for their involvement with this study.
Overall, there were 28 participants (19 males, 9 females). The average age of participants was 33, with ages ranging from 18 to 63 (SD=9.97). The majority of the sample (71.5%) had obtained a 12th grade education or higher, with the mean of years of education being 12.4 (SD=2.39). The education levels of participants are outlined in Table 1, presented in the Results section. These participants were all adults (over the age of 18), who had a personal history of methamphetamine abuse and were actively involved in either outpatient or inpatient substance abuse treatment.
| Highest Grade Completed | Frequency | Percent |
|---|---|---|
| 8th Grade | 2 | 7.1 |
| 9th Grade | 2 | 7.1 |
| 10th Grade | 2 | 7.1 |
| 11th Grade | 2 | 7.1 |
| 12th Grade/High School Graduate | 4 | 14.3 |
| Some College | 11 | 39.3 |
| Associates Degree | 1 | 3.6 |
| Bachelor’s Degree | 3 | 10.7 |
| Graduate School | 1 | 3.6 |
Table 1: The education level of the participants broken down by frequency and percent, Education of participants, N=28.
Materials and Procedures
Data was collected using a questionnaire consisting of basic demographic information as well as information regarding the participant’s substance use. The questionnaire consisted of items asking gender, age and questions related to history of methamphetamine use and suicide attempts. There were also items aimed at one’s mental health history, education level, work experience, use of other substances and drug of choice. The items were written at an eighth grade reading level for ease of use and were written only in English. This questionnaire was developed by the primary researcher and was available in both electronic and paper forms(Table 2).
| Type of Work | Frequency | Percent |
|---|---|---|
| No Work History | 5 | 17.9 |
| Mental Health | 2 | 7.1 |
| Substance Abuse | 3 | 10.7 |
| Counselor | ||
| Business | 2 | 7.1 |
| Service Industry | 7 | 25 |
| General Labor | 9 | 32.1 |
Table 2: The work history for the participants, work history was separated into six categories based on the type of job reported, the substance abuse counsellors were not currently in treatment, despite these participants not being currently involved in treatment, they had a considerable history of methamphetamine abuse, however, the two participants who reported working in mental health were active in substance abuse treatment at the completion of the survey.
Results
In total, data were collected with 28 participants. While all participants had a history of methamphetamine use, 18 reported a history of intravenous methamphetamine use (12 males, 6 females). The average age for IV-users was 34.2 (SD=10.36), with ages ranging from 23 to 63. The average age for non-IV users was 31.3 (SD=9.44), with ages ranging from 21-46.
In regard to work history, 57.1% of participants reported being unemployed, while 42.9% reported having a job. Work history was separated into six categories based on the type of job reported (Table 2). The majority of the sample (57.1%) endorsed working in either “general labor” or the “service industry;” however, the most common types of jobs categorized as “general labor” were: factory/warehouse work, landscaping, truck driver and temp agencies. Meanwhile, the most frequent job types categorized as “service industry” included waitressing, store clerk, working fast food or retail.
Work history
As an aggregate, this sample averaged 6.2 arrests per person; however, there were notable differences between IV and non-IV cohorts. Out of the entire sample, only one individual denied ever being arrested; although, despite most participants experiencing multiple arrests, 82.1% of the participants denied ever going to prison. Based on the data collected, if a participant were to be incarcerated, it was most likely to be for a drug-related offense. The data collected in this study indicate most methamphetamine users in treatment have a history of multiple arrests. However, IV-users tended to have a much lengthier criminal record, including twice as many drug-related arrests than non-IV users (M=8.03 for IV-users, versus M=2.7 for non-IV users). The mean number of incarcerations for intravenous users was 0.33 (SD=0.69), versus 0.1 (SD=0.32) for the non-IV group; therefore, as would be expected, IV-users within this sample were more likely to have been imprisoned for their crimes. Out of the entire cohort of non- IV users, only one participant reported being incarcerated and this was for a drug-related offense. The differences between arrest records for each cohort can be compared in Tables under Arrest records for the entire sample and because one’s history of arrest was factored into whether or not one attempted suicide, the data from the cohort of intravenous users has been separated to display the discrepancies between IV-users who made a suicide attempt and those who did not for ease of comparison.
