Research Article Open Access
The Relationship between Femoral Nerve Tension and Hip Flexor Muscle Length
| Philip A Anloague*, Wendy Somers-Chorny, Kelly E Childs, Matthew Frankovich, Carisse Graham and Kasey Birchfield | |
| University of Dayton, Dayton, Ohio, USA | |
| Corresponding Author : | Philip A Anloague University of Dayton Dayton, Ohio,USA Tel: 9038633082 E-mail: panloague1@udayton.edu |
| Received December 16, 2014; Accepted January 06, 2015; Published January 13, 2015 | |
| Citation: Anloague PA, Chorny WS, Childs KE, Frankovich M, Graham C, et al. (2015) The Relationship between Femoral Nerve Tension and Hip Flexor Muscle Length. J Nov Physiother 5:244. doi: 10.4172/2165-7025.1000244 | |
| Copyright: © 2015 Anloague PA, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Adverse neural tension is the inability for a nerve to glide freely in its mechanical interface. Studies demonstrate that there is relationship between muscular facilitation and adverse neural tension in the upper extremity and in the posterior thigh, but few examine a potentially similar interaction in the anterior hip. The purpose of this study was to determine the relationship between femoral nerve tension and hip flexor muscle tightness. The Prone Knee Bend test and the Thomas test were performed on a group of 20 normal subjects (40 unilateral lower extremities) without back pain or dysfunction, and on a group of 12 patients (21 unilateral lower extremities) treated with physical therapy for low back pain. The results demonstrated a significant correlation for the control and patient groups combined (r=0.530; p=0.0001); for the control group only (r=0.322; p=0.043) and the patient group only (r=0.601; p=0.002). This study indicates a correlation between the Thomas Test and the Prone Knee Bend Test suggesting a relationship between adverse neural tension of the femoral nerve and muscle length of the iliopsoas muscle. Increased femoral nerve tension may influence hip tightness in normal and patient populations. Likewise, adaptive shortening of the hip flexors may lead to adverse femoral nerve tension.
| Keywords |
| Femoral nerve; Adverse neural tension; Prone knee bend test; Thomas test |
| Introduction |
| Current neurodynamic concepts can be traced to Cyriax’s work on dural pain and theories on adverse neural tension (ANT) as described by Maitland, Elvey and Butler. The peripheral nervous system is surrounded by connective tissue forming a “neural container.” If a nerve is not able to slide or glide freely within this mechanical interface, adverse neural tension may result [1,2]. ANT has been described in many ways. Butler defines it as “an abnormal physiological and mechanical response produced from nervous system structures when their normal range of movement and stretch capabilities are tested” [3]. Controversy still exists regarding the cause of the decrease in range of movement. Elvey et al. suggest it may be a result of secondary protective muscle spasm due to increased stimulation of the nerve prior to motion [4]. |
| Dysfunctions affecting the nerve can occur mechanically or chemically, and can be extra or intra neural. Extra neural dysfunction occurs when the nerve is unable to move dynamically in relation to its interface. This may lead to decreased ability to glide, slide, translate, or displace, due to either mechanical restrictions or impingement [1]. Areas that are more vulnerable to extra neural dysfunction include: soft tissue, osseous tunnels, fibro-osseous tunnels, nerve bifurcations, anatomical anomalies, fixed areas, and friction sites [2]. Tension points, scar tissue, ectopic bone growth, and facilitated, guarded or tight muscles may also create fixed areas that limit neural motion [2,5,6]. |
