Case Report Open Access
An Alternative Approach for the Treatment of Major Aphthosis: Case Report
Gianna Maria Nardi1, Felice Roberto Grassi2, Dorina Lauritano3* and Massimo Petruzzi21Department of Oral and Maxillofacial Sciences, Sapienza University of Rome, Italy
2Dental Clinic of University of Bari “Aldo Moro”, Italy
3Department of Translational Medicine, University of Milan-Bicocca, Milan, Italy
- Corresponding Author:
- Dorina Lauritano
Department of Translational Medicine
University of Milan-Bicocca, Milan, Italy
Tel: 00393356790163
E-mail: dorina.lauritano@unimib.it
Received date: February 10, 2014; Accepted date: August 04, 2014; Published date: August 11, 2014
Citation: Nardi GM, Grassi FR, Lauritano D, Petruzzi M (2014) An Alternative Approach for the Treatment of Major Aphthosis: Case Report. J Interdiscipl Med Dent Sci 2:137. doi: 10.4172/2376-032X.1000137
Copyright: © 2014 Nardi GM, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Visit for more related articles at JBR Journal of Interdisciplinary Medicine and Dental Science
Abstract
An effective treatment for aphthous stomatitis is not still available and its treatment consists only of therapeutic measures to suppress its symptoms. We report a case of a 60-year caucasian woman presented a 16-year history of episodes of multiple major recurrent ulcers in the oral mucosa. Topical application of Oralmedic® caused an improvement of pain, discomfort and healing of the aphthous ulcer. No adverse events or side effects were recorded. Oralmedic® is an effective topical device for the major aphthous ulcers treatment.
Keywords
Major aphthosis; Topical treatment; Ulcerous stomatitis
Introduction
Aphthae are common oral lesions that affect approximately 10% to 20% of the population. The etiology of aphthous stomatitis is unknown but according to an increasing evidence, its development has an immunogenic process that causes the ulceration of the involved oral mucosa. Aphthous ulcers are usually classified into three different types: minor, herpetiform and major [1,2]. Minor aphthae are generally located on labial or buccal mucosa, the soft palate, the floor of the mouth, the ventral surface and the border of the tongue. They can be singular or multiple and tend to be small (less than 1 cm in diameter) and shallow [2]. Herpetiform aphthae are rare and their clinical aspect is similar to the Herpes virus vesciculae. Major aphthae are similar to minor aphthae but they are larger (may reach over 1 cm in diameter) and cause a deeper ulceration. This subtype makes up about 10% of all cases of aphthous stomatitis. Major aphthous ulceration usually affects non keratinized mucosal surfaces, but less commonly keratinized mucosa may also be involved. Pariadenitis mucosa necrotica recurrens or Sutton disease is characterized by the involvement of minor salivary in the oral mucosal destructive process that causes the ulcers. Major aphthous ulcerations can persist for several days or weeks and often heal with scarring. The pain associated with major aphthae lesions can affect eating, speaking and oral hygiene practices [3]. There have been many attempts over the years to find an effective treatment for aphthous stomatitis, but the etiology of this stomatitis remains unknown and its treatment consists only of therapeutic measures to suppress its symptoms rather than bringing about a definitive cure. The therapeutic choice depends on the severity of the disease which is measured by the frequency of ulcers recurrence, the number of ulcers, their location, duration and the level of associated orofacial pain [4]. Most of major aphthosis cases are characterized by pain, fever, dysphagia and require a systemic therapy. Several systemic drugs have been used to treat major aphthosis, including systemic corticosteroids, dapsone, colchicine, thalidomide, pentoxifylline, low-dose interferon-α and levamisole [5]. The use of systemic corticosteroids and immunomodulating agents has been the mainstay of treatment for major aphthae. Intralesional steroid injections, containing betamethasone dipropionate and betamethasone disodium phosphate, combined with levamisole therapy may successfully treat the large ulcers associated with major aphthosis [6]. A recent Cochrane review on the systemic treatment for the recurrent aphthous stomatitis concluded that “no single treatment was found to be effective and therefore the results remain inconclusive in regard to the best systemic intervention for recurrent aphthous stomatitis” [7].
