Case Report Open Access
Correction of Midline Diastema and Rotated Central Incisors Using a Versatile Fixed Partial Appliance in Mixed Dentition: A Case Report
Rapala Harika1*, Dwijendra KS2, Parsa Arun3 and Sai Sree Swetha G21Department of Pedodontics and Preventive Dentistry, Mamata Dental College and Hospital, Khammam, Telangana, India
2Department of Pedodontics and Preventive dentistry, MNR Dental College and Hospital, Sangareddy, Telangana, India
3Department of Pedodontics and Preventive Dentistry, Meghana Institute of Dental Sciences, Nizamabad, Telangana, India
- *Corresponding Author:
- Harika R
Department of Pedodontics and Preventive Dentistry, Dr. NTR University of Health Sciences
Mamata Dental College, Khammam, Telangana, India
Tel: 09948213219
E-mail: harika_rapala@yahoo.com
Received date: July 21, 2016; Accepted date: July 28, 2016; Published date: August 04, 2016
Citation: Harika R, Dwijendra KS, Arun P, Sai Sree Swetha G (2016) Correction of Midline Diastema and Rotated Central Incisors Using a Versatile Fixed Partial Appliance in Mixed Dentition: A Case Report. Pediatr Dent Care 1:116.
Copyright: © 2016 Harika R, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Neonatal and Pediatric Medicine
Abstract
Midline Diastema is a Space between the Central Incisor. Although Physiologic ephemeral maxillary midline diastema is ascertained in children during eruption of maxillary anterior teeth, in most cases it is self-corrected subsequently by the eruption of maxillary canines as described by Broadbent. However midline diastema unrelated to the eruption of teeth has been observed owing to multiple etiologic factors. Treatment to align the central incisors depends on treating the predisposing factors.
Keywords
Midline diastema; 2 × 4 Appliances; Rotated incisors
Introduction
Midline diastema is a space between the central incisors. The frequency of midline diastema is high in children and it drops off with age [1]. Although physiologic fugacious maxillary midline diastema is noticed in children during eruption of maxillary anterior teeth in most cases, it is self-corrected after eruption of maxillary canines. However, midline diastema unrelated to the eruption of teeth has been observed owing to noxious etiologic factors, such as supernumerary teeth, midline bony clefts, congenital absence of permanent teeth, deleterious oral habits, certain pathological conditions, ethnic and racial characteristic high frenal attachments and others such as peg shaped laterals and microdontia [1,2].
Midline diastema larger than 2 mm in the mixed dentition should be fully investigated due to its relation to pertubations in tooth eruption [2]. For patients who reckon a diastema unacceptable, active treatment is available. However, not all diastemas can be tempered in the same in terms of modality or timing. The extent and the etiology of the diastema can be properly evaluated. In some cases interceptive therapy can bring forth positive results early in the mixed dentition. Tooth rotation, which is one of the most usual side effects of a mesiodens, is defined as observable mesiolingual or distolingual intra-alveolar displacement of the tooth around its longitudinal axis. Proper selection of a case, adequate patient co-operation and good oral hygiene all are vital for treating such cases [2]. Hence in the present paper we report a case of midline diastema associated with high labial frenal attachment and rotation of maxillary central incisors treated with labial frenectomy and using a versatile 2 × 4 appliance.
