Research Article Open Access
Use of Root Cause Analysis to Prevent Falls and Promote Patient Safety in Clinical Rehabilitation
| Shih-Hui Wu1 and Ru-Lan Hsieh2,3* | |
| 1Department of Physical Medicine and Rehabilitation, Cardinal Tien Hospital, Taiwan | |
| 2Department of Physical Medicine and Rehabilitation, Shin Kong Wu Ho-Su Memorial Hospital, Taiwan | |
| 3School of Medicine, College of Medicine, Taipei Medical University, Taipei, Taiwan | |
| Corresponding Author : | Ru-Lan Hsieh Department of Physical Medicine and Rehabilitation Shin-Kong Wu Ho-Su Memorial Hospital, No. 95 Wen-Chung Rd, Shih-Lin District, Taipei 111, Taiwan Tel: +866-228332211 Fax: +866-228389319 E-mail: M001052@ms.skh.org.tw |
| Received March 22, 2013; Accepted April 09, 2013; Published April 11, 2013 | |
| Citation: Wu SH, Hsieh RL (2013) Use of Root Cause Analysis to Prevent Falls and Promote Patient Safety in Clinical Rehabilitation. J Nov Physiother 3:132.doi: 10.4172/2165-7025.1000132 | |
| Copyright: © 2013 Wu SH, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Objective: To apply Root Cause Analysis to explore the causes of patient falls and determine the implement procedures to prevent them.
Design: Root Cause Analysis was conducted retrospectively using comprehensive error review to discover and correct the causes of errors.
Setting: Physical medicine and rehabilitation department in a medical center in Taiwan. Interventions: We used causal trees to clarify possible reasons for patient falls, including the patients’ personal characteristics, factors pertaining to the interactions among the medical team, the team’s workload and level of training, and the quality of communication between medical staff and the patient. In advance, Root Cause Analysis was analyzed by using reactive barriers for each factor.
Main outcome measures: Incidence and complications of patient falls before and after Root Cause Analysis.
Results: No patient falls occurred during the first 6 months after implementing the measures identified in the analysis. Two falls occurred after 6 months, but the patients were both assisted promptly and suffered no injuries. The annual incidence of falls decreased from 4.8 per 100,000 subjects to 1.9 and 0.9 in the next two years of follow up, respectively.
Conclusion: The application of root cause analysis in the setting of clinical rehabilitation did not completely prevent falls. However, the incidence and complication of falls were reduced. Therefore, it is worthwhile to promote application of Root Cause Analysis to clinical rehabilitation treatment to enhance the quality of patient safety in the future.
| Keywords |
| Root cause analysis; Patient safety; Falls; Rehabilitation medicine |
| Introduction |
| It is estimated that in 2030 the geriatric population will increase to 20% of the total population from 12.4% in 2000 [1]. Aging itself will bring many functional disabilities. Among people who are over 65 years of age, about 55% of them will encounter situations of limited ability in daily functions, movement, or cognition; this number rises to about 74% among people of over 80 years of age [1]. These disabled persons usually need some assistance in daily life and consume as much as 46% of adult medical health cost [1]. In Taiwan, 10.7% of the population was older than 65 years and 15.2% was older than 60 years in 2010 [2]. Over the last decade, the rates of population older than 65 years and 60 years have respectively increased by 24.6% and 25.8% [2]. Our previous community-based geriatric health status survey showed that 3.4% of those surveyed scored <60 on the Barthel index while 1.5% scored 65~85, and 95.1% scored 90~100 [3]. The prevalence of disabilities in Taiwan increased from 3.7% to 4.5% from 2002 to 2007, for an increase of 22.8% [4]. |
| Falling is a serious issue as the elderly population grows all over the world. Fall prevalence was reported to be one-fourth to onefifth among elderly populations [5]. Falling is the most commonly seen accident, which can happen easily during transfer or positionchanging, because of overly-high bed positions, desks or chairs, and lack of installation of safety features in the bathroom. Serious complications, such as fractures, neurologic or soft tissue damages, shoulder dislocation, and even death may follow falls. In Taiwan, among people over 65 years of age (10% of the total population in 2006), accidental injury was the seventh leading cause of death [6]. The average number of deaths caused by falls in the elderly was 146.8 annually from 1985~1994, which accounted for 43.81% of all deaths [6]. According to the Bureau of Health Promotion, Department of Health in Taiwan, the incidence of falls in the geriatric population increased to 20.5% in 2005, from 18.7% in 1999 [7]. The probability of a second fall was 39.2% and about 66% occurred outdoors [6]. Women suffered more falls, but men suffered a slightly higher mortality rate [7]. |
