Guide Wire Augmented Nasofrontal Sinusotomy (GWANS)
Published Date: 04-Mar-2014 DOI: 10.4172/2161-119X.1000162
Abstract
Endoscopic frontal sinus surgery remains as a very challenging technique with potential for serious morbidity and even mortality. The close proximity of orbital contents, the cribriform plate and the anterior skull base pose serious challenges in performing this operation safely. The frontal recess anatomy is even more treacherous in recurrent cases and in diseased processes such as polyps and other tumors blocking the nasofrontal recess.
Guide Wire Augmented Nasofrontal Sinusotomy (GWANS) allows for real time surgical guidance allowing the surgeon to confidently dissect through diseased tissue knowing all along where the boundaries of the nasofrontal recess lies and thus avoid injuring vital structures. This is a new and adjunctive tool for augmenting the standard endoscopic nasofrontal sinusotomy technique.
Keywords: Endosocopic frontal sinus surgery, Minimally invasive frontal sinus surgery, Guide-wire assisted frontal sinus surgery, Balloon assisted frontal sinus surgery
246165Introduction
Since 1985 Functional Endoscopic Sinus Surgery (FESS) has become the gold standard in surgical management of intractable sinusitis in the United States [1-3]. Over 200,000 FESS cases are performed in the US on an annual basis, surgical success rates are reported as high as 98% for isolated maxillary disease and relatively lower success rates are reported for Ethmoid and sphenoid disease [4].
Frontal sinus recess is the most difficult area to dissect endoscopically, and the lowest success rates are quoted for the intractable frontal sinus disease [5-7]. Post-operative failure after frontal sinus surgery is often due to retained or residual diseased cells in the frontal recess [8]. This may be due to difficulty in surgical dissection and the surgeon’s uncertainty of anatomical landmarks thus leaving disease behind.
Frontal sinus anatomy remains difficult and elusive, especially in recurrent disease and cases with polyps or other neoplasm in the frontal recess. Complicated frontal recess anatomy with potential risk of serious complications to the orbit or the brain, in combination with the surgeon’s lack of anatomical confidence may lead to residual disease at the frontal recess.
Stereotactic Sinus Navigation has provided much improved surgical guidance, but it remains to be based on a pre-operative static CT scan and not real time imaging. However, ongoing surgical dissection can alter the observed anatomy on a real time basis and distort boundaries seen on a pre-operative navigational CT scan. It appears that computer guided sinus surgery may not necessarily improve clinical outcome, but it may reduce surgical complication rates [9,10].
In order to overcome the lack of real time data during computer assisted surgical dissection, other investigators have suggested the use of intra-operative volume controlled computed tomography scans. There seems to be a positive promise for this technique; however it is time consuming, cumbersome in the cramped operating rooms and very costly [11].
Guide Wire Augmented Nasofrontal Sinusotomy is a new and novel method that allows for a fast and relatively simple surgical guidance in a very difficult anatomy. It allows surgeon to clean disease process and widen the frontal recess with more confidence knowing where the recess is located and to avoid injuring adjacent vital structures. This method can be used on all difficult primary or revision frontal sinus cases where the nasofrontal recess anatomy is abnormal or is obscured by polyps, granulation tissue or scar tissue.
Method
Standard Endoscopic sinus surgery instruments were utilized. The fiberoptic Luma Guide wire assembly from the Acclarent Company of Menlo Park, California was used for all the cases in this study [12]. In all cases, the three dimensional LandMarx Navigation CT Scan, Stealth protocol, from Medtronic Company of Minneapolis, Minnesota were utilized [13].