Arrest records for the entire sample(Table 3)
| # of Arrests | # of Drug-Related Arrests | # of Prison Sentences | # of Drug-Related Prison Sentences | |
|---|---|---|---|---|
| Mean | 6.2 | 2.2 | 0.25 | 0.21 |
| Median | 3 | 1 | 0 | 0 |
| SD | 7.22 | 3.08 | 0.59 | 0.56 |
| Minimum | 0 | 0 | 0 | 0 |
| Maximum | 30 | 10 | 2 | 2 |
Table 3: The arrest records for the sample, this table is broken down by the number of drug related arrests, number of prison sentences, and number of drug-related prison sentences for the entire sample.
Arrest records for each cohort(Table 4)
| Non-IV users | IV-users | IV-users with a suicide attempt | IV-users without a suicide attempt | |
|---|---|---|---|---|
| N | 10 | 18 | 10 | 8 |
| Mean # of arrests | 2.7 | 8.03 | 8.85 | 7 |
| Median | 2 | 4.25 | 3.5 | 6.25 |
| SD | 2.79 | 7.94 | 9.41 | 6.09 |
| Minimum | 0 | 1 | 1 | 1 |
| Maximum | 10 | 30 | 30 | 20 |
| N | 10 | 18 | 10 | 8 |
| Mean # of drug-related arrests | 1.3 | 2.61 | 1.7 | 3.75 |
| Median | 0 | 1.5 | 1 | 2.5 |
| SD | 3.14 | 3.03 | 2.45 | 3.45 |
| Minimum | 0 | 0 | 0 | 1 |
| Maximum | 10 | 10 | 8 | 10 |
Table 4: The average number of arrests for each cohort. Because one’s history of arrest was factored into whether or not one attempted suicide, the data from the cohort of intravenous users has been separated to display the discrepancies between IV-users who made a suicide attempt, and those who did not for ease of comparison. It is also divided so that the top half represents the number of entire arrests for each cohort; whereas, the bottom half of table represents the average number of drug-related arrests for each cohort.
Data was also gathered on mental health and substance abuse histories to examine if these were related to participant’s methamphetamine use and the prevalence of suicidal ideations. Overall, 67.9% of the sample reported previous mental health treatment, but only 17.9% had undergone psychiatric hospitalization. Of the 17.9% who had been hospitalized, no individual reported more than two hospitalizations and only one non-IV user reported being hospitalized. This would suggest intravenous users experience more severe psychiatric difficulties, which is commensurate with research findings by Domier et al. [16], who also noted a lengthier history of psychological problems for injectors versus non-injectors.
In regard to history of substance abuse treatment, 60.7% of the sample had previously undergone drug and alcohol rehabilitation, with an average of 1.71 episodes of treatment prior to participation in this study (SD=1.78). The group of non-injectors reported slightly less treatment with an average of 1.2 previous episodes of substance abuse treatment (SD=2.2), whereas the IV-users averaged 1.97 episodes of previous treatment (SD=1.46).
In respect to suicide, 60.7% of the sample endorsed having experienced previous suicidal ideations, with 35.7% having also attempted suicide at some point. Of those participants who made a suicide attempt, they were all intravenous users. These individuals reported an average of 1.9 attempts (SD=2.72). The data on participant hospitalizations, number of suicide attempts and age of first attempt for the entire sample is outlined in Tables.
Hospitalizations and suicide attempts(Table 5)
| # of Hospitalizations | # of Suicide Attempts | Age of First Attempt | |
|---|---|---|---|
| Mean | 0.25 | 1.23 | 18.8 |
| Median | 0 | 0 | 17 |
| SD | 0.59 | 2.36 | 6.02 |
| Minimum | 0 | 0 | 12 |
| Maximum | 2 | 10 | 28 |
Table 5: The average number of hospitalizations for the entire sample, it also represents the average number of suicide attempts, as well as the average age of making a first suicide attempt.
In essence, over half of the sample endorsed previous thoughts of suicide, with less than half of those individuals actually acting on such thoughts. However, when these individuals did act on these ideations, they did so on more than one occasion. The most common form of attempted suicide reported was “overdose.” This is not surprising, considering only intravenous users made an attempt and this would be an easily accessible means for these individuals. Most participants who attempted to overdose did so on more than one occasion and every participant who reported a suicide attempt indicated they utilized this method, with the exception of one subject, who reported a single suicide attempt through the use of a firearm. This data is outlined in Tables.
