Review Article Open Access
Health Behaviour Change: Advancing the Utility of Motivational Interviewing(MI) to Health Promotion
Emmanuel Appiah-Brempong1*, Paul Okyere1, Ruth Cross2 and Rose Odotei Adjei11Kwame Nkrumah University of Science and Technology, Ghana
2Leeds Metropolitan University, UK
- *Corresponding Author:
- Emmanuel Appiah-Brempong
Lecturer, Kwame Nkrumah University of Science and Technology
Community Health, Ghana
Tel: +233 3220 60021
E-mail: brempong2003@yahoo.com
Received date: July 26, 2013; Accepted date: December 10, 2013; Published date: December 28, 2013
Citation: Appiah-Brempong E, Okyere P, Cross R, Adjei RO (2013) Health Behaviour Change: Advancing the Utility of Motivational Interviewing (MI) to Health Promotion. J Addict Res Ther 4:167. doi:10.4172/2155-6105.1000167
Copyright: © 2013 Appiah-Brempong E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
Originally developed to address addictive health behaviour, Motivational Interviewing (MI) is gaining recognition in health promotion as a style for eliciting individual’s intrinsic motivation to change. The growing recognition could be attributed to the increasing understanding that the practice of unhealthy behaviours may not be due to deficiency in knowledge of consequences, but rather a lack of adequate motivation to change. In this paper the utility of MI to the field of health promotion is discussed, elaborating the important contribution of MI to client empowerment. A model for MI delivery in health promotion has been suggested by authors, highlighting some essential elements to be targeted by practitioners. Though MI may not be a panacea to all addictive health behaviour change, it presents useful principles which may be lacking in conventional cognitive behavioural therapies. Thus, from literature, MI is presented as a promising approach which can augment the existing socio-environmental strategies of health promotion.
Keywords
Motivational interviewing; Behaviour change; Health promotion; Utility
Introduction
Numerous studies have established a direct relationship between health behaviours and health outcomes and have demonstrated their significant role in both morbidity and mortality [1-3]. Due to the significant impact of health behaviour on many health outcomes, there is abundance of health promotion interventions and/or programmes that aim to engender healthful lifestyle among the populace. There is evidence that theory-based interventions or programmes have a higher likelihood of being effective in eliciting behaviour change in individuals [4,5]. Health promotion practitioners have relied on a number of behaviour change theories and approaches in their quest to facilitate individual health behaviour change [4,6]. One of such approaches (Motivational Interviewing) is discussed in this paper.
Motivational Interviewing is a promising approach for addressing contemporary health issues in health promotion practice [7,8]. Motivational Interviewing is a person-centred counselling style for addressing the common problem of ambivalence about change [9]. Miller and Rollnick have refined further the MI style into a four-process model instead of phases that encapsulate engaging, focusing, evoking and planning. These four processes are both sequential and iterative, implying that practitioners can move forward and backwards in an encounter with client. The underlying spirit of MI includes partnership/ collaboration, acceptance, compassion and evocation [9].
The primary purpose of this paper is to discuss the utility of MI to the field of health promotion, suggesting a model for MI delivery in health promotion.
MI: Description and Theoretical Basis
Miller and Rollnick have put forward three different but interrelated definitions of Motivational Interviewing. For the purposes of this paper, (MI) is defined as a person-centred counselling style for addressing the common problem of ambivalence about change. MI interview is therefore designed to strengthen motivation for and commitment to a specific goal by eliciting and exploring the person’s own reason for change within an atmosphere of acceptance and companion [9]. According to Miller and Rollnick, MI involves four sequential and recursive processes namely engaging, focusing, evoking and planning. The process of engaging requires the practitioner and the client establishing a helpful working relationship which is fundamental to any therapeutic encounter. Focusing refers to the process whereby the practitioner together with the client develops and maintains specific direction towards change goals. Evoking entails eliciting the client’s own motivation for change while planning involve developing commitment to change and enacting specific plan of action. These four processes that comprise MI delivery in practice are not mutually exclusive and each later stage builds upon the previous one. The delivery of MI should be underpinned by the ‘spirit’ of MI. The spirit of MI is that of collaboration and not confrontation, evocation and not education, compassion and attitude of profound acceptance of clients. Thus, the practitioner administering MI is required to be in partnership with clients, respecting their expertise and perspectives, and recognising that resources for change reside with the client (ibid). In a bid to explore and resolve ambivalence, a key strategy of MI is to initiate a change talk; which involves the client’s personal expression of the advantages of change, as against the disadvantages of maintaining the status quo [8].
