Maxillary Antrostomy in a Boy to Prevent Silent Sinus Syndrome Evolution
Received: 11-Nov-2013 / Accepted Date: 02-Dec-2013 / Published Date: 10-Dec-2013 DOI: 10.4172/2161-119X.1000151
Abstract
The Silent Sinus Syndrome (SSS) is a quite rare idiopathic clinical condition characterized by atelectasis/hypoplasia of the maxillary sinus which outlines a subclinical chronic maxillary sinusitis. This framework therefore causes some ipsilateral eyepieces alterations, such as silent and progressive enophtalmos and hypoglobus that may be associated with visual changes; in all cases the medical history is negative for previous facial trauma and sinonasal or maxillofacial surgery. Montgomery (1964), Wilkins and Kulwin (1981) described some cases of spontaneous and monolateral enophtalmos and hypoglobus with diplopia and ptosis caused by pauci or asymptomatic maxillary sinus disease. The term Silent Sinus Syndrome was used for the first time 30 years later by Soparkar and co. in the ophthalmic literature. Rose and co. use instead the term “imploding antrum syndrome” to emphasize the concept that a chronic sinus condition may lead in a relatively brief period to ocular signs. This study refers the case of an 11-year old boy affected by SSS.
Keywords: Silent sinus syndrome, Pedriatic maxillary sinusitis, Atelectasis/hypoplasia of maxillary sinus, Ennophtalmos
255480Case Presentation
We report an 11 year old boy affected by chronical nasal obstruction resistant to medical therapy. Nasal endoscopy evaluation highlighted adenoidal hypertrophy and abnormal findings in the right nasal cavity: lateralization of the medial wall of the maxillary sinus, occlusion of the ostio-meatal complex, hypertrophy of the lower and middle turbinates. The left nasal cavity was normal. The CT scan images showed:
– Enlargement of the right orbital cavity
– a hypoplastic right maxillary sinus
– a lateralization of the medial maxillary sinus wall
– a thickening of the floor of the right maxillary sinus
– an hypertrophy of the middle and lower ipsilateral turbinates
– a marked adenoid hypertrophy
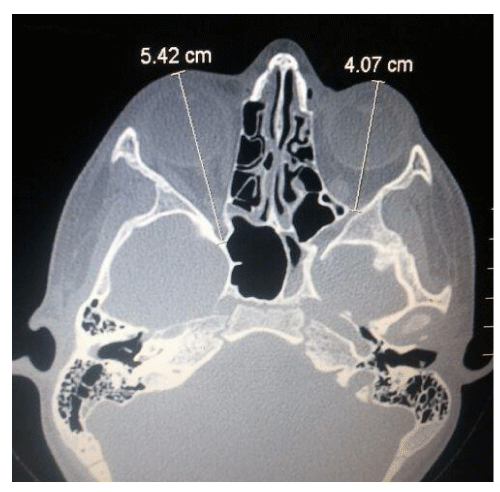
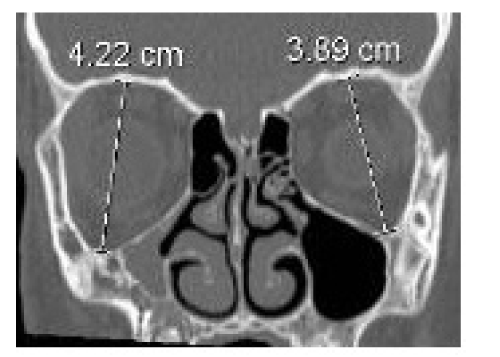
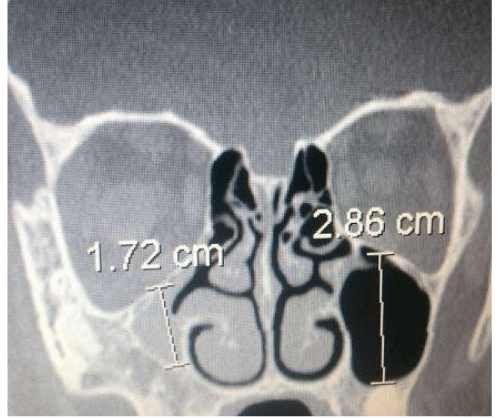
A measurement of the orbital and of the maxillary sinus structures was carried out. Analysis of axial sections showed a maximum longitudinal diameter of the orbit in the unaffected side of 4.07 cm compared to 5.42 cm on the affected side (Figure 1). The evaluation of coronal sections showed a maximum vertical orbital diameter of 3.89 cm in the left side compared to 4.22 cm on the affected side (Figure 2) and a maxillary vertical sinus diameter of 2.86 cm compared to 1.72 cm (Figure 3). An ophthalmologic assessment showed no alterations of visual acuity or of the fundus oculi, and the position or movements of the eyeball were normal. The persistence of the Wachendorf ’s membrane in the right eye, ipsilateral to the sinus atelectasis was also reported.