Hospitalizations for each cohort(Table 6)
| Non-IV users | IV-users | IV-users with a suicide attempt | IV-users without a suicide attempt | |
|---|---|---|---|---|
| N | 10 | 18 | 10 | 8 |
| Mean # of hospitalizations | 0.1 | 0.28 | 0.5 | 0 |
| Median | 0 | 0 | 0 | 0 |
| SD | 0.64 | 0.57 | 0.71 | 0 |
| Minimum | 0 | 0 | 0 | 0 |
| Maximum | 2 | 2 | 2 | 0 |
Table 6: The average number of psychiatric hospitalizations broken down by cohort.
Mode of suicide attempt(Table 7)
| Frequency | Percent | |
|---|---|---|
| Firearm | 1 | 3.6 |
| Overdose | 6 | 21.4 |
| Overdose-Cut Wrists | 3 | 10.7 |
| Overdose-Hanging | 1 | 3.6 |
Table 7: The modality of attempting suicide, as well as the frequency at which this modality was reported consisting of all intravenous users.
Participants were also asked to report their “drug of choice,” along with other substances used. These data are outlined in Tables 8 and 9. To no surprise, methamphetamine was listed as the most common substance used, with 60.7% of the sample endorsing this as their drug of choice. Marijuana ranked second, with 17.9% of the sample listing this as their favorite substance, followed by heroin and opiates, alcohol and cocaine. When looking at each participant’s “second drug of choice,” most individuals listed “none,” followed by marijuana. This suggests methamphetamine and marijuana appear to be the most favorable substances used within this cohort, followed by heroin and opiates.
Participant’s drug of choice (Table 8)
| Frequency | Percent | |
|---|---|---|
| Cocaine | 1 | 3.6 |
| Marijuana | 5 | 17.9 |
| Alcohol | 2 | 7.1 |
| Methamphetamine | 17 | 60.7 |
| Heroin & Opiates | 3 | 10.7 |
Table 8: The education level of the participants broken down by frequency and percent.
Participant’s other drug of choice (Table 9)
| Frequency | Percent | |
|---|---|---|
| Cocaine | 1 | 3.6 |
| Marijuana | 5 | 17.9 |
| Alcohol | 1 | 3.6 |
| Methamphetamine | 1 | 3.6 |
| Opiates (Including morphine & heroin) | 2 | 7.1 |
| None | 18 | 64.3 |
Table 9: Participant’s other drug of choice, aside from their main drug of choice reported along with the entire sample.
Of the 28 participants, 18 (64.3%) reported intravenous methamphetamine use. However, 60.7% of these IV-users report using methamphetamine through a different method prior to injection (i.e., smoked, snorted or ate the drug prior to injecting for the first time). Only five IV-users denied injecting any other substance aside from methamphetamine; meanwhile, 57.1% of injectors also reported using heroin, morphine or other opiates intravenously, in addition to their IV-methamphetamine use. The list of intravenously used substances for this cohort are outlined in Table 10. Nonetheless, it appears over half of this sample has used methamphetamine intravenously; however, they tend to inject multiple substances, rather than remaining restricted to purely methamphetamine use.
Reported substances injected (Table 10)
| Frequency | Percent | |
|---|---|---|
| Only Methamphetamine | 5 | 3.6 |
| Heroin or Morphine | 10 | 35.7 |
| Other Opiates | 6 | 21.4 |
| Cocaine | 5 | 17.9 |
| Benzodiazepines | 2 | 7.1 |
| Alcohol | 2 | 7.1 |
| Methylenedioxyamphetamine (MDA) | 1 | 3.6 |
Table 10: The various substances participant’s reported injecting in their lifetime, several participants reported injecting multiple substances.
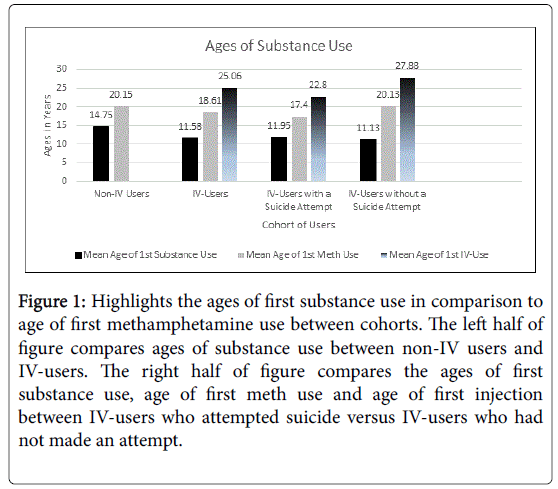
The average age of first substance use for the entire sample was 12.7 years old (SD=3.53), with one participant reporting in-utero exposure. The average age of first methamphetamine use was 19.2 years old (SD=6.68), with age of first meth use ranging from 11 to 45. There were discrepancies between IV and non-IV users in regards to age of first substance use, as well as in regards to age of first meth use. To begin, the cohort of non-injectors tended to try their first substance at a later age (M=14.75, SD=2.46) than the cohort of injectors (M=11.58, SD=3.58). Likewise, non-injectors were more likely to initiate meth use at a later age than other substance use as well (M=20.15, SD=4.42, versus M=18.61, SD=7.78, respectively). The average age of first injection was 25 (SD=7), with the youngest age of first injection being 15 and the oldest age being 45. The typical IV-user averaged 36.1 methamphetamine injections a month (SD=33.94, Range=1-105). Additional information regarding participant substance use for each cohort is available in Figure 1.