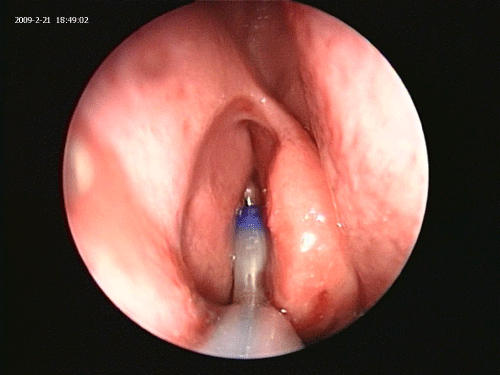
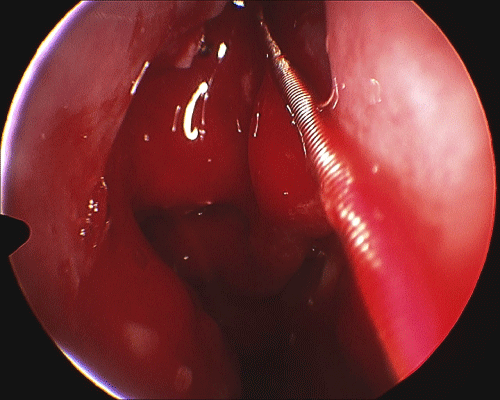
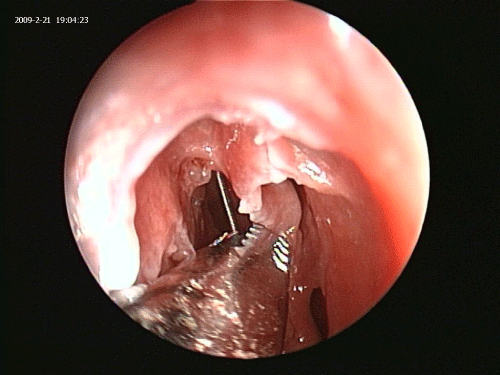
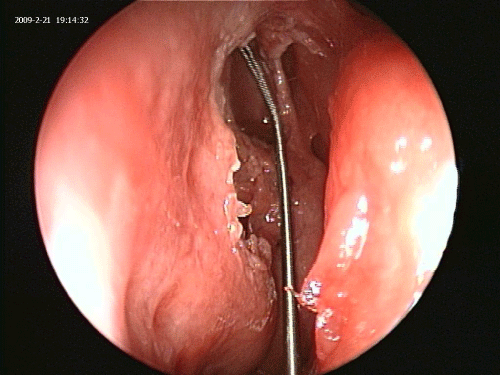
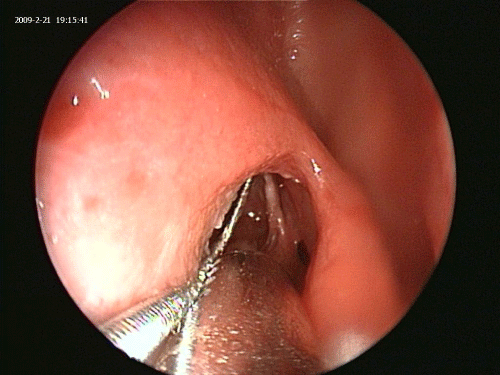
The fiberoptic Luma guide wire is inserted under direct endoscopic visualization using a 45 degree Sinus Endoscope and a 70 degree frontal catheter guide. This can be accomplished in great majority of Polypoid and scarred recesses even where there is no visualization of an opening into the recess (Figures 1 and 2).
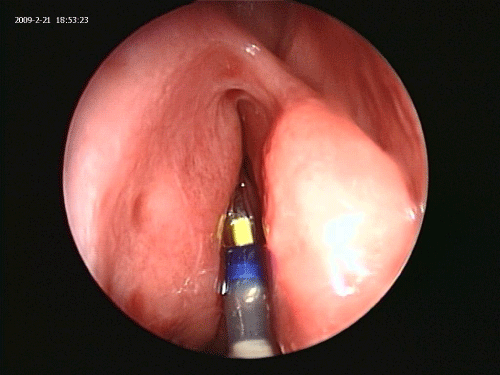
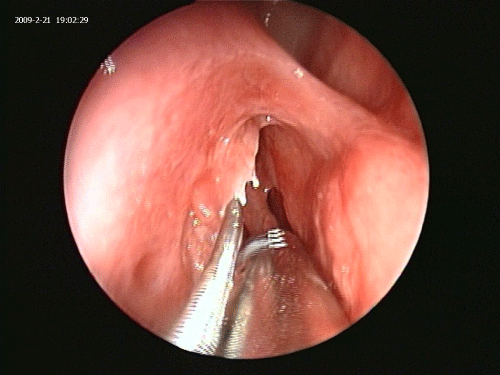
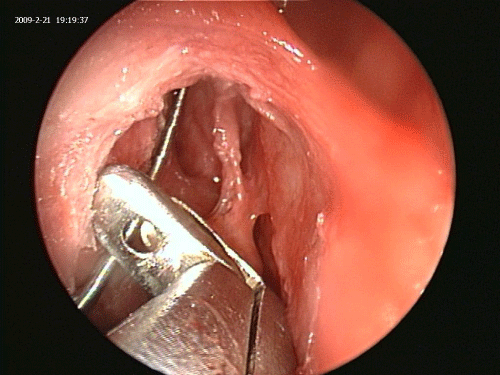
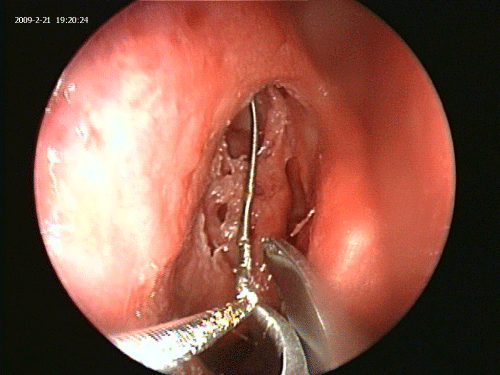
Operative room lights are dimmed to a minimum. Endoscopy light source is dimmed. Patient’s forehead is scanned for the light reflection of the Luma guidewire (Figure 3). Once the location of the guide wire tip in the frontal sinus is confirmed via transillumination of the frontal sinus, a 7 by 24 ml frontal dilation balloon is inserted over the guide wire and inflated in the nasofrontal recess to 10 atmospheric pressure for one second (Figure 4) [13].
On all cases, once the forehead transillumination was confirmed, the navigational image guidance also confirmed the accurate positioning of the guide wire in the naso frontal recess.
The most important part of the GWANS technique is to carefully remove the balloon along with the catheter guide, but leaving the guide wire in place. In order to make sure the guide wire stays in place during the dissection, the surgical assistant holds the guide wire in place and keeps the frontal sinus transillumination in the same spot on the forehead throughout the procedure.
With the guide wire left in the nasofrontal recess all the way into the frontal sinus, the surgeon then proceeds with the standard endoscopic resection of the uncinate process, the agar nasi cells, polyps, obstructing frontal bony spurs/beak and granulation tissue thus enlarging the recess with full view of the guide wire at all times (Figures 5-7) [14,15].
