Deep Presentation of a Tufted Angioma in an Adult
Received: 29-Mar-2012 / Accepted Date: 02-May-2012 / Published Date: 07-May-2012 DOI: 10.4172/2161-119X.1000112
251223Introduction
Tufted angioma is a rare vascular tumor most commonly localized to the skin and subcutaneous tissues and characterized by slow angiomatous proliferation. Although adult-onset cases, with subcutaneous manifestations but not the deep presentation, have been fewly described, tufted angiomas occur far more frequently in children. These tumors have a benign course, with no reported cases of aggressive behavior or metastases. In our case report tufted angioma was a deep mass in an adult. This manifestation was never mentioned in the literature till now.
Case Report
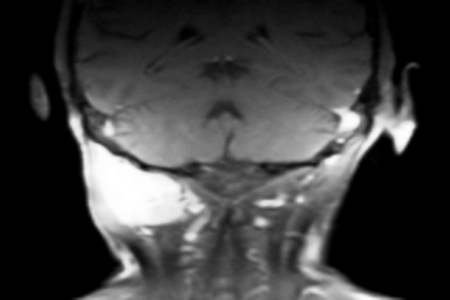
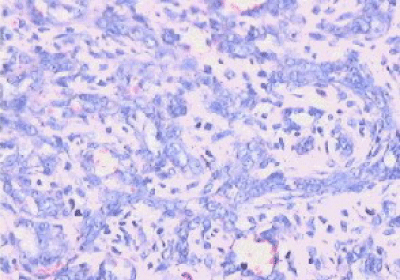
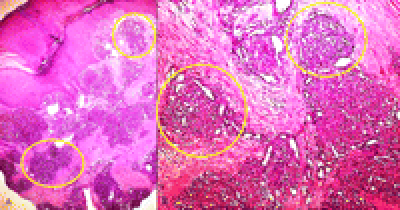
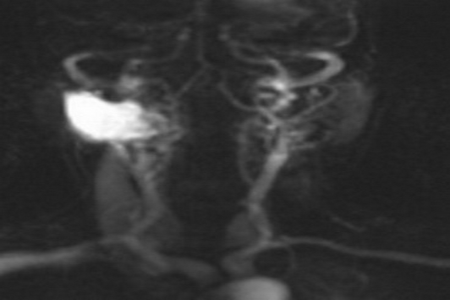
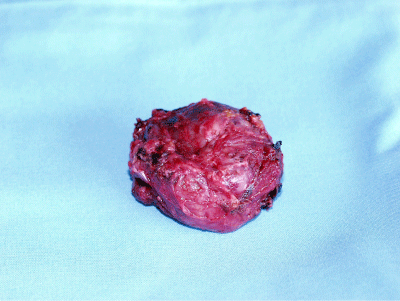
68 year-old lady presented to our outpatient department complaining of a hard retro-auricular swelling on the right side of the neck for six weeks with subjective size change. No other complains. She was known with bilateral hearing loss and hearing aids. On examination, a deep retroauricular swelling on the right side of the neck was noted, no tenderness on palpation, and no skin changes. The rest of examination was not related. Radiologically, the MRI of the head and neck showed well defined oval space occupying lesion with sharp contour, and lying between the dorsal spinal process and the transverse spinal process at the level of the right 1st and 2nd vertebrae (Figure 1). No lymphadenopathy. Core needle biopsy showed haemngioendothelioma (Figure 2). The immunohistochemical examination showed capillary haemangioma (Tufted Angioma, Angioblastoma of Nakagawa) (Figure 3). The lesion was embolised preoperatively, as the lesion was arterially hyperperfused (Figure 4) and it was removed surgically with the neurosurgery team as the lesion was located nuchal-sub-occipital (Figure 5). The postoperative hospital stay was without complications. In our OPD follow-up, the patient was with no complains and U/S of the neck showed no sign of recurrence. MRI skull 1 year postoperatively showed no signs of recurrence.
Discussion
Solitary tufted angioma also known angioblastoma, is a rare, benign vascular tumour. The actual number of cases has been difficult to quantify since it has been mentioned under several names in the literature [1]. This entity was first described by Nakagawa in 1949 as angioblastoma, and since that time more than 200 cases have been reported, mainly in the Japanese literature [2]. Macmillian and Champion [3] described a similar vascular proliferation, but under the name progressive capillary hemangioma in 1971. In 1976 while discussing the differential diagnosis of a well differentiated angiosarcoma, Jones [4] was the first to use the term tufted angioma when he briefly mentioned a similar tumor. In Jones and Orkin [5] separated it from all the variants of lobular capillary haemangioma. Solitary tufted angioma is a rare, recurring, slowly growing vascular tumour with a variable clinical morphology that can present as red to purple and more rarely bluish papules or plaques. The lesions range from to 5 cm in size but may be larger [6]. Hypertrichosis can also be seen in association with tufted angioma [6,7]. The lesions may persist for years and can regress spontaneously. Localised hyperhidrosis was present in some of the case [8]. Most of the lesions are asymptomatic but may present with tenderness or even pain. Tenderness, hypertrichosis, and induration can be useful in differentiating tufted angioma from common haemangioma [6]. The lesions can be found anywhere, but are mainly seen on the neck, trunk, and occasionally on the extremities. Although this condition is entirely benign, extensive involvement is common and this can result in a disfiguring clinical appearance No malignant transformations have been reported to date. Only in a few cases, however spontaneous partial or complete regression has been reported [9]. Generally, the lesion is described as solitary. However, multifocal presentations are reported. These lesions are always localized to the skin and rarely involve the subcutaneous tissues, which is not the situation in our case report. Occasionally, tufted angiomas may be associated with more serious disease for example Kasabach-Merritt Syndrome [10]. Most series report that 60-70% of tufted angiomas develop before the age of years, and 25% of tumors appear by the time the patient is aged 1 year. The Japanese-language literature, however, reports that more than 50% of tufted angiomas appear in the patient's first year of life. Of these patients, 15% are believed to have had a blemish in the area where the tufted angioma later developed; this observation suggests a congenital mode of presentation fewer than % of tufted angiomas develop in individuals older than 50 years [5,11]. One 81-year-old patient with a tufted angioma of 2 years' duration is reported in the French-language