Make the best use of Scientific Research and information from our 700+ peer reviewed, Open Access Journals that operates with the help of 50,000+ Editorial Board Members and esteemed reviewers and 1000+ Scientific associations in Medical, Clinical, Pharmaceutical, Engineering, Technology and Management Fields.
Meet Inspiring Speakers and Experts at our 3000+ Global Conferenceseries Events with over 600+ Conferences, 1200+ Symposiums and 1200+ Workshops on Medical, Pharma, Engineering, Science, Technology and Business
Research Article Open Access
Ayurveda a Boon for Epileptics
| Avinash Shankar1*, Amresh Shankar2 and Anuradha Shankar2 | |
| 1National Institute of Health & Research, Bihar, India | |
| 2Centre for Indigenous Medicine & Research, Bihar, India | |
| Corresponding Author : | Dr. AvinashShankar Chairman, National Institute of Health & Research (RA. Hospital & Research Centre) Warisaliganj (Nawada), Bihar, 805130 India E-mail: dravinashshankar@gmail.com |
| Received August 21, 2013; Accepted September 25, 2013; Published September 27, 2013 | |
| Citation: Shankar A, Shankar A, Shankar A (2013) Ayurveda a Boon for Epileptics. J Homeop Ayurv Med 2:134. doi: doi: 10.4172/2167-1206.1000134 | |
| Copyright: © 2013 Shankar A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Traditional Medicine & Clinical Naturopathy
Abstract
Apsmar denotes epilepsy, that usually persists in majority of patients with mental debility and disability, in spite of multidrug therapy with advanced anti-epileptics. But by supplementing Sodium valproate with indigenous composite of some Indian herbs as an adjuvant at 8 hourly dosing, tends to modulate the therapeutic outcome positively due to bioregulation of altered GABA bio kinetics and neurogenic action. Thus this adjunction seems a boon in epilepsy management.
| Keywords | |
| Epilepsy; Convulsions; Apsmar; Seizure; Neuronal disorder | |
| Introduction | |
| Apsmar, an Indian equivalent of Epilepsy, duly documented in vedic and post vedic literature of Charak and Sushrut 1000 BC is a non specific manifestation of hyper (synchronous discharge of cortical neurons and its prevalence in developing country is 57 in thousand, while in developed country like America and South Africa it is very high. Even in India also, incidences are increasing in geometric progression [1]. | |
| It is a complex brain disorder associated with both mental and physical debility, occurrence of recurrent convulsions causes neural hypoxia resulting in neuronal disorder or degeneration [2]. | |
| Improper drug scheduling among epileptics promote resistance to the receptor site causing recurrence even with wide range of available antiepileptic drugs such as; Phenobarbitone, Phenytoin, Sodiumvalproate, Carbamazepine, Ethosuccimide, Folvamate, Gabapentine, Labotegu, Oxycarbamazepine, Toperonoid, Tiagevin, Zenisonide, Tectal, Lamotrigine, Lavetiraceton, Pregabalin etc. But, non ensure complete cure of the disease except transient control of the seizure. | |
| Almost one third of the people with epilepsy continue to have seizure (s) despite appropriate therapy with above mentioned drugs and possess considerable risk of cognitive and psychosocial dysfunction and increased health risk among the resistant epileptics. Mono therapy facilitates drug compliance, associated with lower risk of toxicity, affordability and regularity with minimized drug untoward effects. | |
| Considering the IHO study of status of epilepsy patient taking treatment through an NGO Sanchar Kolkata and London epilepsy forum, majority cases presented with physical and mental debility in 90% cases while physical and mental handicap in 46%. | |
| Hence a study was conducted to evaluate an indigenous composite as an adjuvant with conventional antiepileptic mono therapy in proper schedule to assess the therapeutic efficacy and safety profile [3]. | |
| Materials and Methods | |
