Naso-Ethmoidal Angioleiomyoma: A Mini-Invasive Combined Endoscopic and Microscopic Surgical Approach
Received: 15-Feb-2012 / Accepted Date: 06-Mar-2012 / Published Date: 12-Mar-2012 DOI: 10.4172/2161-119X.1000110
250970Introduction
Angioleiomyomas (AL) of the nasal cavity and paranasal sinuses are extremely rare benign tumors, representing less than 1% of all leiomyomas in the human body [1]. Common sites are the uterus and the gastrointestinal tract [2]. It is very rare into the nasal-paranasal cavities (only fifteen cases are reported in the literature) due to the paucity of smooth muscle tissue in this site [3].
Because of its rarity, the literature of AL in the nasal cavity and paranasal sinus is reviewed and the management is discussed.
Case Report
A-40-year-old man was admitted to the Radiology Department of our institution for the evaluation of a palpable tender mass protruding at the right medial canthus. The patient had observed a slow growth of this mass, associated with progressive reduction of smell, right nasal obstruction an omolateral recurrent self limited nasal bleeding.
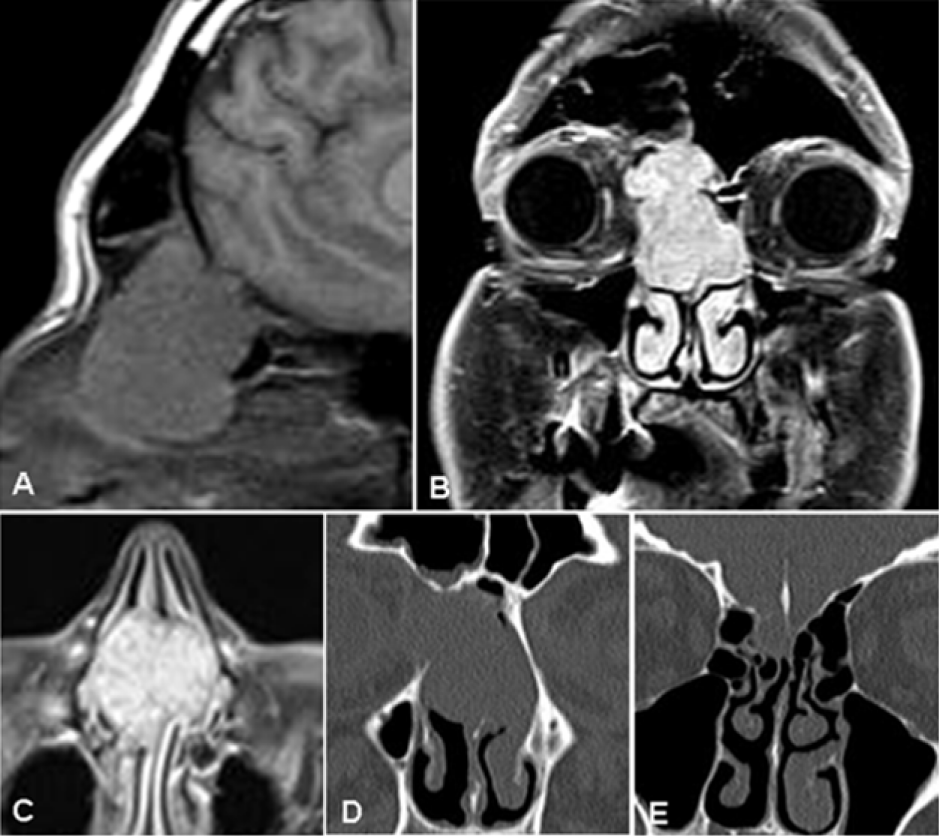
Ultrasound examination revealed a lobulated solid tissue with a rich homogeneous vascularity at the color-doppler. Nasal fibroendoscopic examination revealed an easily bleeding mass occupying the right nasal cavity completely. MRI confirmed a solid mass (38 x 28 x 28 mm) centered at the level of the right nasal cavity and anterior ethmoid cells, crossing the midline, with lateral involvement of the medial orbital wall and dislocation of the right peri-bulbar fat with cranial extension. Disruption of the right paramedian cortical bone of the anterior cranial fossa due to bone remodelling was observed at the contextual CT examination with coronal reformatted images (Figure 1). After gadolinium-containing contrast agent (Omniscan) intravenous administration, the lesion showed intense and homogeneous enhancement with tiny hypointense spots in the context of the lesion. The pathologic study revealed fragments of nasal mucosa with aspects of hyperaemia and mild inflammation.
Figure 1: MR/CT diagnostic work-up. Solid mass showed hypointense signal on sagittal T1 weighted images (A) with net and homogeneous enhancement after intravenous administration of gadolinium contrast agent on coronal (B) and axial (C) planes. CT images (D and E) demonstrated bone remodelling of the cribriform lamina and the medial wall of the right orbit.