literature, and a case has been described in an 84-year-old man in Japan [12]. The pathogenesis of tufted angioma is unknown. It is probably neoplastic. Secretion of growth factors such as Iterleukin (IL)-8,known to affect angiogenesis, is thought to be involved, prompting the development of numerous tufts of vessels [13]. Trauma does not appear to be a predisposing factor, although a report describes the appearance of a lesion of tufted angioma at the site of a previous arthropod bite. Histo-pathologic examination is the gold-standard investigation to confirm the diagnosis of Tufted angioma and to exclude other vascular malformation and vascular tumors. The distinction from malignant vascular tumors is important. Despite progressive enlargement, tufted angiomas have a benign histologic appearance. The feature specific for a tufted angioma is the "cannonball" distribution of distinct cellular tufts of capillaries and endothelial cells [5,14]. Treatment guidelines for tufted angioma have yet to be established. In general, treatment may be divided into that given for cosmetic reasons and that instituted because of complications or anticipated complications, such as Kasabach-Merritt syndrome, obstruction of vital structures such as airway or visual axis, or functional compromise. Most of the authors agree that this group of patients should be aggressively treated with systemic steroids or interferon (IFN)-b. There have only been two case reports in the English literature of successful use of oral corticosteroids. The topical and intralesional corticosteroids have been tried without a reduction in size [14]. Subcutaneous daily injections of IFN-b may be used if lesion is not responding to systemic corticosteroids with a variable success rate [15]. In lesions particularly those in vital areas, such as our case report, surgical excision is the treatment of choice. However, in the series by Jones [5], three of five lesions recurred after surgical excision. Pulsed Dye Laser (PDL) has been tried with varying success. A case has been cited where PDL laser was unsuccessful after several attempts, but argon tunable-dye laser lightened and induced resolution in adult [16]. Cryotherapy and radiotherapy have been tried with little success and are not recommended [5]. As tufted angioma is benign and stabilizes in size after a period of time, even regressing spontaneously in minority of patients, "active non intervention" is reasonable in uncomplicated cases, and may be all that necessary. However, long-term follow-up in these patients would be important.
References
- Tsang WY, Chan JK, Fletcher CD (1991) Recently characterized vascular tumors of skin and soft tissues. Histopathology 19: 489-501.
- Okada E, Tamura A, Ishikawa O, Miyachi Y (2000) Tufted angioma (angioblastoma): case report and review of 41 cases in Japanese literature. Clin Exp Dermatol 25: 627-630.
- Macmillan A, Champion RH (1971) Progressive capillary hemangioma. Br J Dermatol 85: 492-493.
- Jones EW (1976) Dowling oration 1976. Malignant vascular tumours. Clin Exp Dermatol 1: 287-312.
- Jones EW, Orkin M (1989) Tufted angioma (angioblastoma). A benign progressive angioma, not to be confused with Kaposi's sarcoma or low-grade angiosarcoma. J Am Acad Dermatol 20: 214-225.
- Wong SN, Tay YK (2002) Tufted angioma: a report of five cases. Pediatr Dermatol 19: 388-393.
- Herron MD, Coffin CM, Vanderhooft SL (2002) Tufted angiomas: variability of the clinical morphology. Pediatr Dermatol 19: 394-401.
- Chu KH, Kim SH, Park KC, Lee AY, Song KY, et al. (1991) Angioblastoma (Nakagawa)--is it the same as tufted angioma? Clin Exp Dermatol 16: 110-113.
- Murano S, Fujita Y (1985) Angioblastoma (Nakagawa). The spontaneous regression and the course of sweat abnormality. Rinsho Derma 39: 509-512.
- Leaute-Labreze C, Bioulac-Sage P, Labbe L, Meraud JP, Taieb A (1997) Tufted angioma associated with platelet trapping syndrome: response to aspirin. Arch Dermatol 133: 1077-1079.
- Ban M, Kamiya H, Kitajima Y (2000) Tufted angioma of adult onset, revealing abundant eccrine glands and central regression. Dermatology 201: 68-70.
- Murakami M, Nitta Y, Ikeya T, Hara K (1997) Two cases of angioblastoma (Nakagawa): A one-month baby and an 84-year-old man (in Japanese). Rinsho Derma (Tokyo) 39: 925-929.
- Bernstein EF, Kantor G, Howe N, Savit RM, Koblenzer PJ, et al. (1994) Tufted angioma of the thigh. J Am Acad Dematol 31: 307-311.
- Francis JS, Benjamin DR (1997) Indurated purple-red plaque. Pediatr Dermatol 14: 53-55.
- Robenzadeh A, Don PC, Weinberg JM (1998) Treatment of tufted angioma with interferon-alfa: role of bFGF. Pediatr Dermatol 15: 482.
- Suarez SM, Pensler JM, Paller AS (1995) Response of deep tufted angioma to interferon alfa. J Am Acad Dermatol 33: 124-126.
Citation: Al-Sihan M (2012) Deep Presentation of a Tufted Angioma in an Adult. Otolaryngology 2:112. DOI: 10.4172/2161-119X.1000112
Copyright: © 2012 Al-Sihan M. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15050
- [From(publication date): 6-2012 - Dec 22, 2025]
- Breakdown by view type
- HTML page views: 10405
- PDF downloads: 4645