The following report describes a case of major aphthosis involving the oral mucosa successfully treated with topical applications of Oralmedic®.
Case Report
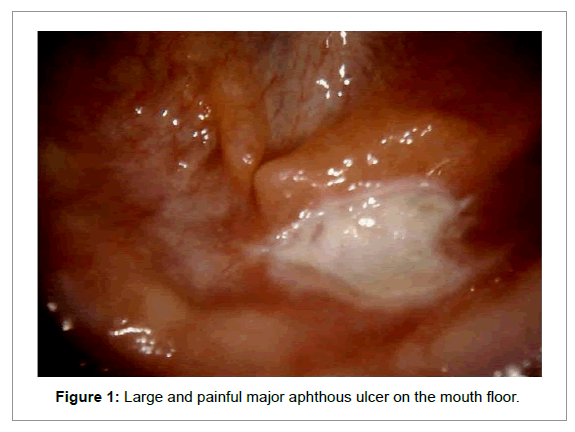
A 60-year-old caucasian woman presented a 16-year history of episodes of multiple major recurrent ulcers in the oral mucosa (non keratinized mucosa). During the patient’s anamnesis, she reported having had these episodes since the first pregnancy and having already been treated with corticosteroids, without success. Clinical examination revealed a symptomatic ulcer with a perilesional erythematous halos covered with a pseudomembrane and located in the floor of the mouth mucosa, exceeding 10 mm in diameter (Figure 1). A clinical diagnosis of major aphthous ulcer was made on the basis of the history and the clinical examinations. The other aspects both of the patient’s medical history and the family medical history were insignificant. Laboratory tests including a blood count analysis were performed to determine the levels of folic acid, iron, ferritin, as well as vitamins B2, B6 and B12. All the results were normal.
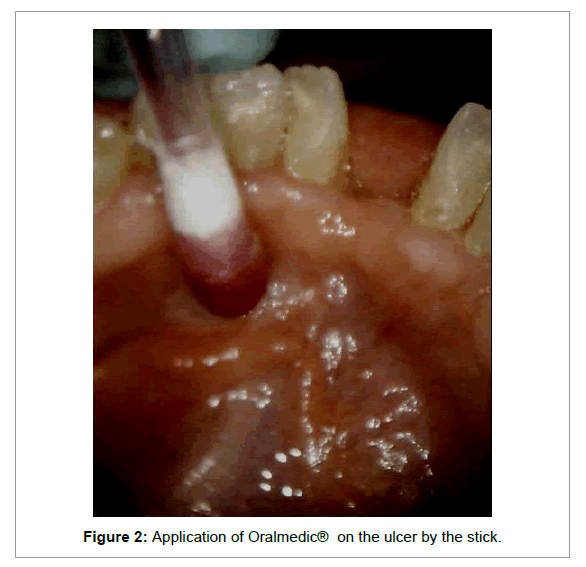
The patient was subjected to a therapeutic regimen consisting of daily topical application of Oralmedic® (Ceuta Healthcare, Hill House, Richmond Hill, Bournemouth, UK). After buffering and drying the ulcerative area, approximately 0.2 ml of the cauterizing solution was delivered from a hollow shaft of a cotton wool swab to the tip which was then placed upon the ulcer (in situ) for 10 seconds (Figure 2).