The term Motivational Interviewing (MI) has its root in the work of Miller (1983), and offers an approach based on the principles of experimental social psychology [10]. MI is recognised to have been developed drawing from theories such as the cognitive dissonance theory the self-perception theory and the work of Rogers on clientcentred therapy [11-13]. The fundamental principles underlying these theories are that, people consider change when their personal goals or values conflict with their current behaviour, people tend to be committed to what they hear themselves argue for and defend, and practitioner’s attitude and care is vital for intervention success [8,14].
MI and Cognitive Behaviour Therapies
Cognitive Behaviour Therapies (CBTs), emerged from the Cognitive Behaviour model which categorises human experience into four components namely; behaviour (situation, events, actions, skills), affect (mood, feelings, emotions), cognitions (thoughts, attitudes, beliefs, assumptions, memories, expectations), and physiology (tension, fitness, diet, health status). Underpinning CBTs is the notion that an individual’s health conditions are as a result of what they think and what they do [8].
Though CBTs are widely used in both clinical and field settings, it is distinguished from MI. Practitioners of CBTs tend to confront client’s irrational or maladaptive behaviours; however, MI rarely involves such confrontations of beliefs [7]. In MI there is no direct attempt to question, persuade or provide advice; instead practitioners using MI are expected to offer reflective listening and positive affirmations (ibid). In the light of this, Michael et al. (2006) exhorts practitioners to approach clients with respect and desist from passing judgements on clients’ experiences and perspectives [15]. It is in this way that MI distinguishes itself from CBTs by offering ingredients necessary for understanding health behaviour, and helping trigger innate motivation which is paramount for behaviour change.
The Complementary Role of MI and the Stages of Change
An understanding of the Stages of Change is essential to health promotion practice. Knowledge of the precise stage which characterises a target group enables practitioners to design appropriate interventions and develop measurable indicators for assessing intervention outcomes. At the heart of the Stages of Change is the notion that behaviour change journeys through five main stages which are; pre-contemplation, contemplation, preparation, action, and maintenance [16].
Owing to the complementary role played by MI and the Stages of Change, Miller and Rollnick (2002) have described the two as a ‘natural fit’ [17]. The Stages of Change has played an essential role in the development of MI [18,19]. Similarly, MI facilitates the process of health behaviour change. Precisely, MI is able to contribute to the generation of clients’ intrinsic motivation necessary for moving clients from one stage of change to the other. Gintner and Choate (2003) have asserted that MI is well suited for handling the peculiar characteristics displayed by pre-contemplators especially in an alcohol intervention [20].
MI For Health Promotion
Developing personal skills
To a large extent, the Ottawa Charter continues to influence health promotion practice in the 21st century [21]. It continues to provide a systematic framework for considering any major public health challenge through its five action areas – build healthy public policy; create supportive environments for health; strengthen community actions; develop personal skills; and reorient health services [22]. The Ottawa Charter has also broadened the scope of health promotion and shifted attention away from models of individual behaviour change to embracing a socio-ecological model of health promotion [23,24]. A key action area of the charter is to “develop personal skills”. Developing personal skills is essentially dependent on information flow from health practitioners to individuals [25]. Thus, health information enables individuals to increase in knowledge, and contributes to sharpening their skills to be able to engage in healthy practices. Rubak has asserted that MI is essential for developing the personal skills of individuals toward a complete state of physical, mental and emotional health and well-being. MI enables individuals to identify and do something about their health behaviour [26]. One of the four process-model of the MI style is planning. The process of planning as described by Miller and Rollnick is instrumental in helping the client to develop decisionmaking skills regarding when and how to change as the client works through the ambivalence. It is also at this point that the practitioner may provide information and advice regarding how and when the client can proceed when the decision has been made by the client to change (ibid). In view of this, MI is useful for eliciting intrinsic motivation for behaviour change and strengthening the client’s own capacities to change.