Figure 1: Highlights the ages of first substance use in comparison to age of first methamphetamine use between cohorts. The left half of figure compares ages of substance use between non-IV users and IV-users. The right half of figure compares the ages of first substance use, age of first meth use and age of first injection between IV-users who attempted suicide versus IV-users who had not made an attempt.
Half of this sample indicated they know someone who uses methamphetamine regularly and who has attempted suicide. When asked if they knew if this person used methamphetamine intravenously, 39.3% said yes and 28.6% said this person injected methamphetamine regularly.
In order to address the research hypothesis, that intravenous users of meth will report a higher rate of suicide attempts than non-injecting users, a correlation matrix and independent sample t- test were completed. Results demonstrated frequent methamphetamine use was related to suicidal ideations (r=0.431, p=0.022), with intravenous users experiencing more suicidal ideations (r=0.556, p=0.002). Furthermore, there was a significant relationship between methamphetamine injection and number of suicide attempts (r=0.397, p=0.036). Overall, those participants who inject methamphetamine reported a significantly higher number of suicide attempts (M=1.9) than those who do not inject (M=0), t (26)=2.206, p=0.036. There was not a similar significant difference in number of suicide attempts when comparing individuals who use methamphetamine regularly (via any form of administration) versus those who reported not using methamphetamine regularly (M=2 and M=1.1, respectively), indicating an important difference in suicidality particularly in those individuals who inject this drug. Data on the correlation between number of suicide attempts and IV-use is outlined in Table 11.
| Have you ever injected methamphetamine? | N | Mean # of Suicide Attempts | Standard Deviation |
|---|---|---|---|
| No | 10 | 0 | 0 |
| Yes | 18 | 1.92 | 2.72 |
Table 11: The average number of suicide attempts between participants who injected methamphetamine versus participants who had never injected.
Suicide and methamphetamine use (Table 11)
To explore interrelationships among education, employment, history of arrest, previous suicide attempts and history of intravenous methamphetamine use, a correlation matrix was utilized. The only significant relationship identified was between the number of previous suicide attempts and history of injecting methamphetamine. Given the lack of association between the other variables and either history of suicide attempts or methamphetamine injection, only the relationship between these two variables was analyzed using a t-test, rather than conducting an ANCOVA with education, employment and arrest record as covariates. The fact that there was no correlation amongst these variables is an interesting finding, which may be attributed to the small sample size. Nonetheless, this information would reject the subhypothesis which suggests these factors would impact the prevalence of suicidal ideations.
Discussion
This study did find several discrepancies between IV and non-IV methamphetamine users. There were also many other notable differences within the IV-using sample who endorsed a previous suicide attempt, when compared to IV-users who denied such an attempt. However, the results of this study appear to raise more questions than answers. It seems evident intravenous users of methamphetamine are at a significantly higher risk for attempting suicide than non-IV users, yet contributing factors leading to suicide attempts remain unknown. Furthermore, participants who had attempted suicide were more likely to make an attempt prior to ever injecting meth, which suggests that perhaps there are other underlying factors associated with suicidal ideations that lead to intravenous meth use (Table 12).
