Giant Cystic Parathyroid Adenoma Masquerading as a Retropharyngeal Abscess
Received: 05-Sep-2013 / Accepted Date: 09-Jan-2014 / Published Date: 17-Jan-2014 DOI: 10.4172/2161-119X.1000154
Abstract
Objective: A case report of a retropharyngeal cystic parathyroid adenoma and a review of its embryology, differential diagnosis and management are presented.
Material and Method: A 34-year-old woman presented with a 2-year history of a right-sided discrete, cystic, submucosal cervical mass displacing the oropharynx anteriorly. MRI showed a large, cystic hyperdense mass occupying the parapharyngeal and retropharyngeal spaces. Surgical resection revealed a right-sided multinodular neck mass originating from the thyroid gland and extending along the prevertebral space and towards the contralateral neck, displacing the pharynx and larynx. Histology was consistent with a cystic parathyroidadenoma.
Discussion: Cystic parathyroid adenoma has rarely been reported and may mimic a retropharyngeal abscess. The unusual location of parathyroid tissue can be explained by its origin from ectopic superior parathyroid glands or tumor extension from parathyroid glands intothe retropharyngeal space.
Conclusion:The differential diagnosis of a retropharyngeal mass should include parathyroid tumours.
Keywords: Parathyroid adenoma, Ectopic parathyroid, Retropharyngeal space, Retropharyngeal abscess
255656Introduction
Cysts of the parathyroid glands are uncommon and account for <0.001% of neck masses [1]; less than 200 cases of cystic parathyroid adenomas have been reported [2,3]. The diagnosis is therefore unlikely to be consideredand islikely to be confused with a retropharyngeal abscess. We report a case of a giant retropharyngeal cystic parathyroid adenoma and review the pathophysiology and management of this unusual condition.
Clinical Case
A 34-year-old female presented with a 2-year history of discomfort and a foreign body-like sensation in the throat. There was no history of dysphagia or dyspnoea. Palpation revealed a non-tender right-sided neck mass which was discrete, moved with swallowing, and had normal overlying skin. A diffuse, fluctuant retropharyngeal masscovered by a healthy, non-ulcerated mucosa displaced the posterior wall of the oropharynx anteriorly. Aspiration yielded 120 ml of thick, sticky, chocolate-brown fluid following which there was partial resolution of the mass. Bacteriological and cytologic examinations of the fluid were unremarkable.
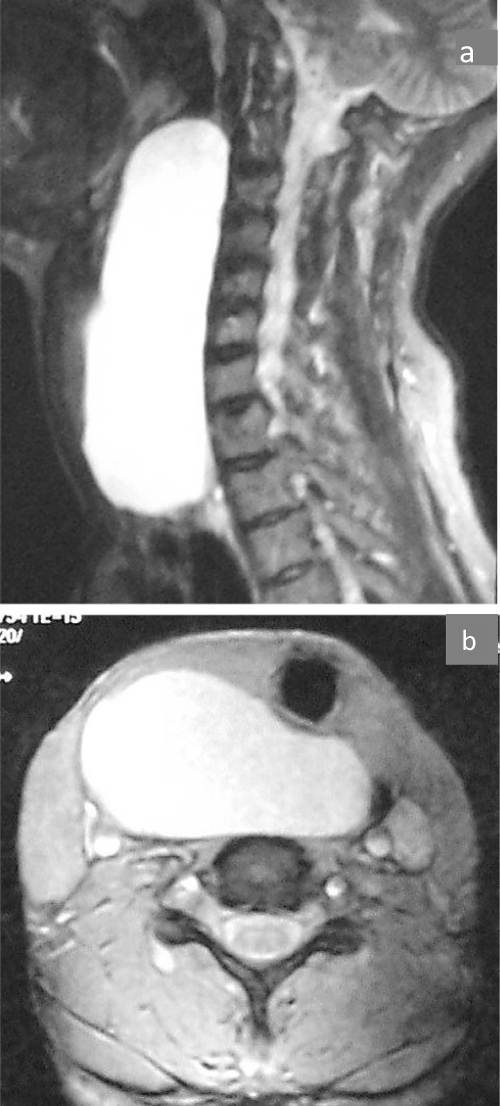
Six weeks later the patient represented with discomfortand partial obstruction of the oropharynx due to recurrence of the retropharyngeal mass. MRI revealed a large; hyperdense cystic mass occupying the right parapharyngeal and retropharyngeal spaces with significant mass effect whichdisplaced the larynx and pharynx anteriorly (Figures 1a and b).