| To evaluate the clinical efficacy of an indigenous composite as an adjuvant with widely prescribed antiepileptic monotherapy and study the status of old epileptic cases, a mass propaganda to create awareness for epilepsy patient in a multi centre epilepsy treatment camp was organized and 4568 cases of grand mal epilepsy were selected, duly interrogated (both patient and their parent), evaluated, investigated ,treated and follow-up observation was given by Centre For Indigenous Medicine & Research, RA. Hospital & Research Centre and Indian epilepsy forum. | |
| Patients of convulsive disorder with associated other systemic diseases, patients of status epileptics and patients unable to follow the therapeutic and follow up schedule were excluded from the study. | |
| Patient’s non responsive to major therapeutics are termed resistant epileptics. | |
| All the selected patients were investigated for CT scan, EEG, Hematological index and biochemical parameters to evaluate safety profile of the prescribed drug. | |
| Irrespective of the disease duration, age of the patient, status of illness and previous therapeutics, all patients were given: | |
| • Sodium valproate in recommended dose at 8 hourly schedule, strictly. (We practiced/administered doses at 6 AM, 2 PM and 10 PM) | |
| • Indigenous composite containing (equal portions of ) | |
| - Acorus calamus (rhizome) | |
| - Nardostachys jatamanshi (root) | |
| - Convolvulus pluricaulis | |
| - Herpestis monneiri (leaf) | |
| - Crotalaria verrucosa (seed) | |
| Dose: For adult: 1 cap of 500mg daily, while in children a 1/8th decoction 5 ml in >5 yrs; <5 yrs 2.5 ml; <1 year 1.25 ml every 12 hours. | |
| Patients were examined and data were recorded in a follow up card. | |
| Initially, weekly for 1st month, every 15th day for next 6 months and monthly for rest of the period during the therapy and every 3 month for 2 yrs post therapy follow up during the follow up, patients were evaluated for- | |
| • incidence of attack of seizure | |
| • frequency of seizure | |
| • duration of seizure | |
| • severity of seizure | |
| • any untoward effect | |
| • physical and mental status | |
| To ensure 100% follow up with an instruction to the parent of the patient to enter the requisite information and observation in the follow up card. | |
| To assess safety profile, patients were re-examined for hemato, hepato and renal status. | |
| Therapeutic response was adjudged, analyzed and graded as per following index (Table 1). | |
| Observations | |
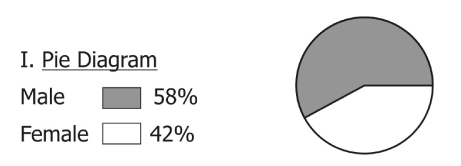
| • 4658 Patients of age range 5-40 years were selected for the present study. Among them 58% (2680) were male and rest female; 40.57% of all patients were of age group 10-20 years (Figure 1 and Table 2). | |
| • Whereas disease status wise, 55.38% were recently detected, 38% were old cases of epilepsy without treatment, among them 21.9% patients were suffering from the past 1 year and others were 1-5 years old. Remaining 6.62% of patients were suffering from recurrent episodes of epilepsy in spite of a therapeutic regime (Figure 2 and Tables 3 and 4). | |
| • As per clinical presentation 13% patients were presenting with convulsion, unconsciousness, frothing and autonomic dysfunction while old resistant cases (21%) were presenting with associated physical and mental debility (Table 5). | |
| • Among selected patients 42.01% were with hemoglobin less or equal to 10gm%, 1.05% with altered hepatic and 1.24% with altered renal functions (Table 6). | |
| • All newly detected cases, 96.2% of old cases and 67% of chronic resistant cases had complete cessation of epileptic attack from beginning of therapy while 23% of old cases failed to respond within 48 hours but slowly severity, frequency and duration of convulsion regressed markedly. No patient exhibited autonomic dysfunction. | |
| • Overall 99.76% patients revealed improved mental status in terms of psychosocial behavior and intelligence (mental ability) while 0.23% (11 cases) or 3.53% of resistant cases showed no change in their mental status but all had improved physical status. | |
| • No post therapy recurrence of seizure was reported during 2 years follow-up observation | |
| • All newly detected cases, 96.20% of old patients and 67.52% of resistant cases had grade I clinical response while 3.8% of old and 21.8% of resistant cases had grade II response and 4.18% of resistant cases failed to respond. | |
