Foreign Body In TemporomandibularJoint Region
Received: 29-May-2013 / Accepted Date: 23-Jul-2013 / Published Date: 30-Jul-2013 DOI: 10.4172/2161-119X.1000137
Abstract
Objective: The objective of this study is to investigate the safety and effectiveness of a new minimally invasive technique of coblation used in infants with epiglottic cyst.
Methods: 42 consecutive patients with epiglottic cyst underwent surgery by use ArthroCare ENT Coblator II Surgery System.
Results: All patients, including 29 males and 13 females, ranging in age from 1week to 4 years when surgery. All these patients recovered with no complications and was discharged from hospital in 7 days after surgery, no perioperative bleeding noted in any patient. The postoperative follow-up period ranged from 6 to 60 months, no recurrence was found during the follow-up examinations.
Conclusion: Use ArthroCare ENT Coblator II Surgery System for treatment of infant epiglottic cysts is simple, safe, and effective.
Keywords: Foreign body, Temporomandibular joint
253833Introduction
Foreign bodies are frequently encountered by otolaryngologists even then, they can represent a challenge for the surgeons due to several factors, such as object size, accessibility difficulties and a close anatomic relation with vital structures [1]. Usually, they are a consequence of accidents. Foreign bodies lodged accidently through external trauma pose a danger of injury to vital structures on the face. Their removal also requires a meticulous dissection so as to avoid injury to important anatomical structures of the face. The removal of foreign bodies occurs in approximately one third of the cases, because initially they are radiologically missed or misdiagnosed [2]. Occasionally, foreign bodies may be retained for some time causing persistent and distressing symptoms [3]. There are several ways to detect foreign bodies: radiographies, computed tomography, magnetic resonance and even ultrasonographies can be used depending on the foreign body localization and composition [4,5]. Facial surgical procedures implies a risk of damaging important anatomic structures. Even if the exact position of the foreign body is known from imaging data, the accurate reproduction of this position in the patient body can be difficult if this object is not adjacent to a definitive anatomic landmark.
A rare case of a foreign body lodged accidently in the temporomandibular joint (TMJ) has been presented
Case Report
A 17 year old male patient was presented to the department of otorhinolaryngology, JJ Hospital, Byculla, Mumbai with history of accidental insertion of a metallic foreign body in right postauricular region. Patient had major complaint of pain over the right postauricular region and trismus.
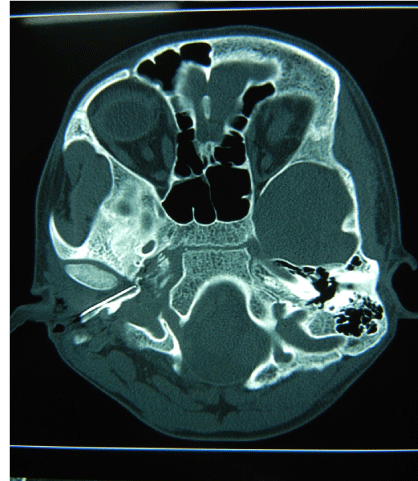
On observation, tenderness was found over the right post auricular region with an entry wound at angle of mandible, externally clinically the foreign body could not be located by palpation. Plain radiograph of the face in apical and lateral view revealed foreign body over the right TMJ. The CT scan of the face revealed a 2.1 cm long sharp metallic foreign body lodged into the Right Temporomandibular joint 8mm deep to the skin surface lying parallel along the angle of mandible (Figure 1-3).
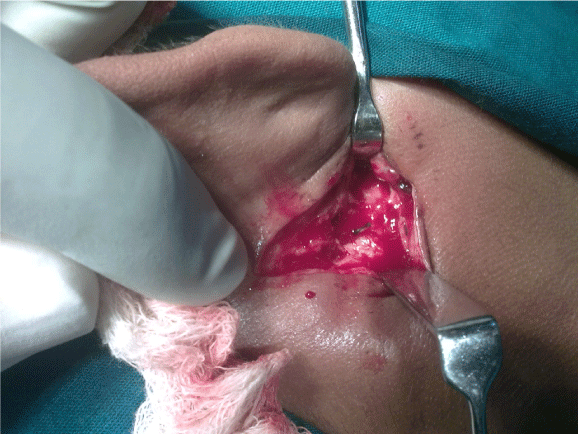
The patient was posted for surgery. He was taken under general anaesthesia. A 2 cm incision was taken along the angle of mandible from the ear lobule downwards. A small flap was raised anteriorly and dissection done. The metallic foreign body being compatible with a needle was exposed. It was removed with careful dissection around the body and securing hemostasis and avoiding any injury to the facial nerve. The wound was thoroughly washed with antiseptic and closure done, in layers. The post operation period was unremarkable and patient was discharged after 24 h of observation.
