Research Article Open Access
An Attachment-Based Parenting Training Program for Opiate Dependent Carers
Mathew James Coleman*Great Southern Mental Health Service, Albany, WA, Australia
- Corresponding Author:
- Mathew James Coleman
Great Southern Mental Health Service
Albany, WA, Australia
E-mail: mathew.coleman@health.wa.gov.au
Received date: October 02, 2014; Accepted date: November 18, 2014; Published date: November 28, 2014
Citation: Coleman MJ (2014) An Attachment-Based Parenting Training Program for Opiate Dependent Carers. J Addict Res Ther 5:201. doi:10.4172/2155-6105.1000201
Copyright: © 2014 Coleman MJ. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
Background: Parental substance use can impede parenting, placing a significant number of children at risk, accounting for the high rates of child protection service (CPS) involvement with substance use affected families. Very few parenting programs provide evidence for improving parenting skills in this high risk group. However, attachment-based parenting programs provide some promise in improving outcomes for parents and children. This pilot study introduces such a program, the Circle of Security (COS), with opiate dependent carers.
Method: Pre and post COS intervention measures of substance use (ATOP), mental health (DASS21) and child-parent attachment (CHQ) were conducted. A qualitative feedback questionnaire was also undertaken to determine the tolerability, acceptability and experiences of participants.
Results: 8 participants commenced the study with a retention rate of 75%. Heroin (M=-2.4), other opiate (M=-2.3), alcohol (M=-2.7), nicotine (M=-0.1) and injecting drug days (M=-3.0) were reduced following the intervention. Parental stress (M=-4, 19%), depression (M=-3.29, 16%) and anxiety (M=-2.57, 12%) improved over the study period. No clinically significant shift in carer-helplessness was identified, however parents reported improved parenting in a number of areas. Participants highly rated the program across multiple domains.
Conclusions: The COS is well tolerated, accepted and positively experienced by this group of opiate dependent carers. The program appears to assist in reducing substance use levels and improving mental health symptoms in this vulnerable group of parents. The program warrants further evaluation with opiate dependent parents as part of a randomised control trial.
Keywords
Attachment; Parent training; Opiate; Dependence; Pilot study
Background and Literature Review
Problem drug use can impede parenting and the provision of a safe, nurturing environment for children’s social and emotional development. These parenting deficits begin when children are infants and continue as the child moves through school-age and into adolescent years. High rates of child abuse and neglect, up to 40%, occur in many families in which either or both parents abuse illicit drugs [1,2]. Maternal substance abuse specifically, more than most other psychiatric or social problems (with the exception of poverty) is the most common factor involved when children come to the attention of Child Protection Service (CPS) [3,4].
The self-reported impact of drug dependence on children includes material neglect, exposure to drug use and dealing, increased exposure to and to the risk of violence and physical abuse, exposure to criminal behaviour and family break up [5]. Research has consistently shown a pattern of significantly less supervision of a child, more punitive forms of discipline, less discussion and positive involvement with the child, more parental disagreement regarding discipline and less pro-social skills in parenting [6-10].
Australian research by Quinlivan et al. [11] suggests that despite excellent perinatal care, established drug abuse is associated with poorer maternal attachment. These attachment difficulties are manifested by parental guilt, anxiety, anger and uncertainty associated with drug use [12]. User’s own attachment experiences, that may have significantly influenced the initiation and maintenance of drug use problems, are evoked with the pressures of parenthood. Without intervention, these parents risk the intergenerational transmission of attachment difficulties with their own children [13]. Disorganized or insecure attachment independently in many studies has been shown to result in enduring adverse outcomes for children including behavioural, social, affective and substance use problems [3,7,14,15]. Research studies broadly examining parenting interventions have shown that helping drug dependent parents in improving their parenting skills results in significant positive change for parents, including reducing their drug use but also across other domains of family and child functioning [2,16].
Behavioural parent training programs for drug-dependent mothers have had limited success in improving parent-child relationships or children’s psychological adjustment [17-19]. In Australia, Dawe and Harnett [2] developed an intensive, home-based intervention, the Parents Under Pressure (PUP) program for families with a parent on a methadone maintenance program. The intervention combined methods for improving parental mood and parenting skills through the use of mindfulness techniques in cognitive therapy with weekly sessions over 10-12 weeks. Although the program resulted in a reduction in child abuse potential, rigid parenting attitudes and child behaviour problems, follow up studies of PUP have suggested the program can achieve short-term change in some but not all families [20]. To date, these interventions have been expensive, resource intensive and have shown limited evidence of improving outcomes for substance using parents or their children.