| Age of 1st Substance Use for Non-IV Users | Age of 1st Substance Use for IV-Users | Age of 1st Substance Use for IV-Users with a Suicide Attempt | Age of 1st Substance Use for IV-Users without a Suicide Attempt | ||
|---|---|---|---|---|---|
| N | Valid | 10 | 18 | 10 | 8 |
| Missing | 0 | 0 | 0 | 0 | |
| Mean | 14.75 | 11.58 | 11.95 | 11.13 | |
| Median | 14.5 | 12 | 12 | 12 | |
| Std. Deviation | 2.33 | 3.49 | 2.33 | 4.4 | |
| Minimum | 10 | 0 | 5.5 | 0 | |
| Maximum | 19 | 16 | 14 | 16 | |
| Age of 1st Meth Use for Non-IV Users | Age of 1st Meth Use for IV-Users | Age of 1st Meth Use for IV-Users with a Suicide Attempt | Age of 1st Meth Use for IV-Users without a Suicide Attempt | ||
| N | Valid | 10 | 18 | 10 | 8 |
| Missing | 0 | 0 | 0 | 0 | |
| Mean | 20.15 | 18.61 | 17.4 | 20.13 | |
| Median | 19.75 | 15 | 16 | 15 | |
| Std. Deviation | 4.02 | 8.69 | 4.45 | 12.18 | |
| Minimum | 16 | 0 | 11 | 0 | |
| Maximum | 30 | 45 | 27 | 45 | |
| Age of 1st IV-Use | Age of 1st IV-Use for IV-Users with a Suicide Attempt | Age of 1st IV-Use for IV-Users without a Suicide Attempt | |||
| N | Valid | 18 | 10 | 8 | |
| Missing | 0 | 0 | 0 | ||
| Mean | 25.06 | 22.8 | 27.88 | ||
| Median | 25.5 | 23 | 28.5 | ||
| Std. Deviation | 6.81 | 8.7 | 8.29 | ||
| Minimum | 15 | 15 | 16 | ||
| Maximum | 45 | 29 | 45 | ||
Table 12: Additional information regarding participant substance use for each cohort.
Interestingly, amongst the group of non-IV users, there were no previous suicide attempts. In fact, only 40% of this cohort even reported experiencing suicidal ideations. However, when comparing these two groups, it is apparent the IV-users began their first substance use at an earlier age (11.58 years old versus 14.75 years old). This earlier substance use may have played a factor in their decision to use methamphetamine intravenously, but also in their experience of depression and suicidal ideations as well. Regardless, IV-users reported their first methamphetamine use at age 17.4, versus 20.15 for non-IV users. However, the average age of first methamphetamine use for IVusers who did not attempt suicide (20.13 years old) was nearly identical to that of non-IV users (20.15 years old). In general, the IVusers who did not attempt suicide appear to have many things in common with the non-IV using cohort. This again indicates something unique about IV-users who made an attempt and differentiates them from other IV-users.
Intravenous methamphetamine use and suicide do appear to be related, although, based on the results obtained in this study, it remains difficult to identify what factors specifically contributed to attempting suicide within this sample. It is apparent meth users face many difficulties, oftentimes this includes suicidal ideations. These difficulties, particularly suicidal ideations, seem to be exacerbated with the initiation and continuation of intravenous meth use. However, what remains puzzling, is the fact that meth users who attempted suicide (n=10) tended to make their initial suicide attempt (M=18.8 years old) prior to injecting for the first time (M=22.8 years old). This is contradictory to the hypothesis suggesting intravenous meth-use leads to suicidal ideations. In reality, it may be more appropriate to assert that early methamphetamine use is oftentimes accompanied by suicidal ideations, which are only strengthened after continued intravenous meth-use. Therefore, we can surmise intravenous methuse and suicide are related, but not necessarily that IV-use is the cause of suicidal ideations, thus making it difficult to identify what factors strengthen this relationship. This in turn places responsibility/duty on researchers to identify what childhood influences lead to early substance use, including early meth-use, as well as examining what factors lead up to meth injection. The fact that no other demographic or historical variables examined in this sample were related to suicidality raises further questions around what factors serve as stronger predictors of suicidal behaviors. Regardless of what these factors may be, it seems apparent they are present during the earlier years of one’s life.
This study also identified a possible relationship between attempting suicide and later injecting meth or other substances. Perhaps, experiencing suicidal ideations at an early age indicates a higher risk for intravenous drug use later on in life. Or perhaps, there are certain underlying factors contributing to having suicidal ideations at an early age, that lead to IV-meth use. For example, maybe these individuals who attempted suicide and later injected meth share a common diagnosis or a certain type of trauma or other unbeknownst factors.
Although there were no statistical correlations between IV and non- IV users based on education, employment, arrest record or history of mental health treatment, there does appear to be minute differences within these groups. For example, IV-users tended to report a higher frequency of psychiatric hospitalization (M=0.28) than non-IV users (M=0.1). IV-users with a suicide attempt also were more likely to be unemployed and tended to have a higher number of arrests.
