Case Report Open Access
Resolution of Hepatic Hydatid Cyst with Biliary Communication with ERCP
Sanjay Kumar Somani* and Amit Prakash SrivastavaConsultant Gastroenterologist, Sahara Hospital, Gomti Nagar, Lucknow, 226010, UP, India
- *Corresponding Author:
- Dr. Sanjay Kumar Somani, MD, DM
Consultant Gastroenterologist 76
Chandganj Garden, Aliganj
Lucknow-226024, India
Tel: 91 979215 5555
Fax: 91 522 6782110
E-mail: sanjayksomani@rediffmail.com
Received date: February 05, 2012; Accepted date: June 25, 2012; Published date: June 27, 2012
Citation: Somani SK, Srivastava AP (2012) Resolution of hepatic hydatid cyst with biliary communication with ERCP. J Gastroint Dig Syst 2:114. doi: 10.4172/2161-069X.1000114
Copyright: © 2012 Somani SK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Background: Hydatid cyst of the liver may be complicated by spontaneous rupture into the biliary tract with biliary obstruction.
Methods: ERCP of hydatid cyst liver with biliary communication was done and bile duct cleared and cyst was assessed for resolution.
Results: A 56 year lady who had jaundice, right upper abdomen pain and cholangitis was diagnosed to have hydatid cyst of liver with biliary obstruction and membranes in common bile duct. ERCP was performed and bile duct membranes were extracted and duct was cleared. Her jaundice, fever and abdominal pain resolved and the repeat CT scan abdomen also showed resolution of the liver hydatid cyst.
Conclusion: Hepatic hydatid cyst with biliary communication may drain off and resolve completely after ERCP clearance of bile duct.
Keywords
Hydatid cyst liver; Biliary communication; ERCP
Introduction
Liver is the most common site of hydatid cyst formation. Hydatid cysts of the liver exert pressure on the surrounding parenchyma, and in approximately one-fourth of the cases, due to higher pressure in the cyst, the cysts eventually leak into small bile ducts or perforate into large ones [1]. The most common complication of hydatid cyst of the liver is spontaneous rupture into the biliary tract with biliary obstruction being reported to occur in 5% to 17% of cases [1]. Intrabiliary rupture occurs into the right duct in 55-60% of cases, into the left duct in 25- 30% and rarely into the confluence or gall bladder [2]. We present a case of a hydatid cyst of the liver which ruptured spontaneously into the common hepatic duct resulting in jaundice and cholangitis which resolved following endoscopic papillotomy and endoscopic clearance of the membranes from the common bile duct.
Case Report
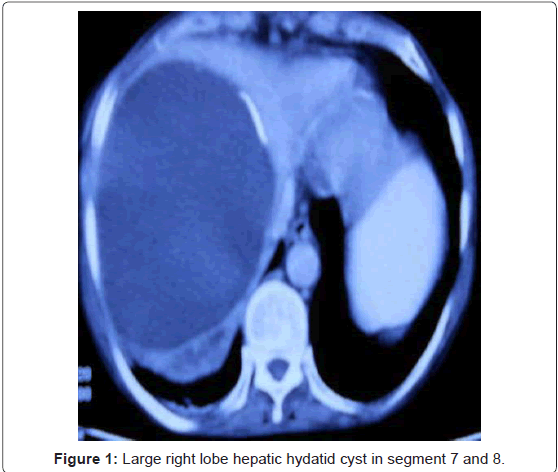
A fifty six year old female patient presented with history of highgrade fever and right hypochondrial pain of two week duration. The patient was icteric, febrile and had a tender hepatomegaly. Investigations showed a deranged liver function test (LFT) with a total bilirubin of 11.0 mg/dl (direct of 7.5 mg/dl) and raised serum alkaline phosphatase (436 U/L). CT scan revealed a moderate hepatomegaly with large well defined cystic SOL in the right liver lobe (segment 7 and 8) with dilated intrahepatic biliary radicals and common bile duct (Figure 1).
