Exploring the Limits of the Endoscopic Approach to Frontal Sinus Osteoma
Received: 09-Aug-2013 / Accepted Date: 21-Aug-2013 / Published Date: 28-Aug-2013 DOI: 10.4172/2161-119X.1000140
Abstract
Objective: We present the case of a frontal sinus osteoma in a 71-year-old Japanese woman who presented with an approximately 2-year history of head dullness.
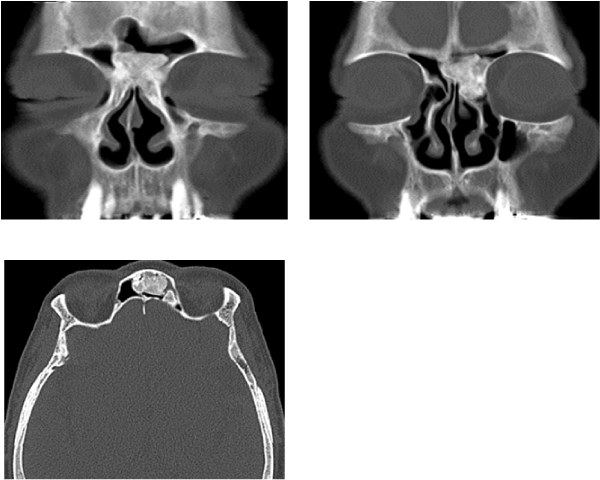
Case report: CT showed a 45×39 mm radio dense mass extending from the left to the right frontal sinus. Under general anesthesia the mass was removed by endoscopic surgery. Although the tumor was large and extended into both frontal sinuses, the tumor was completely removed, without CSF leakage or orbital complications, by using a modified Lothrop procedure.
Conclusion: A unique osteoma of the frontal sinus is described. The challenges related to surgical treatment of this particular case and similar lesions are addressed.
Keywords: Frontal sinus, Osteoma, Endoscopic approach, Modified Lothrop procedure
254023Introduction
Frontal sinus osteomas are mostly asymptomatic and slow-growing benign tumors most frequently involving the frontal sinus [1]. The surgical procedures available for osteoma removal can be classified into external, endoscopic, or a combination of both [2]. The external approach is often selected to ensure complete and safe removal of frontal sinus osteoma located close to both orbits [3]. Here, we present the case of a symptomatic frontal sinus osteoma that was successfully removed by using an Endoscopic Modified Lothrop Procedure (EMLP).
Case Report
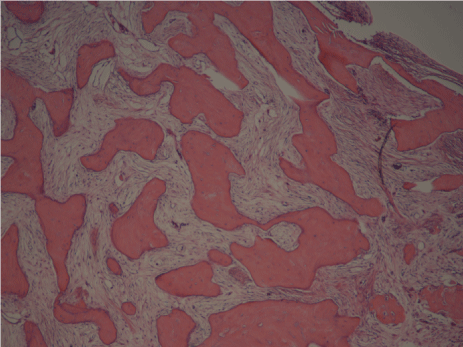
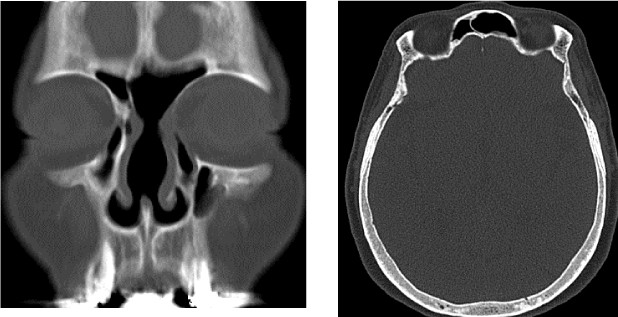
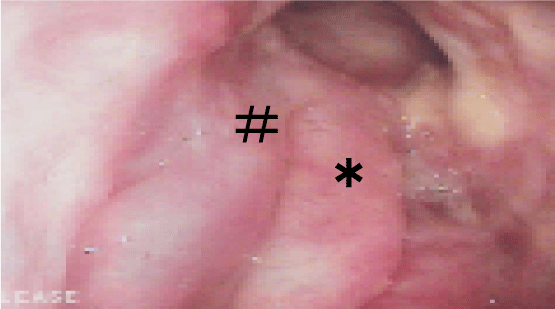
A 71-year-old Japanese woman was referred to our otolaryngology department with a chief complaint of head dullness for about 2 years. X-ray of the paranasal sinuses at the time revealed left-sided frontal sinus osteoma. The patient was followed up in the ENT department regularly. At the next paranasal X-ray, 6 months after the initial visit, there were radiological changes in the size and shape of the osteoma. Computed tomography revealed a 45×39 mm radio dense mass extending from the left to the right frontal sinus (Figure 1). The mass was removed by endoscopic surgery under general anesthesia. Although the tumor was large and extended into both frontal sinuses, it was removed completely, without CSF leakage and orbital complications, by using EMLP. Magnetic-resonance-imaging integrated neuronavigation was used intraoperatively to facilitate orientation during endoscopy. Multi-angled high-speed intranasal drills and shavers (Medtronic) were used to remove the tumor. The endoscopic drill technique was used to resect the margin of the osteoma, starting at the periphery and moving to the center, which was at risk of fragmentation; the tumor was removed transnasally without damage to the surrounding tissues. The time for operation was 4 and half hours. Histological examination confirmed the diagnosis of osteoid osteoma, since the typical nidus was found in the histological specimen (Figure 2). The patient did well postoperatively, and no recurrence was noticed at a 12-month followup. (Figures 3 and 4).
