Research Article Open Access
The Most Effective Therapeutic Regimen for Patients with Severe Middle East Respiratory Syndrome Coronavirus (MERS-CoV) Infection
| Tawalah HA1, Al-Qabandi S1, Sadiq M1, Chehadeh C2, Al-Hujailan G3 and Al-Qaseer M1* | |
| 1Clinical Virology Unit, Mubarak Al Kabeer Hospital/Health Science Centre, Kuwait | |
| 2Department of Microbiology, Health Science Centre, University of Kuwait, Kuwait | |
| 3Infectious Diseases Unit, AlAddan Hospital, Kuwait | |
| Corresponding Author : | Mamoun Al-Qaseer Faculty of Clinical Virology Kuwait Institute for Medical Specialization P.O. Box 1793, Safat, 13018, Kuwait Tel: +96524636529 E-mail: dr.almamoun@gmail.com |
| Received: March 23, 2015 Accepted: July 06, 2015 Published: July 13, 2015 | |
| Citation: Tawalah HA, Al-Qabandi S, Sadiq M, Chehadeh C, Al-Hujailan G et al. (2015) The Most Effective Therapeutic Regimen for Patients with Severe Middle East Respiratory Syndrome Coronavirus (MERS-CoV) Infection. J Infect Dis Ther 3:223. doi:10.4172/2332-0877.1000223 | |
| Copyright: © 2015 Tawalah AH. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
| Related article at Pubmed, Scholar Google | |
Visit for more related articles at Journal of Infectious Diseases & Therapy
Abstract
Background: More than two years after its discovery, the Middle East respiratory syndrome coronavirus (MERSCoV) continues to have a high case-fatality rate. A specific therapy with proven effectiveness for MERS-CoV infections still does not exist.
Method: MERSCoV-positive patients were treated with different suggested treatment options. The virological and clinical progress of these patients in response to the treatment was evaluated.
Results: Both patients had co-morbidities and were critically ill with acute respiratory distress syndrome on mechanical ventilation at the time of diagnosis. Even though low dose ribavirin/ pegylated interferon α combination was started early for the first patient, it was provided late for the second patient. Both patients recovered from their infection.
Conclusion: By evaluating the clinical and virological response of the patients to the different treatment options implicated, it seems that currently the most effective therapy against severe MERS-CoV infection is the low dose ribavirin/ pegylated interferon α combination.
Initially the patient was managed with biphasic positive airway pressure (BIPAP). However, his condition continued to deteriorate and, four days later, he developed acute respiratory distress syndrome (ARDS) and was transferred to the intensive care unit where he was intubated for mechanical ventilation. The patient was found to be positive for MERS-CoV by RT-PCR in a BAL fluid on November 11 when the oseltamivir and steroids were discontinued. The patient was started on pegylated interferon α2a (PEG-IFN α2a) 180 µg subcutaneously. Oral ribavirin 400 mg every 12 hours with no loading dose was added by the initial treating physician.
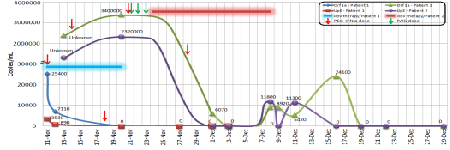
The patient continued to be febrile with temperatures ranging from 38.5-40â�¦C. On November 18, the patient developed acute kidney injury necessitating hemodialysis. On the same day, a second dose of PEG-IFN α2a was given. Two days later, the tracheal aspirate tested negative for MERS-CoV by RT-PCR (Figure 2) and ribavarin was discontinued as a result of gradual drop of the hemoglobin level to 8.9 g/dl (Table 1). The patient was symptomatically managed and steadily continued to improve. The last hemodialysis session he required was on December 2, and he was weaned from the mechanical ventilator on December 9. He was discharged from the hospital on December 23, and started on rehabilitation therapy.