For resolution of nasal obstruction and restoration of the physiological pneumatization of the right maxillary sinus, we performed a surgical adenoidectomy, surgical turbinotomy with volume reduction of the right inferior turbinate and endoscopic maxillary sinus ostium dilatation with a Balloon Sinuplasty device (Acclarent®). The insertion of the balloon in the natural ostium was difficult since the medial wall of the maxillary sinus was lower than normal and significantly lateralized. After 3 months patency of the maxillary ostium was endoscopically was maintained. Therefore, considering the young age of the patient, the postoperative CT scan was delayed to reduce the X-rays exposure.
Discussion
In the last 20 years the SSS was recognized as a clinical entity characterized by specific clinical and radiological findings [1-3]. The clinical features are represented by spontaneous and unilateral enophthalmos and hypoglobus associated with malar depression and facial asymmetry. Visus distortion such as vertical diplopia, lagophthalmos and blurred vision occur less frequently. Although there is underlying maxillary sinus ipsilateral atelectasis, specific sinonasal symptoms are absent [4,5]. Etiological theories attempting to explain this phenomenon are numerous. The basis of the most widely accepted theory is an obstruction of the ostio-meatal complex which would result in a sinus hypoventilation. The onset of a negative pressure state in the sinus cavity would cause a progressive atelectasis of the air cavity, with a similar mechanism of the middle ear atelectasis secondary to Eustachian tube dysfunction. Furthermore, it would induce a decrease of osteoblastic activity and osteomalacic process of maxillary sinus bony walls and of the orbital floor [4]. The primary mechanism underlying the infundibulum obstruction has not yet been clarified. A particular anatomical configuration of the ostio meatal complex in combination with the sinonasal mucosal thickness of that has been suggested [6-8]. Other authors have suggested a condition of unilateral congenital hypoplasia of the maxillary sinus and subsequent changes causing a framework of chronic obstructive sinusitis. Several authors define, with no doubt, the acquired origin of this syndrome as presence of normal maxillary sinus bony structures before the onset of clinical and radiological signs of SSS are documented [9-11]. In 1997 Kass introduced a staging of chronic atelectasis by outlining anatomical changes of the maxillary sinus (Table 1). In this classification, alterations range from lateralization of the membranous fontanelle region (stage 1) to the development of anatomical deformity (stage 3) [12]. In the literature, a higher incidence of the disease between the third and fifth decade of life without a different prevalence between male and female is reported [13,14]. In a review performed by Numa, 84 cases were examined and reported in the literature [15]. The mean age of symptom onset was 39 years. In all cases enophthalmos was the dominant symptom associated with diplopia in 28% of cases. Rarely, sinonasal symptoms were reported. All cases were surgically treated with endoscopic techniques, restoring the patency of ostiomeatal complex, decompressing and evacuating the atelectatic maxillary sinus. Some patients underwent a transconjuntival reconstruction of the orbital floor with placement of a titanium mesh, achieving an improvement of the symptoms and clinical signs. In our case, discovery of the right maxillary sinus atelectasis was accidental. Although the bone structure of the maxillary sinus walls and the orbital floor were altered, the child did not yet show any ocular signs or symptoms caused by the dilation of orbital volumes. In this patient, the early diagnosis of maxillary atelectasis due to the blockage of the ostiomeatal complex prevented the potential evolution to a classical picture of a silent sinus syndrome with the surgical need of orbital floor reconstruction [16-18]. A balloon sinuplasty device was used to perform maxillary ostium dilatation to prevent damage to the mucosa and to the developing sinonasal structures [19]. In this case maxillary antrotomy in a young individual may prevent progressive enophtalmus that would require secondary orbital surgery.
| Stage I (membranous deformity) | Lateralized maxillary fontanelle |
| Stage II (bone deformity) | Inward bowing of one or more osseous walls (anterior, superior, and/or posterolateral bony walls) of the maxillary antrum |
| Stage III (clinical deformity) | Enophthalmos, hypoglobus, and/or midfacial deformity |
Table 1: Staging of Chronic Maxillary Atelectasis.