Suchman et al. [21] postulate that one reason behavioural parenting programs may have had limited success with drug dependent parents is their lack of attention to the emotional quality of the parent-child relationship. Research on attachment suggests that the emotional quality of mother-child relationships is an important predictor of children’s psychological development through school-age and adolescent years [15]. For children, interventions aimed at improving parents’ reflective and mindfulness capacities have demonstrated improvements over 6 months in rates of potential child abuse, rigid parenting attitudes and child behaviour problems [2]. Furthermore, metallization, the capacity for understanding behaviour in light of underlying mental states and intentions, is recognized as another domain in which mother-child attachment can be enhanced for the benefit of child emotional development and resilience [22]. Attachment style parenting interventions have also been shown to have long term effects on reducing substance use disorders of the children of drug dependent parents [22]. The evidence from intervention studies with high-risk non-substance-using parents has shown attachment-based approaches hold considerable promise, especially when maternal representations and reflective functioning are targeted [23]. Studies of attachment-based parenting interventions with at-risk mothers (including the Circle of Security and Watch, Wait and Wonder) have shown that mental representations of caregiving and child attachment classification can change in response to intervention [24-27].
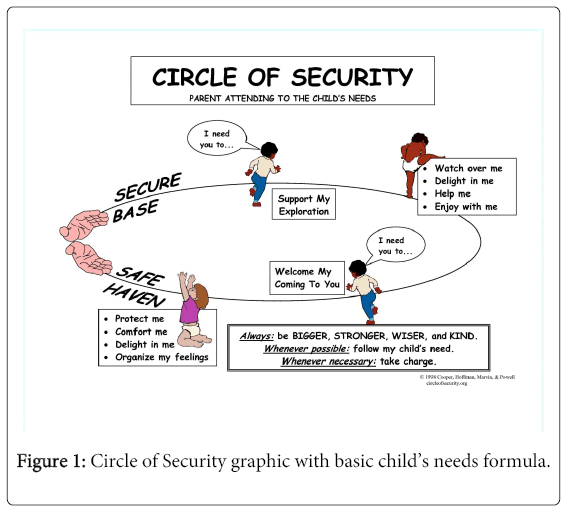
The Circle of Security (COS) has been one such program that has gained some popularity within Australian infant and child mental health and community services. Its development has drawn on the dynamics of secure/insecure attachment patterns whilst also exploring caregiver patterns of behaviour and caregiver representations. The program has five key goals including: (a) establish the therapist and group as a secure base from which to explore caregiver-child relationships; (b) increase caregiver sensitivity and responsiveness by providing a map of children’s basic attachment needs; (c) increase caregivers knowledge of verbal/nonverbal cues signaling children’s internal states; (d) increase caregiver empathy by supporting reflection regarding attachment orientated interactions; and (e) increase caregiver reflection about their own developmental history and patterns of care giving behaviour (Figure 1) [25].
Research studies of the COS intervention have shown it to be effective in reducing insecure attachment and increasing security for children in the age range between toddlerhood and early school years [25]. COS intervention evidence is based on a study of 65 toddlers and pre-schoolers assessed for attachment security before and immediately after intervention. The participants recruited were from vulnerable child programs in the US; all had low incomes, and most parents and some of the children had experienced maltreatment or trauma (no comment on substance use was made). Prior to COS intervention, only 20% of the children were classified as secure; following the COS intervention, a significant shift occurred with 54% re-classified as secure. A significant reduction in rates of disorganized attachment (from 60% to 25%) was also found [25]. Given that insecure and disorganized attachment can be a risk factor for future psychopathology, the COS protocol offers a preventative and treatment intervention for vulnerable child-parent dyads. Importantly the COS program can make evidence-based claims of low risk of negative outcomes, i.e to do no harm.
The Present Pilot Study – Enhancing Secure Attachment for Opiate Dependent Parents and their Young Children
While reporting rates of child neglect or abuse in Australia involving substance using parents remains high, around 50% of CPS cases, preventative and treatment interventions are unfortunately rarely available from Drug and Alcohol services [28-30]. Despite the high needs, substance disordered clients are frequently excluded from traditional mental health services, including child and adolescent focused services. To the author’s knowledge, the 8 week COS program has never been trialled or studied in a specific substance disordered population.
The aim of this study was to evaluate a pilot study of the COS 8 session DVD group program, with opiate dependent caregivers. The study hypotheses were that the intervention would improve caregiver reflectiveness and empowerment in the child-parent dyad, reduce parent substance use, and improve parent mental health. A final objective was to qualitatively examine the tolerability, acceptability and experiences of this group of parents to the short version COS program.
