Surgical Reconstruction of Interdental Papilla using Subepithelial Connective Tissue Graft by Microsurgical Technique: A Clinical Study
Received: 12-Feb-2018 / Accepted Date: 12-Mar-2018 / Published Date: 19-Apr-2018 DOI: 10.4172/2376-032X.1000229
Abstract
Background: Loss of interdental papilla is one of the most concerning esthetic problem for the patient and equally challenging for the clinician. Management of papillary loss has shown limited success and is limited to case reports with lack of long-term follow-up.
Method: Surgical microscope was used at 6X magnification in this study to enhance the visual acuity in the narrow interdental space. 13 cases with 20 sites in the maxillary anterior region were selected for surgical reconstruction. Tunnelling was performed under the deficient papillae and connective tissue graft used to fill the space created.
Results: Among 20 sites, 5 sites showed complete papillary fill, while 3 sites were 1 mm deficient. The mean vertical gain achieved was 1.63 mm which was statistically significant at P value <0.01. A significant adverse surgical outcome was diastema formation within 4 weeks postoperatively.
Conclusion: Microsurgery enhances the surgeon’s ability to handle delicate papillary tissue and hence more predictable. Splinting of teeth prior to papillary reconstruction may be considered to prevent diastema formation.
Keywords: Interdental papilla; Gingival embrasure; Microsurgery
Introduction
Periodontal plastic surgery encompasses a broad range of procedures aimed at correcting or eliminating anatomic, developmental or traumatic deformities of gingiva or alveolar mucosa [1].
One of the major challenges in this field is related to the ability of rebuilding papillae lost either due to periodontal disease or therapy. Loss of interdental papillae in the maxillary region results in esthetic and phonetic aberrations [2].
A major limiting factor in all papillary reconstruction techniques is inadequate blood supply. The recipient interdental space borders nonvascularized tooth surfaces and has small surface area for manipulation and grafting [2].
Several surgical and non-surgical approaches have been suggested to improve esthetics but with limited success [3].
Microsurgery in general is not an independent discipline, but is a technique that can be applied to different surgical disciplines. It is based on fact that human hand, by appropriate training, is capable of performing finer movements than the naked eye is able to control.
Microsurgery enhances the capability of operator by enhancing the visual acuity by means of illumination and magnification. Literature on periodontal microsurgery shows improved surgical outcome when used for root coverage procedure [4,5-13] and regenerative therapy [14,15].
In this clinical study, a microsurgical approach is attempted to manage papillary loss using connective tissue graft harvested from the palate. The emphasis is on minimizing trauma by utilizing microsurgical instruments to work in the narrow interdental region of anterior maxilla.
Materials and Methods
A total of 13 patients with 20 sites in maxillary anterior region were selected to undergo microsurgical papillary reconstruction. The inclusion criteria included systemically healthy individuals in age group of 20-50 years, with interdental papillary loss in maxillary anterior teeth without diastema. The exclusion criteria included chronic smokers, pregnancy, root exposure with proximal restoration and endodontically treated teeth.
This clinical study assessed the efficacy of microsurgical reconstruction of lost interdental papilla using interposed connective tissue graft harvested from palate. The assessment was based on single surgical intervention irrespective of class of papillary loss. Surgical procedure was explained to the patients and informed consent obtained. All patients with papillary loss in maxillary anterior region and willing for surgical reconstruction were taken up for study. Patients diagnosed with periodontitis were taken up for the surgical reconstruction after the completion of active periodontal therapy.
The amount of vertical gain that can be achieved with one surgical intervention was assessed. The measurements were recorded to the nearest millimeter and tabulated for each site (Table 1). Wilcoxon Signed Ranks Test was carried out to compare parameters within group at baseline and 6 months interval.