Once the frontal recess is widely opened up, the Vortex Irrigation catheter from the Acclarent Company was inserted over the guide wire into the frontal sinus. Aspiration for culture and saline irrigation was then performed on all sinuses.
Guide wire’s tensile strength test in the laboratory
The Fiberoptic Luma Guide wire was also tested for strength in the cadavers in the laboratory. The concern was that could the surgeon accidently cut the Guide wire during surgery using sharp instrumentations, such as the microdebrider, cutting forceps or scissors. The test was conducted in the cadaver laboratory to assess the Fiberoptic Luma Guide wire’s tensile strength and resistance to fragmentation when faced with sharp cutting instruments. Multiple deliberate attempts to grab the wire with cutting forceps, even scissors, failed to transect the guide wire. Microdebrider and high-speed sinus drills also were unable to grab and transect the guide wire. After over 20 such deliberate attempts on a single wire, the Guide wire was bent and damaged but it still conducted light and did not transect. Multiple Luma Guide wires were tested in a similar fashion; none could be transected in vivo while staying in the nasofrontal recess. The laboratory data proved that the Luma Guide wire was relatively safe around cutting instruments, microdebrider (shaver) and drills (Figures 8-11).
Cases
Eighteen (18) patients with difficult, intractable frontal sinusitis were treated with this method over a 15 month period with a minimum of 3 month post-operative CT scan and office endoscopy. Thirty four (34) frontal sinuses were operated upon. Pre-operative CT Scans and infrared Image Guidance system was used on all patients. Only fiberoptic Luma Guide Wire was used. Fluoroscopy was not utilized. All patients were adults, age range of 36-67 years old. All cases were performed under general anesthesia using mild hypotension maintaining the systolic blood pressure around 90 mmHg. Intravenous antibiotic and Dexamethasone were used on all patients at the induction of general anesthesia (Table 1).