| Each time a nerve bifurcates, neural tissue glide is sacrificed, predisposing the structure to adverse tension by either neural entrapment or irritation, possibly resulting in muscle guarding and ultimately increasing the chance of injury [3,7]. |
| Studies on the brachial plexus have suggested facilitation and muscular guarding in relation to anatomical variations in the upper extremity [8,9]. These variations have been linked to increased tone in the upper trapezius and various symptoms in patients who suffer from cervical, thoracic, and/or rib dysfunctions. Other investigators studied the relationship between neural mobility and muscular injuries in Australian Rules football players. They suggested that intervention that included a slump stretch for adverse neural tension in the sciatic nerve was more effective in treating players with a grade I hamstring strain when compared to a group of players treated with traditional intervention. This study presents a possible relationship between ANT of the sciatic nerve and muscular facilitation and strain [10]. |
| Less studied are the lumbar plexus anomalies and the potential adverse affects on neural mobility. The lumbar plexus supplies the anterior thigh, groin, and pubic region and is composed of six major branches formed by the ventral rami of L1 to L3, the upper portion of L4 and occasionally T12. The lumbar plexus then pierces the psoas major muscle, but has been known to have variations and anomalies [11]. Several studies note femoral nerve anomalies occur and may involve piercing by the iliacus or psoas [11-14]. Anloague and Hubijbregts studied anatomical variations of the lumbar plexus and the surrounding musculature in 19 male and female cadavers. Of the 34 unilateral lumbar plexuses deemed appropriate for the study, anatomical variation was noted in 88% of cadavers and in 17% of the nerves studied. Anomalies were noted in the iliohypogastric (20.58%); genitofemoral (47.05%); lateral femoral cutaneous (17.64%). The femoral nerve was found to vary in 35.29% of the investigated lumbar plexes. In these 12 specimens the femoral nerve was observed to bifurcate into 2 and sometimes 3 separate slips. These slips were separated by the fibers of the psoas major before they rejoined and proceeded to pass beneath the inguinal ligament. Most of the cadavers demonstrated a bifurcation of the femoral nerve within the midsubstance of the psoas major where the nerve proceeded to rejoin prior to its exit from the pelvic cavity. One cadaver presented with a medial and lateral bifurcation of the nerve with psoas major musculature passing between, an intermediate connection between the two nerve slips, then a rejoining of the nerve segments [11]. Spratt et al. studied 68 cadaver dissections and reported the presence of variant slips of the psoas and iliacus muscles with splitting of the femoral nerve in 4.4% of these specimens [12]. Jacubowicz noted that in 4.3% of the 60 human fetuses studied the femoral nerve divided into two trunks, anterior and posterior. In one case it was reported that the nerve split into 3 trunks, 2 anterior and one posterior [13]. Adverse neural tension has been linked to increased tone in the surrounding musculature [10,15]. The anomalies may lead to tension on the femoral nerve, which could result in muscle guarding, referred pain to the hip and knee joints and to the lumbar dermatomes of L2, 3, and 4 [6,12]. This raises the possibility that anatomical variations of the femoral nerve in the lumbar plexus may indeed affect hip musculature, specifically the psoas musculature. It must also be considered that the relationship between adverse neural tension signs and muscle dysfunction of the psoas musculature may be bidirectional. While reflexive activity in the psoas may be due to adverse neural tension in the femoral nerve and its roots, adaptive shortening of the psoas may also lead to limitations in neural mobility. |
