Case Report Open Access
A 16 Year Old Girl with Atypical Bronchial Carcinoid Tumor
Alzoobaee Saif1*, Khani Francesca2, Narula Navneet2, Veler Haviva1, Modi Vikash3, Kovanlikaya Arzu4 and Stone Anne1
1Department of Pediatrics, Weill Cornell Medical College, New York, USA
2Department of Pathology, Weill Cornell Medical College, New York, USA
3Department of Otolaryngology, Weill Cornell Medical College, New York, USA
4Department of Radiology, Weill Cornell Medical College, New York, USA
- *Corresponding Author:
- Alzoobaee Saif
435 East 70th street, Payson House 33L
New York, 10021, USA
Tel: 3474327164
E-mail: saa2041@nyp.org
Received: November 30, 2015; Accepted: December 21, 2015; Published: December 28, 2015
Citation: Saif A, Francesca K, Navneet N, Haviva V, Vikash M, et al. (2015) A 16 Year Old Girl with Atypical Bronchial Carcinoid Tumor. Neonat Pediatr Med 1: 102. doi: 10.4172/2572-4983.1000102
Copyright: © 2015 Saif A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Neonatal and Pediatric Medicine
Abstract
We report a 16 year old girl who presented with recurrent pneumonias and abnormal chest imaging who we diagnosed with an atypical bronchial carcinoid obstructing the left main-stem bronchus. This case highlights the lack of data on adjuvant therapy after surgical resection and the absence of surveillance guidelines for children with pulmonary carcinoid.
Keywords
Carcinoid; Lung; Tumor; Pediatric; Bronchial
Introduction
Bronchial carcinoid tumors are malignant neoplasms comprised of neuroendocrine cells [1,2]. Carcinoids are classified histologically as either typical or atypical. The majority are typical (80-90%), occurring most frequently in the fifth and sixth decades, and have 5 and 10-year survival rates ranging from 87-100% and 82-94%, respectively [3]. Patients with atypical carcinoids are typically a decade older and have worse 5 and 10-year survival rates (44-88% and 18-64%, respectively) [3]. Although most affected patients are adults, carcinoid is the most common primary pulmonary malignancy of childhood [3,4], with the youngest reported patient diagnosed at 3 years [5]. Atypical carcinoids in children are rare [6].
