Bilateral Adrenal-Renal Fusion: A Radiological Diagnosis
Received: 16-May-2018 / Accepted Date: 04-Jun-2018 / Published Date: 11-Jun-2018 DOI: 10.4172/2167-7964.1000298
Abstract
In normal anatomy, the kidneys and adrenal glands are contained within the renal fascia and separated by a connective tissue capsule derived from mesenchymal tissue. Incomplete encapsulation can occur during embryonic development, resulting in adrenal-renal fusion. The true incidence of this developmental anomaly is unknown, as it has primarily been described in the literature following incidental detection on surgical or histological examination.
We report the first documented case of bilateral adrenal-renal fusion, diagnosed radiologically.
Keywords: Thorax; Abdomen; Pelvis; Pelvic MRI
Case Report
A 55 year old man with a past medical history of HIV presented with increased urinary frequency and haematuria. Physical examination revealed no abdominal tenderness or masses. He was thought to have prostatism and was referred for a pelvic MRI, which showed thickening of the bladder wall. Cystoscopy and bladder biopsy confirmed the presence of a mostly papillary but partly solid high grade (grade 3) urothelial carcinoma, pT2 at least with further prostatic urethral biopsies showing invasive urothelial carcinoma pT1 at least.
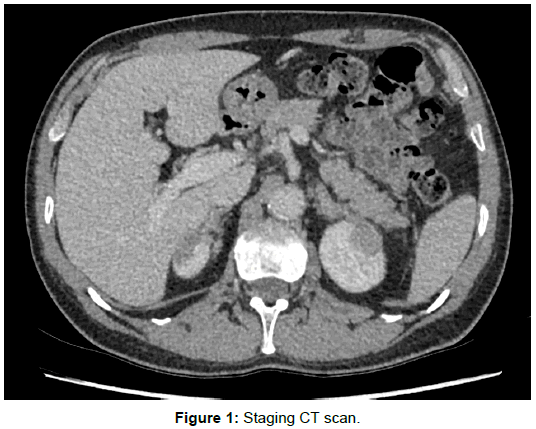
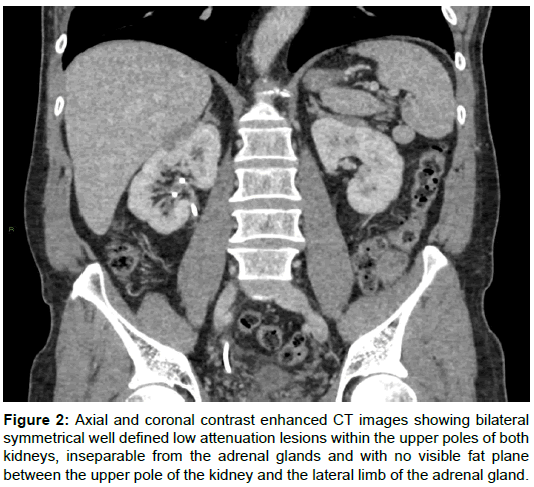
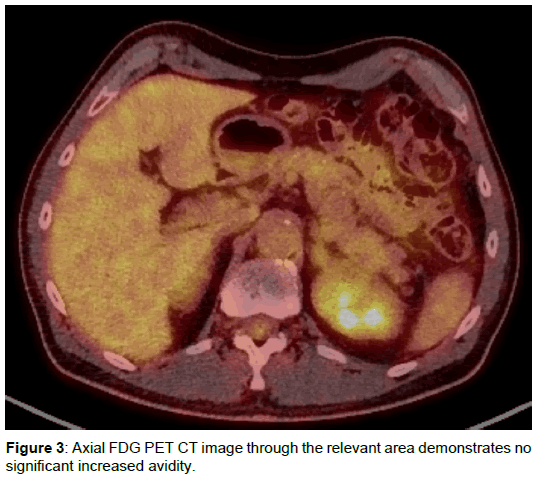
A staging CT scan of the thorax, abdomen and pelvis showed no definite metastases although note was made of a nodular appearance of the adrenal glands and symmetrical well-defined low attenuation subcapsular lesions at the upper poles of both kidneys, each measuring 2.3 cm (Figure 1). On review of the multiplanar image reformats, there was no demonstrable fat plane between the renal lesions and the lateral limbs of the adrenal glands (Figure 2). These appearances were thought to represent incidental congenital adrenal-renal fusion. An FDG PET-CT scan was performed to exclude adrenal metastases and showed low grade tracer uptake within the body of the adrenal glands bilaterally in keeping with adrenal hyperplasia but no abnormal uptake to suggest malignancy (Figure 3). Increased tracer uptake was noted in a right external iliac lymph node suggestive of metastasis. No other developmental abnormality was detected.
Figure 2: Axial and coronal contrast enhanced CT images showing bilateral symmetrical well defined low attenuation lesions within the upper poles of both kidneys, inseparable from the adrenal glands and with no visible fat plane between the upper pole of the kidney and the lateral limb of the adrenal gland.