Method
The research project received ethics approval by the Northern Sydney Coast EC0012 (NSC) Human Research ethics Committee – 1205-118M. The research study evaluated the COS 8 session group program for opiate dependent primary carers of children between 0 and 5 years of age. As this has been the first time that the COS intervention has been studied in an opiate dependent parent group, no randomised control group was established and the study was undertaken as a pilot study.
The study was advertised to active clients of two Opiate Treatment Program (OTP) clinics in the Sydney metropolitan area via posters displayed in clinic waiting areas, and by notification from case managers. To be eligible for the study, participants had to be active clients of one of the OTPs and must be a primary career to one or more children aged 0 to 5 years of age. Children did not have to be permanently in the participants care at the time of commencing the study so as not to exclude participants’ who may have had their children temporarily removed by CPS. Informed consent to participate was obtained and all participants were provided with verbal and written information about the research pilot and COS program. Participants were informed of the mandatory notification requirements to local CPS if their participation identified any child who was thought to be at risk of abuse or neglect.
The COS sessions occurred at 2 separate locations, comprising 2 groups of 4 caregivers. The first 8 participants recruited were accepted into the study. Sessions occurred at the same time, on the same day, for 8 consecutive weeks. Participants were encouraged to privately arrange child care. However, caregivers were not excluded if they attended with their child (ren). Supervision of participants’ children remained the responsibility of the participant.
Each session ran for approximately one hour, and was delivered directly from the COS manual in conjunction with the relevant DVD chapter by the primary investigator who has COS facilitation accreditation. Non-COS trained co-facilitators were utilised in both groups. Participants received free car parking permits for session times, otherwise received no financial or material incentives for participating in the study.
Measures
Data collection occurred at either the beginning of the first session (pre-intervention) and/or at the end of the last session (post-intervention).
a). Depression, Anxiety, Stress Symptoms 21 (DASS 21) – pre and post intervention. The DASS is a set of three self-report scales designed to measure the core negative emotional symptoms of depression, anxiety and stress.The DASS 21 is a short version of the questionnaire, containing 7 items for each domain. The DASS 21 has been shown to have high internal consistency and to yield meaningful discrimination in a variety of research and clinical settings [31].
b). Caregiving Helplessness Questionnaire (CHQ) – pre and post intervention.
A screening tool designed to assist researchers and clinicians in studying parent-child relationships from an attachment perspective, specifically disorganization of attachment. It contains three subscales including mother helplessness, mother-child frightened, and child caregiving. All three subscales have shown discriminant validity in multiple large scale studies [32].
c). Australian Treatment Outcome Project (ATOP) – pre and post intervention.
The ATOP is a single page instrument that uses client self-report responses to 24 items of drug and alcohol use.The ATOP assesses individual client status across two general domains in the preceding four weeks: substance use (including injecting behaviours); and general health, including physical, psychological, social and quality of life indicators. The ATOP has had psychometric validation in more than 300 clients across 3 OTP clinics in New South Wales, and refined in line with client and clinician feedback. The ATOP was completed by the participants’ case manager.
d). Circle of Security Parenting Questionnaire – post intervention only.
Developed in 2010 by the authors of the Circle of Security protocol, this evaluation is a 13 question qualitative feedback/satisfaction questionnaire completed by participants at the end of the COS intervention to determine the tolerability, acceptability and experiences of this group of parents to the program. Pre and post intervention measures were compared using standard statistical analysis identifying variations across a number of research variables.
Results
6 female and 2 male participants were included in the study. The mean age of participants was 36 years (range 20-54). All participants were financially supported by welfare payments, none were employed and all were of Anglo-Australian background. All participants were primary caregivers; however 4 of the participants had their child (ren) in temporary CPS custodial arrangements at the time of commencing the study. The average number of children per participant was 1.25. The average child age was 2.7 years (range = 6 months to 8 years; One participant was included with an 8 year old child in view of the participants clinical circumstances and need for parent training at the time of the study). In terms of the opiate treatment of the participants, 5 were managed on methadone with the remaining 3 on buprenorphine/naloxone. All 8 participants attended the first COS session with one participant not continuing thereafter. That participant was lost to follow up and did not complete post intervention questionnaires. One participant completed half of the program, and then voluntarily entered an inpatient rehabilitation program which required her to withdraw from continuing the study. However that participant was included in the post intervention data. The remaining 6 participants completed all 8 COS sessions with retention rate of 75% for the entire program. No mandatory notifications were made during the study period.