While surgical resection is the preferred treatment, there is little data regarding adjuvant therapy. Furthermore, guidelines defining how to monitor for disease recurrence are lacking, particularly among children.
We report a 16 year-old girl with atypical bronchogenic carcinoid treated with sleeve lobectomy. Adjuvant chemotherapy and surveillance serial CT scans were recommended.
Case Report
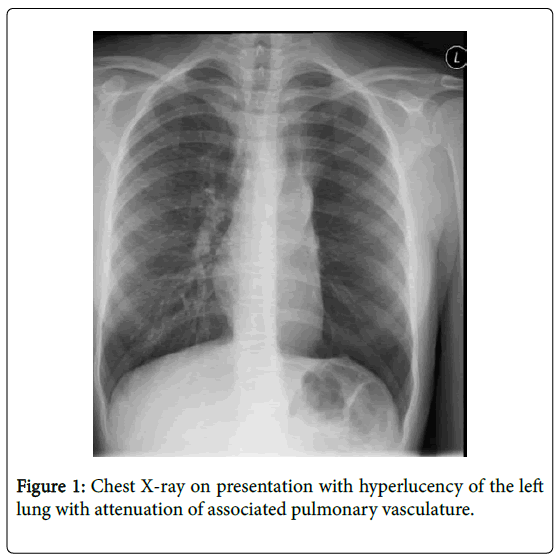
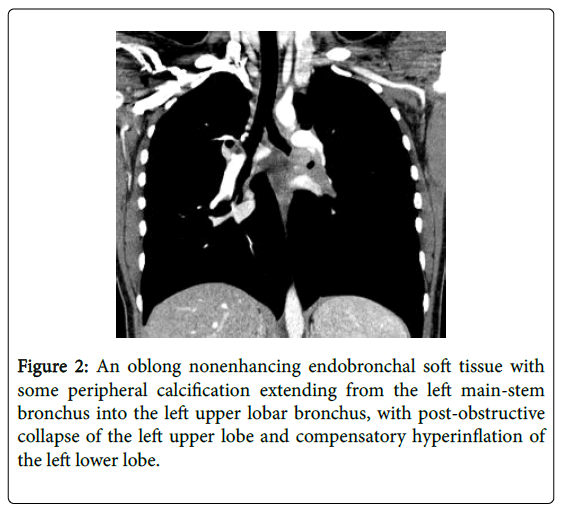
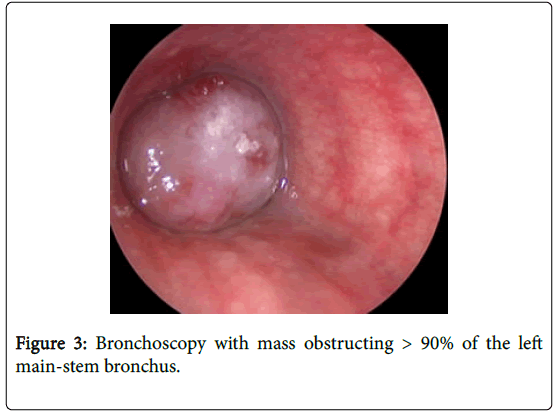
A 16 year-old girl was referred to pediatric pulmonology for recurrent pneumonia and abnormal chest films. The patient had two previous illnesses with cough and fever treated with antibiotics. The first occurred at age 12 and the second at age 16, three months prior to presentation. The patient recovered after these illnesses and did not have a history of chronic cough, dyspnea, or exercise intolerance. Physical exam showed a well-appearing girl. Oxygen saturation was 97%. There were decreased breath sounds throughout the left thorax. Pulmonary function testing demonstrated restriction with decreased FVC (58% predicted), FEV1 (58% predicted), and TLC (68% predicted). Chest radiograph demonstrated hyperlucency of the left lung (Figure 1). Chest CT revealed a nonenhancing endobronchial soft tissue mass at the left mainstem bronchus extending into the left upper lobar bronchus (Figure 2). A mass at the proximal left mainstem bronchus with >90% obstruction (Figure 3) was visualized during flexible bronchoscopy. The child underwent a left upper lobe sleeve lobectomy with resection of a 3.2 cm endobronchial mass (Figure 4).
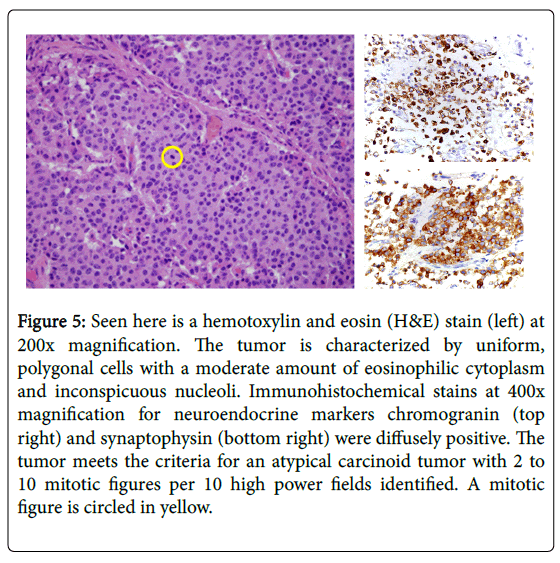
The pathological diagnosis was an atypical carcinoid with invasion of the bronchial wall into the peribronchial soft tissue and involvement of two ipsilateral peribronchial lymph nodes. There were foci of punctate necrosis and 2 mitoses per 10 high power fields (Figure 5). Disease was staged as IIA (T2a N1 M0). Adjuvant therapy with cisplatin and etoposide was recommended as were surveillance chest CT scans every six months for the first two years and then annually.