| Physical and manual therapists have long appreciated the connection between the musculoskeletal and nervous system. This relationship examined via neurodynamic tests to assess the mobility of neural tissue in the extremities. The more popular upper limb tension tests (ULTT) and the straight leg raise (SLR) have received the greatest attention in research. Historically, Wasserman, in 1918, produced the first documented prone knee bend (PKB) to reproduce anterior thigh and shin pain in soldiers whose symptoms could not be reproduced with the SLR [16,17]. The tension from this test is attributed to the femoral nerve, and then to the L2, 3, and 4 nerve roots3. Pain in the anterior thigh experienced during the PKB may indicate tight quadriceps or stretching of the femoral nerve [18].. |
| Although neural tension has been studied in the upper extremity and regarding the sciatic nerve in the lower extremity, the femoral nerve has gone relatively unnoticed [19]. Thus, the purpose of this study was to examine hip flexor guarding, facilitation, or tightness using the Thomas test in conjunction with the PKB test to assess femoral nerve tension. A strong correlation may indicate a potential cause-and-effect relationship between ANT and hip flexor tightness. |
| Methods |
| Subjects |
| A convenience sample of 20 healthy subjects (7 males and 13 females) selected from the physical therapy program at Andrews University and a sample of 12 patients receiving physical therapy for back pain at Orion Physical Therapy (5 males and 7 females) participated in this study. All subjects provided signed written informed consent in accordance with the policies of the Institutional Review Board of Andrews University. Subjects were eligible for the study if they were between ages 18 and 60 and had low back pain for less than 6 months. Subjects were excluded if they had leg pain below the knee and/or had surgical intervention involving the lumbosacral spine. |
| Procedure |
| The Thomas test and the Prone Knee Bend test were performed on each subject by a single qualified physical therapist certified in manual therapy and who is a board certified orthopaedic specialists. Subjects were assigned to patient and non-patient groups. The test order was alternately varied to prevent a testing effect. |
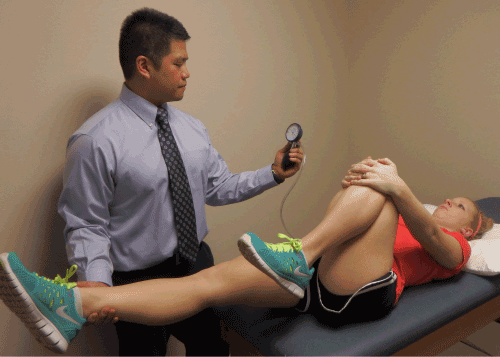
| The Thomas test (Figure 1) was performed with the patient lying supine with a pressurized biofeedback bladder (The Stabilizer from Chattanooga) under the lumbar spine inflated to 40 mmHg to ensure accuracy in determining the outcome. The examiner flexed both of the subject’s knees up to their chest and instructed them to hold one knee while the other was slowly lowered passively to the table. The test was positive if the pressure in the bladder deviated less than 40 mmHg before the leg reached the table due to an anterior tilt of the pelvis. Hip range of motion deficit (Hip ROM Deficit) was recorded via measurement with a universal goniometer. While a positive Thomas test is indicative of tightness in the hip flexors, false positives may be related to weakness in the abdominal musculature, lumbosacral joint instability, or immobility of the hip joint. The test was repeated on the opposite leg and the results were compared. While inter rater reliability was not established, utilization of this device was intended to assist in monitoring anterior tilt of the pelvis (positive sign) in an objective manner. There is little research related to the reliability and validity of the utilization of this device with the Thomas Test at this time. |