Parent Substance Use
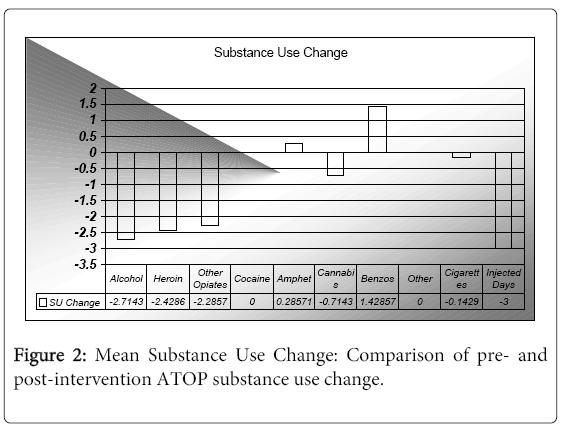
Other than alcohol, the amount of a substance used is difficult to quantify accurately as the purity and weights purchased around the country vary significantly. As such, frequency of use is accepted as the clinically measured indicator in the ATOP. The mean change in substance use frequency across the different substance categories is indicated in Figure 2. The greatest change occurred with a reduction in alcohol intake by M=-2.7143 days. The mean standard units (SU) of alcohol consumed per drinking day was M=6.4, prior to the intervention and M=4.8 after. This equates to a mean reduction of M=1.6 SU per drinking day per participant across the study period. Similarly, mean reductions in the frequency of use occurred with heroin (M=-2.4286), other opiates (M=-2.2857), and cannabis (M=-0.7143). One person stopped smoking cigarettes during the study period resulting in M=-0.1429 reduction in smoking frequency. The number of injecting days reduced by M=-3 across the study period per participant. As only 4participants indicated injecting behaviour before or during the study period, for each participant injecting drugs, the reduction in injecting days equated to 5.25 days each.
The substances that did not follow the trend of decreased use was benzodiazepines and to a lesser extent amphetamines. The increase in use was attributable to two participants who reported a relapse in use due to accommodation and physical health issues during the study.
Parental Mental Health
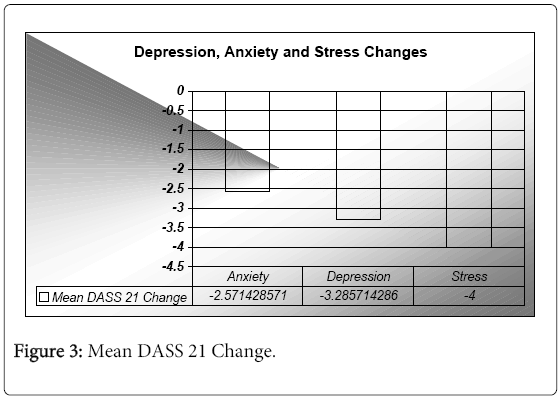
All domains on the DASS 21were reduced following the study intervention as shown in Figure 3. The stress domain showed the greatest reduction in pre- vs post- scores (M=-4, 19%), followed by the depression (M=-3.29, 16%), and then the anxiety domain (M=-2.57, 12%). A similar improvement in overall psychological health occurred on the single question rating scale in the ATOP, with an improvement by M=1.86(18.6%) following the intervention as measured on a Likert Scale from 0-10 (0=poor and 10=good).
Caregiver Reflectiveness and Empowerment
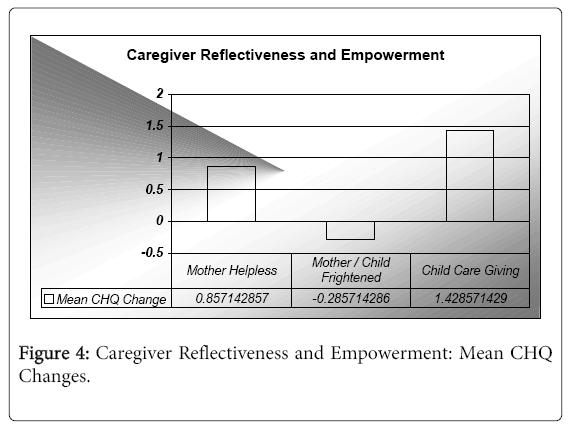
Mean changes in the CHQ pre- versus post-intervention were small, in the order of -0.3 to 1.4 from a CHQ possible change of 35 units (Figure 4). However, the only domain with a trend towards reducing pathology was the Mother/Child Frightened domain (M=-0.29, -0.008%). The domains Mother Helpless (M=0.86, 0.02%) and Child Care Giving (M=1.43, 0.04%) increased following the study intervention.