Furthermore, a vital action area of health promotion is to strengthen community action. Strengthening community action is essential to ensure social action and influence [27]. Community actions can be better strengthened when the personal skills of individuals who make up the community are developed. The level of health and well-being in a community is to a great extent determined by the way of life and behaviour of its members [28]. Consequently, when the individual’s capacities are strengthened through the development of self-efficacy and increased self-awareness, individual community members will be better enabled to take collective action to improve the health and well-being of their community. Further, in a study by Dilion and Philip, it was ascertained that community engagement in health and action was significantly associated with the extent to which individuals valued health or believed that healthiness was important [28]. In this way, triggering the intrinsic motivation to change, developing personal skills, and enhancing self-efficacy of individuals become fertile grounds to enable community action to improve health and well-being. In view of the potential of MI to influence the development of client’s personal skills and intrinsic motivation to change it has the potential to facilitate individual’s engagement in community action, albeit indirectly [8].
Individual participation and empowerment
At the heart of health promotion are the concepts of participation and empowerment [25]. Client participation in intervention delivery is key to achieving positive intervention results [29-31]. MI is designed to be client-centred, and promotes a process of active client participation in the change process to ensure that decisions regarding behaviour change emanate primarily from the client and not from the health practitioner [10,17]. In ‘developing discrepancy’ (i.e. a principle of MI), practitioners are required to assist clients to identify a gap between their personal goals or values and the status quo. Such an activity results in ‘critical consciousness-raising’, which is a key component of the empowerment model of health promotion [6]. Again, MI seeks to develop ‘self-efficacy’ of clients, which is fundamental to individual or self-empowerment [32]. There is a growing recognition of the importance of empowerment in HP, even though this recognition is often an issue of lip service rather than practice and policy [6]. Empowering individuals and communities is critical to ensuring that people take control over and improve their health [25]. It is in the light of this that all health promotion activities should be guided by the principle of empowerment [33]. On the other hand, MI like other individual-level interventions have been criticised for the tendency to neglect issues of the wider social determinants of health. It should however be recognised that health promotion practice is both ‘individual’ and ‘collective’ centred [34]. Thus, individual-level approaches are as essential as approaches that deal with the wider social environment.
Applications of MI: One-on-One Vs. Group Formats
Some studies have reported the efficacy of MI interventions delivered in a one-on-one format and those delivered in a groupformat [35-37]. Although, Nyamathi et al. admit a paucity of research investigating the different outcomes of these two formats, results of their study showed no evidence of difference in efficacy of a one-onone format and group- format in an intervention to reduce alcohol consumption [38]. Conversely, findings of a study by Rubak et al. [26] suggest that relying solely on group-format may not be adequate. A combined approach may therefore be appropriate.
Evidence-base of MI
In a bid to assess the efficacy and effectiveness of MI interventions, some systematic reviews and meta-analyses have been conducted across various domains. Lai et al. in a meta-analysis have reported positive outcomes for studies which used MI for smoking cessation [39]. Furthermore, in a systematic review by Dunn et al., adaptations of MI are reported to be effective in addressing a range of behavioural issues including substance abuse [40].
On the other hand, Lundahl et al. in a meta-analysis of studies conducted on addictive behavioural domains (including tobacco, marijuana and alcohol) have reported that MI only produced significant effects when judged against weak comparison groups [41]. Furthermore, Vasilaki et al. in a meta-analytic review have reported that the efficacy of MI tends to decrease when data on dependent drinkers was included in the analysis [42]. Although few reviews and meta-analysis report no significant difference between MI effectiveness and that of other strong alternatives (e-CHUG), overall the studies admit that MI remains an effective approach for behaviour change [43]. Additionally, MI has been shown to be effective in comparison with traditional advice giving [26]. In moving forward, MI as an intervention will be enhanced enormously if future studies investigate what factors might moderate intervention effectiveness, the format in which MI intervention should be delivered (i.e. whether individual or group based) and whether MI is more effective with mandatory or voluntary clients.