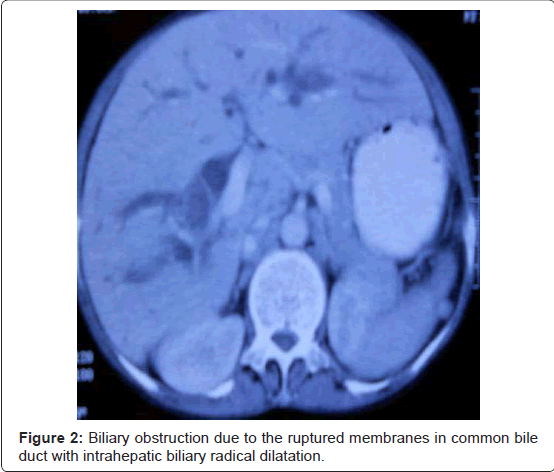
The cyst was seen to communicate inferiorly with common hepatic duct in the region of ductal confluence with extension of the hydatid membranes into common hepatic duct (CHD) and proximal CBD with upstream dilatation of the right and left hepatic ducts and intra-hepatic biliary radicles (Figure 2).
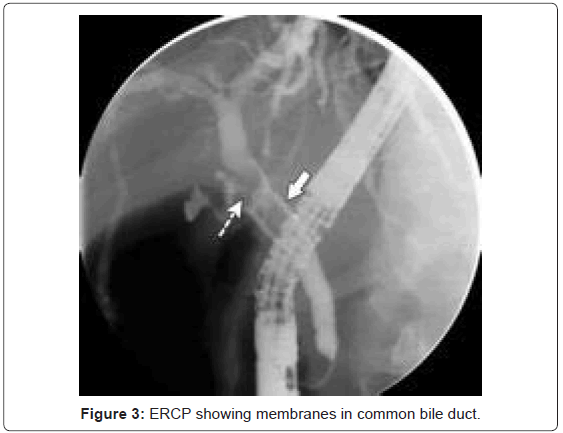
Hydatid Serology was positive. The patient underwent endoscopic retrograde cholangiography (ERCP). During the procedure membranes were seen to be coming out of papilla of Vater. Cholangiogram showed multiple filling defects in CBD (Figure 3).
An endoscopic papillotomy was performed and a large amount of the membranes were removed from the CBD. On repeated balloon sweep large amount of pus also drained. The procedure was completed with CBD stenting. Patient was clinically monitored and TLC and LFT were performed to see for improvement. On repeat ERCP after seven days no more membranes were removed from the CBD. Only clear bile was draining. A completion ERCP established a complete clearance of the CBD. The biliary stent was removed. Antibiotics (Ceftriaxone 1 g IV twice daily) based on blood culture (growth of E Coli) were continued for a total of seven days for cholangitis and patient was also given Albendazole 400 mf BID for eight weeks.
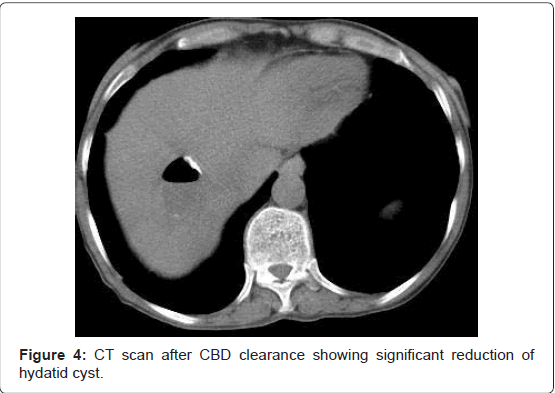
The patient recovered subsequently with decrease in jaundice, fall of total serum bilirubin to 1.2 mg/dl and decrease in size of cavity on CT scan (Figure 4). The patient remained asymptomatic during six months of follow up.
