Research Article Open Access
Unreamed Intramedullary Nailing Versus External Fixation for Type IIIA and IIIB Open Fractures of Tibial Shaft: A Subgroup Analysis of Randomized Trials
| Zhuang Cui, Bin Yu*, Changpeng Xu, Xue Li, Jinqi Song, Hanbin Ouyang and Liguang Chen | |
| Department of Orthopedics and trauma, Nan Fang hospital, Southern Medical University, Guangzhou, Guangdong province, PR China, 510515 | |
| Corresponding Author : | Bin Yu NO,1838 Guangzhou Da Dao Bei Orthopedics and trauma, NanFang hospital Southern Medical University, Guangzhou Guangdong province, PR China, 510515 Tel: 18620087757 Fax: 020-61641888 E-mail: buzaiyouyu5945@163.com |
| Received April 20, 2013; Accepted April 30, 2013; Published May 02, 2013 | |
| Citation: Cui Z, Yu B, Xu C, Li X, Song J, et al. (2013) Unreamed Intramedullary Nailing Versus External Fixation for Type IIIA and IIIB Open Fractures of Tibial Shaft: A Subgroup Analysis of Randomized Trials. J Nov Physiother 3:144. doi:10.4172/2165-7025.1000144 | |
| Copyright: © 2013 Cui Z, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Objects: The aim of this article is to provide a comprehensive and concise review of the literature and subsequent meta-analysis of data regarding the effect of unreamed intramedullary nailing versus external fixation for type IIIA and IIIB open tibial fractures.
Methods: We selected PubMed; Cochrane Library; EMBASE; BIOSIS; Ovid and the relevant English orthopedic journals and pooled data from eligible trials including six eligible prospective randomized trials comparing unreamed intramedullary nailing and external fixation for type IIIA or IIIB open tibial fractures to conduct a subgroup analysis, aiming to summarize the best available evidence.
Results: The results showed compared with external fixation, unreamed intramedullary nailing led to fewer superficial infection rate in patients with type IIIA (95% confidence interval (CI) 0.04–0.39, P=0.0003) and type IIIB open tibial fractures (95% CI 0.22–0.86, P=0.02). And there was the trend of obtaining better clinical effect towards less deep infection rate in unreamed intramedullary nailing group for patients with type IIIA and IIIB open tibial fractures, respectively (95% CI 0.29–1.77, P=0.47) and (95% CI 0.12–1.17, P=0.09), although no significant differences were viewed. Meanwhile, unreamed intramedullary nailing reduced the incidence of reoperation (95% CI 0.25–0.85, P=0.01) and malunion (95% CI 0.14–0.50, P<0.0001) and shortened the radiographic time to union (95% CI (-5.54, -1.86), P<0.0001) while no significant difference was viewed towards nonunion rate (95% CI 0.50–2.77, P=0.71) in patients with type III open tibial fractures.
Conclusions: We suggest that the final results are significant and there are some evidences supporting the use of unreamed intramedullary nailing for type IIIA and IIIB open tibial shaft fractures. Limitations remain, operative duration, blood loss and some functional evaluation indicators such as range of motion in ankle and knee should be more carefully considered and reported in a reliable, consistent and standardized manner.