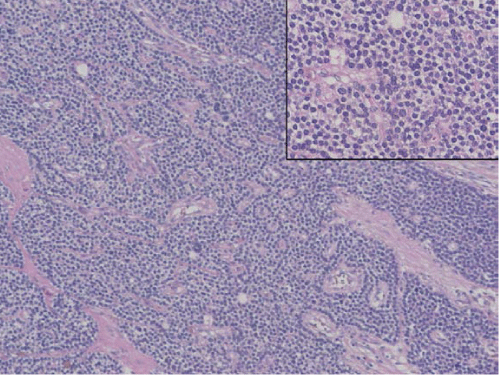
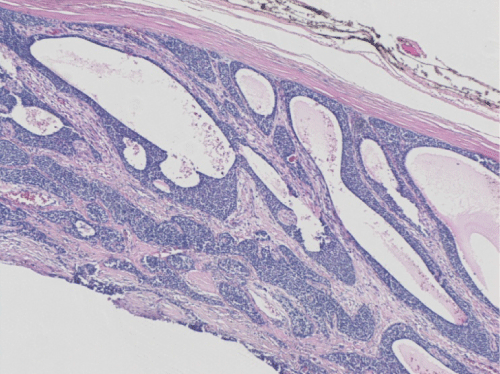
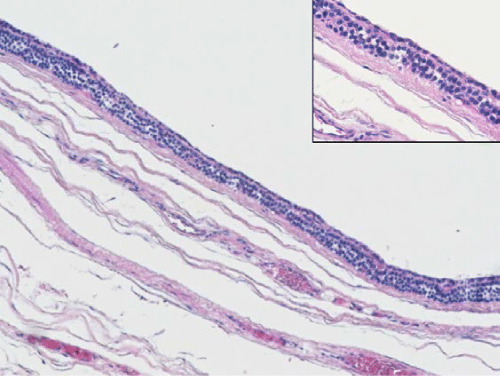
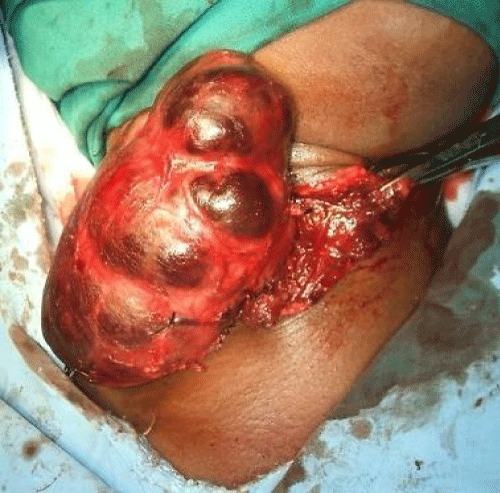
Transcervical surgical exploration yielded a slightly vascular, thinly encapsulated,nodular mass. It measured10cm in length and was situated behind the visceral compartment of the neck i.e. behind the trachea and esophagus. It involved the right lobe of the thyroid, and extended superiorly along the prevertebral space. A right thyroid lobectomy was done without difficulty, with delivery of the superior pole of the tumor by finger dissection. Histological examination of the surgical specimen was consistent with a cysticparathyroid adenoma. Macroscopic examination of the surgical specimen showed an encapsulated multiloculated cystic lesion with focal solid areas and adjacent thyroid tissue. Histological examination confirmed an encapsulated lesion composed predominantly of a cystic component with peripheral solid areas.The solid areas consisted of sheets, nests, and cords of regular cells with pale granular cytoplasm and regular round nuclei (Figure 2a). In addition, focal microscopic nodules of larger cells with water clear cytoplasm were present. Mitotic figures and necrosis was not seen. Some of the solid sheets and islands showed central cystic degeneration (Figure 2b). The large cyst was lined by similar regular small cells (Figure 2c). There was evidence of recent and old haemorrhage. Adjacent thyroid tissue was present. The histopathological features were those of a cystic parathyroid adenoma.