| Parameters Recorded | ||||||
|---|---|---|---|---|---|---|
| Case No | Site | Vertical component (in mm) | Horizontal component (in mm) | Interproximal boneheight (in mm) | ||
| Baseline | 6 months | Baseline | 6 months | Mean value | ||
| 1 | 11-21 | 4 | - | 2 | - | 8 |
| 2 | 11-21 | 3 | 0 | 2 | 0 | 5 |
| 3 | 12-11 | 3 | 3 | 2 | 2 | 7 |
| 3 | 11-21 | 2 | 1 | 2 | 1 | 6 |
| 4 | 11-21 | 4 | 2 | 2 | 1 | 7 |
| 5 | 11-21 | 4 | 3 | 2 | 1 | 9 |
| 6 | 12-11 | 3 | 1 | 2 | 1 | 8 |
| 6 | 11-21 | 3 | 0 | 2 | 0 | 9 |
| 7 | 12-11 | 4 | 2 | 2 | 1 | 9 |
| 7 | 11-21 | 3 | 2 | 2 | 1 | 8 |
| 8 | 12-11 | 3 | 0 | 1 | 0 | 6 |
| 8 | 11-21 | 3 | 2 | 1 | 1 | 7 |
| 8 | 21-22 | 2 | 0 | 2 | 0 | 6 |
| 9 | 11-21 | 3 | 2 | 1 | 1 | 8 |
| 10 | 11-21 | 5 | 7 | 3 | 3 | 8 |
| 11 | 11-21 | 5 | 1 | 2 | 1 | 9 |
| 12 | 12-11 | 5 | 3 | 2 | 2 | 7 |
| 12 | 11-21 | 5 | 5 | 2 | 2 | 9 |
| 13 | 12-11 | 4 | 2 | 1 | 1 | 9 |
| 13 | 11-21 | 3 | 0 | 2 | 0 | 7 |
Table 1: Parameters recorded.
Surgical technique
The patients were scrubbed and adequate local anesthesia was administered using 2% Xylocaine with adrenaline (1:80000). The surgical microscope was appropriately positioned to facilitate easy movements of operator and assistant. All the joints of the microscope were loosened. It was placed in a manner where the eye piece of the microscope was at a 7 O' Clock position in relation to the patients. After setting up the microscope, all the joints were secured by tightening the screws. The patient was placed in a semi-reclining position with head turned towards the microscope. Working field was adjusted at 6X magnification and brightness adjusted as per requirement. Finer adjustments of the microscope were done using foot control.
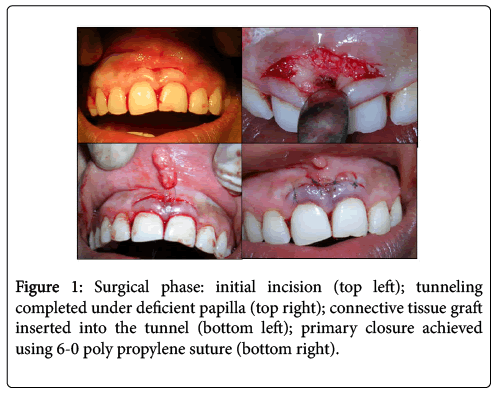
A partial thickness semilunar incision was placed 1 mm coronal to the mucogingival junction. It extended to at least one papilla on either side of the defective papilla (Figure 1). Subsequently, an intra sulcular incision was extended all around the neck of teeth forming the boundary of the defective papilla, and towards the initial incision on labial aspect. This ensured that the interdental papilla was kept intact.
The donor site was then prepared for graft procurement. Contraangle BP handle with No 11 blade was used for the incision on palatal region.
The extension of the incision was limited anteriorly by palatine rugae. Posteriorly, the incision was not extended beyond mid palatal root of first molar.
A partial thickness flap was raised by undermining the palatal mucosa without any release incision. The harvested graft consisted of subepithelial connective tissue from the posterior palatal region.
The graft was then placed in a saline soaked ribbon gauze until the recipient bed was prepared.
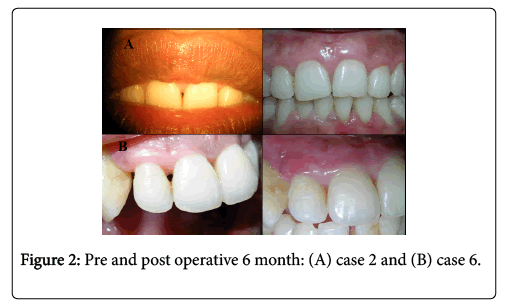
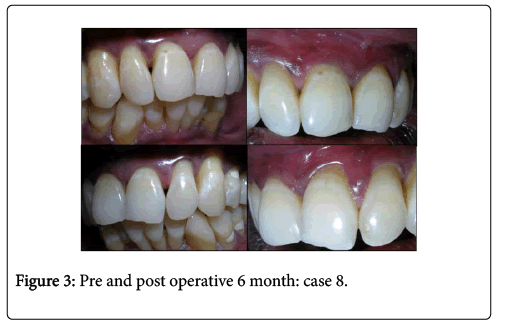
Primary closure was obtained at the donor site by placing aluminum foil over the incision area to avoid entanglement of suture within the periodontal dressing placed with stent (Figures 2 and 3).