| Patient falls are a type of medical error commonly seen in clinics, especially among the patients in rehabilitation clinics, most of whom are elderly or incapacitated. Such medical errors may result from improper medical systems, lack of teamwork, insufficient medical specialization, and inadequate communication between patients and medical staffs or between medical specialists. Prevention of falls becomes an important health related outcome, but this information mainly focuses on falls in the home or community setting. In order to reduce the impact of medical errors, many preventative measures have been adopted. |
| Among them, Root Cause Analysis (RCA) is a commonly applied method in which researchers conduct a retrospective comprehensive error review to discover one or more reasons for the errors and correct the fundamental cause [8]. RCA has been applied primarily in industry to define the proximate and root causes that trigger incidents, especially in high-risk industries such as nuclear power or aviation safety. In the past, analyses of medical errors often ascribed the causes of the errors to the patients themselves or the medical implementers. However, through RCA, the real cause of an error in the procedure or system can be explored. RCA involves three questions: what happened, why did it happen, and what can be done to prevent it from happening again? Every RCA will need 20-90 person-hours to finish the assessment [8]. |
| Most of the patients who receive rehabilitation treatment are old and disabled. Medical errors could be related to fall accidents and result in more serious harm to these patients. The study examines falls in a hospital environment, such as at the department of physical medicine and rehabilitation, may have different context and reasons for falls comparing to falls at home or community setting. Comprehensive review is needed for prevention of the fall accident in patients receiving rehabilitation programs in hospital. It is routine use for investigation of every serious adverse event. However, to our knowledge, there has still been no systematic analysis of RCA-related research in the field of rehabilitation medicine. Therefore, in this study, we applied RCA in the department of physical medicine and rehabilitation in a medical center in Taiwan to identify the reasons for falling, to determine procedures to prevent falls and to implement those procedures. We hypothesized that use of RCA to prevent falls in the department of physical medicine and rehabilitation could reduce the incidence and complications of falls in patients receiving rehabilitation programs effectively. |
| Materials and Methods |
| Setting |
| In Taiwan, National Health Insurance was implemented in 1995 and the coverage rate was 99% at present [9]. The public has received comprehensive medical cares, including inpatient/outpatient care, laboratories test, prescription drugs, and rehabilitation programs. Shin Kong Wu Ho-Su Memorial Hospital is a medical center located in northern Taiwan with 921 beds [10]. Our rehabilitation ward constitutes of 14 beds. We have 20 outpatient clinics in one week with average of 24 patients per clinic. The average daily capacity of patients receiving rehabilitation programs in our department is about 370 persons, including patients from clinic and inpatient consultation. The team consists of 8 qualified attending physiatrists (4 full-time, 4 part-time), 4 residents, 18 physical therapists, 7 occupational therapists, 2 speech therapists, 1 psychologist, 3 counter clerks, 1 technician, 1 assistant and 2 nurses. The rehabilitation programs (including occupational therapy, speech therapy, physical therapy, and psychological therapy) are all prescribed by physiatrists. |
| Investigation process |
