Extranodal Natural-Killer/T-Cell Lymphoma, Nasal Type - Presenting as Non-Healing Palatal Ulcer
Received: 09-Nov-2012 / Accepted Date: 06-Dec-2012 / Published Date: 11-Dec-2012 DOI: 10.4172/2161-119X.1000123
Abstract
Oral cavity T-cell lymphoma occurs rarely. This case report describes a patient with such a tumor. The case was a 48 year old male presenting with a painless ulcer on palate mucosa. He had suffered from nasal obstruction. Pathology revealed the presence of a T-cell lymphoma tumor in the palate. Though rare, the signs and symptoms of the case suggest that T-cell lymphoma should be considered in the differential diagnosis of oral cavity lesions.
Introduction
Malignant lymphoma is a neoplasm originating from lymphocytes, lymphocyte precursor cells, or cells generated during the multipotential differentiation of a stem cell [1]. Approximately 80% of lymphomas originate from B lymphocytes [2]. Non-Hodgkin’s lymphoma (NHL) tends to invade tissues and organs that inherently do not consist of lymphoid cells [3]. Non-Hodgkin’s lymphoma may be located in oral soft tissues, but oral NHL usually involves B cell system, and less often T-cell system [2]. Palatal and nasal lymphomas are rare, and the majority of lymphomas in this region originate from B cells [4]. Since an early detection of hard palate tumors is difficult by clinical examination, the vast majority of such tumors are detected after maxillary or sphenoid bone invasion [5]. The present case report introduces a case of T-cell lymphoma involving the hard palate, the maxillary sinus and the nasal cavity. This type of lymphoma is rare in oral cavity and needs to special tests for correct diagnosis.
Case Presentation
The patient was a 48-year-old male, who was referred to the Department of ENT and Head & neck surgery, JJ Hospital, Mumbai with complaint of ulcer over the hard palate since one and half month. Patient was all right one and half months back when he noticed small ulcer over hard palate and that the ulcer had been rapidly enlarging, and causing loosening of teeth. The patient did not feel any pain, but had nasal congestion with nasal discharge with bilateral nasal obstruction. He was retired, and his medical history did not reveal any specific systemic condition. Also, he did take medications from local doctors but didn’t get any symptomatic improvement and was referred to our centre.
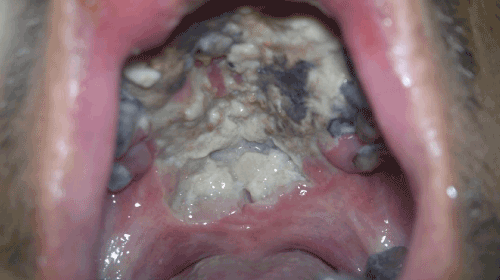
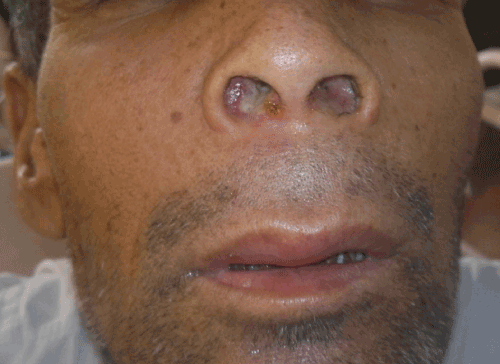
On clinical examination, the patient’s oral cavity revealed an ulcer measuring approximately 5×4 cm on the hard palate (Figure 1). The ulcer was involving both soft and hard palate extending bilaterally to alveolar ridge causing loosening and loss of teeth. The base was necrotic with slough and it did not bleed on touch. There was a mild swelling observed over upper lip (Figure 2). The examination of nose revealed a bulge in the floor of nose bilaterally with edematous and congested mucosa. The examination of the lymph nodes of the head and neck region revealed no palpable lymph node on either side. Patient also complained of intermittent fever and loss of appetite. Considering the rapid the growth of the lesion and a lack of previous history, a malignant lesion was suspected.