Discussion
Astriking feature of this parathyroid mass was its extension to the retropharynx. The retropharyngeal space is a virtual space comprising fat and lymphoid elements. It is more commonly the seat of infections such as retropharyngeal abscesses, including cervical Pott’s disease (tuberculosis), or tumors lymphoma, or lymph node metastases from papillary and anaplastic cancers of the thyroid [4]. Causes of retropharyngeal cysts are listed in Table 1 [5,6].
| Inflammatory | Retropharyngeal abscess (bacterial) Pott's disease (tuberculosis) Hydatid cyst |
| Miscellaneous | Hemangioma Thyroid cyst Papillary carcinoma of thyroid Parathyroid cyst 3rd Branchial cyst [5] Ectopic thymus [6] Cystic lymphangioma Bronchogenic cysts |
Table 1: Causes of retropharyngeal cysts.
Non-functioning parathyroid adenomassuch as was found in our case are very rare; hypotheses found in the literature include:
- Tissue necrosis secondary to cystic degeneration
- “Autoparathyroidectomy” or “parathyroid apoplexy” caused by haemorrhage and infarction; this has to be supported by histopathological evidence of necrosis and degeneration of the adenoma. Generally the haemorrhage is spontaneous [7,8], but may be provoked by multiple needle punctures
- Pressure from ahaematoma causing ischaemia [9,10]
- Rapid growth leading to vascular insufficiency and infarction [11]
- Parathyroid Hormone (PTH) secreted into the lumen of the cyst instead of into the blood stream
The parathyroid cyst in our case is likely to have originated from an ectopic parathyroid gland located either within the retropharynx or intrathyroidally, or may have represented an extension of a large tumour of a normally situated parathyroid gland. Ectopic superior parathyroids are uncommon (1%) and may be found in the posterior neck, retropharyngeal and retroesophageal spaces and intrathyroidally [4,12]. The superior parathyroid glands originate from the 4th pharyngeal pouch. They adhere to the posterior surface of the caudally migrating thyroid. As the larger thymus and thyroid gland migrate from the upper neck into the lower neck and upper chest, they carry the “small passenger” parathyroids with them. The superior parathyroid glands have a much shorter distance to migrate than the inferior parathyroids; this might account for their more predictable location. The superior parathyroids are usually found posteriorly at the level of the upper two thirds of the thyroid gland, about 1 cm above the point where the Recurrent Laryngeal Nerve (RLN) crosses the inferior thyroid artery and are embryologically and anatomically closely related to the Tubercle of Zuckerkandl. The superior parathyroid gland may be trapped within the thyroid parenchyma; this would explain why intrathyroid ectopic superior parathyroids account for 5% of ectopic parathyroids [4,13,14]. In our case, a nodular enlargement of the right thyroid lobe was discovered during surgical exploration and was the reason for doing a right hemithyroidectomy (Figure 2). The pathologists did not indicate the presence or absence of a parathyroid capsule; hence it is not possible to state unequivocally whether it was indeed an intrathyroidal parathyroid adenoma. Other pathological locations of ectopic parathyroid tissue have been reported i.e. posterior mediastinum [15], retrosternally in the anterior mediastinum within the thymus, in the carotid sheath, in the vagus nerve, the pericardium and also in the retrotracheal space [10,15]. Miller et al. [9] also described ectopic parathyroid glands located submucosallyinthe piriform sinus. He reported that in 1200 cervical explorations of parathyroid glands done over 58 years, 0.08%was situated in retropharyngeal space. An embryological explanation is the failure of the superior parathyroid gland to separate from the piriform sinus during its transcervical migration. According to Foroulis and Somparaoesophageal or retrooesophageal parathyroid tumours originating from the superior parathyroid gland should embryologically have a normal blood supply from a branch of inferior thyroid artery [15,16].