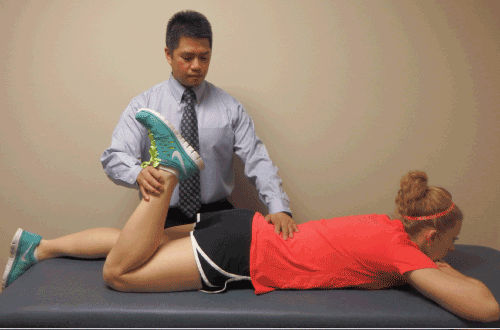
| The PKB test, also known as the femoral nerve stretch test, has received little attention in clinical research. One study published by Kreitz researched the crossed femoral stretching test that was first described by Cyriax in 1947 [17]. Nadler et al. reported on the commonality of false positives due to tight muscles and devised the crossed femoral stretch test, which may improve the specificity of the femoral nerve stretch test [19]. For this reason, we believe that the PKB test should be performed in conjunction with the Thomas test to assess tightness or facilitation in the hip flexor musculature. The Prone Knee Bend (Figure 2) test for femoral nerve tension was performed subsequently on each side with the subject lying prone. The examiner passively flexed one knee slowly as far as possible until the heel touched the buttock, ensuring 0° of hip rotation. The test was positive if there was a reproduction/report of unilateral neurogenic pain (subjectively described as “sharp,” “burning,” “tingling,” “pins and needles,” “hot poker,” etc.) was felt along the lumbar area, buttock, anterior thigh. Knee ROM (ROM PKB) was recorded via universal goniometry at the degree upon which the subjective symptoms were reported. A positive sign is indicative of tension of the femoral nerve or the lumbar nerve roots. Little is known regarding the reliability and validity of the PKB test [3,20]. |
| Statistical analysis |
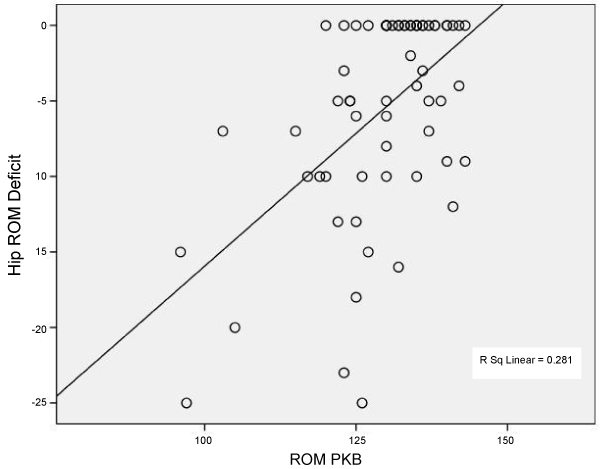
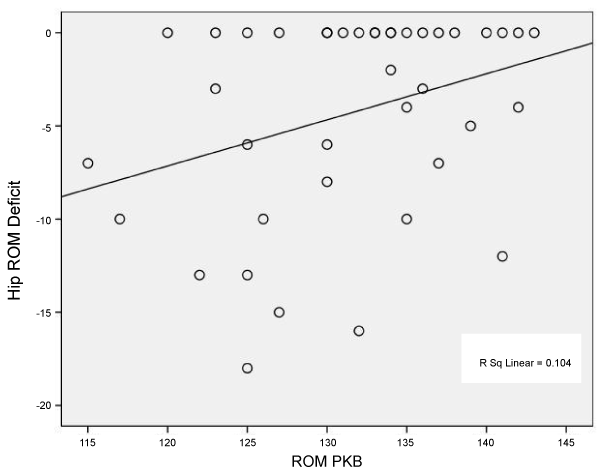
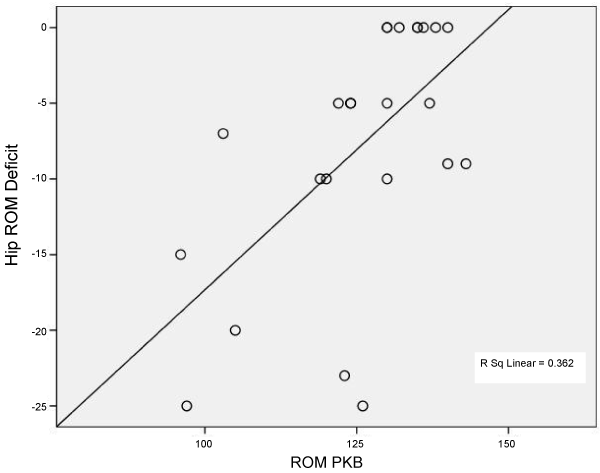
| Data were analyzed using SPSS. Scatter plots of the Thomas Test and the Prone Knee Bend Test measurements were generated to screen data for outliers and to provide evidence of a linear relationship (Figures 3-5). Pearson’s correlations were computed to quantify the strength of the association between the Thomas Test and the Prone Knee Bend Test for the control and patient groups combined (n=32) and for the control (n=20) and patient (n=12) groups individually. Alpha was set at p ≤ 0.05. |
| Results |
| The Thomas Test and the Prone Knee Bend Test were significantly correlated for the control and patient groups combined (r=0.530; p=0.0001); for the control group only (r=0.322; p=0.043) and the patient group only (r=0.601; p=0.002). Tables 1-3 are contingency tables that represent the results obtained for all subjects, symptomatic subjects, and asymptomatic subjects. Figures 3-5 demonstrate the relationship between Hip ROM Deficit and ROM PKB for the combined groups, the control group, and the patient group. |
| Discussion |
| The results of this study indicate that there is a positive correlation between the Thomas Test and the Prone Knee Bend Test suggesting a relationship between adverse neural tension of the femoral nerve and muscle length of the iliopsoas muscle. When reviewing the data for all subjects it was noted that individuals who presented with a positive PKB test (as indicated with a positive sign prior to end range of motion) also demonstrated the greatest ROM deficit with the Thomas Test. In fact, for subjects who had noted the onset of symptoms of ANT earlier in the ROM during the PKB test, the greatest hip ROM deficit was also observed in the Thomas Test. These findings suggest that individuals with ANT of the femoral nerve may display guarding or facilitation of the iliopsoas musculature. While this relationship may be bidirectional, the results also suggest that adaptive shortening of the iliopsoas musculature may lead to ANT. While the control group demonstrated a relationship between the two tests (r=.322), the patient group presented with a stronger correlation (r=.601). Hence, it appears that patients who present with symptomatic, mechanical low back pain should be evaluated accordingly as intervention may necessitate the inclusion of neurodynamic techniques in addition to stretching [21]. |