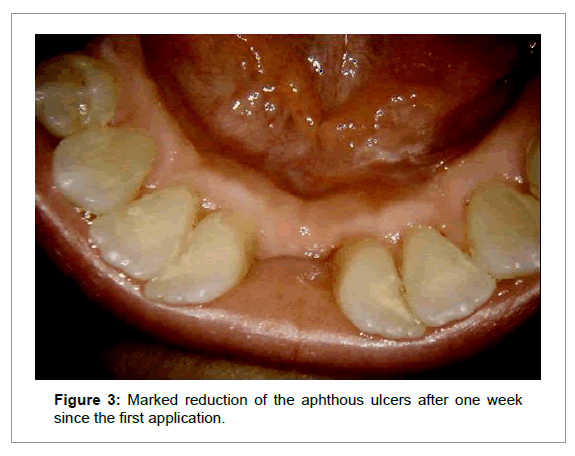
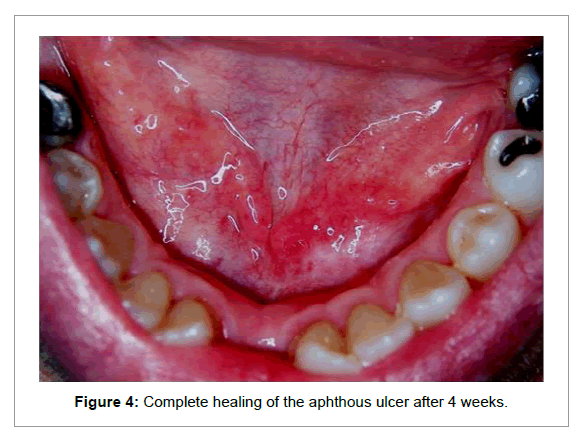
Afterwards the patient rinsed and dried the treated area. The patient was subjected to four applications with Oralmedic® once a week. In the subsequent follow-up visits there was an improvement of pain, discomfort and healing of the aphthous ulcer (Figure 3 and 4). No adverse events or side effects were recorded.
Discussion
Because of its uncertain etiology and variegate clinical presentation, aphthous stomatitis remains a challenge for the specialists in oral pathology and medicine. B group vitamins deficiency or impairment of iron metabolism may be the predisposing factor in the pathogenic cascade but only a restrict number of patients show a vitamin or iron deficit. In the reported case, the patients was in good health and the aphthous ulcer was defined as “idiopathic”. Treatment of aphthous ulcers is fundamentally symptomatic: it is aimed to reduce the severity and duration of the pain and decrease the frequency of the relapse. The lack of an efficacious and definitive prophylactic protocol has led to the development of several treatments that use different drugs, antibacterial agents (eg, minocycline, tetracycline, cephalexin), anti-acidic agents (eg, sucralfate) and antineoplastics (eg, thalidomide) [8-10]. Anti-inflammatory and immunomodulatory agents such as clofazimine, thalidomide, pentoxifylline, colchicine, levamisole, azathioprine, amlexanox and steroids have been administered with varying clinical benefits [11].
The active principle of Oralmedic® utilizes the same technology commercialized for the non-surgical treatment of the dental plaque (HybenX®): it is a desiccant liquid and its application to plaque biofilm instantly causes rapid absorption of water (strong hygroscopic properties), which leads to the precipitation and collapse of organic material. The Oralmedic® solution comprises a concentrated aqueous mixture of free sulphate and sulphonated aromatics, specifically hydroxybenzenesulphonic acid, hydroxymethoxybenzene suphonic acid and suphuric acid. The hydrozybenzenes are keratolytic, whereas the sulphonate groups and sulphuric acid are hygrposcopic and denaturing. The use of Oralmedic® in the treatment of aphtae was first reported by Porter et al. [12]. They examined the potential benefits of HybenX in a prospective randomized trial. Their results revealed that when compared with a device designed to protect areas of oral ulceration, local application of HybenX significantly reduced the pain of RAS after 2 days. Both HybenX and the control device caused a reduction in unchallenged pain scores between days 1 and 4, but the reduction by HybenX was always greater than that of the control device. Denaturation, precipitation and coagulation of the tissue debris on the aphthous ulcer surface and the creation of a protective layer of coagulated tissue debris over the surface of the ulcer decreases local discomfort and protects to painful stimuli. This protective surface debris is resorbed during the “restitutio ad integrum” process [13].
A recent study shows that the topical treatments for recurrent aphthous stomatitis are not efficacious in the improvement of quality of life in the affected patients and only colchicine seems to be effective in the management of signs and symptoms related to aphthous ulcerations [14]. However, the topical treatment offers numerous advantages related to the scarcity of side effects, a more tolerability and its easy use in the delimited area to treat.
