Case Report Open Access
Use of X-box Kinect Gaming Console for Rehabilitation of an Individual with Traumatic Brain Injury: A Case Report
| Jessica M Paavola, Kory E Oliver and Ksenia I Ustinova* | |
| Department of Physical Therapy, Central Michigan University, Mt. Pleasant, MI, USA | |
| Corresponding Author : | Ksenia Ustinova Associate Professor, Doctoral Program in Physical Therapy Central Michigan University, Mt. Pleasant, MI 48858, USA Tel: (989)-774-2699 E-mail: ustin1k@cmich.edu |
| Received March 22, 2013; Accepted March 26, 2013; Published March 28, 2013 | |
| Citation: Paavola JM, Oliver KE, Ustinova KI (2013) Use of X-box Kinect Gaming Console for Rehabilitation of an Individual with Traumatic Brain Injury: A Case Report. J Nov Physiother 3:129. doi: 10.4172/2165-7025.1000129 | |
| Copyright: © 2013 Paavola JM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
The goal of the present experiment was to evaluate the feasibility of utilizing the Xbox Kinect gaming console for restoration of functional and motor abilities in a single representative patient with a history of traumatic brain injury (TBI). The patient was a 29 year old male with severe chronic functional and motor deficits secondary to brain injury that occurred 9 years prior to the study. The patient participated in ten sessions, three times a week for four consecutive weeks playing the Xbox Kinect games. These sessions consisted of playing five different games from Kinect Adventure series. The patient was evaluated with a battery of clinical tests before and after gaming practice. In addition to clinical assessments the patient’s movement performance was recorded with the Qualysis system for motion analysis. From kinematic data, the displacement and velocity of the trunk, dominant hand and foot were calculated and analyzed. After the gaming practice, the patient showed improvements in overall game performance, clinical outcomes, and movement performance characteristics throughout the various games. Results showed that the Xbox Kinect gaming console can be utilized with relative ease for recovery of severe functional, motor, and postural deficits even in a patient at chronic stage after TBI. Larger scale trials will the next viable step in validating the Xbox Kinect in its role of rehabilitation for TBI and other acquired brain injuries.
| Keywords |
| Xbox Kinect gaming console; Traumatic brain injury; Brain injuries |
| Introduction |
| Traumatic brain injury (TBI) is a contributing factor to a third (30.5%) of all injury related deaths in the United States [1]. Research has shown that on average approximately 1.7 million people sustain a traumatic brain injury annually, of these 52,000 die and 275,000 are hospitalized [1]. Survived after a TBI, people are facing a wide range of debilitating outcomes including both physical and mental factors. They require a number of rehabilitation procedures including cognitive, motor, communication, emotional or behavioral rehabilitation of varying intensity and duration of treatment [2]. As with all rehabilitation, the main goal is to help the people return to their prior level of function. |
| TBI rehabilitation requires the involvement of several disciplines and is best managed by a specialized team of health professionals [2], with early therapeutic initiation found to be very beneficial. Recent advances in TBI rehabilitation include task-specific training of cognitive deficits, constraint-induced movement therapy, visualspatial and visual scanning techniques, body weight-supported treadmill training for motor deficit and computer-aided cognitive remediation including use of virtual reality programs [3]. The use of virtual reality in rehabilitation for TBI patients’ is an emerging field. Traditional rehabilitation therapy may become tedious reducing motivation and adherence to the treatment program and thus provide a limited benefit to patients with a TBI [4]. For example, a study focusing on improving standing balance for patients with a TBI using an eBaViR (a system based on the Nintendo® Wii Balance Board) revealed that eBaViR represents a safe and effective alternative to traditional treatment to improve static balance in the TBI population [4]. Another expert report suggests that virtual reality has a great potential to design an individualized enriched practice environments that take advantage of the several principles of motor learning and neural plasticity that will optimize recovery after brain damage or injury [5]. In this regard, Xbox Kinect is the future of affordable virtual reality gaming consoles. It is a controller free camera system using infrared technology and operates through Smart technology features such as the wave of the hand, facial expressions, speech commands and the movement of the body. The software tracks multiple points of the body for as many as two players in real time. This new technology offers full body mobility and is the first 3D full-body video game system that reads the entire body’s movement and makes it part of the game [6]. |