| Case No. | Age | Sex | Stage | Disease Status |
|---|---|---|---|---|
| 1 | 52 | M | Revision | Polyps, scar tissue |
| 2 | 46 | M | Revision | Polyps, bony narrowing |
| 3 | 36 | F | Primary | Polyps, small aggernasi |
| 4 | 60 | M | Revision | Polyps, Granulation tissue |
| 5 | 62 | F | Primary | Low uncinate, stenotic NFR |
| 6 | 36 | M | Revision | Polyps, scar tissue |
| 7 | 40 | M | Revision | Scar tissue, lateralized middle turbinate |
| 8 | 49 | F | Primary | Scar tissue, small aggernasi |
| 9 | 49 | M | Revision | Polyps, no middle turbinates, scar tissue |
| 10 | 37 | F | Primary | Polyps, granulation tissue |
| 11 | 58 | F | Revision | Polyps, scar tissue |
| 12 | 34 | M | Revision | Polyps, no landmarks, scarred uncinate |
| 13 | 44 | F | Primary | Polyps, granulation tissue |
| 14 | 44 | M | Revision | Inverted Papilloma in the frontal recess |
| 15 | 49 | M | Revision | Scar tissue, small aggernasi |
| 16 | 54 | M | Revision | Polyps, no landmarks, scarred uncinate |
| 17 | 55 | F | Revision | Polyps, granulation tissue |
| 18 | 67 | M | Revision | Polyps, granulation tissue |
Table 1: Case distribution.
Results
In all but two cases out of thirty two sinuses, the frontal sinus recesses were successfully entered using the Fiberoptic Luma Guide wire. Once the guide wire was in place, standard endoscopic resection of the obstruction was performed for a wide open naso frontal recess in all cases. There were no complications. There was no entry into the orbit or the intracranial structures and no cases of Ethmoid artery violation.
The two unsuccessful Guide wire cases demonstrated complete bony stenosis where there was no detectable opening for the guide wire to pass, thus requiring standard frontal sinusotomy techniques [16-18]. Even in these two initially unsuccessful Guide-Wire cases, once the recess was partially opened, the Guide wire was passed into the sinus and dissection of the bony disease continued around the Guide wire thus increasing the surgeon’s confidence of the location of the recess into the frontal sinus at all times.
All frontal sinuses showed significant improvement in the degree of mucosal thickening on the post-operative CT Scans as compared to the pre-operative scans. Twenty Six sinuses (80%) showed relatively clear frontal sinuses with less than 3 mm mucosal thickening on the three month post-operative CT Scan. The remaining 20% showed significant reduction in the mucosal thickening. None of the pre-operatively opacified frontal sinuses remained opacified post-operatively thus demonstrating either partial or complete aeration of the frontal sinus (Table 2).
| Case No. Score | Pre-op Right Score | Post-op Right LM | Pre-op Left Score | Post –op Left score |
|---|---|---|---|---|
| 1 | 2 | 1 | 2 | 1 |
| 2 | 2 | 0 | 2 | 0 |
| 3 | 1 | 0 | 1 | 0 |
| 4 | 2 | 0 | n/a | unilateral |
| 5 | 1 | 0 | 1 | 0 |
| 6 | 2 | 1 | 2 | 0 |
| 7 | 2 | 0 | 1 | 1 |
| 8 | 1 | 0 | 1 | 0 |
| 9 | 2 | 0 | 2 | 0 |
| 10 | 1 | 0 | 1 | 0 |
| 11 | 2 | 0 | n/a | unilateral |
| 12 | 2 | 0 | 2 | 1 |
| 13 | 1 | 0 | 1 | 0 |
| 14 | 2 | 0 | 2 | 0 |
| 15 | 2 | 0 | 2 | 0 |
| 16 | 2 | 0 | 2 | 0 |
| 17 | 2 | 0 | 2 | 1 |
| 18 | 2 | 1 | 2 |
Table 2: Pre-operative and Post-operative Lund-MacKay sinus CT Staging.
Discussion
Frontal sinus disease remains mostly a medical disease. Surgical intervention is best reserved for intractable and symptomatic frontal sinusitis [6]. Effective antibiotics and vigilant adjunctive remedies to improve sinus drainage have substantially reduced the need to perform frontal sinus surgery. Nevertheless, frontal sinus surgery remains a very challenging and difficult undertaking with potential for serious lifechanging complications [19].
Abnormal frontal recess anatomy, with or without obstructing polyps or bony obstruction, can further complicate the surgical access into the frontal sinus and increase the risk of serious complications. As surgeons and healers, our primary job is to do no harm. Frontal sinus surgery is designed to improve patients’ quality of life, but it could lead to severe loss of function and morbidity.