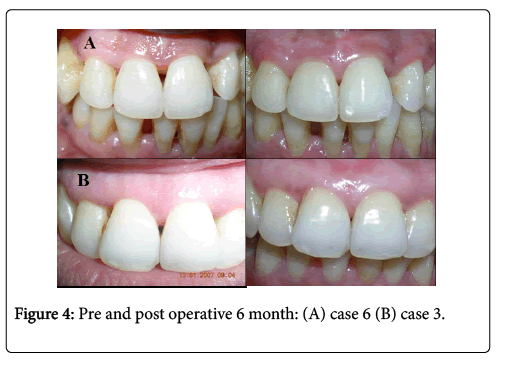
A split thickness flap was initiated from the initial semilunar incision toward the sulcular incision to completely mobilize the gingivo-papillary unit. This flap was undermined carefully below the papilla towards the palatal mucosa initially using Orbans knife and extended palatally using a disposable microsurgical knife. Care was taken to avoid perforating the palatal mucosa and to prevent exposure of the alveolar crest in the interdental region. Once the gingivopapillary unit was completely released, blunt dissection was performed on the palatal aspect to release all the attachments from the tooth surface and to allow for the coronal displacement of the papilla (Figure 4).
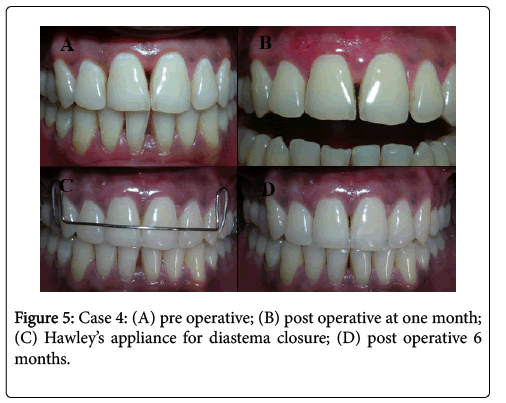
Meticulous scaling and root planing were carried out prior to graft insertion. The void or dead space created between papillary unit and crestal bone was then filled by subepithelial connective tissue graft (SCTG) procured from the palatal region. The graft was pulled into the void space using horizontal mattress suture starting from palatal side using 6-0 prolene non-absorbable suture material. After placement of graft, a full thickness flap was raised apical to gingivo-papillary unit. A release incision was made at the base to coronally displace the flap for primary closure. It was ensured that there was no pressure on the papilla after primary closure of flap. 6-0 prolene was used for the closure of flap. No dressing was placed over the recipient area (Figure 5).
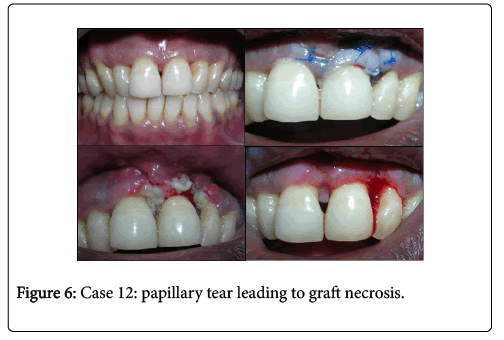
The patients were prescribed Cap Amoxicillin, 500 mg 1 capsule three times daily for 3 days, Tab Ibuprofen 400 mg 1 tablet SOS and 10 ml of 0.2% Chlorhexidine gluconate mouthwash twice daily for a period of 4 weeks. Patients were advised to avoid lifting the lips and touching the surgical sites with finger or tongue. Brushing and flossing of the region were discontinued for 4 weeks. On the third day post operatively, the stent with pack was removed along with sutures from palatal donor site. Remnants of soft tissue deposits were removed gently with moistened gauze pieces and the area was irrigated with normal saline. Sutures from the recipient site were removed after 1 week (Figure 6).
Patients were recalled periodically for check up. All the parameters were recorded and necessary photographs were taken. The baseline measurements were compared with the values recorded at 6 months for clinical and statistical significance.