| The main objective for this study was to determine the feasibility of utilizing the Xbox Kinect gaming console for rehabilitation of a single patient with a history of chronic functional and motor deficits following TBI. If Xbox Kinect is found to be effective, it could provide a way to encourage exercise and treatment compliance, allow safe and motivating therapy and could lead to the ability to provide exercises to clients in distant locations. |
| Case Description |
| History |
| The patient, involved in the study was a 29 year old male with severe sensorimotor deficits and functional disabilities secondary to traumatic brain injury that occurred 9 years prior to the study. Prior to injury the subject was a college student and was actively involved in sport activities. The injury occurred in a motor vehicle accident in which the subject was hit by a car while driving a motorcycle. Immediately following the accident in the emergency department, his condition was evaluated as a 3 per Glasgow coma scale [7] with questionable survivability. Medical examination revealed a skull fracture in the right petrous bone, CT of the head showed intracranial hematoma on the right as well as on the left medial and temporal lobe, with edema suggesting increasing intracranial pressure, also cortical contusions were identified. The patient was not responsive, and was intubated due to respiratory failure. An emergency craniotomy was performed with placement of intraventricular drains. Patient remained intubated and sedated in acute care for one week. The patient was then transferred to a rehabilitation unit to undergo a rehabilitation program including physical and occupational therapy, speech-language therapy, and psychological therapy. Since that time, patient has continued to receive traditional outpatient physical therapy treatment once or twice a year. The patient was not receiving any type of conventional physical therapy during the Xbox Kinect practice |
| Examination |
| Clinical assessment: At the time of case report the patient presented with severe static and dynamic balance and gait deficits, putting patient at increased risk for falls. Balance deficits were clinically demonstrated using the Berg Balance Scale (BBS) [8]. According to the BBS the patient received a score of 33 on two consecutive pre-test examinations. A score of <45 points on the BBS is indicative of significant risk for falls. The Functional Gait Assessment (FGA) was utilized to clinically quantify the subject’s gait deficits [9]. The patient received scores of 10 on FGA pre-test evaluations; this put him at significant risk for falls as a score of <25 is indicative of increased risk for falls. The patient also presented with severe coordination abnormalities affecting his ability to perform functional tasks. The Ataxia Score [10] was utilized to quantify the patient’s coordination deficits. According to the Ataxia Score the subject demonstrated moderate impairments by achieving a score of 26 on two consecutive pre-test evaluations. The Ataxia Score is scored on a scale with 0 demonstrating no impairment and the highest achievable score of 35 signifying most severe impairment. A complete listing of patient’s clinical assessment scores can be viewed in table 1. |
| Cognitive assessment: The patient presented with significant deficits in multiple areas of cognitive ability including his ability to perceptually coordinate fine motor functioning, and multiple visual perceptual deficits including visual memory, visual discrimination and spatial relations. Patient’s cognitive abilities were assessed before the practice with a battery of cognitive tests and revealed that he scored below average in all areas. Visual perception ability was evaluated with the Motor-Free Visual Perception Test (MVPT) [11]. This test measures visual discrimination, visual memory, visual spatial relations, and visual motor integration and is recognized by neuropsychologists as the most sensitive test to detect mild perceptual deficits. A score of 145 on the MVPT indicates the best possible score, and a score of 100 ± 15 points is indicative of average performance. The patient received an overall score of 64, which is indicative of significant visual perceptual deficits. The Rey-Osterreith Complex Figure (ROCF) test was used to assess visuo constructive abilities, by asking the participant to copy an abstract figure from a stimulus card onto a blank card [12]. On the scoring scale the patient can achieve a maximum score of 36 indicating higher quality. The subject received a score of 2 compared to the maximum possible score 36, that indicated severe deficits in visual-perceptual and visual-motor skills. The Visual Reproduction Test (VR1) was utilized to measure nonverbal visual memory [13]. The subject received a score of 1 of 19 best score possible, thereby demonstrating significant deficits in ability to utilize shortterm visual memory. |