Balloon dilation of the frontal recess has been shown to be an effective and safe method for intractable frontal sinus disease [20,21]. Long term frontal sinus outflow tract patency after balloon dilation of the frontal recess has been shown to be in the same range of the standard non-balloon surgical debridement of the frontal recess [22].
The Guide-Wire Augmented Nasofrontal Sinusotomy (GWANS) technique can be applied to uncomplicated primary as well as the difficult primary or the revision cases. However, in uncomplicated primary cases of intractable frontal sinusitis, straightforward guide wire balloon dilation without surgical debridement may suffice in the majority of cases. It is best to reserve GWANS for those difficult cases where the fiberoptic wire is unable to enter the frontal sinus on multiple attempts [7].
In difficult cases where the frontal recess is not overtly visible, the small 1 mm fiberoptic Luma Guide wire almost miraculously finds its way into the frontal sinus with a high degree of probability. Once the wire is in place the surgeon can then proceed with balloon dilation and subsequent standard endoscopic frontal sinusotomy [23,24].
The Guide-Wire Augmented Nasofrontal Sinusotomy (GWANS) as described hereby is utilized primarily in difficult cases where either scar tissue, polyps or granulation tissue with or without bony spurs are obstructing the nasofrontal recess thus necessitating a full nasofrontal sinusotomy. In such difficult cases, polyps or bony obstruction have to be physically removed, and balloon dilation alone may not be sufficient to assure long-term patency of the nasofrontal recess.
The Guide-wire and the subsequent balloon dilation provide a solid framework where standard endoscopic frontal sinusotomy can be accomplished with ease and the safety of knowing where exactly the pathway into the frontal sinus is located throughout every step of the procedure.
The Guide-wire Augmented Nasofrontal Sinusotomy significantly reduces the need to use navigational instruments during the case. For the purpose of this study navigational Image guidance was used in all cases to confirm the location of the guide wire with the transillumination light reflex. On all cases, once the transillumination was confirmed, the navigational image guidance also confirmed the accurate positioning of the guide wire in the naso frontal recess. It is felt that with good transillumination, minimal to no navigational data is necessary in order to complete the Guide-Wire Augmented Nasofrontal Sinusotomy.
Keeping the guide wire in view during the dissection in the recess allows the surgeon real time surgical guidance to avoid injuring vital structures around the recess. This is accomplished by keeping the guide wire in the posterior plane of dissection and only removing obstructing tissues anterior to the guide wire. By keeping the dissection anterior to the guide wire, the more sensitive areas such as the Anterior Ethmoid artery and the skull base are mostly kept away from “harm”.
In two out of 18 patients the nasofrontal recess could not be “intubated” with the guide wire, and a formal frontal recess drill out was needed. It is important to remember that Guide wires and Balloons are only surgical tools for getting the job done, and the surgeon needs to be well-versed on the difficult anatomy and be fully prepared to perform the standard nasofrontal surgical techniques as indicated should the guide wire fail to perform as expected.
It is important to remind ourselves that most of the time frontal sinusitis is not life threatening, but the surgical complications of frontal sinus surgery are definitely life threatening. Cerebrospinal fluid leaks, meningitis, brain abscess, brain hematomas, eye muscle injury, blindness and death are all potential complications of frontal sinus surgery.
It is the goal of this paper to present a relatively straight forward technique for improving the odds of obtaining a good frontal sinus pathway with significant reduction of uncertainty during surgical dissection. The risks of frontal sinus surgery remain with us no matter how we do this difficult operation, but this simple guide wire gives the surgeon a great deal of confidence as to the location of the recess during the surgical debridement of the recess.
The ultimate responsibility rests with the surgeon to master the anatomy and for accomplishing the desired task with the utmost precision and skill while utilizing all available means to insure patient safety and satisfactory outcome. Guide-Wire Augmented Nasofrontal Sinusotomy is one small step towards achieving this goal in frontal sinus surgery.
References
- Messerklinger W(1985)Endoskipische diagnose and chirurgie der rezidivierenden sinusitis. In: Advances in Nose and Sinus Surgery, edited by Z. Krajina, Zagreb Universtity, Zagreb, Yugoslavia.