Results
The baseline measurements were compared with the values recorded at 6 months for clinical and statistical significance. Among the 20 selected sites 1 site with Class I, 16 sites with Class II papillary loss and 3 with Class III papillary loss were treated. Five sites showed complete papilla fill while three sites showed a deficiency of 1 mm which was clinically insignificant (Table 1).
The sites with complete fill included four papillae with Class II papillary loss and one papilla with Class I papillary loss. Average gain in the papillary height after 6 month was 1.63 mm (± 1.36). The observed baseline to postoperative difference in vertical component was highly significant with P value <0.05 (Table 2).
| Parameter | Time of comparison | Mean | Std. Deviation | P value |
|---|---|---|---|---|
| Vertical component | VC-B | 3.526 | 0.96 | 0 |
| VC-06 | 1.894 | 1.82 | ||
| Horizontal component | HC-B | 1.842 | 0.5 | 0 |
| HC-06 | 1 | 0.82 | ||
| Keratinized gingiva | KG-B | 5.526 | 1.12 | 0.01 |
| KG-06 | 6.368 | 1.42 | ||
| Pocket depth | PD-B | 2.1 | 0.44 | 0.1 |
| PD-06 | 1.85 | 0.36 | ||
| Plaque score | PS-B | 0.973 | 0.18 | 0 |
| PS-06 | 0.821 | 0.1 | ||
| Facial recession | FS-B | 1.588 | 1.23 | 0.13 |
| FS-06 | 1.176 | 1.38 |
VC: Vertical component; HC: Horizontal Component; KG: Keratinized Gingiva; PD: Probing Depth; PS: Plaque Score; FS: Facial Recession
Table 2: Statistical analysis using paired t test.
A mean reduction of 0.84 mm (± 0.70) was seen in horizontal component which was highly significant with P value <0.05. The baseline mean value of width of keratinized tissue was 5.53 mm (± 1.12) at the papillary region. At 6 month follow up the mean value recorded was 6.37 (± 1.42), showing a gain of 0.84 mm (± 1.23). The gain observed in keratinized tissue was statistically significant with P value <0.05. Reduction in plaque score was statistically significant with P value <0.05, showing good post operative plaque control by patient. There was no statistically significant difference between baseline and 6 months post operative values of pocket depth, with P value >0.05 (Table 2).
Papilla indexscore (PIS) was recorded at baseline and 6 month to assess the gingival contour in relation to teeth associated with papillary loss. Among 20 sites augmented, 7 sites showed a gain of 1 PIS unit, 3 sites showed 2 PIS unit gain, 10 sites had no change in PIS unit.
Among 13 cases, 7 cases were associated with facial recession in relation to teeth adjacent to papillary loss prior to surgical intervention. The mean facial recession at baseline was 1.58 mm (± 1.23) and at the end of study it was 1.18 (± 1.38). The amount of coverage achieved at the end of study was statistically insignificant with P value >0.05.
Discussion
The loss of the interdental papilla is one of the most concerning aspects in the decision-making process of clinicians and in gaining acceptance from the patient. In periodontal literature, the reconstruction of lost papilla for cosmetic reasons has not received much attention. Although several case reports have showed different periodontal plastic surgical, prosthetic, and orthodontic techniques for correcting lost papilla, no scientific research or reliable data are available for clinicians [3]. Most of the literature is limited towards case reports, providing no evidence of predictability and few demonstrate long term stability [6-12]. No controlled clinical trial has addressed the issue of restoring deficient interproximal spaces. The only case series reported so far is by Nemcovsky on 10 consecutively treated cases for papillae reconstruction using a palatal approach [13].
A buccal approach at 6X magnification was used in this study which gives adequate working zone extending to at least two papillae on either side of deficient papillae. A magnified vision and microsurgical instruments provided an easy handling in the narrow zone of interdental papilla and ensured severing of all fibrous attachment at the base of gingivo-papillary unit for maximum coronal advancement [14].
Although the initial case reports by Shapiro [16], did not use connective tissue graft (CTG) for papillary reconstruction, most of the later approaches were based on CTG procured either from palatal region or maxillary tuberosity [7-12]. The amount of connective tissue required for this procedure was assessed to be 2 × 2.5 × 6 mm which was easily harvested using Class I Type A incision technique as described by Liu from palatal region [17]. No adverse outcomes were observed at the donor site.