| Keywords |
| Tibial shaft fractures; Type III; Unreamed intramedullay nailing; External fixation; Meta-analysis |
| Introduction |
| Tibial fractures are one of the most common long bone fractures, constituting the majority of emergency operating room procedures in most trauma centers. The annual incidence of 492,000 fractures of the tibia and fibula has been reported by the national center for Health Statistics in the United States [1] and type III open fractures of the tibia are among the most difficult to treat, because of the poor softtissue cover and blood supply of the tibial shaft. |
| For the treatment of type III open fractures of tibia, it still rests controversy in the choice of various fixation methods such as reamed intramedullary nailing (IMN), unreamed intramedullary nailing and external skeletal fixation. Choosing between the reamed and unreamed nailing methods is a basic discussion for treating tibial shaft fractrures. Data from the SPRINT trial [2] and the recent Meta-analysis [3] demonstrated that no significant differences were viewed comparing reamed and unreamed nailing in patients with open tibial fractures. In this study, we focus on the comparison between unreaming nailing and external fixation for type III open tibial fractures. External fixation has been popular because of the relative ease of application and the limited effect on the blood supply of the tibia, however its use is also associated with significant rates of malunion and pin tract infection often necessitating premature removal and conversion to alternate forms of stabilization [4-6] Unreamed IMN technique avoids pin-track infection and theoretically offer anatomic alignment of the limb, even in the presence of bone loss or comminution, [7,8] but potentially may compromise stability at the site of the fractures [9,10] By now, there have been some prospective randomized trials basically aimed to compare the effect of unreamed IMN and external fixation for type IIIA or IIIB open tibial shaft fractures [11-16]. However, the optimal treatment of severe type IIIA or IIIB open fractures of the tibial shaft remains ongoing debated, so we pool data from eligible randomized trials to conduct a subgroup analysis, aiming to summarize the best available evidence. |
| Materials and Methods |
| Inclusion and exclusion criteria |
| We included only studies meeting the following criteria: randomized trials comparing unreamed IMN and external fixation; patients included who are bone mature and have sustained type IIIA or IIIB open fractures of the tibial shaft; trials reporting clinical outcomes, complications. Trials would be excluded if patients had the following conditions: other fracture needing treatment; ongoing radiotherapy or chemotherapy; pathologic fracture; metabolic disease or medication affecting the bone. Patients included in all studies having appropriate therapy for the first time. |
| Search Strategy |
| According to guidelines from the Cochrane collaboration, [17] we selected PubMed; Cochrane Library; EMBASE; BIOSIS; Ovid, all databases were searched from the earliest records to October 2011. The following keywords were used: open fracture of tibia; type IIIA or IIIB; unreamed intramedullary nailing; external fixation. The type of articles was limited to prospective randomized controlled trials. We also examined the reference lists of eligible studies for potentially relevant reports and searched for reference in the Cochrane Central Register of Controlled Trials. |
| Studies selection |
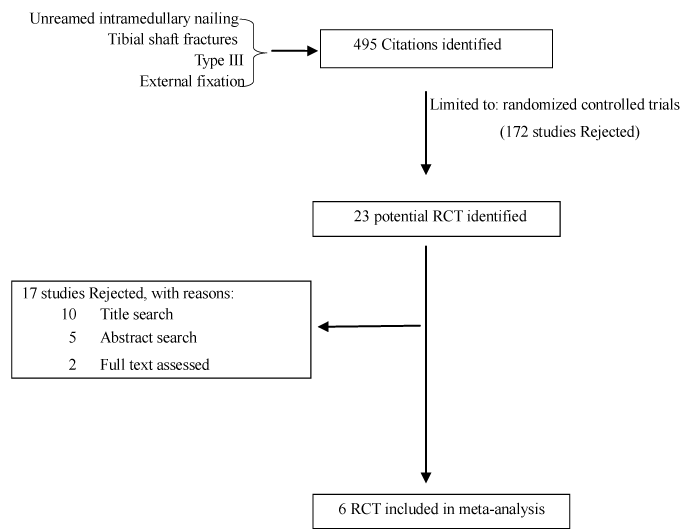
| Trials were included if they were prospective randomized controlled trials comparing unreamed IMN and external fixation for patients with type IIIA or IIIB open tibial shaft fractures. Titles and abstracts were reviewed independently by two of us; all relevant articles were then retrieved and read to determine their eligibility. And a flow chart of study selection process [18] was presented in figure 1. |
| Data extraction |