Discussion
Hepatic hydatid disease (HHD) is a major endemic problem in sheep-rearing regions of the world [3]. The liver acts as a filter for hydatid larvae, making it the most commonly affected organ [3]. The liver is involved in 50% to 70% of patients with hydatid disease [1]. Symptoms arise either when the cyst has grown enough to cause pressure on adjacent organs or when a complication occurs [4]. Rupture, secondary infection, and suppuration are the most common complications. Up to one-third of patients with HHD present with complications such as rupture (into the biliary tree, thorax or peritoneum), secondary infection, anaphylactic shock, sepsis and liver replacement, [2] cysts of the liver exert pressure on the surrounding parenchyma, and in most cases the cysts eventually rupture into the biliary tree in 1% to 25% of cases although an incidence of 64.75% has been reported from a multicentric study in Tunisia [5]. It occurs in two forms: an occult rupture, resulting from small tears between the cyst wall and small biliary radicles, seen in 10% to 37% of the patients, or a frank rupture, involving large bile ducts, seen in 3% to 17% of the patients [6].
Obstructive jaundice occurs when cyst elements empty into the biliary tree [1]. Rupture is most likely to occur in centrally located cyst with a high intracystic pressure up to 80 cm H2O [2]. According to Lewall and McCorkell the cyst rupture can occur in three clinical forms: contained, communicating and direct [7]. Contained rupture occurs when the cyst contents are confined within the pericyst. Communicating rupture defines tearing of the pericyst and evacuation of cyst contents into the biliary tract or bronchioles. Direct rupture describes complete tear of the cyst wall and spillage of the cyst contents into the peritoneal or pleural cavity. Although biliary obstruction is reported to occur in only 5% to 17% of cases [1], obstructive jaundice occurs in 57% to 100% of cases following intrabiliary rupture, especially when the rupture occurs into the large bile ducts thus emptying the contents into the biliary tract [3]. It has been reported that if the cystobiliary opening is larger than 5 mm, cystic content migration into the biliary tract would occur in 65% of the cases [8]. Other presentations are right upper abdominal pain (82%), fever (70-90%), acute cholangitis (20-37%), abdominal lump (22-39%), and rarely with acute pancreatitis, liver abscess or septicaemia; or in 5% to 6% it may be asymptomatic [2].
Early diagnosis and proper management are mandatory in these patients, since serious clinical complications with an increased mortality may ensue [7]. The reported morbidity and mortality rates of all patients in literature are 19.44-43.03% and 1.8- 4.5% respectively [5]. The most common causes of deaths were sepsis and hepatic failure [5]. Ultrasound is the most commonly employed initial investigation [3]. Gharbi et al. [9] have described five types of echinococcal cysts on USG: purely cystic except for hydatid sand; detached membrane; multiseptated; peripheral or diffuse distribution of coarse echoes in a complex heterogeneous mass; and calcified wall. These five types are believed to correspond to evolutionary stages of the hydatid cyst.
Computed tomography and magnetic resonance imaging are useful in diagnosing biliary hydatid disease resulting from rupture of a liver hydatid cyst; MRI is a useful tool in difficult cases such as intrabiliary rupture, where CT and ultrasound are not conclusive [2]. However, ERCP and, more recently, MRCP, are confirmatory for intrabiliary rupture of the hepatic hydatid cyst. In addition ERCP may be of therapeutic benefit in selected cases [2].
The classic treatment for hydatidosis with rupture into the biliary tract has been surgery [5,10]. However, persistent postoperative external bile drainage is a serious complication, occurring in 3.8% to 27.5% of cases, that often necessitates reoperation [11,12]. Other complications include infection within the residual cavity and sinus formation; recurrence or dissemination can also occur [1]. However, since al-Karawi et al. [13] reported the use of ERCP with endoscopic sphincterotomy and extraction of retained echinococcal daughter cysts from the common bile duct, endoscopic sphincterotomy with extraction of the cysts from the CBD has emerged as a safe and an effective alternative treatment for patients with intrabiliary rupture of hepatic hydatid cysts [1,13-17]. It has been suggested that two to three courses of mebendazole may play an important role in prophylaxis after surgery or endoscopic evacuation of a ruptured cyst into the biliary tree [1]. Percutaneous approach with PAIR (Percutaneous aspiration instillation and reaspiration) should not be performed in patients with cyst-biliary communication.