Knowledge of the anatomical spaces of the neck is needed to understand the pathophysiology of retropharyngeal extension of parathyroidand thyroid tumours [16,17]. The pretracheal, retrooesophageal and retropharyngeal spaces are a continuum [1,3]; this explains the extension of a large retropharyngeal thyroid or parathyroid into these spaces. Tahim [18] reported a case of a cystic parathyroid adenoma that extended into the mediastinum. The thyroid compartment is located in the anterior and inferior parts of the neck and overlies the tracheal rings; the thyroidcapsule is formed by the deep layer of the deep cervical fascia or visceral layer of the pretracheal fascia and is limited posteriorly and laterally by the visceral and vascular axes of the neck respectfully. Anteriorly it is covered by strap muscles, which in turn arecovered by the middle layer of deep cervical fascia. The muscular layer of the pretracheal fascia is limited superiorly by the inferior edge of the hyoid bone.This visceral compartmentincludes the thyroid gland, parathyroid gland, trachea and oesophagus. Superior and anterior extension is hindered by the attachment of the pretracheal fascia to the hyoid bone. The retrovisceral space is a single virtual space that extends laterally around the larynx and trachea and joins pretracheal space. Itstretches from the base of the skull to the posterior mediastinum at the tracheal bifurcation. Behind the pharynx it is called the retropharyngeal space; behind the oesophagus it is called the retrooesophageal space.
The clinical diagnosis of a cystic parathyroid adenoma is often missed especially when the parathyroid adenoma is non-functional as in our case [19]. Our patient presented with symptoms of dyspnoea following haemorrhage into a cervical cystic parathyroid adenoma, as has been previously described [8]. Other clinical signs associated with a cervical cystic parathyroid adenoma may include primary hyperparathyroidism [1,15], manifesting as hypercalcemia and even multiple organ failure; parathyroid crisis complicating hyperparathyroidism, also called acute hyperparathyroidism or parathyroid intoxication or parathyrotoxicosis are also reported in the literature [18]. Although it may be negative, Sestamibiscan is the gold standard for making a diagnosis of a parathyroidadenoma;CT and MRI are not 1st line investigations as their accuracy is too poor [9,20].
Conclusion
The diagnosis of a non-functional cystic parathyroid adenoma can be confusing especially when in a retropharyngeal position. Delimitations and connections between the neck spaces explain why such cases may be confused with other causesof retropharyngeal masses.PTH and calcium levels should be included in the diagnostic workup of cervical masses whenthe diagnosis is unclearin order to exclude parathyroid aetiology.
• Retropharyngeal cystic parathyroid adenomas can mimic a retropharyngeal abscess
• Cystic non-functional parathyroid adenomas are rare and may result for haemorrhage in a parathyroid gland and rapid growth of an adenoma
• Diagnostic workup of cervical masses of uncertain aetiology should include serum PTH and calcium levels to exclude parathyroid aetiology
Tc-sestamibiscintigraphy is the gold standard for diagnosing ectopic parathyroid adenomas.
References
- Asghar A, Ikram M, Islam N (2012) A case report: Giant cystic parathyroid adenoma presenting with parathyroid crisis after Vitamin D replacement. BMC Endocr Disord 12: 14.
- Jha BC, Nagarkar NM, Kochhar S, Mohan H, Dass A (1999) Parathyroid cyst: a rare cause of an anterior neck mass. J Laryngol Otol 113: 73-75.
