Case Report Open Access
An Unusual Mass at the Colonic Splenic Flexure
Salih Samo* and Srinadh Komanduri
Northwestern University Feinberg School of Medicine, 333 East Ontario Street, Unit 4205, Chicago, IL 60611, USA
- Corresponding Author:
- Salih Samo, MD
Northwestern University Feinberg School of Medicine
Address: 333 East Ontario Street
Unit 4205, Chicago, IL 60611, USA
Tel: 18479979233
E-mail: salihsamo@hotmail.com
Received Date: March 16, 2016; Accepted Date: March 26, 2016; Published Date: March 31, 2016
Citation: Samo S, Komanduri S (2016) An Unusual Mass at the Colonic Splenic Flexure. J Gastrointest Dig Syst 6:406. doi:10.4172/2161-069X.1000406
Copyright: © 2016 Sam S, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
Large bowel obstruction is less common that small bowel obstruction and constitutes about 25% of intestinal obstruction. Chronic functional bowel obstruction can lead to fecal impaction and subsequent fecaloma formation.
Keywords
Splenic flexure; Fecaloma; Constipation
Introduction
Large bowel obstruction is less common that small bowel obstruction and constitutes about 25% of intestinal obstruction [1]. Chronic functional bowel obstruction can lead to fecal impaction and subsequent fecaloma formation. We report a case of large bowel obstruction secondary to a large fecal mass at an unusual place at the colonic splenic flexure that was initially concerning for malignancy.
Case Information
A 56 year-old female with history of irritable bowel syndrome, polymyositis and chronic intestinal pseudo-obstruction (on chronic total parenteral nutrition) presented with 2-week duration of left lower quadrant abdominal pain, nausea, vomiting, and diarrhea (dark green stools).
She also reported a history of chronic constipation and narcotics use for her chronic hip pain. Abdominal examination was notable for left lower quadrant tenderness and a left upper quadrant palpable mass.
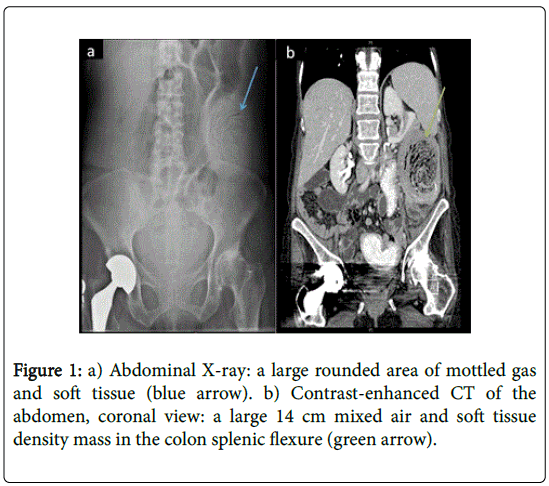
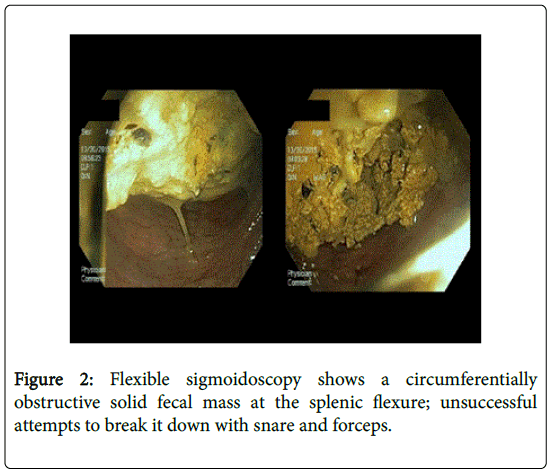
Abdominal X-ray showed, in addition to a few air filled dilated bowel loops consistent with partial bowel obstruction, a large mass in the left hemi-abdomen suspicious for malignancy (Figure 1a, blue arrow). A contrast-enhanced computed tomography (CT) scan of the abdomen showed diffuse dilatation of the proximal and mid small bowel with decompression of more distal loops; it also showed a large 14 cm mixed air and soft tissue density mass in the colonic splenic flexure (Figure 1b, green arrow). Flexible sigmoidoscopy revealed circumferentially obstructive solid fecal mass at the splenic flexure (Figure 2) with unsuccessful attempts to break it down with snare and forceps.
Patient received multiple laxative and stool softener regimens without improvement; repeat flexible sigmoidoscopy did not reveal any significant change in the size of the fecal mass. A repeat abdominal CT scan showed worsening of the colonic obstruction proximal to the fecal mass with a new transition point.
After failed medical and endoscopic management, she underwent surgical removal of the fecal mass, sigmoidectomy with diverting loop ileostomy. She was eventually discharged to a rehabilitation institution.
Discussion
Fecaloma is an organized intraluminal fecal mass that is formed secondary to prolonged retention of fecal residue. Fecaloma is the most severe form of fecal impaction in predisposed individuals [2] and mfost commonly found in the recto-sigmoid area as stool becomes more consolidated due to decreased fluid content in the distal colon [3]. The unusual site of the fecal mass at the colonic splenic flexure in this case was initially concerning for malignancy. Fecaloma may lead to specious diarrhea, bowel obstruction [4], stercoral colon ulceration and perforation [5], and urinary tract obstruction and hydronephrosis [6]. Surgical removal with limited or more extensive resection is required when conservative management fails to adequately remove fecalomas. The chronic pseudo-obstruction and low colonic transit in addition to chronic narcotic use in the patient in this case likely predisposed her to chronic fecal impaction and subsequently developing large fecaloma.
References
- Markogiannakis H, Messaris E, Dardamanis D, Pararas N, Tzertzemelis D, et al. (2007) Acute mechanical bowel obstruction: clinical presentation, etiology, management and outcome. World J Gastroenterol 13: 432-437.
- Aiyappan SK, Ranga U, Samraj A, Rajan SC, Veeraiyan S (2013) A case of fecaloma. Indian J Surg 75: 323-324.
- Saksonov M, Bachar GN, Morgenstern S, Zeina AR, Vasserman M, et al. (2014) Stercoral colitis: a lethal disease-computed tomographic findings and clinical characteristic. J Comput Assist Tomogr 38: 721-726.
- Yoo HY, Park HW, Chang SH, Bae SH (2015) IlealFecaloma Presenting with Small Bowel Obstruction. Pediatric gastroenterology, hepatology& nutrition 18: 193-196.
- Kwag SJ, Choi SK, Park JH, Jung EJ, Jung CY, et al. (2013) A stercoral perforation of the rectum. Annals of coloproctology 29: 77-79.
- Park JS, Park TJ, Hwa JS, Seo JH, Park CH, Youn HS (2013) Acute Urinary Retention in a 47-month-old Girl Caused by the Giant Fecaloma. Pediatric gastroenterology, hepatology& nutrition 16: 200-205.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 19634
- [From(publication date):
April-2016 - Aug 24, 2025] - Breakdown by view type
- HTML page views : 18729
- PDF downloads : 905