| Intervention |
| Practice Content: The therapy consisted of a series of immersive games Kinect Adventure, designed for Xbox 360 Kinect console (Microsoft, Inc). The games were projected onto an 82-inch screen (1080p Mitsubishi DLP® TV bundle, Real D Beverly Hills, CA, USA, Figure 1). The gaming practice included 10 sessions, each approximately 50-55 minutes in duration, scheduled 3 times a week over 4 consecutive weeks. Each session consisted of playing three trials in a row of each of 5 games from the Kinect Adventure series. The game content and therapeutic goals are described in table 2. All games were played at the basic level. On initial trial day the patient was asked to complete one round of each game, as an introduction. Scores were documented as a baseline. During initial trial round verbal instruction and explanation of the game was given prior to starting, no cues were given following start of game. During the second session technical training was provided following the first round of trials for each game. This training included instruction on lateral weight shifting, side/forward/backward stepping, squatting and controlled upper extremity movements, which are components needed to be successful in each of the games. Following this session no further formal training was given besides occasional verbal cuing and reminders as needed. The patient was instructed to obtain as many points awarded as possible. To prevent a risk of falling, the patient was guarded throughout the entire gaming practice. A student physical therapist was standing behind (or near) the patient, while he was performing the games, and preventing him from losing balance as a result of excessive body shift. Prior to the practice, the patient gave informed consent to participate in this study, which was prepared in accordance with Declaration of Helsinki and approved by the institutional review board. |
| Data collection and analysis: The effect of practicing with Xbox Kinect on impairment and functional activity (ICF model, WHO) was evaluated by comparing clinical and movement performance outcomes before and after practice. Our patient was evaluated 4 times: 2 weeks before practice (PRE-TEST I), on the first practice day (PRETEST II); immediately after the practice (POST-TEST); and 2 weeks after the completion of training (RETENTION). During each of the evaluation sessions, a battery of clinical tests was administered as described in sub-section clinical assessment. |
| Movement performance assessment: In addition to clinical assessments, the patient’s movements were recorded during game performance with use of the Qualisys system for motion analysis (Qualisys AB, Gothenburg, Sweden). The system recorded motion of 30 reflective markers (at 100 Hz) placed on the patient’s major bony landmarks, when he performed games. From the data collected the displacement and velocity of the trunk, dominant hand and foot were calculated. The displacement was measured as peak to peak deviation of the body segment in 3D plane. Peak of velocity was a derivative from displacement data. Movement performance was analyzed during Day 1, Day 10, and 2 weeks after the completion of training that corresponded to PRE-TEST II, POST-TEST, and RETENTION evaluation sessions. Game performance success was also evaluated as a number of points awarded to the participant. |
| Statistical analysis was not used for comparing the PRE- and POST-TEST clinical and movement performance data. Scores from 4 assessments did not provide enough data points (5 is minimum) to run a serial dependency test, which is required prior to applying any type of statistical or semi-statistical methods for single case design studies [14]. T-scores are provided in the text for better visualization of the practice related outcomes. |
| Results |
| Game and movement performance |
| Despite the severe postural and coordination deficits, our patient managed to perform the rather complex gaming tasks well. He was guarded by a student physical therapy and felt secured. Some of the actions required for successful game performance were substituted with easier movements. For example, an initiation of the game Curvy Creek required a vertical jump. While not being able to jump, the patient performed a quick squat down, which started the game. In 2,000 Leaks game, some of leaks could be stopped by standing on one leg, and placing the other leg over a crack, located close to the floor level. Inability to stand on one leg was compensated by bending and plugging the crack with a hand. Thus, most of the gaming tasks were performed with relative ease. |