| We collected all subjects with falls when receiving rehabilitation treatment from December 2007 to March 2008, and followed up for 2 years. The fall was defined as an event resulting from a person coming to rest on lower level or on the ground inadvertently with either loss of consciousness, injury or not [11]. Falls from major intrinsic events, such as seizure or stroke, were excluded. |
| Every fall process was recorded immediately by our staffs and reported at monthly routine meeting in our department. We used the first injurious case as an example to establish preventive mechanisms through RCA meeting. The participants in the RCA meeting included relevant physiatrist, therapist, nurses and counter clerks. A causal tree was used to display possible causes of falls. After the implementation of preventive measurements, we analyzed all the fall cases from May 2008 to December 2008. The case number and complications of falls before and after the RCA were compared. |
| RCA method |
| Through graphic display, all the possible links that influence the incidents are represented together. During the analysis, we should ask ourselves the two questions “Why?” and “What else?” constantly, to broadly extend the details of the causal tree. In order to successfully discover the causal factors and to demonstrate the usefulness of incident reporting, we took the culture of the organization, standardized methodologies, classification systems, tools for analysis, and feedback to staff into consideration in the RCA [12]. RCA was performed using reactive barriers. If the preventative mechanisms - evaluating the patient’s risk category and determining the suitability of the patient’s overall condition for rehabilitation treatment at the time—could be implemented effectively, the incidence of patient falls would decrease. |
| The annual incidence of falls was calculated as the number of subjects with falls when receiving rehabilitation treatment in the department of physical medicine and rehabilitation divided by the total number of subjects who received rehabilitation treatment in one year. The annual incidence of falls is presented as rate of falls per 100,000 subjects per year. |
| Results |
| Background |
| The first case involved an 82-year-old woman who had a history of hypertension, cardiac disease, and esophageal cancer (after surgery). She received physical therapy in the rehabilitation clinic because of her low back pain. The patient always traveled alone to the clinic by bus. In January 2008, she fell down when she was about to get out of the treatment bed after therapy resulting in contusions and bleeding over the right side of her face. She was sent to the Emergency Department immediately; and brain CT showed a mild subarachnoid hemorrhage. She was discharged after being observed for three days without any sequelae. |
| Two additional serious falls occurred in January and March 2008, respectively. The second patient was a 69 year-old man recovering from cerebellar hemorrhage. He fell when transferring from the para-bars to a wheelchair, suffered a subdural hemorrhage, and was hospitalized for an operation. Unfortunately, after the surgery, the patient had re-bleeding and underwent a second operation. After being hospitalized for a 2-month reconditioning program, the patient gradually recovered to the pre-fall condition and was discharged from the hospital. The third patient was a 5-year-old girl with traumatic brain injury. She fell in the restroom of the rehabilitation clinic; at that time, her mother had come out of the restroom and was having a conversation with others. The patient’s face was scraped and bleeding, and she received stitches. |
| RCA meeting |
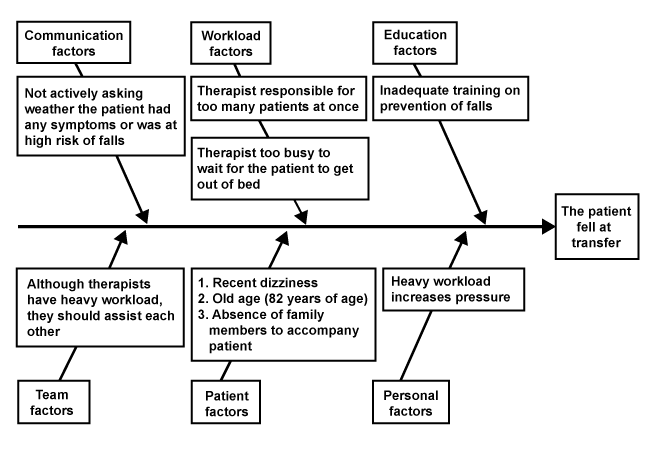
| After these 3 falls occurred, all physicians and therapists in the department of physical medicine and rehabilitation met to explore the reasons for falls. A Causal Tree was adopted to clarify the possible reasons that may result in falls in the first case (Figure 1). The relevant personal factors for the patient included old age, presence of multiple comorbidities, occasional dizziness noted recently, and absence of accompanying relatives during the rehabilitation visit. The relevant factors for the medical team included (1) An excessively heavy workload resulting in a single therapist responsible for multiple patients at the same time. (2) Insufficient support and assistance among the treatment team to allow staff to mutually take care of each other’s patients. (3) Factors related to training included inadequate health education training related to prevention of falls within the hospital. (4) Poor communication: medical personnel did not proactively ask patients about their symptoms. (5) Patients were not evaluated to determine whether they were at high risk of falling. |