Case Report
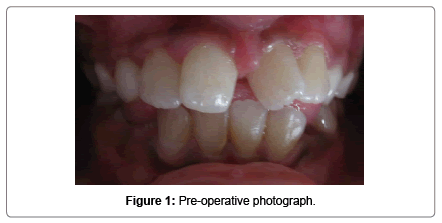
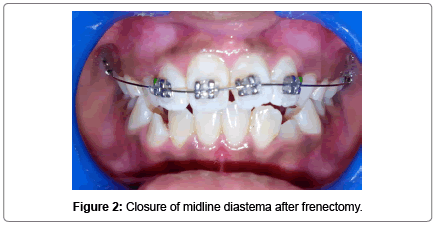
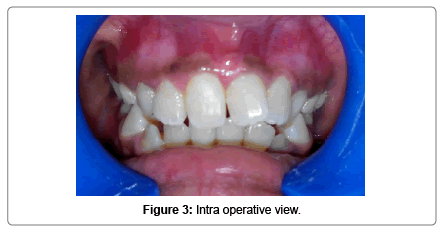
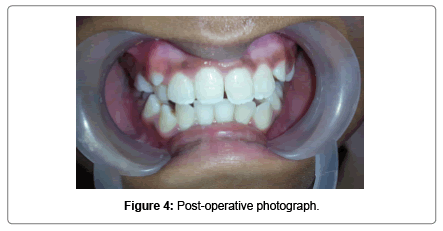
A 10 year old female patient reported to Department of Pedodontics and Preventive Dentistry with a chief complaint of spacing and rotated upper front tooth region since 4 years. Her medical and dental history of the patient was non contributory. No abnormality was detected on extraoral examination. Intraoral examination showed that the patient was in the mixed dentition stage, with the permanent incisors and first molars already erupted. In addition, there was a 4-mm midline diastema associated with high frenal attachment extending till the incisive papilla and mesiolingually rotated central incisors with Angle’s class I molar relationship (Figure 1). To rule out the presence of any unerupted supernumerary teeth or any other underlying pathology intra oral periapical radiographs were advised. The radiographic findings revealed the absence of supernumerary teeth or any pathology. Blanching test was done to check for high frenal attachment in the maxillary arch and it was found positive. Based on the clinical and radiographic findings the present case was diagnosed as Angle’s class I malocclusion with midline diastema and rotated 11-21. The treatment plan was designed to achieve some clinical objectives such as closure of midline diastema and orthodontic correction of rotated teeth. In the first appointment alginate impressions of both upper and lower arches were realized and working models were obtained with dental stone to check the arch length tooth material discrepancy. Upon model analysis no such discrepancy was observed. The treatment plan was explained to the patient along with her parents and written informed consent was obtained to carry out the procedure. 2% xylocaine with adrenaline local anaesthetic infiltration was given on the labial and palatal aspect near the base of the fraenum and labial frenectomy was performed. After 2 month post-operative follow up the midline diastema got corrected by itself, however the rotation of the teeth still persisted (Figure 2). So a sectional fixed 2 × 4 appliance was inserted in patients mouth by bonding 2 buccal tubes on 16, 26 and placing metallic MBT brackets on 11, 12, 21 (Figure 3). After monthly and periodic activation of 2 × 4 appliance the rotation of the teeth was corrected in 3 months interval. Circumferential supracrestal fibrotomy was done to prevent derotation of teeth. Debonding of the appliance was done and a lingual fixed retained was placed in patients mouth (Figure 4). The patient was under constant follow-up.
Discussion
The interplay of different factors during dental development can cause some form of malocclusion. The case described here tangled an interaction of two major elements, a high labial frenal attachment and rotation of central incisors leading to midline diastema. It is the most common type of malocclusion easily noticed by parents or general dentists as it is located in the maxillary anterior region. The space can be a normal growth characteristic during the primary and mixed dentition, however the medial erupting path of maxillary lateral inciors and canies results in normal closure of this space as described by Broadbent [2]. For some individuals however, the diastema does not close down spontaneously.
Racial and gender differences also exist for diastemas. Maxillary median diastema was comparatively high in Africans (West Africa) than in Caucasians (British) or Mongoloids (Chinese from Hong Kong and Malaya) [3]. Horowitz reported that among 10 to 12 years children, midline diastema exhibited a higher prevalence of 19% in black children than do white children (8%) [4]. Becker confirmed the same and stated that the midline diastema as an ethnic norm among blacks and Mediterranean whites [5]. Richardson and co-workers found that females in both black and white races had a higher prevalence than males at age 6; however, at age 14, the prevalence was more in males in both races [6].
The diagnosis of diastema must be based on a thorough medical/ dental history, clinical examination and radiographic survey because of the possibility for multiple etiologies. When the diastema may be due to malocclusion or tooth and or arch size discrepancy diagnostic study models also may be necessary for analysis and measurement as in the present case. The medical/dental history should investigate any pertinent medical condition (hormonal imbalances), oral habits, previous dental treatment and or surgeries and family history of diastema or other related dental problems. Panoramic and periapical radiographs are necessary to evaluate the patient’s dental age and physical impediments, abnormal suture morphology, missing teeth, dental anomalies, improper teeth alignment or abnormal eruption paths. Proper treatment of midline diastema depends on its etiology [2]. Multiple treatment protocols had been proposed ranging from the classic frenectomy or orthodontic treatment, to even more radical procedures or sub apical osteotomies, corticotomies, septotomies [7-9] and reverse level gingivectomies [10]. No single method can be used to treat all diastema cases.
The success in treating diastemas reckon upon the following treatment phases [2].