| As a result of a 10-day practice, our participant improved game performance throughout consecutive practice sessions. On 20,000 Leaks game patient was able to increase the number of points (M ± SD) received on the initial day from 34 points (only one trial of each game was performed during Day 1) to 88 ± 12 points on the last day with retention of 97 ± 7 points after a 2-week retention interval. On Curvy Creek patient was able to improve number of points from 36 points to 57 ± 9 points by the end of last day with retention of 78 ± 11 points following the 2-week retention interval. Collection of results for all five games completed can be found in table 3. |
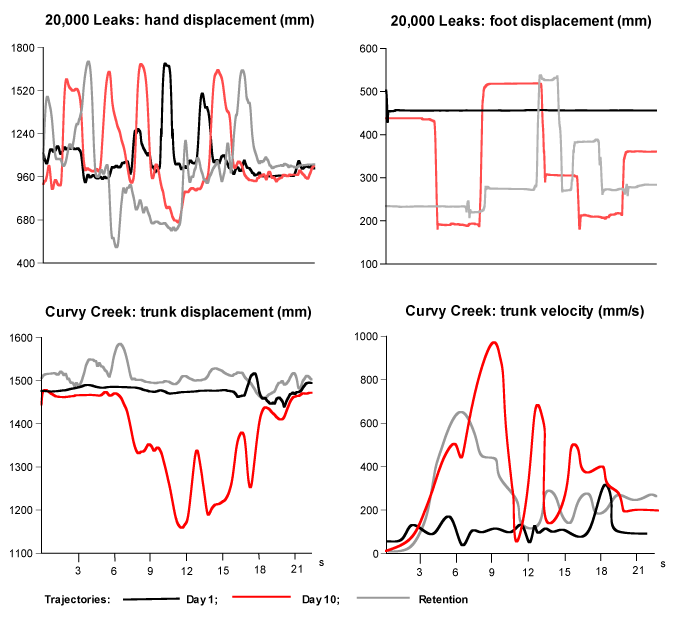
| The increased number of points through the end of the practice was proportional to improvements in his movement performance. Figure 2 shows displacements of the arm and foot during performance of the game 20,000 Leaks on the first day (black), last day (red) and retention (gray). An initial attempt to perform the gaming task was characterized by a minimal displacement of the lower extremity; the patient could not even take a step. By the end of the practice on the last day (gray), the magnitude of the hand and foot displacement became greater with a partial retention on the retention day. |
| The participant also increased the displacement and velocity of the trunk during performance of the game Curvy Creek, as illustrated in figure 2. The initial trial demonstrated minimal trunk displacement; during the last day patient was able to utilize trunk significantly more, which was required for game success through lateral weight shifting. Minimal retention of the trunk displacement was demonstrated on the retention day. Figure 2 also shows trunk velocity on first day (black), last day (red) and retention (gray). The initial attempts on Day 1 were characterized by decreased velocity when compared to the final trial on day 10. Patient began moving much faster to the end of gaming practice with partial retention on the retention trial. |
| Overall, in 20,000 Leaks game hand displacement improved from 800 mm to 943 ± 176 mm by the final session. Partial retention was maintained after a 2-week interval with 920 ± 115 mm. Foot displacement improved greatly from 30 mm at initial session to 486 ± 87 mm at final testing session. Partial retention was maintained following 2-week retention interval with a score of 450 ± 119 mm. No changes in hand velocity were observed in the same game from Day 1 to Day 10. An improved performance score in the Curvy Creek game coincided with improvement in trunk displacement and velocity. Trunk displacement improved from 360 mm at initial testing session to 620 ± 201 mm following final session. Further improvements were made following the 2-week retention interval with a result of 656 ± 184 mm. Velocity of trunk displacement increased from 412 mm/s to 1045 ± 456 mm/s following final testing session. Partial retention remained following 2-week retention interval with a result of 781 ± 312 mm/s. Parameters and improvements of movement characteristics for all five games tested can be found in table 4. |
| Clinical characteristics |
| Upon completion the gaming practice, our patient essentially improved clinical scores, as demonstrated in table 1. His scores on the POST-TEST evaluation exceeded the mean ± 2SD compared to the PRE-TEST evaluations. The BBS score improved by 4 points on the POST-TEST evaluation, and by 7 points on the RETENTION test from an initial PRE-TESTI and II average score of 32 ± 0.7. The FGA scores revealed a change in our patient’s results from 11 ± 0.7 points at PRE-TEST to 14 points at POST-TEST. Severity of ataxia was also slightly reduced by 2 points from to 26 ± 0 to 24 on the Ataxia Scale. It is important to mention that all these changes retained over a 2-week retention interval. |
| Discussion |
| The primary aim of this study was to determine the feasibility of utilizing the Xbox Kinect gaming console in the rehabilitation of a single patient with chronic post-injury functional and motor deficits. The information obtained in this study demonstrates that even patient with severe TBI-related abnormalities can benefit from the use of Xbox Kinect during a relatively short rehabilitative period. Results of this study showed that this gaming console can be utilized with relative ease to effectively improve game performance levels and both kinematic and clinical characteristics even at chronic stage. |