A suggested model for MI delivery in health promotion
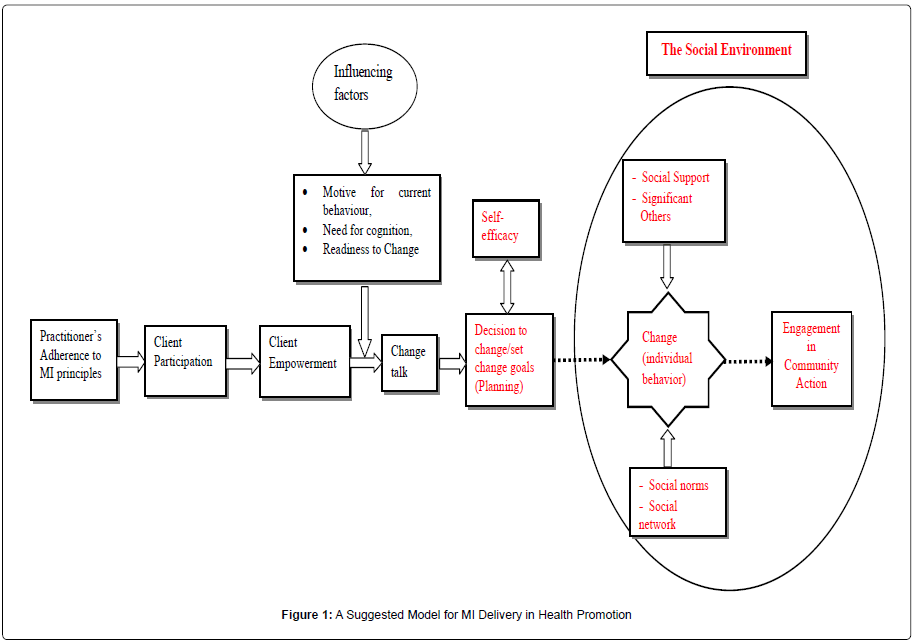
Owing to the numerous adaptations of MI in health promotion practice, it is possible to misjudge the effectiveness of MI in an intervention study. Nevertheless, some vital elements within the client’s ‘intrinsic environment’ as well as the wider social environment could be influenced in a manner that ensures the attainment of optimal health outcomes. It is for this reason that we suggest a simple model which links the MI delivery processes to community action for health promotion. Model is presented as Figure 1.
The success of any MI intervention is highly dependent on practitioners’ adherence to the principles and processes of MI which have succinctly stated to encapsulate - engaging; focusing, evoking; and planning [9]. Adhering to these processes is fundamental to clients’ willingness and readiness to participate in the MI process. Citizen participation in health decision making in terms of setting priorities, planning strategies and implementing actions is critical to and indeed a positive outcome of health promotion intervention [25].
One of the important goals or outcomes of health promotion interventions is empowerment. This recognition has resulted in the development of the empowerment model of health promotion. According to Naidoo and Wills this model seeks to enable individuals to identify their own concerns and gain the skills and confidence to act upon [31]. Characteristically, the role of the health promoter is to facilitate the process whereby individuals come to gain control over their lives and are empowered to change their social reality.
In a similar vein, the role of the health professional that makes use of the model suggested in this paper is to primarily adhere to the principles of MI which recognises that the individual possesses the resources for change and consequently the role of the practitioner is to help the client elicit this expertise. As indicated in the model, empowerment of the client will be attained when the practitioner adheres to the MI principles and the client fully engages and participate in the process of change. The eventual outcome of the whole intervention process is to elicit behaviour change although admittedly, it is not every intervention process that ultimately produces behaviour change.
It is imperative to also stress that health behaviour change can be significantly affected by factors that pertain to the individual’s social environment (social support, social norms, social network etc) even after the individual has made the decision to change his/her behaviour. Therefore, such socio-environmental variables should be favourable in order for change to occur. We posit that the potential and propensity to engage in community action will be highly strengthened after the individual has gone through this change process. This may emanate from the development of client’s skill, enhanced self-efficacy and a commitment to change. Thus the model illuminates our understanding of how MI contributes to the achievement of participation, individual empowerment and the enablement of community action which are all very important goals or outcomes of empowerment approach to health promotion interventions.