Both cohorts endorsed significant polysubstance use. However, this also did not appear to be a factor in whether or not one attempted suicide. Likewise, there were no differences in suicide attempts between users who injected only methamphetamine, as opposed to users who injected other substances as well. Although there was frequent polysubstance use within this sample, methamphetamine was considered the “drug of choice” by the majority of participants. Future studies should explore the effects of interacting multiple substances on the user and their likelihood to withhold from attempting suicide. For example, the majority of the sample reported frequent marijuana use in addition to their meth use. Likewise, IV-users reported frequently injecting heroin or other opiates. The results of this study may indicate polysubstance use is not a factor in whether or not one attempts suicide; however, it remains unknown if the psychoactive effects of using multiple substances somehow actually helps prevent users from attempting.
There are several interesting facets between IV-users who attempted suicide versus IV-users who did not attempt that are worth examining. To begin, both cohorts experienced their initial substance use before the age of 12; however, it remains unknown if the individuals within these two groups continued to use substances regularly following their initial use. Nonetheless, it appears IV-users who attempted suicide began using methamphetamine a few years earlier than IV-users without an attempt (17.4 years of age versus 20.13 years of age). Likewise, IV-users with a suicide attempt began injecting methamphetamine about five years sooner than IV-users who did not attempt suicide (22.8 years of age versus 27.88 years of age). There was obviously something unique about the group of IV-users with a suicide attempt that propagated these behaviors at such early ages and differentiates them from the rest of the IV-using cohort. This raises more questions than answers, but indicates factors aside from IV-meth use.
There also were no psychiatric hospitalizations within the cohort of IV-users who did not report a suicide attempt, which is similar to the non-IV using group. It is worth noting the injectors who did not attempt suicide had more drug-related arrests (M=3.75, SD=3.45) than the IV-users who did make an attempt (M=1.7, SD=2.45). Therefore, these individuals were more likely to be incarcerated, which perhaps forced them to detox and engage in some form of treatment. Perhaps the time during incarceration kept them from not only requiring hospitalization, but played some factor in their lack of suicide attempts. Nonetheless, imprisonment may serve as a suitable punishment for drug-related crimes, particularly for younger offenders.
Future Directions
Although the demographic variables which were analyzed in this study failed to produce a significant correlation between meth use and suicide, there was other intriguing information obtained. For example, it appears beneficial to examine what early childhood factors increase the tendency to not only attempt suicide, but to use methamphetamine intravenously as well. Perhaps there is a disruption in attachment style, a certain family dynamic or a particular set of diagnoses which increase this. At this point it remains unknown; however, there were observable differences between IV-users who attempted suicide and the rest of the sample. When we scrutinize these differences it seems apparent they originated in childhood, as IV-users with a suicide attempt began injecting at a younger age than the rest of the sample.
Since IV-users with a suicide attempt not only initiated early methamphetamine use, but were also more likely to have been hospitalized for psychiatric reasons, future studies should explore the mental health variables which may be related to suicide and specifically pertain to this population. For example, we have a better understanding for the long and arduous depression meth users encounter during periods of abstinence, but this fails to account for why some IV-users attempt suicide (typically more than once) and others do not. Unfortunately, this study was unable to identify any factors based on the demographic variables examined.
Participants were asked about previous mental health treatment and number of hospitalizations, but not about previous diagnosis received. Therefore, presence of various diagnoses, particularly at a young age, may create a higher propensity to attempt suicide, particularly if one begins using meth intravenously. Or, perhaps there is an unidentified correlation between certain medications combined with a particular diagnosis and meth use, which increases suicidal ideations. At this point it remains unidentified, although it appears worthy of exploration.
Future studies also would benefit from examining the differences between frequent injectors versus sporadic injectors. There was a considerably large range within the frequency of injecting (1 to 105 times per month) thus it seems logical this would be worthy of examination. From a physiological standpoint, it would be interesting to gain a more clear understanding of the comorbid use of methamphetamine and other substances, particularly marijuana and opiates since these appear to be the most commonly used substance, based on data from this sample.