Laboratory tests revealed normal complete blood count (CBC), low hemoglobin and normal serum concentrations of urea, creatinine, uric acid, sodium, potassium, bilirubin, alkaline phosphatase, alanine transaminase (ALT) and aspartate trasaminase (AST). Histopathologic findings showed Hematoxylin and eosin staining of the biopsy specimens from the mass demonstrating diffuse proliferation of relatively small and atypical monoclonal lymphocytic cells. Neoplastic cells had round and hyperchromatic nuclei with dense and coarse chromatin. The tumor cells were positive for LAC, CD3 and CD43, CD56 and negative for CD20. Given the histopathological and clinical findings, the lesion was diagnosed as T-cell lymphoma. The patient was then referred to a hematologist and an oncologist for further evaluation. Spiral CT scans of the chest, abdomen and pelvic cavity, with injected and oral contrast media and pulmonary and mediastinal windows, did not reveal any other lymphadenopathy. Moreover, CT scans of the cardiovascular system, liver, gall bladder, spleen, pancreas, adrenal glands, urinary bladder and retroperitoneal areas revealed no pathologic changes. Metastasis and lymphadenopathy were not observed as well. Thus, the tumor was diagnosed as stage one lymphoma according to WHO staging system [2].
Treatment
The patient received chemotherapy in 3 phases. The chemotherapeutic drugs used were cyclophosphamide, methotrexate, doxorubicin, dexamethasone and prednisolone. After 3 chemotherapy sessions, histochemical examination of the patient’s blood revealed a decrease in WBC, red blood cells, hemoglobin, hematocrite, mean corpuscular volume, mean corpuscular hematocrite, mean corpuscular hemoglobin concentration and platelet counts, which was deemed to be the side effects of immunosuppressive drugs. After 3 months, a decrease in tumor size was observed, while the patient was suffering from the complications of the treatment and respiratory infection. Unfortunately, patient succumbed during treatment after 3 chemotherapy cycles.
Discussion
Malignant lymphoma can appear in all parts of the body, and may have varied radiographic manifestations [5]. Waldeyer’s ring, which consists of the nasopharynx, tonsils and the base of the tongue, is the most common location for malignant lymphoma in the head and neck region [2]. However, paranasal sinuses are considered rare locations for extra nodular lymphomas [4]. The present case was a T cell lymphoma invading the palatal, nasal and maxillary bones. Nasal natural killer/T- (NK/T) cell lymphomas are aggressive, locally destructive, mid facial and necrotizing lesions. Most of them were initially diagnosed as lethal midline granuloma, a term that is slowly being phased out [6]. A 15-year study demonstrated that 74% of nasal and paranasal sinuses lymphomas were of B cell origin [4]. The nasal cavity is the predominant site for the involvement of T-cell and NK/T-cell lymphoma, whereas sinus involvement without nasal disease is common in B-cell lymphoma [7]. An important consideration is the origin of the tumor’s T cells. It is not clear whether tumor was initiated from the maxillary sinus or palate. However, it had greatly expanded and invaded the maxillary sinus, nasal cavity and palate. The smooth surface of the mass could make the differential diagnosis of the minor salivary gland tumors or soft tissue sarcomas difficult. The rapid growth of lymphoma, compared to salivary gland tumors, is helpful in primary diagnosis; however, biopsy is necessary to confirm the diagnosis. Moreover, leukemia can cause radiolucency in the jaws, but there is usually no any jaw expansion and laboratory tests such as CBC and alkaline phosphatase that can be used in the diagnosis of leukemia. It is important for clinicians to differentiate malignant tumors such as lymphoma from benign lesions such as odontogenic cysts or tumors, which can cause jaw expansion. Rapid progression and bone destruction can indicate malignancy. The clinical presentation of malignant lymphomas of the oral cavity varies with the origin and type of the tumor, but in most cases, it appears as a smooth mass or occasionally as an ulcerated mass similar to salivary glands neoplasm or lymphoma. The presence of a specific subtype of T-cell lymphoma in the oral cavity appearing as gingival swelling in both maxilla and mandible was reported in a 76- years-old woman. Histopathological evaluation of the patient’s lesion led to the diagnosis of non-Hodgkin’s lymphoma with small cells. The tumor cells were positive for CD45 and CD3, which indicate that it was most likely of T-cell origin [8]. It has been reported that only 21% of NHLs are of T cell or NH/T cell origins, and are positive for CD56, CD43, CD45 and CD3 [9] Another important consideration in NHLs is the common signs and symptoms such as fever, weight loss, weakness, nocturnal sweating, increased susceptibility to infection, peripheral lymphadenopathy and splenomegaly [10]. One study has reported that systemic B symptoms such as fever, weight loss, weakness, nocturnal sweating, were frequently observed in NK/T-cell lymphoma. The patients in the present study did not show the above-mentioned signs and symptoms, but complained of nasal obstruction and bleed which indicated the involvement of the nasal cavity. Sinonasal lymphoma may present with nasal obstruction and bleeding, the invasion of oropharynx, palate and nasopharynx but other sites may be involved (sinonasal and intestinal). Furthermore, NHLs usually affects individuals over 40 years of age. Some studies have reported the highest prevalence for NHLs of Waldeyer’s ring in the fifth and sixth decades of life [11,12]. After diagnosing a lymphoma through physical examination, chemical examination of blood, CT scans of chest and abdomen and biopsy of bone marrow are required to determine the invasion of lymphoma [13]. Generally, the long-term survival rate of lymphoma is weak, and patients with a non-Hodgkin’s lymphoma tumor of 5 cm in diameter in the head and neck appear to have a worse prognosis than those with smaller tumors [12,13]. The treatment of choice for localized non- Hodgkin’s lymphoma is surgery and radiotherapy. In advanced cases, radiotherapy is applied following chemotherapy. In the case of diffuse neoplasm, chemotherapy is the treatment of choice. Similar to other lymphomas in the head and neck region, oral lymphoma seems to respond to chemotherapy and radiotherapy. The sign and symptoms of the present case indicate that non-Hodgkin’s lymphoma should be considered in the differential diagnosis of lesions observed in the sinonasal and oral cavity. Most of oral lymphomas are of B-cell origin, however, T-cell lymphomas should be considered as well. Moreover, clinical evaluation, histopathology and proper immunohistopathologic examination of the biopsy from the mass are essential for the correct diagnosis and successful treatment.