Qualitative Feedback
Overall, the participants highly rated the COS parenting program (see Table 1).The program rated highly in terms of being easily understood and in improving child-parent relationships. A majority of participants reported the program had helped to reduce their stress levels, with most being able to view their child’s behaviour differently after completing the program. Comments from participants included, “I learned to relax and take time to breathe before dealing with highly stressful situations” and “It gives me the chance to separate what are my things and what my child needs.... it gives me (a) chance to change things”
| Positive response | Neutral response | Negative response | Mean strength of response | |
| Overall Rating of COS program | 7-Jul | - | - | 0.95 |
| Easy to understand | 7-Jul | - | - | 1 |
| Reduced parental stress | 7-Apr | 7-Mar | - | 0.79 |
| Did COS affect your relationship with your child | 7-Jun | 7-Jan | - | 0.95 |
| Do you now view your child’s behaviour differently | 7-May | 7-Feb | - | 0.9 |
| Better able to identify own “Shark Music” | 7-May | 7-Feb | - | 0.9 |
| Better able to identify child’s needs | 7-Jun | 7-Jan | - | 0.95 |
| Better able to repair ruptures to carer-child relationship | 7-Apr | 7-Feb | 7-Jan | 0.71 |
| Improved reflective capacity | 7-Apr | 7-Jan | 7-Feb | 0.64 |
| Improved child behaviour | 7-Jan | 7-Jun | - | 0.71 |
| Developed improved parent abilities | 7-May | 7-Jan | 7-Jan | 0.79 |
| Ceased some old parenting behaviours | 7-Jun | 7-Jan | - | 0.93 |
| Would recommend COS to other parents | 7-Jul | - | - | 1 |
Table 1: Results from the COS Parent Feedback Questionnaire. (Mean strength of response calculated from Likert scales, 0=disagree, 1=agree).
All participants reported gaining an understanding about their own “shark music”, a program specific concept for internal signals of stressful/difficult personal emotions when parenting, whilst a majority felt they could now reflect on child behaviour and child-parent interactions. Improvements were noted in participants’ being better able to identify their child’s needs and in repairing ruptures of the parent-child relationship, eg. “I now see that she has needs and it is not about her just being naughty”.
Only one participant had noticed an improvement in their child’s behaviour since completing the program however most reported having developed new parenting abilities. All the participants indicated they would highly recommend the COS program to other parents.One parent commented, “It’s a way to help parents connect more with their child’s emotional needs and help them develop emotionally into healthy adults. It helps parents see their children better, whilst separating your own issues from what your child needs.”
Discussion
A recognised challenge in the Drug and Alcohol field is difficulties in the engagement of substance users in treatment. Although maintenance opiate programs provide a unique opportunity for clients to interface with health services, their daily contact is often only fleeting and superficial. In a review of maternal engagement in 6 different parenting based programs for drug-dependent mothers, Suchman et al [33] identified that all programs had difficulty in engaging mothers in treatment. In this pilot study, retention rates across the 8 week program were excellent. The high retention rate and positive qualitative feedback in this study suggests that this patient subpopulation has the potential to readily accept and engage in the COS short version format. An important measure of any novel intervention is that it must do no harm. In this study, no mandatory CPS reports occurred during the intervention and the improvements in substance use and depression, stress and anxiety symptoms suggest that the program does not cause harm to participants or to children. The participants strongly endorsed the program and highly recommended it to other parents.
Previous parenting studies of drug-dependent mothers have shown that interventions can play an important role in the reduction of maternal drug abuse and other behaviours that are harmful to their children and families, as well as themselves [33-35]. This study demonstrated a trend towards reducing use of alcohol, heroin, other opiates and the frequency of injecting behaviours of participants, while a small increase in amphetamine and larger benzodiazepine use was limited to two participants. The reasons for the overall trend towards reducing substance use frequency (and alcohol quantities) are likely to be multi-factorial but may in part be attributable to the reduction in corresponding stress, anxiety and depression levels reported by participants. Previous studies have demonstrated that maternal substance abuse severity and psychological maladjustment were the strongest predictors of children’s out-of-home placement [33]. Although one third of participants had children in out-of-home placement, this pilot study builds on previous studies that interventions that reduce substance use and enhance caregiver mental health may improve child related outcomes.