Transnasal surgical resection was planned and performed as follows by S.F. through a combined use of endoscopy and microscopy approach. Cottonoids soaked in oxymetazoline solution were positioned in the nasal cavity and left in place for ten minutes. One percent lidocaine with 1:200 000 epinephrine was subsequently injected at the level of the root of the middle turbinate and of the uncinate process.
A completely endoscopic approach was not possible because tumour bleeding precluded identification of key endoscopic landmarks. A primary microscopic resection was thus performed, assisted by the use of 0, 30 and 45 degree telescopes to assure tumour resection from recesses not visualized microscopically.
The specimen was resected “en bloc”, with care taken that the dissection was carried out in the subperiosteal plane. The intraoperative histological examination ruled out the malignant tissue. A CSF fistula was created during division the adhesions between the mass and dura mater. The fistula was repaired under endoscope vision using an overlay technique with lower turbinate graft; fibrin glue was applied to stabilize the site, which was then covered with surgical absorbable hemostatic gelatine sponge. The nasal packing was removed on the second day. The postoperative recovery period was uneventful. Blood transfusions were unnecessary. The patient was discharged three days later.
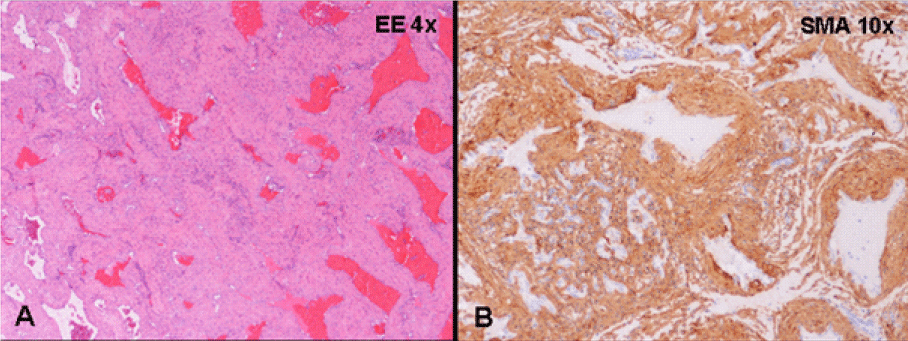
Histological examination of the mass revealed the presence of vascular formations with thick muscular wall and abundant fibrous connective stroma, with a definite diagnosis of angioleiomyoma (Figure 2).
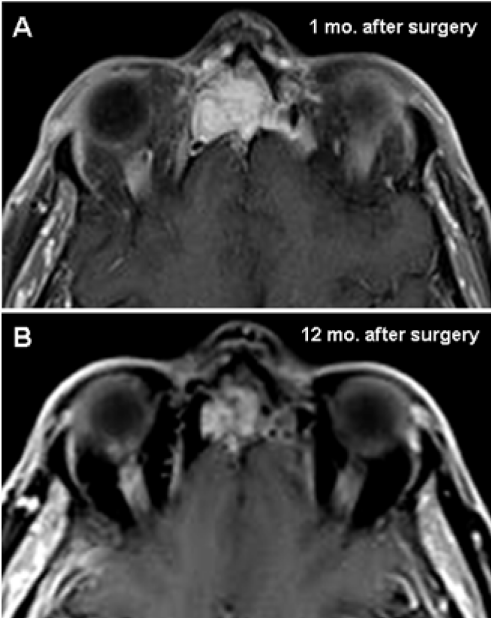
One month after surgery MRI examination showed a solid tissue located at the ethmoidal vault with post-gadolinium enhancement. At the six and twelve months follow-up MRI examination, reduction of size and of gadolinium enhancement suggested the presence of postsurgical granulation tissue with no evidence of residual tissue (Figure 3).
Discussion
We report a case of endo-scopic removal of a large naso-ethmoidal vascular leiomyoma with cortical bone disruption of the orbital and anterior cranial fossa.
Vascular leiomyomas of the nasal cavity and paranasal sinuses are extremely rare, making up less then 1% of all human leiomyomas. This rarity is partially due to the paucity of smooth muscle in the nasal cavity; three theories have been put forward for the origin of angioleiomyomas: from aberrant undifferentiated mesenchyme, from smooth muscle in the wall of blood vessels, or from both [4]. When they are in the nasal cavity, the most frequent location is the inferior turbinate [5]. Other reported sites include the nasal vestibule, within nasal polyps and from the nasal septum [6].
Histological classification of leiomyomas by the World Health Organization [1,7] includes: leiomyoma, angio-leiomyoma (vascular leiomyoma or angiomyoma) and epithelioid leiomyoma (bizarre leiomyoma and leiomyoblastoma). Angiomyomas may stem from surface or deep tissue. In both cases, the neoplasia seems to develop from the vessels’ smooth muscle [8]. Vascular leiomyomas are made up of bundles of relatively organized smooth muscle cells, permeated by thick walled vessels. The surface lesions are made mainly by thick wall vessels associated with proliferative muscle tissue. Deeper lesions are usually larger, probably because of a delay in diagnosis, and frequently present varied histological alterations which are not seen on the surface types. These alterations include an increase in cell number and build up of myxoid substance. Fibrosis, calcifications and giants cell reaction may also be observed. Morimoto (1973) classified these tumours histologically into three types: (i) capillary or solid, (ii) cavernous and (iii) venous. In the limbs, these tumours are mainly solid, while in the head and neck they are frequently of the venous type [8,9]. Histopathological differential diagnosis includes hemangioma, angiofibroma, fibromyoma, leiomyoblastoma, angiomyolipoma, vascular leiomyosarcoma [8].