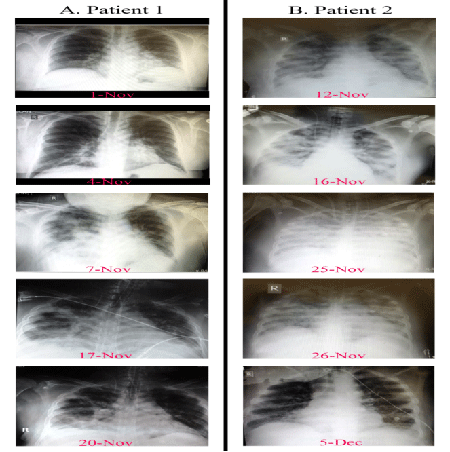
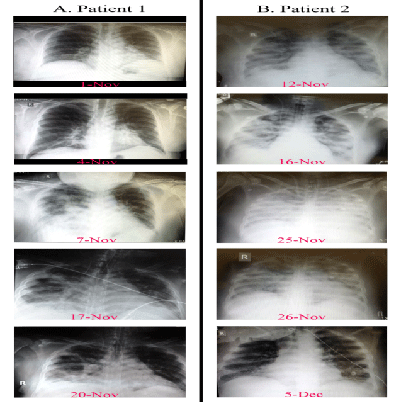
On admission, the patient was started on broad spectrum antibiotics and oseltamivir. Chest radiography showed bilateral interstitial infiltrates with lower lobe consolidations and a minimal right sided pleural effusion (Figure 1b). The initial management with BIPAP was not sufficient and, two days later, the patient was transferred to the ICU where he was intubated for mechanical ventilation. The patient was found to be positive for MERS-CoV by RT-PCR in a BAL fluid on November 13. On the next day subcutaneous pegylated interferon-α2b (PEG-INF α2b) 1.5 µg/kg was given. Intravenous corticosteroids (prednisolone 100 mg/day and hydrocortisone 100 mg three times a day) were also added briefly and were discontinued three days later. The patient continued to rapidly deteriorate which demanded the utilization of extracorporeal membrane oxygenation (ECMO) on November 16. The next day, the patient was started on hemodialysis as a result of acute renal failure. Packed red blood cells were also transfused for the first time as a result of progressive anemia.
The patient showed no signs of improvement. His condition continued to worsen becoming anuric and fully dependent on ECMO support for oxygenation. A second dose of PEG-INF α2b was administered on November 21. Intravenous immunoglobulin (IVIG) (400 mg/kg/day for three days) was also added. However, due to the continuous clinical deterioration of the patient, oral ribavirin was added to the treatment on November 24. A loading dose of 800 mg was given followed by 200mg every 8 hours. Amazingly, significant clinical and virological improvement was noticed. His chest radiography showed marked decrease in the consolidation bilaterally after showing a complete "white out" one day earlier (Figure 1b).
The third PEG-INF α2b was given on November 28. Symptomatic management of the patient included repeated packed red blood cells transfusions and erythropoietin injection to compensate for the hemolytic anemia. On December 3, the patient was weaned from ECMO and MERS-CoV was found to be negative for the first time in endotracheal secretion (Figure 2).
Viral load estimation based on Orf1a quantification is almost always higher than that based on upE quantification. Eventhough, Orf1a and upE became undetectable in Patient 1 at the same time, Orf1a persisted for a longer duration than upE in Patient 2. We should also mention that blood, urine and stool samples were consistently negative for both patients at different stages of the infection. With regards to Patient 3, Orf1a quantification was 4.76 × 104 copies/ml and upE quantification was 4.64 × 104 copies/ml.
Patient 2:
Ribavirin was discontinued on December 8. Interestingly, on the same day MERS-CoV was detectable again in endotrachial secretion. However, the antiviral treatment was not restarted as the patient continued to show clinical improvement and one week later he was undergoing trials of weaning from the mechanical ventilator. On December 19, MERS-CoV was undetectable again in endotracheal secretion by RT-PCR. Unfortunately, after his recovery from MERS-CoV infection, the patient passed away more than a month later, on February 2, as a result of multiple hospital acquired infections with multidrug resistant organisms (Table 2).
Highlights: Two MERS-CoV infected patients were successfully treated
• Different treatment options were utilized
• Clinical and virological parameters of both patients were closely monitored
• The most effective treatment option was , PEG-INF α/Ribavirin combination
• The most sensitive virological monitoring/diagnosis test was Orf1a real-time PCR
It was intended to treat the first patient with PEG-IFN α2a monotherapy. However, ribavirin 400 mg every 12 hours with no loading dose was added by the initial treating physician. After taking over, the drug was not discontinued by the specialist since the dose was not high and the patient did not have contraindications for the drug. Within one week of therapy, when the condition of the patient was stable enough to allow for the collection of tracheal aspirates, MERS-CoV was undetectable in that sample (Figure 2). At this stage, it was not possible to attribute the rapid virological response of the patient to the PEG-IFN α/ribavirin combination. The patient developed the frequent hemolytic anemia known to be associated with this combination which led to the discontinuation of ribavirin nine days after its initiation. However, his situation was possible to manage with few blood transfusions.