Figure 5: Seen here is a hemotoxylin and eosin (H&E) stain (left) at 200x magnification. The tumor is characterized by uniform, polygonal cells with a moderate amount of eosinophilic cytoplasm and inconspicuous nucleoli. Immunohistochemical stains at 400x magnification for neuroendocrine markers chromogranin (top right) and synaptophysin (bottom right) were diffusely positive. The tumor meets the criteria for an atypical carcinoid tumor with 2 to 10 mitotic figures per 10 high power fields identified. A mitotic figure is circled in yellow.
Discussion
We describe a 16 year old girl with an atypical carcinoid of the left main-stem bronchus with lymph node involvement. The prognosis of bronchial carcinoid among children is poorly defined [7]. A review of 15 children suggests a more favorable prognosis than among adults. Subjects were surgically treated at a median age of 15 years (range 8-18); the authors reported disease-free survival rates of 96% and 94% at 10 and 20 years, respectively [7,8]. There were no mortalities with a median follow-up of 10 years, although two patients developed recurrence [8]. Only two subjects had atypical carcinoid [8].
Atypical carcinoids among children are rare. In a recently published case report, Geramizedah summarizes seven cases (age range 10-21 years) [6]. All but one were treated surgically (four with pneumonectomy/lobectomy, two with sleeve resection, and one by bronchoscopic polypectomy). Three of the seven were treated with chemoradiation. Two of the seven, with metastatic disease, died within a year of diagnosis. Only short-term follow-up of 6-18 months were reported except for a single case of a 17 year old who was asymptomatic at 134 months [7,9,10].
Larger adult case series reveal high rates of nodal involvement and disease recurrence for atypical carcinoid (48-75% and 26% respectively) [11,12] compared to typical carcinoid (3-20% and 3% respectively). Additionally, there is a shorter time to disease recurrence for atypical carcinoid (22 months, range 2-83) compared to typical carcinoid (50 months; range 9-141) [12]. The majority of disease recurrence for atypical carcinoid involves distant metastases [12]. Lymph node involvement increases the recurrence rate for both pathologic types [13].
There is little data on adjuvant therapy for atypical carcinoid. In a review of 31 adults (median age 60 years) with metastatic pulmonary carcinoid, Granberg et al. describes 3/8 treated with cisplatin and etoposide who experienced disease stabilization or decreased tumor size for 6-8 months [14]. Similarly, Grote et al. reports response to chemotherapy alone in 3/8 adults with atypical carcinoid; the duration of response ranged from 5-12 months [10]. There is no first-line chemotherapy regimen, but medications that have been used previously include octreotide, cyclophosphamide, vincristine, and etoposide to name a few. However, The North American Neuroendocrine Tumor Society and the International Association for the Study of Lung Cancer state that there is insufficient data to recommend adjuvant therapy [15,16]. Additionally, there is no data evaluating the role of adjuvant therapy among children.
Lastly, there are no guidelines for monitoring for disease recurrence. The North American Neuroendocrine Tumor Society recommends that patients be reassessed with physical examination, laboratory testing and imaging once between 3 and 6 months after resection, and subsequently every 6 to 12 months for at least 7 years [16]. Others suggest yearly CT scans with contrast of the chest and upper abdomen for typical and atypical carcinoids with lymph node involvement [12]. With disease recurrence reported years after diagnosis, however, it is unclear how to screen patients over time. This is particularly true among affected children who potentially would be exposed to the risks of years of CT screening [12].
Follow-up
The patient elected to be treated at an outside institution and on follow-up, it was determined that she was treated with everolimus and octreotide over the course of 9 months. There was no disease recurrence on imaging two years after resection.
In summary, atypical bronchogenic carcinoids are rare among children with little to no data to guide adjuvant chemoradiation or disease surveillance.
References
- Bertino EM, Confer PD, Colonna JE, Ross P, Otterson G (2009) Pulmonary neuroendocrine/carcinoid tumors: A review article. Cancer 115: 4434-4441.
- Travis WD, Brambilla E, Müller-hermelink HK, Harris CC (2004) World Health Organization Classification of Tumours: Tumours of the Lung, Pleura, Thymus and Heart. Lyon: IARC Press, France.