References
- Kozakiewicz M, Karolewski M, Kobos J, Stolecka Z (2003) Malignant lymphoma of jaw bone. Med Sci Monit 9: 110-114.
- Greenberg M, Glick M, Ship AJ (2008) Burket’s Oral Medicine. (11thedn), USA: BC Decker INC. 174-175.
- Clearly KR, Batsakis JG (1994) Sinonasal lymphoma. Ann Otol Rhinol Laryngol 103: 911-914.
- Fellbaum C, Hansmann ML, LennertK (1989) Malignant lymphomas of the nasal cavity and paranasal sinuses.Virchows Arch A PatholAnatHistopathol 414: 399- 405.
- Ueda F, Suzuki M, Matsui O, Minato H, Furukawa M (2005) MR findings of nine cases of palatal tumor. MagnReson Med Sci 4: 61-67.
- Mehta V, Balachandran C, Bhat S, Geetha V, Fernandes D (2008) Nasal NK/T cell lymphoma presenting as a lethal midline granuloma. Indian J Dermatol Venereol Leprol 74: 145-147.
- Kim GE, Koom WS, Yang WI, Lee SW, Keum KC, et al. ( 2004) Clinical relevance of three subtypes of primary sinonasal lymphoma characterized by immunophenotypic analysis. Head neck 26: 584-593.
- Matsumoto N, Ohki H, Mukae S, Amano Y, Harada D et al. (2008) Anaplastic large cell lymphoma in gingiva: case report and literature review. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 106: e29-e34.
- Yin HF, Jamlikhanova V, Okada N, Takagi M (1999) Primary natural killer/T-cell lymphomas of the oral cavity are aggressive neoplasms. Virchows Arch435: 400-406.
- Huang KJ, Wang LF, Lee KW, Ho KY, Kuo WR et al. (2003) Sinonasal NK/T-cell lymphoma with upper gastrointestinal bleeding: a case report. Kaohsiung J Med Sci 19: 639-643.
- Tham IW, Lee KM, Yap SP, Loong SL (2006) Outcome of patients with nasal natural killer (NK)/T-cell lymphoma treated with radiotherapy, with or without chemotherapy. Head Neck 28: 126-134.
- Tauber S, Nerlich A, Lang S (2006) MALT lymphoma of the paranasal sinuses and the hard palate: report of two cases and review of the literature. Eur Arch Otorhinolaryngol 263: 19-22.
- Ezzat AA, Ibrahim EM, El Weshi AN, Khafaga YM, AlJurf M, et al. (2001) Localized non-Hodgkin's lymphoma of Waldeyer's ring: clinical features, management,and prognosis of 130 adult patients. Head Neck 23: 547-558.
Citation: Shreyas Joshi S, Jagade MV, Saurabh A, Dnyaneshwar A, Sunita B (2012) Extranodal Natural-Killer/T-Cell Lymphoma, Nasal Type - Presenting as Non-Healing Palatal Ulcer. Otolaryngology 2:123. DOI: 10.4172/2161-119X.1000123
Copyright: © 2012 Shreyas Joshi S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 18746
- [From(publication date): 12-2012 - Dec 07, 2025]
- Breakdown by view type
- HTML page views: 13871
- PDF downloads: 4875