The effect of the PEG-IFN α/ribavirin combination can be more elucidated by examining the response of the second patient whose case was more complicated. This patient developed acute renal failure and progressive anemia early during the course of his MERS-CoV infection complicating the utilization of ribavirin in the therapy. Therefore, PEG-INF α2b and a brief course of intravenous corticosteroids were used as a first line therapy. However, due to his continuous deterioration and lack of clinical and virological response, IVIG was added with the intention to modify the inflammatory response and possibly provide the patient with cross reactive antibodies against MERS-CoV. The effect of the addition of IVIG was negligible and the condition of the patient worsened even further reaching a critical stage. As a result, ribavirin was added as a desperate measure to save the patient despite contraindications. The PEG-IFN α/ribavirin combination resulted in significant clinical, radiological, and virological improvements. The tracheal aspirates became negative for MERS-CoV nine days after the addition of ribavirin (Figure 2). Interestingly, the virus was detectable again in tracheal aspirates five days later despite the continuous administration of ribavirin. It is possible the reason for this reactivation is the fading of the effect of the last dose of PEG-INF α2b which was administered ten days before, resulting in the patient receiving ribavirin monotherapy for three days. Even though this reactivation seemed to be of little clinical significance, it may indicate that monotherapy with lower doses of ribavirin is not sufficient to inhibit the replication of MERS-CoV, therefore, supporting the proposed synergistic effect of PEG-IFN α and ribavirin [4].
The most important adverse reaction of the PEG-IFN α/ribavirin combination experienced in treated patients was the drop in hemoglobin level. Few blood transfusions, in addition to erythropoietin for the second patient, were sufficient to stabilize the hemoglobin level above 9 g/dl. No life threatening side effects were witnessed.
It is interesting that the second patient responded well to the treatment even though ribavirin was added 14 days after his admission. Other published cases treated with a related combination were less successful [5]. One reason for this inconsistency could be the early initiation of PEG-IFN α in our case which may have played an important role in enhancing the response to the combination later. Another reason is our utilization of PEG-IFN α which is possibly more effective than the standard IFN α against MERS-CoV.
Another interesting feature that should also be noticed is that the Orf1a was detectable by RT-PCR for a longer duration and in higher quantity than the upE. This may indicate that testing for the Orf1a is more sensitive than the upE for screening and following up patients (Figure 2).
Although the findings highlighted above may indicate that the of PEG-IFN α/low dose ribavirin combination is the most effective therapy for the treatment of MERS-CoV infected patients, stronger evidence is still needed for the determination of the most effective and safest treatment regimen for this infection.
References
- Zaki AM, van Boheemen S, Bestebroer TM, Osterhaus ADME, Fouchier RA (2012) Isolation of a novel coronavirus from a man with pneumonia in Saudi Arabia. N Engl J Med 367:1814-1820.
- Corman V, Eckerle I, Bleicker T, Zaki A, Landt O, et al (2012) Detection of a novel human coronavirus by real-time reverse-transcription polymerase chain reaction.EuroSurveill 17.pii:20285.
- Brown C, Carson G, Chand M, Zambon M (2014) Clinical Decision Making Tool for Treatment of the MERS-CoV v.1.1, 29 July, 2013.
- Falzarano D, de Wit E, Martellaro C, Callison J, Munster VJ, et al (2013) Inhibition of novel β coronavirus replication by a combination of interferon-α2b and ribavirin. Sci Rep 3: 1686.
- Al-Tawfiq JA, Momattin H, Dib J, Memish ZA (2014) Ribavirin and interferon therapy in patients infected with the Middle East respiratory syndrome coronavirus: an observational study. Int J Infect Dis 20:42-46.
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
 |
 |
 |
| Figure 1a | Figure 1b | Figure 2 |
Relevant Topics
- Advanced Therapies
- Chicken Pox
- Ciprofloxacin
- Colon Infection
- Conjunctivitis
- Herpes Virus
- HIV and AIDS Research
- Human Papilloma Virus
- Infection
- Infection in Blood
- Infections Prevention
- Infectious Diseases in Children
- Influenza
- Liver Diseases
- Respiratory Tract Infections
- T Cell Lymphomatic Virus
- Treatment for Infectious Diseases
- Viral Encephalitis
- Yeast Infection
Recommended Journals
Article Tools
Article Usage
- Total views: 16965
- [From(publication date):
August-2015 - Aug 17, 2025] - Breakdown by view type
- HTML page views : 12247
- PDF downloads : 4718