The patient underwent neo-adjuvant chemotherapy, followed by radical cysto-prostatectomy and lymph node clearance for his bladder cancer. A repeat FDG PET-CT performed following neo-adjuvant chemotherapy showed unchanged appearances of the adrenal glands, providing further reassurance that this did indeed represent a benign anatomical variant. The uptake in the right pelvis node was felt to be indeterminate on this repeat image. It was not deemed ethical to obtain a tissue sample as the imaging appearances were felt to be classical and the patient will undergo regular surveillance CTs following his bladder cancer treatment. The pathology from the cysto-prostatectomy showed residual tumour with histological staging ypT3a ypN1 transitional cell carcinoma, with 1/5 lymph nodes on the right and 0/6 lymph nodes on the left involved.
Discussion
The adrenal gland is formed of two embryologically-distinct layers: the cortex and medulla. The adrenal cortex is derived from mesoderm and the medulla originates from neural crest cells. Around 52 days post-conception, the adrenal gland begins to separate from the mesenchymal cells and becomes encapsulated by fibrous tissue [1]. Adrenal-renal fusion was first described by Rokitansky in 1855 [2], who differentiated between congenital lesions and those acquired following inflammation of the peri-renal fat. The congenital form is considered to be caused by failure of the retroperitoneal mesenchymal cells to stimulate capsule formation [3]. Consequently, capsule formation is incomplete, and the adrenal gland and kidney become conjoined. The aetiology of adrenal-renal fusion is not known, but it is likely to be a local event around 52 days post-conception, due to the absence of other congenital abnormalities [4].
While isolated adrenal-renal fusion is a benign diagnosis with no clinical implications, there are several case reports in which the radiological appearances have been misinterpreted, particularly when there is a concurrent adrenal lesion, and have resulted in unnecessary surgery. In 2004, Fan et al. reported, an intra-operative frozen-section misdiagnosed histologically as a renal cystic mass, leading to a radical nephrectomy. Post-operatively, when the en bloc specimen was reviewed, adrenal-renal fusion and adrenal adenoma were diagnosed [5]. In 2009 Mahadevia et al. described a case of an adrenal adenoma with adrenal-renal fusion which was misdiagnosed as an invasive renal cell carcinoma, resulting in an adrenalectomy and partial nephrectomy [6]. The only previous case study not to have been diagnosed histologically was the intra-operative diagnosis by Boll et al. based on the lack of a vascular plane between the renal and adrenal capsule [7], which negated the need for a larger resection.
Adrenal-renal fusion is considered difficult to diagnose radiologically, and the imaging appearances described in the existing literature have been observed retrospectively. The characteristic findings are lack of a discrete fat plane between the upper pole of the kidney and adrenal gland, with or without a contiguous well-defined lesion within the adjacent kidney. The routine use of thin-slice CT image acquisition and multi-planar reformats in the last 10-15 years allows better detection of an absent fat plane, although this finding is not specific for adrenal-renal fusion and in unilateral cases is it difficult to exclude an invasive renal, adrenal or retroperitoneal lesion. Furthermore, artefactual degradation of images from diaphragmatic motion can limit evaluation of the peri-renal region. In this particular case, the striking symmetry of the appearances, well-defined margins of the sub-capsular renal lesions and lack of suspicious uptake on PETCT allowed a confident radiological diagnosis to be made.
Conclusion
We believe this is the first reported case of bilateral adrenalrenal fusion and adds to the existing case reports on the condition. Developments in imaging methods and new functional imaging techniques allow greater understanding of the radiological characteristics and features of the condition. We re-iterate the importance of radiologists being aware of this condition and communicating with the operating surgeon if any renal or adrenal surgery is planned.
References
- Xing Y, Lerario AM, Rainey W, Hammer GD (2015) Development of adrenal cortex zonation. Endocrinol Metab Clin 44: 243-274.
- Rokitansky K (1855) A manual of pathologic anatomy. Philadelphia, Blanchard & Lea, pp: 188.
- Honoré LH, O’hara KE (1976) Combined adrenorenal fusion and adrenohepatic adhesion: a case report with review of the literature and discussion of pathogenesis. J Urol 115: 323-325.
- Colberg JW, Cai X, Humphrey PA (1998) Unilateral adrenal heterotopia with renal-adrenal fusion. J Urol 160: 116.
- Fan F, Pietrow P, Wilson LA, Romanas M, Tawfik OW (2004) Adrenal pseudocyst: a unique case with adrenal renal fusion, mimicking a cystic renal mass. Ann Diag Pathol 8: 87-90.
- Mahadevia S, Rozenblit A, Milikow D, Marinovich A (2009) Renal-Adrenal fusion: instance of an adrenal adenoma mimicking a solid renal mass at CT-case report1. Radiol 251: 808-812.
- Boll G, Rattan R, Yilmaz O, Tarnoff ME (2015) Intraoperative identification of adrenal-renal fusion. J Minimal Acc Surg 11: 205.
Citation: Bamford RK, Bretherton J, Rosenfelder N, Bell J (2018) Bilateral Adrenal-Renal Fusion: A Radiological Diagnosis. OMICS J Radiol 7: 298. DOI: 10.4172/2167-7964.1000298
Copyright: © 2018 Bamford RK, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Open Access Journals
Article Tools
Article Usage
- Total views: 5469
- [From(publication date): 0-2018 - Nov 12, 2025]
- Breakdown by view type
- HTML page views: 4553
- PDF downloads: 916