In addition, the impact of more positive parenting experiences for caregivers may alter reward neurobiology to reduce substance use levels [33]. Many substances of abuse have been shown to affect neurotransmitter pathways and areas in the brain associated with initiation of behaviour, hedonic reward and motivation [36,37]. These central pathways, especially dopaminergic systems, are also thought to be critically involved in a parent’s capacity to invest in the care of their children [38]. The importance of treatment interventions that focus on helping parents invest in their children through a securely attached relationship, rather than substances that subsume similar neurobiological pathways, may “reset” the focus of the reward system [39,29]. If parenting satisfaction were to assist in shifting reward focused patterns of behaviour, specifically substance use, then parenting interventions focused on enhancing positive child-parent interactions such as the COS program, may provide a novel intervention in the armament of substance use disorder treatments.
Past parenting intervention studies with substance dependent mothers have not shown significant measurable changes in mother-child interactions [33]. This COS pilot study also demonstrated no clinically significant change in career-child interactions by way of the CHQ.A number of reasons may account for this. The CHQ [32] utilises the concept of maternal helplessness when thinking about the underlying representational and behavioural associated with disorganized attachment, an extreme end of insecure attachment. The small sample size may be reflected in the absence of disorganized attachment in the study group. The temporal nature of measuring attachment variables may also be an important contributor to the study’s CHQ findings. Indeed, an initial increase in Carer Helplessness may reflect a heightened reflective capacity by parents of attachment difficulties. Limited reported change in child behaviour by participants at the completion of the study may also indicate the need for time in significantly changing parent-child interaction and therefore further studies may warrant serial or delayed attachment measures for meaningful results and conclusions to be drawn.Further research of the COS would warrant careful selection of more sensitive, perhaps multiple, attachment measures conducted beyond the delivery and completion of the program.
The program was easy to provide, has reported high fidelity of delivery [25] and in this opiate dependent caregiver group was well received. The availability of the program throughout Australia is increasing, and this high needs, vulnerable group of parents and children, appear to benefit from the program. Previous studies focused on attachment with substance abusing parents suggest a possible intergenerational effect consistent with the theoretical underpinnings of Bowlby’s (1982) concept of attachment [33]. These studies suggest that early caregiving experiences play an important role in directly shaping mothers’ substance abusing behaviour and comorbid psychopathology, and in directly and indirectly influencing the continuity of parenting styles. The longer term, preventative role that this program may affect is unknown and warrants further longitudinal investigation.
Finally, Velleman and Templeton [40] have noted that “many child care practitioners have told us that they lack the skills to work with substance-misusing parents ...” and “strangely, many practitioners in substance misuse services tell us the converse: that they do not have the skills to work with children and the wider family to the same purpose”. Beyond the common therapeutic techniques common to both groups of health professionals, that is, empathy, developing therapeutic alliances, exploration of difficulties, setting achievable goals, and empowering individuals, specific parenting programs such as COS, provide a valuable bridge of the two health care settings for this vulnerable group of parents and children in the community.
Limitations
The study has many limitations as it a pilot study and thus is statistically limited by the small sample size and therefore is under powered to draw conclusions with confidence. In addition, it is difficult to determine the significance of single measure trends. Alternate cross validating measures that have been used in similar attachment intervention studies may be more appropriate in future studies. They could also be repeated at longer intervals to determine the strength and stability of any change. Furthermore, the study did not provide detailed demographics of the study population, and therefore the results are not generalized to representative clinical groups.However, as the intervention has never been studied in this population, the pilot suggests that further research is warranted including a randomised control trial to determine effect size considering the positive trends in participant feedback and quantitative study results.
The measures used in the study provide only general, broad indices of the study hypotheses. Furthermore, the CHQ has been designed for caregivers (specifically mothers) with children between 3 and 11 years whilst in this study the mean age of children was 2.7 years and for those with disorganized attachment. Careful consideration and selection of sensitive measures of attachment are required for future studies.
Finally, the study only included participants who were opiate dependent and in a maintenance program, therefore the results are not generalizable to the broader substance using population. Significant differences exist between (eg opiate versus alcohol) and within (eg binge pattern versus dependent) substance type subpopulations. However, the study was representative of clinical group of opiate dependent parents including both stable and unstable substance use circumstances [41,42].
Conclusion
The COS (short version) program is a widely available, evidence based attachment parenting program that appears to be well tolerated by opiate dependent caregivers of young children. Although highly operationalised, the program provides valuable advice, guidance and experience to substance using parents, perhaps benefiting them in improving their caregiving capacities’, whilst reducing their stress, depression and anxiety levels when caring for young children. These findings were also associated with a reduction in the frequency and quantities of some substances used in this caregiver groups. This pilot study has provided valuable information suggesting that further research in attachment parenting, specifically the COS program, should be conducted in this vulnerable and high need group.