1. Exact diagnosis of specific etiology or etiologies.
2. Pre-treatment thoughtfulness of appropriate orthodontic objectives
3. Intervention of specific etiology or etiologies
4. Long term retention and stability
In the present case midline diastema was associated with mesiolingual rotation of the teeth. So treatment plan also should consider the facial type, esthetics, treatment time and cost. Orthodontic closure of the midline diastema can be divided into four categories [2].
1. Treatment involving mesial tipping of incisor.
2. Treatment involving mesial bodily approximation of incisor.
3. Treatment involving decrease of the enlarging over jet.
4. Closing the space as part of more comprehensive orthodontic treatment.
When present in the anterior region, rotation of the teeth could be attributed to mild crowding and have often been found to be accompanied by other dental anomalies. Cognition of the biomechanical principles of tooth movement is crucial for the orthodontist to accomplish an individualized treatment plan. If the location of the centre of resistance of a tooth or group of teeth is known, the correct moment-to-force ratio can be applied at the brackets to obtain specific centres of rotation-in other words, controlled movement. The studies have shown that the location of the centre of resistance of the maxillary central incisor depends on the palatal bone level and is at approximately two-thirds of the palatal alveolar bone height, measured from the root apex [11]. During mixed dentition stage the treatment carried out may take as little as a couple of weeks, but in the more difficult cases it can be longer. In the majority of cases, the end result can be more effectively and efficiently achieved than if a removable appliance was used. In this case, the treatment was carried out in early mixed dentition period. The major advantage in carrying out this treatment with fixed brackets are the ease with which the force magnitude and vector can be controlled much more precisely than with a removable appliance. Other advantage includes minimal discomfort to the patient and reduces need for patient co-operation. Although rotations can be treated at various stages of root development, an early correction of rotated teeth before root completion is conducive to better retention [12]. Early, derotation of the central incisors was planned and achieved to reduce any possible psychological trauma. A 2 × 4 appliance was planned for correcting the rotation in mixed dentition stage in the present case. The appliance described is versatile, easy to use and well tolerated by all patients.
Conclusion
In treating these potentially challenging mixed dentition problems, the functional improvement coupled with the obvious psychological benefit gives this simple and easily placed appliance a significant advantage over the traditional methods.
References
- Gardiner JH (1967) Midline spaces. Dental Practitioner 17: 287-298.
- Huang WJ, Creath CJ (1995) The midline diastema: A review of its etiology and treatment. Pediatric Dentistry 17: 171-179.
- Lavelle CL (1970) The distribution of diastemas in different human population samples. Scand J Dent Res 78: 530-534.
- Horowitz HS (1970) A study of occlusal relations in 10- to 12-yearold Caucasian and Negro children: summary report. Int Dent J 20: 593-605.
- Becker A (1977) The median maxillary diastema: A review of its etiology. Isr J Dent Med 26: 21-27.
- Richardson ER, Malhotra SK, Henry M, Coleman HT (1973) Biracial study of the maxillary midline diastema. Angle Orthod 43: 438-443.
- Cole JR II, Staples AF (1973) Correction of diastemas by anterior osteotomy and midline osteomy. J Oral Surg 31: 308-313.
- Kraut RA, Payne J (1983) Osteotomy of intermaxillary suture for closure of median diastema. J Am Dent Assoc 107: 760-761.
- Spilka CJ, Mathews PH (1979) Surgical closure of diastema of central incisors. Am J Orthod 76: 443-447.
- Ewen SJ, Pasternak R (1964) Periodontal surgery - an adjunct to orthodontic therapy. Periodontics 2: 162-171.
- Jahanbin A, Baghaii B, Parisay I (2010) Correction of a severely rotated maxillary central incisor with the Whip device. Saudi Dent J 22: 41-44.
- Dowsing P, Sandler PJ (2004) How to effectively use a 2x4 appliance: Journal of Orthodontics 31: 248-258.
Relevant Topics
- About the Journal
- Birth Complications
- Breastfeeding
- Bronchopulmonary Dysplasia
- Feeding Disorders
- Gestational diabetes
- Neonatal Anemia
- Neonatal Breastfeeding
- Neonatal Care
- Neonatal Disease
- Neonatal Drugs
- Neonatal Health
- Neonatal Infections
- Neonatal Intensive Care
- Neonatal Seizure
- Neonatal Sepsis
- Neonatal Stroke
- Newborn Jaundice
- Newborns Screening
- Premature Infants
- Sepsis in Neonatal
- Vaccines and Immunity for Newborns
Recommended Journals
Article Tools
Article Usage
- Total views: 14612
- [From(publication date):
specialissue-2016 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 13383
- PDF downloads : 1229