- Benson RE, Rosado-de-Christenson ML, Martínez-Jiménez S, Kunin JR, Pettavel PP (2013) Spectrum of pulmonary neuroendocrine proliferations and neoplasms. Radiographics 33: 1631-1649.
- Hurt R, Bates M (1984) Carcinoid tumours of the bronchus: A 33 year experience. Thorax 39: 617-623.
- Moraes T, Langer JC, Forte V, Shayan K, Sweezey N (2003) Pediatric pulmonary carcinoid: A case report and review of the literature. Pediatr Pulmonol 35: 318-322.
- Geramizadeh B, Foroutan HR, Shokripour M, Dehghanian AR (2013) Pulmonary atypical carcinoid tumor in a 15-year-old girl: A case report and review of the literature. Rare Tumors 5: e45.
- Rizzardi G, Bertolaccini L, Terzi A (2011) Paediatric Oncology Bronchial Carcinoid Tumours in Children - A Review. Eur J Oncol Hematol 7: 196-199.
- Rizzardi G, Marulli G, Calabrese F, Rugge M, Rebusso A, et al. (2009) Bronchial carcinoid tumours in children: Surgical treatment and outcome in a single institution. Eur J Pediatr Surg 19: 228-231.
- Yu Y, Song Z, Chen Z, Jian H, Lu S (2011) Chinese pediatric and adolescent primary tracheobronchial tumors: A hospital-based study. Pediatr Surg Int 27: 721-726.
- Grote TH, Macon WR, Davis B, Greco FA, Johnson DH (1988) Atypical carcinoid of the lung. A distinct clinicopathologic entity. Chest 93: 370-375.
- Fink G, Krelbaum T, Yellin A, Bendayan D, Saute M, et al. (2001) Pulmonary carcinoid: Presentation, diagnosis and outcome in 142 cases in Israel and review of 640 cases from the literature. Chest 119: 1647-1651.
- Lou F, Sarkaria I, Pietanza C, Travis W, Roh MS, et al. (2013) Recurrence of pulmonary carcinoid tumors after resection: implications for postoperative surveillance. Ann Thorac Surg 96: 1156-1162.
- Thomas CF Jr, Tazelaar HD, Jett JR (2001) Typical and atypical pulmonary carcinoids : outcome in patients presenting with regional lymph node involvement. Chest 119: 1143-1150.
- Granberg D, Eriksson B, Wilander E, Grimfjärd P, Fjällskog ML, et al. (2001) Experience in treatment of metastatic pulmonary carcinoid tumors. Ann Oncol 12: 1383-1391.
- Lim E, Goldstraw P, Nicholson AG, Travis WD, Jett JR, et al. (2008) Proceedings of the IASLC International Workshop on Advances in Pulmonary Neuroendocrine Tumors 2007. J Thorac Oncol 3: 1194-1201.
- Phan AT, Oberg K, Choi J, Harrison LH Jr, Hassan MM, et al. (2010) NANETS consensus guideline for the diagnosis and management of neuroendocrine tumors: Well-differentiated neuroendocrine tumors of the thorax (includes lung and thymus). Pancreas 39: 784-798.
Relevant Topics
- About the Journal
- Birth Complications
- Breastfeeding
- Bronchopulmonary Dysplasia
- Feeding Disorders
- Gestational diabetes
- Neonatal Anemia
- Neonatal Breastfeeding
- Neonatal Care
- Neonatal Disease
- Neonatal Drugs
- Neonatal Health
- Neonatal Infections
- Neonatal Intensive Care
- Neonatal Seizure
- Neonatal Sepsis
- Neonatal Stroke
- Newborn Jaundice
- Newborns Screening
- Premature Infants
- Sepsis in Neonatal
- Vaccines and Immunity for Newborns
Recommended Journals
Article Tools
Article Usage
- Total views: 13889
- [From(publication date):
December-2015 - Aug 30, 2025] - Breakdown by view type
- HTML page views : 12834
- PDF downloads : 1055