References
- Ammerman RT, Kolko DJ, Kirisci L, Blackson TC, Dawes MA (1999) Child abuse potential in parents with histories of substance use disorder. Child Abuse Negl 23: 1225-1238.
- Dawe S and Harnett P. (2007). Reducing potential for child abuse among methadone-maintained parents: Results from a randomised controlled trial. Journal of Substance Abuse Treatment. Vol 32, pp.381-390
- Suchman NE, McMahon TJ, Zhang H, Mayes LC, Luthar S (2006) Substance-abusing mothers and disruptions in child custody: an attachment perspective. J Subst Abuse Treat 30: 197-204.
- Taplin S and Mattick R (2011) Child Protection and Mothers in Substance Use Treatment. Technical Report Number 320, NDARC: Randwick
- McKeganey N, Barnard M and McIntosh J (2002) Paying the price for their parents’ addiction: meeting the needs of the children of drug-using parents. Drugs: Education, prevention and policy. Vol 9(3), pp.233-246
- Bauman PS and Dougherty FE (1983) Drug-addicted mothers’ parenting and their children’s development. International Journal of the Addictions, Vol 18, pp.291-302
- Bauman PS and Levine SA (1986) The development of children of drug addicts. International Journal of the Addictions. Vol 21, pp.849-863
- Kandel D (1990). Parenting styles, drug use and children’s adjustment in families of young adults. Journal of Marriage and the Family. Vol 52, pp.183-196
- Luthar SS and Suchman NE (2000) Relational psychotherapy mother’s group: A developmentally informed intervention for at-risk mothers. Development and Psychopathology. Vol 12, pp.235-25
- Barnard M, McKeganey N (2004) The impact of parental problem drug use on children: what is the problem and what can be done to help? Addiction 99: 552-559.
- Quinlivan JA, Evans SF (2005) Impact of domestic violence and drug abuse in pregnancy on maternal attachment and infant temperament in teenage mothers in the setting of best clinical practice. Arch WomensMent Health 8: 191-199.
- Shieh C, Kravitz M (2002) Maternal-fetal attachment in pregnant women who use illicit drugs. J ObstetGynecol Neonatal Nurs 31: 156-164.
- Kumpfer KL, Fowler MA (2007) Parenting skills and family support programs for drug-abusing mothers. Semin Fetal Neonatal Med 12: 134-142.
- Murray L, Fiori-Cowley A, Hooper R, Cooper P (1996) The impact of postnatal depression and associated adversity on early mother-infant interactions and later infant outcome. Child Dev 67: 2512-2526.
- Lyons-Ruth K (2008) CONTRIBUTIONS OF THE MOTHER-INFANT RELATIONSHIP TO DISSOCIATIVE, BORDERLINE, AND CONDUCT SYMPTOMS IN YOUNG ADULTHOOD. Infant Ment Health J 29: 203-218.
- Catalano RF, Gainey RR, Fleming CB, Haggerty KP, Johnson NO (1999) An experimental intervention with families of substance abusers: one-year follow-up of the focus on families project. Addiction 94: 241-254.
- Schuler ME, Nair P, Black MM (2002) Ongoing maternal drug use, parenting attitudes, and a home intervention: effects on mother-child interaction at 18 months. J Dev BehavPediatr 23: 87-94.
- Nair P, Schuler M and Black MM (2003) Cumulative environmental risk in substance abusing women: Early intervention, parenting stress, child abuse potential, and child development. Child Abuse and Neglect. Vol 27, pp.997-1017
- Duggan A, MacFarlan E, Fuddy L, Burrell L, Higman S, Windham A et al (2004). Randomised trial of a statewide homevisiting program: impact in preventing child abuse and neglect. Child Abuse and Neglect. Vol 28, pp-597-622
- Harnett PH and Dawe S (2008) Reducing child abuse potential in families identified by social services: Implications for assessment and treatment. Brief Treatment and Crisis Intervention. Vol 8(3), pp.226-235
- Suchman NE, Mayes L, Conti J, Slade A and Rounsaville B (2004). Rethinking parenting interventions for drug dependent mothers: From behaviour management to fostering emotional bonds. Journal of Substance Abuse and Treatment.Vol 27, pp.179-185
- Suchman NE, DeCoste C, Leigh D, Borelli J (2010) Reflective functioning in mothers with drug use disorders: implications for dyadic interactions with infants and toddlers. Attach Hum Dev 12: 567-585.