References
- Akkiz H, Akinoglu A, Colakoglu S, Demiryürek H, Yagmur O (1996) Endoscopic management of biliary hydatid disease. Can J Surg 39:287-292.
- Kumar R, Reddy SN, Thulkar S (2002) Intrabiliary rupture of hydatid cyst: diagnosis with MRI and hepatobiliary isotope study. Br J Radiol 75: 271-274.
- Ahuja SR, Karande S, Koteyar SR, Kulkarni MV (2001) Hepatic hydatid cyst rupturing into subdiaphragmatic space and pericardial cavity. J Postgrad Med 47: 37-39.
- Mottaghian H, Saidi F (1978) Postoperative recurrence of hydatid disease. Br J Surg 65: 237-242.
- Erzurumlu K, Dervisoglu A, Polat C, Senyurek G, Yetim I, et al. (2005) Intrabiliary rupture: An algorithm in the treatment of controversial complication of hepatic hydatidosis. World J Gastroenterol 11: 2472-2476.
- Becker K, Frieling T, Saleh A, Häussinger D (1997) Resolution of hydatid liver cyst by spontaneous rupture into the biliary tract. J Hepatol 26: 1408-1412.
- Lewall DB, McCorkell SJ (1986) Rupture of echinococcal cysts: diagnosis, classification, and clinical implications. AJR Am J Roentgenol 146: 391- 394.
- Zaouche A, Haouet K, Jouini M, El Hachaichi A, Dziri C (2001) Management of liver hydatid cysts with a large biliocystic fistula: multicenter retrospective study. Tunisian Surgical Association. World J Surg 25: 28- 39.
- Gharbi HA, Hassine W, Brauner MW, Dupuch K (1981) Ultrasound examination of the hydatid liver. Radiology 139: 459-463.
- al-Akayleh A (2000) Frank intrabiliary rupture of hydatid hepatic cyst: diagnosis and treatment. East Mediterr Health J 6: 522-555.
- Rodriguez AN, Sánchez del Río AL, Alguacil LV, De Dios Vega JF, Fugarolas GM (1998) Effectiveness of endoscopic sphincterotomy in complicated hepatic hydatid disease. Gastrointest Endosc 48: 593-597.
- Agarwal S, Sikora SS, Kumar A, Saxena R, Kapoor VK (2005) Bile leaks following surgery for hepatic hydatid disease. Indian J Gastroenterol 24: 55-58.
- Al Karawi MA, Mohamed AR, Yasawy I, Haleem A (1987) Non-surgical endoscopic transpapillary treatment of ruptured echinococcus liver cyst obstructing the biliary tree. Endoscopy 19: 81-83.
- Shemesh E, Klein E, Abramowich D, Pines A (1986) Common bile duct obstruction caused by hydatid daughter cysts -- management by endoscopic retrograde sphincterotomy. Am J Gastroenterol 81: 280-282.
- al Karawi MA, el-Shiekh Mohamed AR, Yasawy MI (1990) Advances in diagnosis and management of hydatid disease. Hepatogastroenterology 37: 327- 331.
- al Karawi MA, Yasawy MI, Shiekh Mohamed AR (1991) Endoscopic management of biliary hydatid disease: report on six cases. Endoscopy 23: 278-281.
- Becker K, Frieling T, Saleh A, Häussinger D (1997) Resolution of hydatid liver cyst by spontaneous rupture into the biliary tract. J Hepatol 26: 1408-1412.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 16006
- [From(publication date):
August-2012 - Dec 24, 2025] - Breakdown by view type
- HTML page views : 11165
- PDF downloads : 4841