| • The abnormal hemato, hepato and renal parameters of some old patients with refractory epilepsy were sustained or improved but not worsened (Table 7). | |
| Discussion | |
| Medical literature and study shows that available antiepileptic fails to ensure cure and prevent recurrent intense and repeated attack of seizure associated with physical and mental debility due to hypoxia, loss of GABA mediated inhibition of dentate granule and death of GABAergic inhibitory neuron results in attenuation of inhibitory control which in turn results in hyper excitation of the remaining neuron of the hippocampus. In spite of the fact that GABA neurons are more resistant to seizure induced neuronal death than other hippocampus neurons. Mossy cells (located in dentate hilus, a part of hippocampus) are extremely sensitive to seizure induced neuronal death and damage following intense synaptic activator i.e., excite-tonic mechanism of activator of NMDA (N methyl D aspartate) a sub type of glutamate receptor which results in excessive intracellular calcium. | |
| Release of cellular zinc attenuate GABA response and induce hyper -excitability of neurons. | |
| GABA binds to GABA-A (coupled to calcium/chloride channel and a main target of currently prescribed drugs) as excitatory post synaptic potential are the main form of communication between neurons and is mediated by release of excitatory amino acid-Glutamate from presynaptic elements which is mediated by | |
| - NMDA (N methyl D aspartic acid/aspartate) | |
| - AMPA(Alpha-amino-3 hydroxy 5 methyl isoxazole propionic acid) kinate | |
| - Metabotropic | |
| GABA-B (Couples to potassium channel, a cause of latency and long duration of action) located in pre-synaptic element of an excitatory pre-neuron and inhibits pre-synaptic neuron by | |
| - direct induction of IPSP | |
| - inhibition of release of excitatory neuro transmitters [4,5] | |
| Hence clinical supremacy of the adjunct indigenous composite with Sodium valproate mono drug therapy can be attributed to bioregulative action of indigenous composites active ingredients for GABA neurodynamics i.e., Nardostachys jatamansi (Jatamansin, Jatamanose, Nardostachine) Herpestis monnieri(Monnerein) bio regulate GABA biokinetics and act in synergism with Sodium valproate and prompt control of the seizure, while Acorus calamus (Acorin, Beta asarone and calaminidine) and Crotolaria verrucosa (crotallidine and verrucosin) acts as a neurogenic and helps in regeneration and repair of damaged neuron due to epileptic attacks thus improve and check neural debility and alleviate physical disability . | |
| In addition Convolvulus pluricaulis (Covolvulin) and Herpestis monnieri (Bacoside A & B) both promote neural growth due to activation of nerve growth factor-Tyrosine kinase A receptor, preserve m RNA level of muscarnic receptors and check accumulation of lipid and protein damage ,thus improve both mental ability and capability [6]. | |
| Hence bioregulation of altered GABA neuro kinetics prompt non recurrence of seizure even after drug withdrawal and neurogenic action improve mental capability and physical capability. | |
References
|
|
Tables and Figures at a glance
| Table 1 | Table 2 | Table 3 | Table 4 |
| Table 5 | Table 6 | Table 7 |
Figures at a glance
 |
 |
| Figure 1 | Figure 2 |
Post your comment
Relevant Topics
- Acupuncture Therapy
- Advances in Naturopathic Treatment
- African Traditional Medicine
- Australian Traditional Medicine
- Chinese Acupuncture
- Chinese Medicine
- Clinical Naturopathic Medicine
- Clinical Naturopathy
- Herbal Medicines
- Holistic Cancer Treatment
- Holistic health
- Holistic Nutrition
- Homeopathic Medicine
- Homeopathic Remedies
- Japanese Traditional Medicine
- Korean Traditional Medicine
- Natural Remedies
- Naturopathic Medicine
- Naturopathic Practioner Communications
- Naturopathy
- Naturopathy Clinic Management
- Traditional Asian Medicine
- Traditional medicine
- Traditional Plant Medicine
- UK naturopathy
Recommended Journals
Article Tools
Article Usage
- Total views: 18853
- [From(publication date):
November-2013 - Sep 03, 2025] - Breakdown by view type
- HTML page views : 14157
- PDF downloads : 4696