Although only 35.7% of the sample attempted suicide, 60.7% endorsed previous suicidal ideations. Because suicidal thoughts are so prevalent within this population, future research should seek to explore what factors kept users with suicidal ideations from acting on these thoughts. One participant in this study spoke about the difficulties meth injectors encounter during the course of their addiction. This individual described a mental state of depression, which is strengthened during intravenous use. According to this participant, the problem lies in the fact that IV-users typically go on “binges” where they use a considerable amount of meth over a span of several days. During this time, it is typical for users to enter a state of peculiar behavior, oftentimes described as “tweaking.” This particular individual stated that if a user becomes “tweaked out,” they find it incredibly difficult to shift their mind from whatever task they are focused on. This becomes problematic if the user is “tweaked out” on the idea of committing suicide. Other participants in this study also described a mental state of imprisonment where they could only think of ways to commit suicide. As time passes their sense of reality dissipates and these thoughts become overwhelmingly troublesome. Future research should examine this mental state and education should be provided on this behavior to users in treatment so that awareness is increased and users are not as alarmed when they find themselves in this troubling position. Given the neurological effects of methamphetamine use, one can presume this behavior is the result of damage to the self-control tract (fasciculus retroflexus, ventral tegmental area) and judgment centers (frontal lobes) of the brain [17]. These areas become damaged, so when one becomes “tweaked out” on the idea of committing suicide, they may not be able to inhibit this impulse, similar to the way they cannot inhibit the desire to use.
Since the findings in this study point to factors which may occur during early childhood and later lead to suicidal ideations, treatment providers should make note of this when working with juvenile substance users. It seems prudent to conduct very thorough risk assessments with juveniles in substance abuse treatment, especially if the individual endorses suicidal ideations or a previous suicide attempt. Psychoeducation also should be provided to parental figures regarding the dangers of early meth use and suicide. Since overdose appears to be the most common means of attempting suicide, parents should be warned of this and should take extra diligence in securing medications around their home.
Given the fact that almost every participant who attempted suicide did so through overdosing on more than one occasion, it seems worthwhile to examine what substances these users attempted to overdose on. Given the physical nature of a methamphetamine overdose, it seems unlikely these participants would attempt with this substance. However, this study failed to examine what substances users attempted to overdose with; therefore, it remains unreasonable to make speculations based on this study. Since most meth users attempted suicide through this method, treatment centers should incorporate education on how overdosing damages the body and hastens death.
Limitations
It is unfortunate only 28 participants were ultimately solicited to complete the survey, as this is below the desired number initially proposed prior to the onset of data collection. Nonetheless, this study acquired more IV-users (n=18) than non-IV users (n=10), which was unexpected and may highlight a greater need/tendency for IV-users to seek out treatment.
From a qualitative perspective, there was an ostensible sense of paranoia from participants in general. During the in-person data collection phase, there were several individuals who were present throughout this entire time period, but who chose to wait to complete the survey until mid-way through the data collection process, almost as if they were unsure if they could trust the nature of the study. Participants asked many questions about the purpose of the study and seemed to be particularly interested in understanding why the researcher chose to focus on this particular aspect of meth use. After a few days of data collection, individuals in treatment seemed to become more comfortable with the researcher’s presence and in turn became more willing to participate in the study. However, the majority of those who completed the paper survey chose to place the survey in the locked box, rather than return it to the researcher or treatment facility staff, a behavior which may be subconsciously driven by paranoia. In addition, only five individuals chose to complete the electronic version of the survey over the paper version. This too, could be considered a token of ongoing paranoia due to the idea of the paper version being more anonymous than using a computer. It also is worth noting there were 28 surveys completed, but nearly twice as many questionnaires were given to potential participants. It remains unknown what kept these participants from completing the survey, but perhaps paranoia played a part in this as well. However, if paranoia were a factor, this could explain part of the reasoning why there is such limited research on this population and helps account for some of the difficulty experienced when collecting data on this population.
Other limitations apply as well. For example, portions of the survey focused on previous episodes of substance abuse treatment; however, detailed information was not gathered, such as when or where those treatments took place. This made it impossible it identify what type of treatments were utilized so comparisons could be made in regards to overall effectiveness and suicidal behaviors. For example, perhaps users who received treatment in prison had a better outcome, versus users who received treatment in a more traditional outpatient setting. Or, perhaps users who received substance abuse treatment at an earlier age where less likely to engage in intravenous use. These variables may be worth scrutiny and future research could benefit from exploring these factors in hopes to identify which of these modalities produce the most effective outcomes.
The survey also failed to ask more in-depth questions pertaining to the type of previous mental health treatment the participants engaged in. It would have been nice to have a better understanding of what age participants first entered mental health treatment and for what reasons. It also would have been beneficial to have added questions about previous diagnoses to see if any similarities were present. This information seems especially pertinent considering the underlying causes of attempting suicide appear to be present at a young age and are intensified with early meth use. Finally, this survey failed to ask about participant’s ethnicity, which makes it difficult to examine for any possible differences that may have been present.