Authors have used multiple surgeries in an attempt to reconstruct the lost papilla [11]. The main objective of this study was to assess the gain in papillary height that can be achieved with one surgical attempt. To achieve complete fill, embrasure volume to be filled seems more important than bone level. The inter-proximal bone level for cases with complete fill varied from 5 mm-9 mm (Table 1). It was also observed that when multiple papillae are augmented in the same case, more coronal advancement can be achieved with gingivo-papillary unit. All the sites showing complete fill except for one site were in case with multiple papillary augmentation.
Sanctis and Zucchelli, proposed a hypothesis in an attempt to explain the increase of keratinized tissue after connective tissue graft and coronal advancement of flap based on Ainamo and Karrings theory [18]. As described by Ainamo, the mucogingival line always regains its original, ‘‘genetically determined’’ position [19]. It is also known that mucogingival junction remains stationary throughout life and any attempt to coronally or apically advance the mucogingival junction shows relapse towards its original position [20]. Karring et al. reported that the main determining factor for the nature of tissue developing at a region is genetically determined, and it’s the connective tissue that possess the ability to induce changes in the differentiation of the epithelium [21]. The coronal advancement of flap for primary closure which was resting over connective tissue base of keratinized gingiva might have induced the differentiation of alveolar mucosa and hence an increase in width of keratinized tissue achieved in this study.
In this study the gingival contours were assessed at baseline and at the end of the study, using the Papilla index score as suggested by Jemt et al. [22] and modified by Nemcovsky CE [12]. With one surgical attempt at reconstruction of lost papilla there was noticeable improvement in the scalloping and gingival contour at the end of study.
First of the adverse outcome faced was necrosis of graft tissue. Since the interdental space is surrounded by avascular root surfaces on either side, the only source of blood supply is from the coronally advanced gingivo-papillary unit and the crest of the alveolar bone. Any tear or excess trauma to this narrow band of papillary tissue results in compromised vascularity which leads to graft necrosis. Excessive force while inserting the graft into the tunnel is a common error leading to papillary tear. Graft procured from the palate must be trimmed to the size of interdental space and then gently pulled into the space using horizontal mattress suture from the palatal aspect.
An important post operative finding of this study was development of diastema among 6 patients, 5 females and 1 male. In all the cases diastema appeared between central incisors within 2 weeks post operatively. It was observed that these were the cases in which only single papilla was surgically augmented. One of the cases was associated with graft necrosis and diastema formation of 2 mm. All the cases in which multiple sites were augmented, no diastema formation was noticed. Except for one case, all the other cases were managed using hawley’s appliance in consultation with orthodontist. Hawley’s appliance was given after 3 months of surgical procedure so as to ensure complete healing at the donor and recipient site. Diastema closure was achieved in 4 weeks and a fixed retention was placed on the palatal aspect using 0.016 inch co-axial wire and light cure composite.
Formation of midline diastema was an incidental finding of this study. The surgical procedure involved severing of supra crestal fibers including trans-septal fibers during the tunneling procedure. A thick connective tissue graft was then inserted into the tunnel under the coronally advanced gingivo-papillary unit. Trans-septal fibers on the distal surface of the same tooth were not severed in order to avoid damaging the adjacent papilla. An active trans-septal group of fibers on either side [23], with pressure exerted upon by graft and inflammation might have lead to the diastema formation.
Conclusion
In this study, it was observed that connective tissue graft is useful in correction of papillary loss, but its application is limited by the maximum gain that can be achieved with single procedure. A complete fill is feasible for Class I and II papillary loss using microsurgical approach along with microsurgical instruments. Microsurgery improves the access to papillary region but it’s the surgical skill of operator that would define the surgical outcome and better healing. A hands-on training and understanding of microsurgical procedure and instrumentation is must for favorable outcome. It is recommended to use a splint in the region of papillary reconstruction for initial 3 month of healing phase for preventing diastema formation.
The limitations of the study are being of a smaller sample size and short period of follow up. Larger long term clinical and histological follow up studies are necessary before its predictability can be established.
References
- Takei HH, Azzi RR, Han TJ (2006) Periodontal plastic and esthetic surgery. In:Newman MG, Takei HH, Klokkevold PR, Carranza FA (eds.), Clinical Periodontology (10th edn.). Saunders Elsevier, Philadelphia pp: 1005-1029.
- Thomas AH, Henry HT (1996) Progress in gingival papilla reconstruction. Periodontol 2000 11: 65-68.