| The concept of a possible relationship between adverse neural tension and muscular facilitation or shortening is not new. In the upper extremity the relationship between brachial plexus anomalies and upper extremity neural tension has been a well-researched topic [6-9]. Rusnak-Smith et al. reported on the variations found at the scalene triangle. Their investigation on 10 cadavers demonstrated that anomalies of the scalene musculature are often associated with variations of the brachial or cervical plexus [22]. These variations have been linked to increased tone in the upper trapezius and various symptoms in patients who suffer from cervical, thoracic, and/or rib dysfunctions (Rusnak). In the posterior thigh, the sciatic nerve and the straight leg raise test has been studied frequently [15,23-25]. Kornberg and Lew studied the relationship between neural mobility and muscular injuries. Their study included 28 Australian Rules football players who had been diagnosed with a grade I hamstring injury. Sixteen of the subjects were treated with traditional intervention including: rest, ice, compression, elevation, stretches, ultrasound, and interferential therapy. The remaining 12 subjects were treated with the slump stretch in addition to the traditional intervention. The results demonstrated that only one player of the 12 subjects who received the traditional treatment and the slump stretch missed more than one game. In contrast, all 16 players in the group that was treated in the traditional manner missed one or more games. It was concluded that the slump stretch, combined with traditional treatment, is more effective in treating Australian Rules football players with a grade I hamstring strain suggesting a relationship between ANT of the sciatic nerve and muscular facilitation and strain [10]. |
| There is a paucity of research regarding adverse neural tension of the femoral nerve and the implications for iliopsoas muscle length and flexibility. When nervous tissue has tension or is inflamed, the surrounding muscles may become facilitated, giving the muscles a protective role [6]. Studies have shown that patients testing positive on neurodynamic tests are more prone to ankle sprains, hamstring sprains, tennis elbow, and thoracic outlet syndrome [2,21]. In a study by Turl, it was demonstrated that 57% of Rugby players presenting with a repetitive grade I hamstring strain also had a positive slump test compared to the control group [21]. In cases concerning the lumbar spine, shortening of the hip flexor musculature increases the likelihood of lumbosacral sprains [25]. |
| A positive relationship between the two tests would suggest the importance of treating neural tension in conjunction with the muscle facilitation. The results of this study demonstrate a positive relationship between the two tests in both the normal and the patient populations. In the normal population, the relationship was small but statistically significant. It was anticipated that the normal population, having no injuries to the back, would test negative to both tests. These findings are clinically relevant when related to data obtained from the patient population, where the normal population tests negative to both tests and patients with low back pain test positive to both tests. A positive relationship was found to be large in the patient population. |