There are, also, reports of malignant tumour variants of this line. Lack of mitosis seems to indicate the tumor’s benign characteristics [8]. Immunohistochemical tests have been used to identify vascular leiomyomas. These tumours grow slowly and may persist for a long time [10] as observed in our patient.
In the nasal cavity, the most frequently reported location of the vascular leiomyoma has been the inferior turbinate. According to Barr et al. [3], the high incidence of leiomyomas in the inferior turbinate may be attributed to the large local amount of contractile vascular tissue in the smooth muscle.
According to the literature, the most common symptoms are: nasal obstruction (56.25%), facial pain (25%) and headache (25%) [1,3,10- 13]. Progressive anosmia was the only clinical complaint in this case, due to the deep unusual location of the mass in our patient.
Treatment for these tumours is based on local resection, and there are no reports of recurrence after total excision [1,2,8,9].
Surgical approach by naso-sinusal endoscopic surgery or by lateral rhinotomy depends on tumour location and extension, as well as the need for a better bleeding control and surgeon’experience [1,9,10]. A preoperative CT scan is essential for the evaluation of extension to the paranasal sinuses, to look for bony erosion and to plan the most appropriate surgical approach. Our patient underwent to tumor “en bloc” removal by an endonasal combined microscopic endoscopic technique. We believe that endoscopic combined with microscopic approach allows to better achieve minimal invasiveness. The surgeon benefits from the depth-of-field and the three dimensional view magnified by the microscope. The endoscope, meanwhile, grants a close up view of the lesion and allows to inspect from the midline with the use of wide-angle lenses.
Conclusion
In cases of rare benign tumors of the naso-ethmoidal region, such as angioleiomyomas, a mini-invasive combined surgical approach avoids suffering a demolitive and disfiguring surgery as well as external scars of the facial skin.
References
- Bloom DC, Finley JC Jr, Broberg TG, Cueva RA (2001) Leiomyoma of the nasal septum. Rhinology 39: 233-235.
- Hanna GS, Akosa AB, Ali MH (1988) Vascular leiomyoma of the inferior turbinate - report of a case and review of the literature. J Laryngol Otol 102: 1159-1160.
- Barr GD, More IA, McCallum HM (1990) Leiomyoma of the nasal septum. J Laryngol Otol 104: 891-893.
- Meher R, Varshney S (2007) Leiomyoma of the nose. Singapore Med J 48: e275-e276.
- Batsakis JG (1979) Tumors of the Head and neck: Clinical and pathological considerations. (2nd edn), Baltimore: Williams and Wilkins Co., p. 354-356.
- Lijovetzky G, Zaarura S, Gay I (1985) Leiomyoma of the nasal cavity (report of a case). J Laryngol Otol 99: 197-200.
- Murono S, Ohmura T, Sugimori S, Furukawa M (1998) Vascular leiomyoma with abundant adipose cells of the nasal cavity. Am J Otolaryngol 19: 50-53.
- Nall AV, Stringer SP, Baughman RA (1997) Vascular leiomyoma of the superior turbinate: first reported case. Head Neck 19: 63-67.
- Khan MH, Jones AS, Haqqani MT (1994) Angioleiomyoma of the nasal cavity - report of a case and review of the literature. J Laryngol Otol 108: 244-246.
- Ardekian L, Samet N, Talmi YP, Roth Y, Bendet E, et al. (1996) Vascular leiomyoma of the nasal septum. Otolaryngol Head Neck Surg 114: 798-800.
- Fonseca MT, Araújo PAK, Barreiros AC (2002) Leiomyoma of the paranasal sinuses: a case report and review of the literature. Rev Bras Otorrinolaringol 68: 436-439.
- Daisley H (1987) Leiomyoma of the nasal cavity. West Indian Med J 36: 181-183.
- Sawada Y (1990) Angioleiomyoma of the nasal cavity. J Oral Maxillofac Surg 48: 1100-1101.
- Enzinger FM, Weiss SW (1983) Benign tumors in smooth muscle. In: Soft Tissue Tumors. C.V. Mosby Co., 282-285.
Citation: Casale M, Yuri E, Filomena O, Antonino I, Carla R, et al. (2012) Naso- Ethmoidal Angioleiomyoma: A Mini-Invasive Combined Endoscopic and Microscopic Surgical Approach. Otolaryngol 2:110. DOI: 10.4172/2161-119X.1000110
Copyright: © 2012 Casale M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 14552
- [From(publication date): 3-2012 - Dec 20, 2025]
- Breakdown by view type
- HTML page views: 9929
- PDF downloads: 4623