Conclusion
In summary, frequent meth use does lead to suicidal tendencies, particularly intravenous use. Overall, the participants who inject methamphetamine reported a significantly higher number of suicide attempts (M=1.9) than those who do not inject (M=0). The main hypothesis of this study was confirmed in the sense that IV-meth use and suicide are related; however, they appear to be related in a nontraditional sense. For example, the meth-users within this sample who endorsed a previous suicide attempt typically made their first attempt prior to ever injecting meth. Therefore, we cannot surmise that IVmeth use leads to suicidal behaviors; rather, suicidal ideations and IVmeth use are related for other reasons which are yet to be identified. Perhaps future researchers can accentuate the factors identified in this study and more properly identify other variables related to meth-use and suicide.
Conflict of Interest
There is no conflict of interest regarding this study. There were no financial interests, benefits or payments received to help produce this study.
References
- Anglin MD, Burke C, Perrochet B, Stamper E, Dawud-Noursi S (2000) History of the methamphetamine problem. J Psychoactive Drugs 32: 137-141.
- Morgan P, Beck JE (1997) The legacy and the paradox: Hidden contexts of methamphetamine use in the United States. In: H, Klee (Eds.), Amphetamine misuse: International perspectives on current trends. Boca Raton, FL: CRC Press.
- Joe KA (1995) Ice is strong enough for a man but made for a woman: A social cultural analysis of crystal methamphetamine use among Asian Pacific Americans. Crime, Law, and Social Change, 22: 269-289.
- Kozel N, Miller M (1991) Methamphetamine abuse: Epidemiological issues and implications. Rockville, MD: U.S. Department of Health and Human Services, Public Health Service, Alcohol, Drug Abuse, and Mental Health Administration, National Institute of Drug Abuse.
- Freese TE, Obert J, Dickow A, Cohen J, Ford RH (2000) Methamphetamine abuse: Issues for special populations. J Psychoactive Drugs 32: 177-182.
- Glittenberg J, Anderson C (1999) Methamphetamine use and trafficking in the Tucson-Nogales area. Subst Use Misuse 34: 1977-1989.
- United Nations Office on Drugs and Crime (2009) World drug report 2009.
- Substance Abuse and Mental Health Services Administration (SAMHSA) (2013). Behavioral health services for people who are homeless: A treatment improvement protocol 55. (SMA Report No. 13-4734).
- National Institute on Drug Abuse (2010) Comorbidity: Addiction and other mental illnesses. (NIDA Publication No. 10-5771).
- Substance Abuse and Mental Health Services Administration (SAMHSA) (2013) Results from the 2012 national survey on drug use and health: Summary of national findings (HHS Publication No. 13-4795).
- Berger S (2011) Injected meth is associated with an increased risk of attempted suicide. Mental health, substance dependence.
- Marshall BD, Galea S, Wood E, Kerr T (2011) Injection methamphetamine use is associated with an increased risk of attempted suicide: A prospective cohort study. Drug Alcohol Depend 119: 134-137.
- Callor WB, Petersen E, Gray D, Grey T, Lamoreaux T, et al. (2005) Preliminary findings of noncompliance with psychotropic medication and prevalence of methamphetamine intoxication associated with suicide completion. Journal of Crisis Intervention and Suicide Prevention 26: 78-84.
- Kalechstein AD, Newton TF, Longshore D, Anglin MD, van Gorp WG, et al. (2000) Psychiatric comorbidity of methamphetamine dependence in a forensic sample. The J Neuropsychiatry Clin Neurosci 12: 480-484.
- Domier CP, Simon SL, Rawson RA, Huber A, Ling W (2000) A comparison of injecting and non-injecting methamphetamine users. J Psychoactive Drugs 32: 229-232.
- Holley M (2006) How reversible is methamphetamine related brain damage? North Dakota Law Review 82: 1135-1149.
Citation: Hypse JD (2018) Suicide Rates between Methamphetamine Users who inject versus Non-Injectors. J Addict Res Ther 9: 359. DOI: 10.4172/2155-6105.1000359
Copyright: ©2018 Hypse J. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 9998
- [From(publication date): 0-2018 - Dec 15, 2025]
- Breakdown by view type
- HTML page views: 9004
- PDF downloads: 994