- Stammberger H (1985) Endoscopic surgery for mycotic and chronic recurring sinusitis. Ann OtolRhinolLaryngolSuppl 119: 1-11.
- Stammberger H (1986) Endoscopic endonasal surgery--concepts in treatment of recurring rhinosinusitis. Part II. Surgical technique. Otolaryngol Head Neck Surg 94: 147-156.
- Huang BY, Lloyd KM, DelGaudio JM, Jablonowski E, Hudgins PA (2009) Failed endoscopic sinus surgery: spectrum of CT findings in the frontal recess. Radiographics 29: 177-195.
- Levine HL (1995) Endoscopi c Sinus Surgery: reasons for failure. Op Tech Otolaryngol. Head & Neck Surg6:176-179.
- Kennedy DW, Senior BA (1997) Endoscopic sinus surgery. A review. OtolaryngolClin North Am 30: 313-330.
- Stammberger H, Posawetz W (1990) Functional endoscopic sinus surgery. Concept, indications and results of the Messerklinger technique. Eur Arch Otorhinolaryngol 247: 63-76.
- Kuhn FA (1996) Chronic Frontal Sinusitis: the endoscopic frontal recess approach. Operative techniques. Otlaryngolo Head Neck Surg 7:222-229.
- Tschopp KP, Thomaser EG (2008) Outcome of functional endonasal sinus surgery with and without CT-navigation. Rhinology 46: 116-120.
- Masterson L, Agalato E, Pearson C (2012) Image-guided sinus surgery: practical and financial experiences from a UK centre 2001-2009. J LaryngolOtol 126: 1224-1230.
- Batra PS, Kanowitz SJ, Citardi MJ (2008) Clinical utility of intraoperative volume computed tomography scanner for endoscopic sinonasal and skull base procedures. Am J Rhinol 22: 511-515.
- Acclarent, Inc. 1525-B O’Brien Drive, Menlo Park, CA 94025, USA
- Medtronic, Inc., 710 Medtronic Parkway, Minneapolis, MN 55432-5604, USA
- Bolger WE, Brown CL, Church CA, Goldberg AN, Karanfilov B, et al. (2007) Safety and outcomes of balloon catheter sinusotomy: a multicenter 24-week analysis in 115 patients. Otolaryngol Head Neck Surg 137: 10-20.
- Levine HL, Sertich AP 2nd, Hoisington DR, Weiss RL, Pritikin J; PatiENT Registry Study Group (2008) Multicenter registry of balloon catheter sinusotomy outcomes for 1,036 patients. Ann OtolRhinolLaryngol 117: 263-270.
- Wormald PJ (2008) Surgical Approach to the Frontal Sinus and Frontal Recess. In: Endoscopic Sinus Surgery, Anatomy, Three-Dimensional Reconstruction, and Surgical Technique. (2nd Edn), Thieme Medical Publishers,New York.
- Wormald PJ (2005) Surgery of the frontal recess and frontal sinus. Rhinology 43: 82-85.
- Wormald PJ (2002) The axillary flap approach to the frontal recess. Laryngoscope 112: 494-499.
- Plaza G, Eisenberg G, Montojo J, Onrubia T, Urbasos M, et al. (2011) Balloon dilation of the frontal recess: a randomized clinical trial. Ann OtolRhinolLaryngol 120: 511-518.
- Catalano PJ, Payne SC (2009) Balloon dilation of the frontal recess in patients with chronic frontal sinusitis and advanced sinus disease: an initial report. Ann OtolRhinolLaryngol 118: 107-112.
- Batra PS, Ryan MW, Sindwani R, Marple BF (2011) Balloon catheter technology in rhinology: Reviewing the evidence. Laryngoscope 121: 226-232.
- Chan Y, Melroy CT, Kuhn CA, Kuhn FL, Daniel WT, et al. (2009) Long-term frontal sinus patency after endoscopic frontal sinusotomy. Laryngoscope 119: 1229-1232.
- Schaefer SD, Close LG (1990) Endoscopic management of frontal sinus disease. Laryngoscope 100: 155-160.
- Wormald PJ (2003) Theaggernasi cell: the key to understanding the anatomy of the frontal recess. Otolaryngol Head Neck Surg 129: 497-507.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 15962
- [From(publication date): 5-2014 - Aug 24, 2025]
- Breakdown by view type
- HTML page views: 11261
- PDF downloads: 4701