Discussion
The frontal sinus is one of the commonest sites of occurrence of paranasal sinus osteoma. Small, favorably located asymptomatic osteomas can be managed conservatively [1-3]. Osteomas that in the past have required open approaches can now be managed successfully with the endoscopic approach alone or with combined approaches, thus reducing overall morbidity without sacrificing outcome [1-3]. If surgery requires substantial widening of the frontal recess, then the EMLP on its own or combined with an osteoplastic flap should be considered [4-6]. There appears to be a consensus that small, asymptomatic osteomas do not need surgery and a “wait and see” policy can be chosen [1-6]. Indications for surgery are 1) rapid growth of the tumor, 2) the presence of symptoms, 3) chronic rhinosinusitis due to obstruction by the tumor, 4) tumor-related bone erosion or facial deformity, 5) tumor occupying more than 50% of the frontal sinus, 6) tumor causing partial or complete blockage of the frontal recess and 7) the presence of complications [4-6].
The surgical approaches available for osteoma removal are classified into external, endoscopic, or a combination of both [1-3]. Endoscopic frontal sinus procedures can be classified as Draf IIA frontal sinusotomy (removal of all ethmoid cells obstructing frontal sinus drainage, with resection of the floor of the frontal sinus between the lamina papyracea and the middle turbinate) and Draf IIB frontal sinusotomy (resection of the floor of the frontal sinus from the lamina papyracea and the nasal septum) [4-6]. Draf III (also called the EMLP) involves resection of the frontal sinus floor on sides, as well as the superior part of the adjacent nasal septum and the inferior part of the interfrontal septum, thus creating large frontal sinus drainage [4-6]. The time need for complete resection of tumor depends on the procedures and the pathlogical types of osteoma. It is also widely accepted that it takes more time to remove the osteoma transnasally than using osteoplastic flap procedure and spongious type of osteoma is easier to remove compared to ivory osteoma [4-6]. The transnasal approach is not usually indicated with the osteroma(s) located far lateral in the frontal sinus or widely attached to skull base [2-6].
Tumor characteristics, patient factors, availability of appropriate instrumentation, and technical expertise should be taken into account to determine the most appropriate surgical approach.
Conclusion
Appropriate imaging techniques are needed for preoperative diagnosis of frontal sinus osteoma. EMLP can be used successfully to resect frontal sinus osteoma extending completely into the left and right frontal sinuses.
Consent
Written informed consent in Japanese was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent is available for review by the Editor-in-chief of this journal.
Author’s Contributions
Nobuo Ohta used all of the data available and wrote the majority of this report. Yusuke Suzuki was the main consultant surgeon involved in the management of this patient. Yasuyuki Hinohira supplied the principles of surgical information in this article. Takayoshi Waki and Kazuya Kurakami saw the patient in hospital and contributed the case history notes used here. Takayoshi Waki reported on the histopathological findings and provided us with slides. All authors read and approved the final manuscript.
References
- Rokade A, Sama A (2012) Update on management of frontal sinus osteoma. Curr Opin Otolarygol Head Neck Surg 20: 40-44.
- Ledderose GJ, Betz CS, Steleter K, Leunig A (2011) Surgical management of osteoma of the frontal recess and sinus: extending the limits of the enodoscopic approach. Eur Arch Otorhinolaryngol 268: 525-532.
- Bigami M, Dallan I, Terranova P, Battaglia P, Miceli S, et al. (2004) Frontal sinus osteomas: window of endoscopic approach. Rhinology 42: 315-320.
- B Schick, C Steigerwald, A el Rahman el Tahan, W Draf (2001) The role of endoscopic surgery in the management of frontoethmoid osteomas. Rhinology 39: 66-70.
- Draf W (2005) Endonasal frontal sinus drainage type I–III according to Draf. In Kountaks S, Seniro B, Draf W. editors. The frontal sinus. (1st ed.) New York: Springer 219-231.
- Erdogan N, Demir U, Songu M, Ozenler NK, Uluç E, et al. (2009) A prospective study of paranasal sinus osteoma in 1889 cases: changing patterns of localization. Laryngoscope 119: 2355-2359.
Citation: Ohta N, Suzuki Y, Waki T, Kurakami K, Hinohira Y, et al. (2013) Exploring the Limits of the Endoscopic Approach to Frontal Sinus Osteoma. Otolaryngology 3:140. DOI: 10.4172/2161-119X.1000140
Copyright: © 2013 Ohta N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 16404
- [From(publication date): 9-2013 - Dec 23, 2025]
- Breakdown by view type
- HTML page views: 11537
- PDF downloads: 4867