| All relevant data from papers that met the initial inclusion criteria were extracted independently by two of the authors. Disagreement was resolved by discussion. We sought the following summary data from each study: (1) information on general characteristics of participants; (2) postoperative complications (superficial infection rate and deep infection rate); (3) reoperation rate (4) time to union; (4) malunion and nonunion rate. |
| Statistical analysis |
| Subgroup analyses were carried out to assess the incidence of postoperative complications such as superficial and deep infection rate in patients with type IIIA or IIIB open fractures of tibial shaft. We used a fixed effects model in the meta-analysis unless there was significant heterogeneity between studies, when we used the random effects model of DerSimonian and Laird. Complying with QUOROM guidelines, [19] trial heterogeneity was estimated using the I2 statistic, which describes the percentage of total variation across studies that is due to heterogeneity rather than chance. I2 can be readily calculated from basic results obtained from a typical meta-analysis as I2=100% x (Q–df)/Q, where Q is Cochrane’s heterogeneity statistic and df is the degrees of freedom [20]. Substantial heterogeneity exists when I2 exceeds 50 percent. Dichotomous data were presented as odds Ratio (OR) and continuous variables as weighted mean difference (WMD), both with 95% confidence intervals (CI). The meta-analysis was performed by RevMan 5.0.25 software (The Cochrane Collaboration, Oxford, UK) for outcome measures, a P value of <0.05 was considered statistically significant. |
| Study quality evaluation |
| Two reviewers independently graded each randomized trials using the modified Jadad scale [21]. The modified Jadad is an eightitem scale designed to assess randomization, blinding, withdrawals/ dropouts, inclusion/exclusion criteria, adverse effects, and statistical analysis, presented in table 1. The score for each article can range from 0 (lowest quality) to 8 (highest quality). Scores of [4-8] represent good to excellent (high quality) and 0 to 3 poor or low quality. |
| Sensitivity analysis |
| Sensitivity analysis was used to assess how robust the results are uncertain decisions or assumption about the data and the methods that were used [22]. To analyze the sensitivity of our study, some studies were excluded because they were of low quality with Jadad score of 3 or under 3. They may weaken the conclusions. |
| Results |
| Literature search |
| There were 495 potentially relevant papers. When the type of articles was limited to randomised controlled trials, 23 potential RCT were identified. By screening the title, reading the abstract and the entire article, 17 citations were rejected because of not limited to type III open tibial fracture towards fracture type, retrospective design or no effective data that could be extracted for analysis. Finally, 6 published prospective randomized trials met all the inclusion criteria and were proved eligible for this investigation. Table 2 provides a summary of the studies: author, design, year of publication, age, sample size, follow-up period and Jadad Scores. |
| The results of postoperative infection rate |
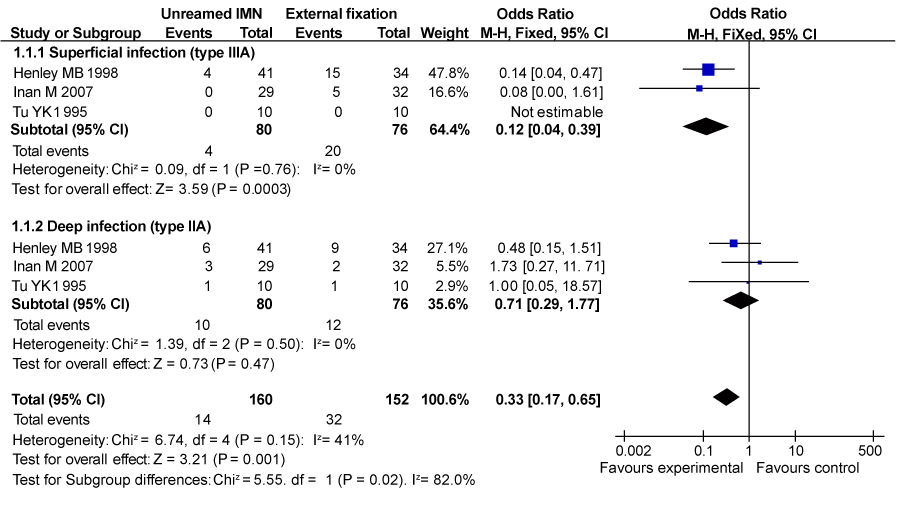
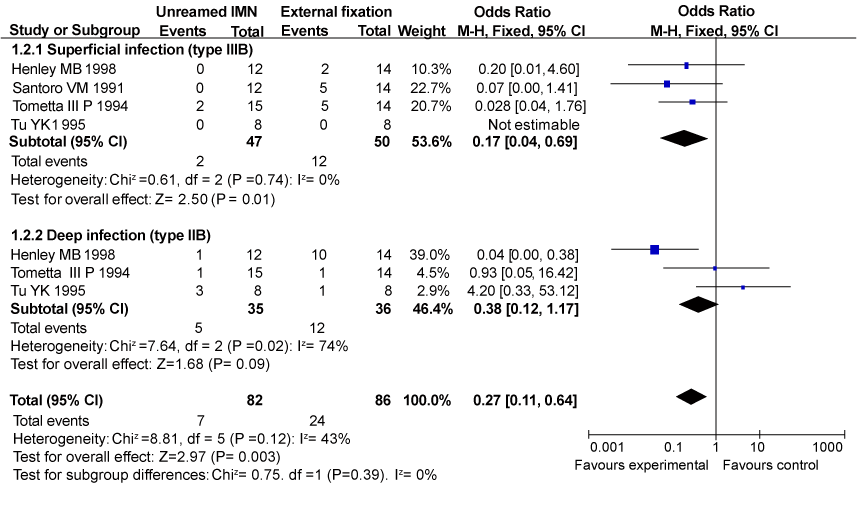
| There were three trials reported superficial and deep infection rate in type IIIA open fractures of tibia while four trials reported superficial infection rate and three provided data about deep infection rate in type IIIB tibial fracture, presented in figures 2 and 3. The subgroup analysis results showed compared with external fixation, unreamed intramedullary nailing led to fewer superficial infection rate in patients with type IIIA (95% confidence interval (CI) 0.04– 0.39, P=0.0003) and type IIIB open tibial fractures (95% CI 0.22–0.86, P=0.02), and there was the trend of obtaining better clinical effect towards less deep infection rate in unreamed intramedullary nailing group for patients with type IIIA and IIIB open tibial fractures, respectively (95% CI 0.29–1.77, P=0.47) and (95% CI 0.12–1.17, P=0.09), although no significant differences were viewed. |