Conclusion
We have discussed the utility of MI in health promotion. Practitioners’ adherence to the principles and processes of MI will enable the clients to fully engage with and participate in the process of change. Through this, the development of clients’ interpersonal skills and enhanced self-efficacy will be enabled, thereby empowering clients. In the suggested model, it is also important for practitioners to identify and/or influence some vital elements within the client’s ‘intrinsic environment’ as well as the wider social environment in a manner that ensures the attainment of optimal health outcomes. A limitation of the model is that it is yet to be empirically applied to any healthrelated behaviour. The paper however contributes to our understanding of how MI intervention reinforces and enables the realisation of critical principles, goals and values of health promotion – developing personal skills, participation, and empowerment and strengthening of community action. In order to build evidence on this model, future research or health promotion interventions should attempt to apply the model to a health-related addictive behaviour. MI as an intervention is presented as a promising approach which can augment the existing socio-environmental strategies of health promotion.
References
- Blaxter M (1990) Health and Lifestyles. London: Routledge.
- Freund KM, Belanger AJ, D'Agostino RB, Kannel WB (1993) The health risks of smoking. The Framingham Study: 34 years of follow-up. Ann Epidemiol 3: 417-424.
- Akl EA, Gaddam S, Gunukula SK, Honeine R, Jaoude PA, et al. (2010) The effects of waterpipe tobacco smoking on health outcomes: a systematic review. Int J Epidemiol 39: 834-857.
- Holloway A, Watson HE (2002) Role of self-efficacy and behaviour change. Int J Nurs Pract 8: 106-115.
- Nutbeam D, Harris, E Marilyn W (2010) Theory in a Nutshell: A practical guide to health promotion theories. (3rdedn) Sydney: McGraw-Hill.
- Green J, Tones K (2010) Health promotion: Planning and strategies. (3rdedn) London, SAGE Publications Limited.
- Resnicow K, DiIorio C, Soet JE, Ernst D, Borrelli B, et al. (2002) Motivational interviewing in health promotion: it sounds like something is changing. Health Psychol 21: 444-451.
- Hillsdon M (2006) Motivational interviewing in health promotion (p74). In: Macdowall W, McGraw-Hill.
- Miller WR, Rollnick S (2013) Motivational Interviewing: Helping people change. (3rd edn) New York, Guilford Press.
- Miller WR (1983) Motivational interviewing with broken drinkers. Behavioural Psychotherapy 11: 147-172
- Festinger L (1957) A theory of cognitive dissonance. Stanford, CA: Standford University Press.
- Bem DJ (1972) Self-perception theory. In: Berkowitz L (edn) Advances in experimental social psychology. New York, Academic Press.
- Rogers CR (1951) Client-centered therapy. Boston: Houghton-Mifflin.
- Farber BA (2007) On the enduring and substantial influence of Carl Rogers' not-quite necessary nor sufficient conditions. Psychotherapy (Chic) 44: 289-294.
- Michael KD, Curtin L, Kirkley DE, Harris R (2006) Group-Based Motivational Interviewing for Alcohol Use Among College Students: An Exploratory Study. Professional Psychology 37: 629-634.
- Prochaska JO, DiClemente CC (1983) Stages and processes of self-change of smoking: toward an integrative model of change. J Consult Clin Psychol 51: 390-395.
- Boardman T, Catley D, Grobe JE, Little TD, Ahluwalia JS (2006) Using motivational interviewing with smokers: do therapist behaviors relate to engagement and therapeutic alliance? J Subst Abuse Treat 31: 329-339.
- DiClemente CC (1999a) Motivation for change: Implications for substance abuse. Psychological Science 10: 209-213.
- Miller WR, Rollnick S (1991) Motivational interviewing: Preparing people to change. New York, Guilford Press.
- Gintner GG, Choate LH (2003) Stage-Matched Motivational Interventions for College Student Binge Drinkers. Journal of College Counselling 6: 99-113.
- Nutbeam D (1998b) Health promotion glossary. Health Promotion International: 13 (4) Oxford University Press.