- Piniprato GP, Rotundo R, Cortellini P, Tinti C, Robert A (2004) Interdental papilla management: A review and classification of the therapeutic approaches. Int J Periodontics Restorative Dent 24: 246-255.
- Burkhardt R, Lang NP (2005) Coverage of localized gingival recessions: Comparison of micro- and macrosurgical techniques. J Clin Periodontol 32: 287-293.
- Burkhardt R, Niklaus PL (2008) Periodontal plastic microsurgery. In: Lindhe J, Niklaus PL, Thorklid K (eds.), Clinical periodontology and implant dentistry(5th edn.). Blackwell Munksgaard, UK pp: 1029-1040.
- Azzi R, Etienne D, Carranza F (1998) Surgical reconstruction of the interdental papilla. Int J Periodontics Restorative Dent 18: 467-473.
- Azzi R, Etienne D, Sauvan J, Miller PD (1999) Root coverage and papilla reconstruction in class IV recession:A case report. Int J Periodontics Restorative Dent 19: 449-455.
- Cardaropoli D, Re S, Corrente G, Abundo R (2004) Reconstruction of the maxillary midline papilla folloming a combined orthodontic-periodontic treatment in adult periodontal patients. JCP 31: 79-84.
- Cardaropoli D, Re S (2005) Interdental papilla augmentation procedure following orthodontic treatment in a periodontal patient. J Periodontol 76: 655-661.
- Azzi R, Daniel E, Takei HH, Carranza FA (2001) Root coverage and papilla reconstruction using autogenous osseous and connective tissue graft. Int J Periodontics Restorative Dent 21: 141-147.
- Carnio J (2004) Surgical reconstruction of interdental papilla using an interposed subepithelial connective graft: A case report. Int J Periodontics Restorative Dent 24: 31-37.
- Nemcovsky CE (2001) Interproximal papilla augmentation procedure: A novel surgical approach and clinical evaluation of 10 consecutive procedures. Int J Periodontics Restorative Dent 21: 553-559.
- Francetti L, del Fabbro M, Calace S, Testori T, Weinstein RL (2005) Microsurgical treatment of gingival recession. Int J Periodontics Restorative Dent 25: 181- 188.
- Cortellini P, Tonetti MS (2001) Microsurgical approach to periodontal regeneration. Initial evaluation in a case cohort. J Periodontol 72: 559-569.
- Wachtel H, Schenk G, Bohm S, Weng D, Zuhr O, et al. (2003) Microsurgical access flap and enamel matrixderivative for the treatment of periodontal intrabony defects: a controlled clinical study. J Clin Periodontol 30: 496-504.
- Shapiro A (1985) Regeneration of interdental papillae using periodic curettage. Int J Periodontics Restorative Dent 5: 27-33.
- Liu CL, Wiesgold AS (2002) Connective tissue graft: A classification for incision design from the palatal site and clinical case reports. Int J Periodontics Restorative Dent 22: 373-379.
- de Sanctis M, Zucchelli G (2007)Coronally advanced flap: A modified surgical approach for isolated recession type defects. J Clin Periodontol 34: 262-267.
- Ainamo A (1978) Influence of age on the location of the maxillary muco-gingival junction. J Periodontal Res 13: 189-193.
- Ainamo A, Bergenholtz A, Hugoson A (1992) Location of the mucogingival junction 18 years after apically repositioned flap surgery. J Clin Periodontol 19: 49-55.
- Karring T, Lang NR, Loe H (1974) The role of gingival connective tissue in determining epithelial differentiation. J Periodontal Res 10: 1-11.
- Jemt T (1997) Regeneration of the gingival papilla after single implant treatment. Int J Periodontics Restorative Dent 17: 327-333.
- Marianne MA, Hom LW (2002)Periodontic and orthodontic treatment in adult. Am J Orthod Dentofacial Orthop 122: 420-428.
Citation: Singh H, Mandlik VB (2018) Surgical Reconstruction of Interdental Papilla using Subepithelial Connective Tissue Graft by Microsurgical Technique: A Clinical Study. J Interdiscipl Med Dent Sci 6: 229. DOI: 10.4172/2376-032X.1000229
Copyright: © 2018 Singh H, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16311
- [From(publication date): 0-2018 - Dec 20, 2025]
- Breakdown by view type
- HTML page views: 14969
- PDF downloads: 1342