| The results of reoperation rate |
| Six articles provided data regarding to the incidence of reoperation. As the results showed, unreamed intramedullary nailing led to fewer reoperation rate than that in external fixation group (95% CI 0.25- 0.85, P=0.01) for patients with type III severe open fractures of tibia. |
| The results of radiographic time to union |
| Radiographic union was defined as bridging callus on anteroposterior and lateral radiographs, with no pain on palpation or weight-bearing. Three articles provided data about radiographic time to union, reported in the standardized manner of Mean and Standard deviation. As the results showed, the time to bony union was superior in unreamed intramedullary nailing group than that in external fixation group (95% CI (-5.54, -1.86), P<0.0001) for patients with type III severe open fractures of tibia. |
| The results of malunion and nonunion rate |
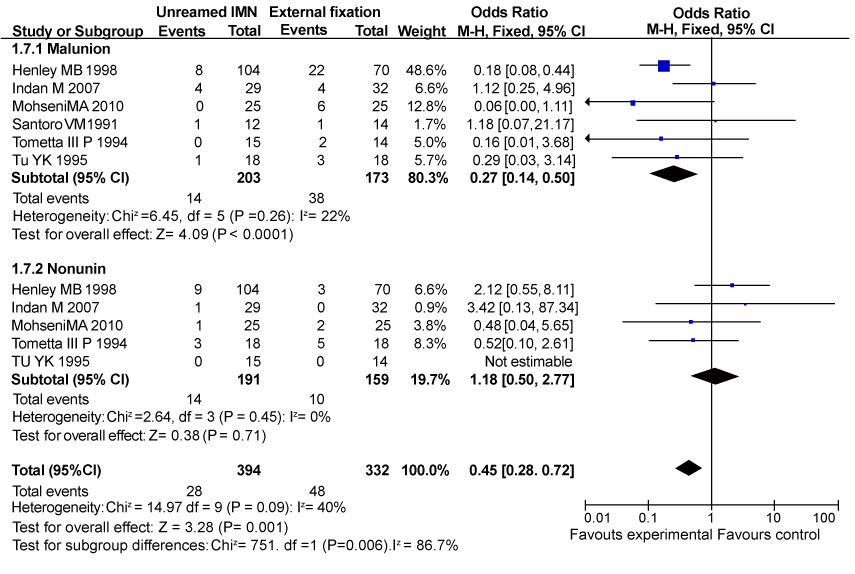
| There were six trials reported the incidence of malunion and five article provided data about nonunion rate in type III open tibial shaft fractures, presented in figure 4. The subgroup analysis showed that unreamed IMN reduced the incidence of malunion (95% CI 0.14– 0.50, P<0.0001) while there were no significant differences towards nonunion rate (95% CI 0.50–2.77, P=0.71). |
| The results of sensitivity analysis |
| The sensitivity analysis revealed that with low quality study (Jadad score of 3 or under 3) excluded, the summary OR, 95% CIs and P value for malunion and reoperation rate (as these were outcomes most studies included in the meta-analysis) were still similar to the results before it was excluded, which are (95% CI 0.13–0.48, P<0.0001) and (95% CI 0.24–0.82, P=0.01) respectively, indicating that the results of our study are reliable and believable. |
| Discussion |
| Principle findings |
| Our subgroup meta-analysis has showed that compared with external fixation, unreamed IMN led to fewer superficial infection rate in patients with type IIIA and type IIIB open tibial fractures, and there was the trend of obtaining better clinical effect towards less deep infection rate in unreamed IMN group for patients with type IIIA and IIIB open tibial fractures, although no significant differences were viewed. Meanwhile, unreamed IMN reduced the reoperation and malunion rate and shortened the radiographic time to union comparing with external fixation in patients with type III severe open fractures of tibial shaft |
| Strengths and limitations |
| Our meta-analysis differs from earlier analyses in several ways [23,24]. We included several recently published studies aimed to compare unreamed IMN and external fixation for the treatment of type IIIA and IIIB open tibial shaft fractures. The trial by Bhandari et al. [23] did not contain novel studies after 2001 and did not limit tibial fractures to type III severe open fractures of tibia. The study by Dervin [24] only included two studies and also no recent literatures after 1996, without concerning the incidence of deep infection, reoperation and malunion rate. Our study is strengthened by the comprehensive search and only prospective randomized trials were included. Meanwhile, subgroup analysis contributes to the higher clinical consistency and more reliable analysis results. |
| However, all meta-analyses are subject to potential bias and our study was not excluded. For methodological limitations resulted from variations in operative technique and treatment protocols between trials investigating the same technology, a differential expertise bias might have existed in our study. Although we have undertaken a comprehensive search strategy, we have not included any unpublished trials. A publication bias might exist. Inconsistent reporting of outcomes across trials also raises the possibility of selective reporting bias [25]. |
| Clinical implications |