- Nutbeam D (2008) What would the Ottawa Charter look like it were to be written right? Critical Public Health 18: 435-441.
- Porter C (2007) Ottawa to Bangkok: changing health promotion discourse. Health Promot Int 22: 72-79.
- Kessler C, Renggli V (2011) Health Promotion: Concepts and practices: A key issue paper focusing on the relevance for international cooperation. Basel: Swiss Centre for International Health.
- World Health Organisation (1986) Ottawa charter for health promotion: an international conference on health promotion, the move towards a new public health. Ottawa, Canada, WHO.
- Rubak S, Sandbaek A, Lauritzen T, Christensen B (2005) Motivational interviewing: a systematic review and meta-analysis. Br J Gen Pract 55: 305-312.
- Nutbeam D (2000) Health literacy as a public health goal: a challenge for contemporary health education and communication strategies into the 21st century. Health Promotion International 15: 259-267.
- Dillion HS, Philip L (1994) Health promotion and community action for health in developing countries. Geneva: World Health Organisation.
- Simonsen-Rehn N, Øvretveit J, Laamanen R, Suominen S, Sundell J, et al. (2006) Determinants of health promotion action: comparative analysis of local voluntary associations in four municipalities in Finland. Health Promot Int 21: 274-283.
- Naidoo J, Wills J (2000) Health promotion: foundations for practice (2nd edn) London, Baillière Tindall.
- Naidoo J, Wills J (2005) Public health and health promotion: developing practice, 2nd edition. London, Baillière Tindall.
- Tones K, Tilford S (2001) Health promotion: effectiveness, efficiency and equity (3rd edn) London, Nelson Thornes Ltd.
- McQueen D, Anderson L (2001) What counts as evidence: issues and debates. In: Rootman I, Goodstadt M, Hyndman B, et al., (edn) Evaluation in Health Promotion: Principles and Perspectives. WHO Regional Publications, European Series, Copenhagen, Denmark WHO: 77.
- Beattie A (1991) Knowledge and control in health promotion: a test case for social policy and social theory. In: J Gabe M Calnan M Bury (eds.) The Sociology of the Health Service, London: Routledge.
- Borsari B, Carey KB (2005) Two brief alcohol interventions for mandated college students. Psychol Addict Behav 19: 296-302.
- Feldstein SW, Forcehimes AA (2007) Motivational interviewing with underage college drinkers: a preliminary look at the role of empathy and alliance. Am J Drug Alcohol Abuse 33: 737-746.
- LaBrie JW, Pedersen ER, Earleywine M, Olsen H (2006) Reducing heavy drinking in college males with the decisional balance: analyzing an element of Motivational Interviewing. Addict Behav 31: 254-263.
- Nyamathi A, Shoptaw S, Cohen A, Greengold B, Nyamathi K, et al. (2010) Effect of motivational interviewing on reduction of alcohol use. Drug Alcohol Depend 107: 23-30.
- Lai DT, Cahill K, Qin Y, Tang JL (2010) Motivational interviewing for smoking cessation. Cochrane Database Syst Rev: CD006936.
- Dunn C, Deroo L, Rivara FP (2001) The use of brief interventions adapted from motivational interviewing across behavioral domains: a systematic review. Addiction 96: 1725-1742.
- Lundahl BW, Kunz C, Brownell C, Tollefson D, Burke BL (2010) Meta-analysis of motivational interviewing: Twenty-five years of empirical studies. Research on Social Work Practice 20: 137-160.
- Vasilaki EI, Hosier SG, Cox WM (2006) The efficacy of motivational interviewing as a brief intervention for excessive drinking: a meta-analytic review. Alcohol Alcohol 41: 328-335.
- Murphy JG, Dennhardt AA, Skidmore JR, Martens MP, McDevitt-Murphy ME (2010) Computerized Versus Motivational Interviewing Alcohol Interventions: Impact on Discrepancy, Motivation, and Drinking. Psychol Addict Behav 24: 628-639.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 16610
- [From(publication date):
December-2013 - Dec 21, 2025] - Breakdown by view type
- HTML page views : 11778
- PDF downloads : 4832