- Cassidy J, Poehlmann J, Shaver PR (2010) An attachment perspective on incarcerated parents and their children. Attach Hum Dev 12: 285-288.
- CohenNJ, Muir E, Lojkasek M, Muir R, Parker CJ, Barwick M and Brown M Watch, wait and wonder:Testing the effectiveness of a new approach to mother-infant psychotherapy. Infant Mental Health Journal. Vol 20, pp.429-451
- Hoffman, K.T., Marvin, R.S., Cooper, G. and Powell, B. (2006). Changing toddlers’ and preschoolers’ attachment classifications: the Circle of Security Intervention. Journal of Consulting and Clinical Psychology. Vol 74, pp. 1017-1026
- Cooper G, Hoffman KT, Powell B and Marvin R (2005) The Circle of Security intervention: Differential diagnosis and differential treatment. In L.J. Berlin, Y. Zin, L.M. Amaya-Jackson and M.T. Greenberg (Eds.), Enhancing early attachments: Theory, research, intervention, and policy (pp.127-151). New York: Guilford Press
- Toth SL, Rogosch FA, Manly JT and Cicchetti D (2006) The efficacy of toddler-parent psychotherapy to reorganize attachment in the young offspring of mothers with major depressive disorder: A randomised preventive trial. Journal of Consulting and Clinical Psychology. Vol 74, pp.1006-1016
- Llewellyn G, McConnell D, Ferronato L (2003) Prevalence and outcomes for parents with disabilities and their children in an Australian court sample. Child Abuse Negl 27: 235-251.
- Delfabbro P, Borgas M, Rogers N, Jeffreys H& Wilson R (2009) The social and family backgrounds of infants in South Australian out-of-home care 2000-2005: Predictors of subsequent abuse notifications. Children and Youth Services Review. Vol31(2), pp.219-226
- Zhou AZ&ChilversM (2010) Infants in Australian out-of-home care. British Journal of Social Work.Vol 40(1), pp.26-43
- Ng F, Trauer T, Dodd S, Callaly T, Campbell S &Berk M (2007)The validity of the 21-item version of the Depression Anxiety Stress Scales as a routine clinical outcome measure.ActaNeuropsychiatrica. 19, 304-310.
- Solomon J and George CC (2011) Disorganised Attachment and Caregiving (pp.133-166). New York: Guilford Press
- Suchman N, Pajulo M, Decoste C, Mayes L (2006) Parenting Interventions for Drug-Dependent Mothers and Their Young Children: The Case for an Attachment-Based Approach. FamRelat 55: 211-226.
- Luthar SS and Suchman NE (2000) Relational psychotherapy mother’s group: A developmentally informed intervention for at-risk mothers. Development and Psychopathology. Vol 12, pp.235-25
- Moore J, Finkelstein N (2001) Parenting services for families affected by substance abuse. Child Welfare 80: 221-238.
- Koob GF (1996) Hedonic valence, dopamine and motivation. Mol Psychiatry 1: 186-189.
- Koob GF, Le Moal M (1997) Drug abuse: hedonic homeostatic dysregulation. Science 278: 52-58.
- Edelman, G.M. and Tononi, G. (1995). Neural Darwinism: The brain as a selectional system. In J. Cornwell (Ed.), Nature’s imagination: The frontiers of scientific vision (pp.78-100). New York: Oxford University Press
- Pajulo M, Suchman N, Kalland M and Mayes LC (2006) Enhancing the effectiveness of residential treatment for substance abusing pregnant and parenting women: focus on maternal reflective functioning and mother-child relationship. Infant Mental Health Journal. Vol 27(5), pp.448-65.
- Velleman R and Templeton L (2007) Understanding and modifying the impact of parents’ substance misuse on children. Advances in Psychiatric Treatment. Vol 13, pp.79-89
- Chaffin M, Kelleher K, Hollenberg J (1996) Onset of physical abuse and neglect: psychiatric, substance abuse, and social risk factors from prospective community data. Child Abuse Negl 20: 191-203.
- Gillath O, Bunge SA, Shaver PR, Wendelken C, Mikulincer M (2005) Attachment-style differences in the ability to suppress negative thoughts: exploring the neural correlates. Neuroimage 28: 835-847.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 15978
- [From(publication date):
December-2014 - Aug 18, 2025] - Breakdown by view type
- HTML page views : 11346
- PDF downloads : 4632