| The choice of unreamed IMN or external fixation for the treatment of type III open tibial shaft fracture remains controversial. Our meta-analysis showed that unreamed IMN led to a lower risk of superficial infection and had a trend of obtaining better clinical effect towards less deep infection rate in type IIIA and IIIB open fractures of tibia. Several reasons may account for these. Firstly, as expected, the external fixation group was prone to pin tract problems, [13] and these problems contributed to a statistically significant higher incidence of superficial infection. Meanwhile, pin-track infection may further result in deep soft tissue infection, so there was the trend of obtaining worse clinical effect towards deep infection rate in external fixation group, though no significant difference was viewed. Secondly, theoretical arguments based on blood supply to the fracture may favor external fixation, but Rhinelander et al. [26] found that unreamed IMN interrupted the blood supply only temporarily and then only when there was direct contact with the cortex, and in fact, small diameter unreamed nails do not require a tight interference fit, and need very little cortical contact for stability. |
| With regard to other results, our meta-analysis revealed that unreamed IMN reduced the incidence of reoperation comparing with external fixation in patients with type III open tibial fractures. Rates of reoperation after open tibial fracture varied between 4% and 48% in studies which include a variety in the severity of softtissue damage and patterns of fractures [13-15, 27-31]. Surgeons can generally identify patients as low risk or as high risk for reoperation according to soft-tissue injury and patterns of fractrues, and for those patients with severe type III open fractures (high risk), unreamed IMN should be utilized to decrease the occurrence of reoperation. Meanwhile, unreamed IMN reduced malunion rate and shortened the radiographic time to union comparing with external fixation in patients with type III open fractures of tibia. The major advantage of unreamed intramedullary nails is that alignment is maintained without additional periosteal damage and theoretically with minimal disruption of the medullary vasculature [32] which may contribute to the lower incidence of maluion and encouraging healing. |
| In addition, the choice of reamed versus unreamed nails for patients with tibial fracture was also ongoing debated. Data from the SPRINT trial2 and the recent Meta-analysis3 revealed that reamed nails might be a better alternative for patients with closed tibial fractures, but no significant differences were viewed in patients with open tibial fractures. Reamed nailing caused more damage to the endosteal blood supply while inducing a six-fold increase in the periosteal blood flow, [33] but in the patients with open fractures, this process of assistant revascularization were interrupted by surrounding soft tissue and periosteum damage. This might be why there were no significant differences in open fractures comparing reamed and unreamed nails. In this study, we focus on the comparison between unreaming nailing and external fixation for type III open tibial fractures. |
| In summary, we suggest that the final results are significant and there are some evidences supporting the use of unreamed IMN for type IIIA and IIIB open tibial shaft fractures. Limitations remain, further studies comparing these interventions should therefore include functional evaluation indicators such as range of motion in ankle and knee in the manner of mean and standard deviation at follow-up periods for the decision making in the treatment of type III tibial fractures. In addition, for better health, we need to more carefully consider the operative duration, blood loss and patient acceptance and report them in a reliable, consistent and standardized manner. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 14185
- [From(publication date):
May-2013 - Aug 19, 2025] - Breakdown by view type
- HTML page views : 9559
- PDF downloads : 4626