| Reactive barriers; for example, 2 barriers were established after the causal tree was displayed (Table 1). And several improvement measures were adopted in the meeting. First, notices regarding patient safety should be posted at every treatment area to encourage patients to actively inform medical staff if they have any special illnesses or need oxygen equipment, to inform patients the contraindications for electrotherapy, and to reinforce health education when patients are receiving rehabilitation treatment. The initial step for preventing falls included detailed assessment of fall risk factors in patients by physiatrists. Next, when the patient is arranging his/her schedule of treatment, the receptionist of the rehabilitation clinic should provide the patient with safety notices. Third, the therapist should assess the patients’ current situations every time before starting rehabilitation therapy according to the safety notice, to see whether they are currently able to receive rehabilitation treatment, and whether they are at high risk for falls. Fourth, volunteers should be asked to assist patients in the high-risk group when they change positions. Last, after rehabilitation treatment is finished, the therapist should assist highrisk patients in leaving the bed and changing their position onto the wheelchair. |
| After RCA meeting |
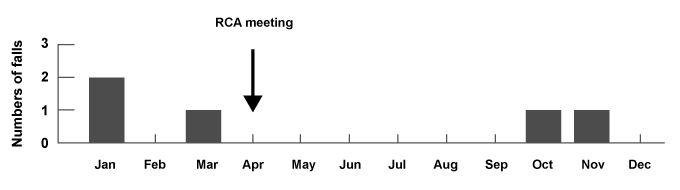
| The RCA meeting was convened after 3 falls occurred (Figure 2). The improvement measures drawn up in this meeting received support and cooperation from every staffs in the department. Adequate support has not been forthcoming for the volunteers, however, because of insufficient human resources. There was no more falls happened within 6 months after this meeting. |
| However, 2 falls occurred after the 6-month period. One case was an 85 year-old man suffering from a stroke and Parkinson disease. He tripped over the foreign caregiver’s heel in the hallway after finishing rehabilitation treatment without landing to the floor. No pain was complained, and physical examination by a physiatrist showed no evidence of sprain or strain. The other was a 60 year-old man with left thalamic hemorrhage. He had a fall when doing ambulation training in the para-bars and right buttock was landed on the ground during weight shifting. Mild ecchymosis over right buttock was noted and emergent radiographic examination of pelvis and right hip showed no evidence of fracture. Fortunately, the two patients were all assisted promptly, without any serious musculoskeletal or neurological injury. |
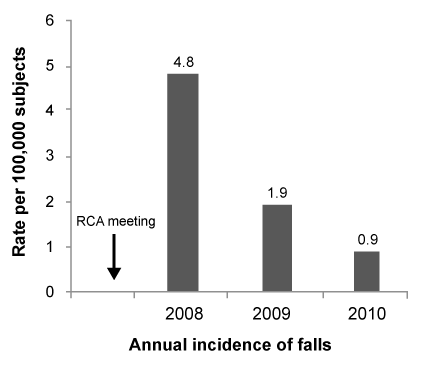
| There were total of 5, 2, and 1 falls in 2009, 2010, and 2011, respectively in department of physical medicine and rehabilitation in our hospital. There were three additional falls happened between 2009 and 2010 in patients with stroke; one happened during sit balance training on a chair, one occurred during treadmill training, and the other happened during standing up from a wheel chair. Fortunately, all of the three patients were assisted promptly without any complaint of pain, or evidence of neurological or musculoskeletal injury. The annual incidence of falls declined from 4.8 per 100,000 subjects in 2008 to 1.9 and 0.9, in the following 2 years (Figure 3). |
| Discussion |
| This was the first study applying RCA to explore the causes of patient falls and determined the implement procedures to prevent them in the department of physical medicine and rehabilitation in Taiwan. The present study showed that although the application of RCA in the setting of department of physical medicine and rehabilitation did not completely prevent falls, the incidence and complication of falls were reduced. |
| Medical errors can be divided into three types including sentinel event/misadventure, no-harm event, and near miss, of which the first type results in the greatest impact [13]. In the area of medication errors, RCA can not only analyze the factors causing clinical errors but also facilitate development of policies on medication errors, such as an online error-reporting system, to enhance the efficiency of reporting medication errors and improve the procedures for medicine usage [14-16]. |