References
- Montgomery WW (1964) Mucocele of the maxillary sinus causing enophtalmos. Eye Ear Nose Throat Mon 43: 41-44.
- Wilkins RB, Kulwin DR (1981) Spontaneous enophthalmos associated with chronic maxillary sinusitis. Ophthalmology 88: 981-985.
- Soparkar CN, Patrinely JR, Cuaycong MJ, Dailey RA, Kersten RC, et al. (1994) The silent sinus syndrome. A cause of spontaneous enophthalmos. Ophthalmology 101: 772-778.
- Rose GE, Sandy C, Hallberg L, Moseley I (2003) Clinical and radiologic characteristics of the imploding antrum, or "silent sinus," syndrome. Ophthalmology 110: 811-818.
- Bossolesi P, Autelitano L, Brusati R, Castelnuovo P (2008) The silent sinus syndrome: diagnosis and surgical treatment. Rhinology 46: 308-316.
- Antonelli PJ, Duvall Aj, Teitelbaum SL (1992) Maxillary sinus atelectasis. Ann Otol Rhinol Laryngol 101: 977-981.
- Hazan A, Le Roy A, Chevalier E, Benzaken J, Waisberg A, et al. (1998) Atelectasis of the maxillary sinus. Analysis of progression stages. A propos of 4 cases. Ann Otolaryngol Chir Cervicofac 115: 367-372.
- Babin E, Bertrand M, Retout A, Gardea E, Choussy O (2009) Silent sinus syndrome with spontaneous orbital floor reconstruction. B-ENT 5: 125-128.
- Davidson JK, Soparkar CN, Williams JB, Patrinely JR (1999) Negative sinus pressure and normal predisease imaging in silent sinus syndrome. Arch Ophthalmol 117: 1653-1654.
- Hourany R, Aygun N, Della Santina CC, Zinreich SJ (2005) Silent sinus syndrome: an acquired condition. AJNR Am J Neuroradiol 26: 2390-2392.
- Ong L, McNab A (2003) The silent sinus syndrome: a case with normal predisease imaging. Orbit 22: 161-164
- Kass ES, Salman S, Rubin PA, Weber AL, Montgomery WW (1997) Chronic maxillary atelectasis. Ann Otol Rhinol Laryngol 106: 109-116.
- Eto RT, House JM (1995) Enophthalmos, a sequela of maxillary sinusitis. AJNR Am J Neuroradiol 16: 939-941.
- Hobbs CG, Saunders MW, Potts MJ (2004) Spontaneous enophthalmos: silent sinus syndrome. J Laryngol Otol 118: 310-312.
- Numa WA, Desai U, Gold DR, Heher KL, Annino DJ (2005) Silent sinus syndrome: a case presentation and comprehensive review of all 84 reported cases. Ann Otol Rhinol Laryngol 114: 688-694.
- Gaudino S, Di Lella GM, Piludu F, Martucci M, Schiarelli C, et al. (2013) CT and MRI diagnosis of silent sinus syndrome. Radiol Med 118: 265-275.
- Behbehani R, Vacareza N, Bilyk JR, Rubin PA, Pribitkin EA (2006) Simultaneous endoscopic antrostomy and orbital reconstruction in silent sinus syndrome. Orbit 25: 97-101.
- Soparkar CN, Patrinely JR, Davidson JK (2004) Silent sinus syndrome:new perspectives? Ophtalmology 111: 414-415.
- Sun DQ, Dubin MG (2013) Treatment of chronic maxillary atelectasis using balloon dilation. Otolaryngol Head Neck Surg 149: 782-785.
Citation: Mazzone S, Mancino R, Di Mauro R, Batipsta P, Di Girolamo S (2013) TMaxillary Antrostomy in a Boy to Prevent Silent Sinus Syndrome Evolution. Otolaryngology 4:151. DOI: 10.4172/2161-119X.1000151
Copyright: © 2013 Mazzone S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 17962
- [From(publication date): 2-2014 - Jul 06, 2025]
- Breakdown by view type
- HTML page views: 13254
- PDF downloads: 4708