Discussion
This was an unusual foreign body being lodged accidentally from entry through angle of mandible below the EAC and into the TMJ. The important anatomical structures, facial nerve and major vessels were in close relation. Precise knowledge of the facial anatomy and the surgical expertise is required for extraction and exact exposition of novel structures.
The treatment for first stage of a trauma patient consists in a detailed analysis of the facial symmetry and function, followed by an adequate antisepsis of the lacerated and contused tissues. This evaluation must be corroborated by image exams, such as radiograph, computed tomography with axial and coronal projections,when necessary. The treatment sequence involved approach, foreign body withdrawal, wound exploration, irrigation and suturing. Regarding wound contamination, antibiotics and tetanus prophylaxis was given [6,7]. The reported case was managed this way. The entire foreign body was removed successfully, without any intercurrences. In the present case, there was a danger of injury to the facial nerve which lies in close proximity to the involved region, during the removal.
We report this case for several reasons. First, the patient’s presentation was unusual with respect to the site of penetration of the rusty needle, in the temporomandibular joint. Second, the curved nature of the foreign body is very important in terms of the surgical removal. If the object is removed suddenly during surgery just by superficial pulling without proper exposure, it may drag the neurovascular structures together with it and may cause fatal injuries.
A foreign body can remain asymptomatic for a long time and, finally, present acute symptoms. Foreign bodies should be extracted immediately as they can lead to recurrent and chronic infections. If retained for a longer period of time, foreign body has a potential to induce an inflammatory reaction and over a period of time may lead to foreign body granuloma and in the present case may lead to ankylosis of temporomandibular joint.
In the last years, many authors have been indicating the use of the navigation systems for foreign bodies in facial region, specially when implies in danger for important anatomical structures, failure of previous attempts at removal the foreign body, the presence of multiple foreign bodies, the desire to achieve a minimally invasive access and to allow a quicker operation [8-10]. The referred method was not used on the case reported, due to the foreign body size and its superficial and easy location. It is of vital importance the professional knowledge about the possible foreign body existence on the patient’s head and neck segment in order to decrease the delayed foreign body’s removal due to several common misdiagnosis errors, reducing the complications that are likely to occur when foreign bodies are retained in the organism.
Conclusion
This is a rare case of foreign body lodged in temporomandibular joint. Precise knowledge about the regional anatomy is essential to prevent injury to the vital structures in the area during foreign body removal. It is important to identify the location of foreign body by appropriate investigations before deciding upon the plan for removal as it may lie over an important neural or vascular structure and pulling out of foreign body without adequate exposure of foreign body may lead to fatal complications.
References
- Holmes PJ, Miller JR, Gutta R, Louis PJ (2005) Intraoperative imaging techniques: A guide to retrieval of foreign bodies. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 100: 614-618.
- Robinson PD, Rajayogeswaran V, Orr R (1997) Unlikely foreign bodies in unusual facial sites. Br J Oral Maxillofac Surg 35: 36-39.
- Cameron M, Phillips B (2006) Snookered Facial infection secondary to occult foreign body. Int J Oral Maxillofac Surg 35: 373-375.
- Krimmel M, Conelius CP, Stojadinovic S, Hoffman J, Reinert S (2001) Wooden foreign bodies in facial injury: a radiological pitfall. Int J Oral Maxillofac Surg 30: 445-447.
- Oikarinen KS, Nieminen TM, Makarinen H, Pythinen J (1993) Visibility of foreign bodies in soft tissue in plain radiographs, computed tomography, magnetic resonance imaging, and ultrasound. An in vitro study. Int J Oral Maxillofac Surg 22: 119-124.
- Shinohara EH, Heringer L, de Carvalho JP (2001) Impacted knife injuries in the maxillofacial region: report of 2 cases. J Oral Maxillofac Surg 59: 1221-1223.
- Waldman LA (1979) Facial cellulitis caused by unrecognized foreign body. Oral Surg Oral Med Oral Pathol 48: 408-409.
- Eggers G, Haag C, Hassfeld S (2005) Image-guided removal of foreign bodies. Br J Oral Maxillofac Surg 43: 404-409.
- Paoli JR, Dekeister C (2001) A tooth in the orbit. Br J Oral Maxillofac Surg 39: 327
- Sießegger M, Mischkoski RA, Schneider BT, Krug B, Klesper B, et al. (2001) Image guided surgical navigation for removal of foreign bodies in the head and neck. J cranioMaxillofac Surg  29: 321-325.
Citation: Agarwal S, Jagade MV, Mishra A, Joshi S (2013) Foreign Body In TemporomandibularJoint Region. Otolaryngology 3: 137. doi:10.4172/2161- 119X.1000137 DOI: 10.4172/2161-119X.1000137
Copyright: © 2013 Agarwal S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 14909
- [From(publication date): 9-2013 - Dec 15, 2025]
- Breakdown by view type
- HTML page views: 10119
- PDF downloads: 4790