| Risk factors for falls included older age, female, poor or retarded cognition, poor health and personal activity, lower level of independence in daily life, and the use of hypnotics or sedatives, etc. [17,18]. How to evaluate of fall risks became the first topic when focusing on fall prevention [18-23]. In clinics, many functional scales and checklists such as Berg Balance scale, Tinetti-test, gait and balance performance, hearing and visual condition, and history of osteoporosis or previous falls had been formed for the assessment of falls [19,24,25]. |
| Although there was absence of obstacles in the hospital, the incidence of falls may increase in hospital environment, especially among patient with old age or disabled who commonly seen in the rehabilitation clinic. Previous study conducted by RCA focused on inpatients with high risk of falls revealed 43% of reduction in fall rate [19]. In this study, we firstly applied RCA to analyze falls at the department of physical medicine and rehabilitation in a hospital setting. The reduction of annual incidences of falls in a 2-year period among the department of physical medicine and rehabilitation in our hospital were 60% in the first year and 81% in the second year after the RCA application. The incidence and complications of falls were reduced after the RCA. Compared with previous study, the higher rate of reduction of fall incidence in the present study might be attributed to the participants included inpatients and outpatients rather than inpatients only. However, the context and reasons for falls in a hospital environment and in the home or community setting could be different [2]. Further studies focuses on the analysis of the differences of falls between these two settings are warranted in the future. |
| It is well known that when performing RCA, personnel who have received training in RCA can more readily apply it to clinical problem solving. However, lack of time, followed by lack of resources, unwilling colleagues, lack of feedback and data, difficulty with teams, inter-professional differences, and unsupportive management have been shown to be the main causes of difficulty in conducting RCA [26]. Therefore, how to arrange and encourage medical staffs to receive comprehensive training in RCA is an important task. |
| The limitations of this study were (1) the reliability, validity, and cost-effectiveness of RCA applied to patient safety were not explored; (2) cultural effects (e.g., errors which are not serious may tend to be unreported due to fear of punishment, especially for Chinese); (3) no comparisons were made of the effectiveness of RCA with other methods, such as Failure Mode and Effects Analysis, which seek to detect, assess, and prevent errors that have not yet happened, or Seniors Falls Investigative Methodology, which was specific for falls among the elderly; and (4) the number and rate of falls listed was low. Our study did not involve more quantitative and statistic evaluation. In further research, extensive fall accidents may be collected. Not only those receiving rehabilitation treatment were included, but also fall accidents at home and inpatient setting. It will provide more power calculation and statistics. |
| Conclusions |
| RCA integrates the insights from every professional domain, facilitating a cooperative relationship among all the direct or indirect personnel who take care of patients including physicians, nurses, administrators, medical implementers, and administrative personnel. Through observation and analysis, the causes of incidents can be discovered and eliminated to prevent recurrence effectively. Meanwhile, patients and their family members are also taught to be alert for dangerous incidents. This is the first comprehensive study applying RCA to clinical rehabilitation treatments in Taiwan. The results have shown that, although the application of RCA was unable to completely prevent falls, the incidence of falls could be reduced. Many complications resulting from falls can also be reduced, and unnecessary medical expenses and burdens can be prevented. Therefore, it is worthwhile promoting application of RCA to clinical rehabilitation treatment to improve patient safety and enhance treatment quality in the future. |
References |
|
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 21902
- [From(publication date):
April-2013 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 17029
- PDF downloads : 4873