- Davies ML, Middleton SB, Mellor SG (2002) Mistaken Identity: Cystic parathyroid adenoma masquerading as goitre. The Internet Journal of Surgery 3.
- Lezrek M, Kabiri H, Al Bouzidi A, Sair K, Rachid K, Benomar S, et al. (1997) Glande parathyroide intra-thyroidienne. Médecine Du Maghreb 62:61.
- Huang RY, Damrose EJ, Alavi S, Maceri DR, Shapiro NL (2000) Third branchial cleft anomaly presenting as a retropharyngeal abscess. Int J Pediatr Otorhinolaryngol 54: 167-172.
- Meyer E, Mulwafu W, Fagan JJ, Brown RA, Taylor K (2010) Ectopic thymic tissue presenting as a neck mass in children: a report of 3 cases. Ear Nose Throat J 89: 228-231.
- Taniguchi I, Maeda T, Morimoto K, Miyasaka S, Suda T, et al. (2003) Spontaneous retropharyngeal hematoma of a parathyroid cyst: report of a case. Surg Today 33: 354-357.
- Shim WS, Kim IK, Yoo SD, Kim DH (2008) Non-functional parathyroid adenoma presenting as a massive cervical hematoma: a case report. Clin Exp Otorhinolaryngol 1: 46-48.
- Miller DL, Craig W, Haine GA (1997) Retropharyngeal parathyroid adenoma: Precise preoperative localization with CT and arterial infusion of contrast material. Am J Roentgenol 169: 695-696.
- Wang CA (1977) Parathyroid re-exploration. A clinical and pathological study of 112 cases. Ann Surg 186: 140-145.
- Efremidou EI, Papageorgiou MS, Pavlidou E, Manolas KJ, Liratzopoulos N (2009) Parathyroid apoplexy, the explanation of spontaneous remission of primary hyperparathyroidism: a case report. Cases J 2: 6399.
- Panieri E, Fagan JJ. Parathyroidectomy: The Open Access Atlas of Otolaryngology, Head and Neck Operative Surgery.
- Korukluoglu B, Kiyak G, Celik A et al. (2008) Our surgical approach to parathyroid adenoma and the role of localization studies Turk Clin J Med Sci 28: 24-29.
- Korukluoglu B, Ergul E, Yalcin S (2008) Giant intrathyroidal parathyroid cystic adenoma. J Pak Med Assoc 58: 592.
- Foroulis CN, Rousogiannis S, Lioupis C, Koutarelos D, Kassi G, et al. (2004) Ectopic paraesophageal mediastinal parathyroid adenoma, a rare cause of acute pancreatitis. World J Surg Oncol 2: 41.
- Som PM, Shugar JM (1991) Retropharyngeal mass as a rare presentation of a goiter: CT findings. J Comput Assist Tomogr 15: 823-825.
- Shamim M (1978) Retropharyngeal goitre. J R Coll Surg Edinb 23: 367-368.
- Tahim AS, Saunders J, Sinha P (2010) A parathyroid adenoma: benign disease presenting with hyperparathyroid crisis. Case Rep Med 2010: 596185.
- Sekine O, Hozumi Y, Takemoto N, Kiyozaki H, Yamada S, et al. (2004) Parathyroid adenoma without hyperparathyroidism. Jpn J Clin Oncol 34: 155-158.
- Wieneke JA, Smith A (2008) Parathyroid adenoma. Head Neck Pathol 2: 305-308.
Citation: Diom ES, Fagan JJ, Govender D (2014) Giant Cystic Parathyroid Adenoma Masquerading as a Retropharyngeal Abscess. Otolaryngology 4:154. DOI: 10.4172/2161-119X.1000154
Copyright: © 2014 Diom ES, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15574
- [From(publication date): 2-2014 - Jul 02, 2025]
- Breakdown by view type
- HTML page views: 10948
- PDF downloads: 4626