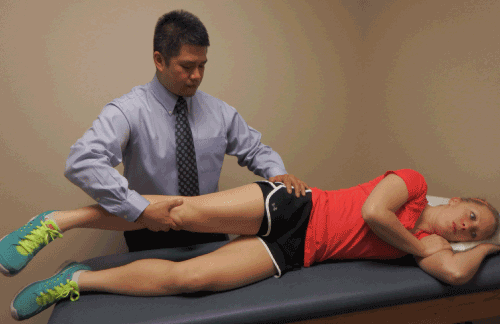
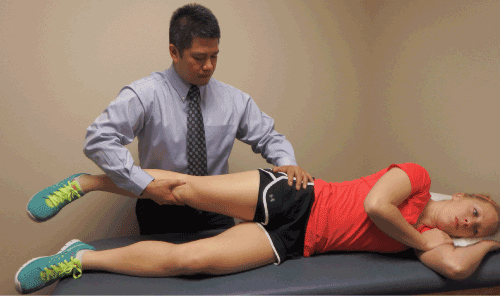
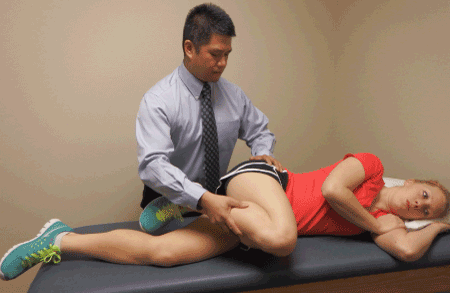
| Mobilization of the femoral nerve can be conducted manually or via patient self-management. While detailed instruction regarding the treatment for ANT of the femoral nerve is beyond the scope of this paper, a general overview can provide insight to the clinical relationship between the presence of peripheral nerve dysfunction and intervention. The initial technique of neural mobilization should be non-provoking without causing an increase in patient symptoms [26-28]. There should be continual monitoring of symptoms with constant verbal and nonverbal communication between the therapist and patient. A common slider technique (Figures 6 and 7) for manually gliding the proximal aspect of the femoral nerve involves placing the patient on the their contralateral side. The therapist stands behind the patient with the cephalad hand supporting and monitoring the ipsilateral hip and pelvis as the caudal hand supports the ipsilateral leg. The therapist then passively brings the hip into extension and performs slow and rhythmic oscillations. A distal slider technique for the femoral nerve can be performed in a similar fashion with the hip and knee flexed (Figure 8) [28]. It has been suggested that large amplitude Grade II mobilizations can be performed with consideration of patient symptoms [26-28]. The technique can be modified with regard to the number of repetitions, amplitude, or amount of tension but it is important to continually assess the patient and only change one variable at a time. The technique can also be modified for self-mobilization (Figure 9). While it has been suggested that the appropriate utilization of neural gliding techniques may be effective in reducing pain and dysfunction [29-36] much more clinical research is needed to prove its efficacy [29,30]. |
| There are several limitations to this study. Foremost, the number of subjects in the patient group, and subsequently the power of the study, was low. Secondly, validity and specificity has not been proven with the prone knee bend test. It may be associated with false positives due to tight muscles of the anterior thigh or joint pathology at the hip [19]. The results of this study should not be affected due to the concomitant utilization of the Thomas test to determine hip flexor tightness. Because there is little data on the reliability of the Thomas Test and the Prone Knee Bend Test, future studies should include the establishment of intra-rater reliability of the examiner prior to the onset of the study. |
| Conclusion |
| The results of the current study demonstrated an association between a positive Thomas test and a positive prone knee bend test in the patient population. The findings of this pilot study suggest that increased femoral nerve tension may influence hip tightness in normal and patient populations or, adaptive shortening of the hip flexors may lead to adverse neural tension. Future research in this area should include the establishment of inter and intra-rater reliability of the tests utilized in this study. Also, further studies must include a greater number of subjects to that statistical power may be improved. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 |
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
 |
 |
 |
 |
| Figure 6 | Figure 7 | Figure 8 | Figure 9 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 32704
- [From(publication date):
February-2015 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 27082
- PDF downloads : 5622