| The participant in this case not only showed improvements in most movement performance characteristics and overall points throughout the various games that may be attributed to a learning effect, but also improved clinical scores for a relatively short time period. Scores on the BBS and FGA tests increased on POST-TEST evaluation exceeding mean ± 2SD of the PRE-TEST evaluation. Although no statistical analysis was done for this single case design study, improvements in balance ability (BBS) by 4 and 7 points to the retention test can be considered as clinically important, because exceeds a minimal detectable change (MDC) established for this test. According to different sources, MDC can range from 2.5 points in patients with chronic stroke [15] to 5 points in patients with stroke, who had initial score within 35-44 points on the BBS [16]. The highest MDC of 3.83 points was established for patients with TBI [17], confirming clinical meaning of results, although not supported statistically. Results based on the FGA, with improvements of 4 points, were not enough to yield a clinically important change. According to Lin et al., MDC depends on patient diagnosis and results range from 4.2 point change in stroke population to 8 point change for vestibular disorders [18]. All these standards were established, however, for patients with stroke and vestibular disorders, while information about MDC on these scales after traumatic brain injury is limited. |
| Several movement performance characteristics remained unchanged over the practice period. This mainly concerned hand velocity in the game 2,000 and trunk velocity in the Space Pop game. The lack of changes on these characteristics cannot be considered as performance decline, because the overall game performance was improved. Most likely that slow speed was compensated by increased precision and optimization of movement strategy allowing for reaching maximum success with minimum effort. |
| Overall, a positive effect of practicing with Xbox Kinect was anticipated and may be related to several key features of immersive virtual reality (VR). As was highlighted by several authors, virtual reality allows practice in a realistic, safe, and motivating environment. While utilizing movements similar to those made in the equivalent physical world [19], VR tasks can incorporate elements essential for the successful restoration of motor abilities. These include the manipulation of timing and precision of environmental interactions, something not easily achieved in the real world [20], real-time performance feedback [21,22] and motivation which is reinforced by the competitive nature of VR games and the adjustment of difficulty to offer a level of success [23]. For example, performance of real-world tasks in a regular therapeutic setting is limited by the client’s ability, and frustration and lack of success in these activities can demotivate the patient from practicing [24,25]. In contrast, game-based therapy offers a variety of scenarios in which mistakes do not pose any risk to the participant (e.g. skateboarding, hitting an obstacle) and criteria for performance success can be scaled according to the individual’s ability. Reinforcement of success encouraged participants and increased compliance as result. |
| Results of our single-case study provided another evidence of successful use of virtual game application for rehabilitation of individual with acquired brain injury. Xbox Kinect gaming console together with Kinect Adventure game series have been shown to be both economical and feasible. The gaming console is a commercially available and relatively inexpensive option for virtual reality based rehabilitation. The patient in our study was able to navigate the system successfully following 3 to 4 practice sessions, regardless of his cognitive ability or lack of experience with the system. At this time more research is needed to assess the usability of the Xbox Kinect gaming system in the clinical setting and in different patient populations. |
| Limitations of the Study |
| Although the Xbox Kinect gaming practice is a promising tool, a single case study is insufficient to draw conclusions as to its overall effect in the entire TBI patient population. This intervention might not be suitable for all individuals because of some drawbacks associated with practice in virtual environment. Unfortunate technology gap can pose significant challenge for some patients with brain injury. Not all of them are able to navigate easily through the Kinect interface menu [26]. Playing the virtual games may cause cyber-sickness in patient with brain injury as well. Another serious limitation of the present study is a lack of information on the transfer of motor skills learned during the game performance to real-world behavior. Changes in performance of activities of daily living were not assessed in our patient. This question is worth of further investigation. |
References |
|
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
Figures at a glance
 |
 |
| Figure 1 | Figure 2 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 17335
- [From(publication date):
February-2013 - Aug 15, 2025] - Breakdown by view type
- HTML page views : 12603
- PDF downloads : 4732