Conclusion
In conclusion, Oralmedic® is an effective topical device for the major aphthous ulcers treatment. Alternative treatment options are required and the benefits and harms of using topical Oralmedic® in people with aphthous stomatitis need a thorough evaluation in properly designed controlled studies.
Competing Interests
The authors declare that they have no competing interests
Authors’ Contribution
MP, GMN and FRG were responsible for the study conception and design. MP and FRG acquired the data and drafted the manuscript. GMN and MP selected and commented on the imaging. All authors read and approved the final manuscript.
References
- Burgess JA, Johnson BD, Sommers E (1990) Pharmacological management of recurrent oral mucosal ulceration. Drugs 39: 54–65.
- Gombos F, Serpico R (1999) Immunopatologia Orale. Piccin, Padova (Italy).
- Jacobson JM, Greenspan JS, Spritzler J, Ketter N, Fahey JL, et al. (1997) Thalidomide for the treatment of oral aphthous ulcers in patients with human immunodeficiency virus infection. National Institute of Allergy and Infectious Diseases AIDS Clinical Trials Group. N Engl J Med 336: 1487–1493.
- McBride DR (2000) Management of aphthous ulcers. Am Fam Physician 62: 149-154.
- Chavan M, Jain H, Diwan N, Khedkar S, Shete A, et al. (2012) Recurrent aphthous stomatitis: a review. J Oral Pathol Med 41: 577-583.
- Altenburg A, Zouboulis CC (2008) Current concepts in the treatment of recurrent aphthous stomatitis. Skin Therapy Lett 13: 1–4.
- Brocklehurst P, Tickle M, Glenny AM, Lewis MA, Pemberton MN, et al. (2012) Systemic interventions for recurrent aphthous stomatitis (mouth ulcers). Cochrane Database Syst Rev.
- Gorsky M, Epstein J, Rabenstein S, Elishoov H, Yarom N (2007) Topical minocycline and tetracycline rinses in treatment of recurrent aphthous stomatitis: a randomized cross-over study. Dermatol Online J 13: 1.
- Gorsky M, Epstein J, Raviv A, Yaniv R, Truelove E (2008) Topical minocycline for managing symptoms of recurrent aphthous stomatitis. Spec Care Dentist 28: 27–31.
- Chiu HY, Tsai TF (2011) Topical use of systemic drugs in dermatology: a comprehensive review. J Am Acad Dermatol 65: 1048.
- Karavana SY, Gökçe EH, Rençber S, Özbal S, Pekçetin C, et al. (2012) A new approach to the treatment of recurrent aphthous stomatitis with bioadhesive gels containing cyclosporine A solid lipid nanoparticles: in vivo/in vitro examinations. Int J Nanomedicine 7: 5693-5704.
- Porter SR, Al-Johani K, Fedele S, Moles DR (2009) Randomised controlled trial of the efficacy of HybenX in the symptomatic treatment of recurrent aphthous stomatitis. Oral Dis 15:155-161.
- Rhodus NL, Bereuter J (1998) An evaluation of a chemical cautery agent and an anti-inflammatory ointment for the treatment of recurrent aphthous stomatitis: a pilot study. Quintessence Int 29: 769-773.
- Hapa A, Aksoy B, Polat M, Aslan U, Atakan N (2011) Does recurrent aphthous stomatitis affect quality of life? A prospective study with 128 patients evaluating different treatment modalities. J Dermatolog Treat 22: 215-220.
Relevant Topics
- Cementogenesis
- Coronal Fractures
- Dental Debonding
- Dental Fear
- Dental Implant
- Dental Malocclusion
- Dental Pulp Capping
- Dental Radiography
- Dental Science
- Dental Surgery
- Dental Trauma
- Dentistry
- Emergency Dental Care
- Forensic Dentistry
- Laser Dentistry
- Leukoplakia
- Occlusion
- Oral Cancer
- Oral Precancer
- Osseointegration
- Pulpotomy
- Tooth Replantation
Recommended Journals
Article Tools
Article Usage
- Total views: 16674
- [From(publication date):
October-2014 - Sep 01, 2025] - Breakdown by view type
- HTML page views : 12008
- PDF downloads : 4666