Demographics, Clinical Presentation and Outcome of Multiple Myeloma in Bermuda
Received: 11-Jan-2017 / Accepted Date: 27-Jan-2017 / Published Date: 31-Jan-2017 DOI: 10.4172/2161-0681.1000301
Abstract
Objectives: The incidence and severity of multiple myeloma (MM) differ among ethnic groups. The purpose of this study was to determine the incidence, demographics, clinical presentation and outcome of multiple myeloma (MM) in Bermuda.
Methods: The study involved a review of patients diagnosed with haematological malignancy including MM using hospital records retrieved from Bermuda Hospital Board database, between January, 2010 and December, 2014. Demographic, clinical and laboratory data on patients with MM were collected and analysed.
Results: Haematological malignancy accounted for 7% (144/2009) of all cancers and MM accounted for 23% (33/144) of all hematologic malignancies with an incidence of 10.2/100,000 population per year (based on Bermuda population of 64,237 in 2010). The male: female ratio was 1:2.3 with a mean age at diagnosis of 68 years. The common clinical presentations at the time of diagnosis were anaemia (26/33, 78.8%), followed by bone pain involving the lower back and hip (15/33, 45.5%), hypercalcaemia (14/33, 42.4%), neoplastic systemic symptoms (13/33, 39%) and renal insufficiency (12/33, 36.4%). The majority of patients (23/33, 69.7%) were diagnosed at stages 2 and 3 of the disease and 91.3% (21/23) of these patients were from Black ethnic groups. All patients (15/15, 100%) with adverse genetic factors were Black and the majority (10/15, 66.6%) were female.
Conclusion: The incidence of MM in Bermuda is higher than that reported from the United Kingdom and the United States and the condition is more common in women. The age at diagnosis and clinical presentation and prognosis of MM in Bermuda are comparable with reports from the Western world. Further studies to address the survival of patients with MM in Bermuda receiving different treatment options should be considered.
Keywords: Multiple myeloma; Demographic; Outcome; Bermuda
315330Introduction
Multiple myeloma (MM) is the neoplastic proliferation of plasma cells in the bone marrow characterized by the production of monoclonal immunoglobulin, extensive skeletal destruction with osteolytic lesions, osteopenia and/or pathologic fractures and hypercalcaemia. The highest incidence occurs in the industrialised regions of Australia/New Zealand, Europe and North America [1]. Incidence and mortality seem to be stable in Asian countries but has been increasing slowly over the decades among whites in the western countries [1]. Multiple myeloma accounts for 1-2% of all cancers and 10-15% of all haematological malignancies in the United Kingdom and United States [2-4]. The incidence of MM in the United Kingdom estimated by the Haematological Malignancy Research Network (HMRN) is 6.9 per 100,000 per year. Incidence rates are similar in the United States, with the Surveillance, Epidemiology and End Results Program (SEER) [4] estimating 6.3 per 100,000 per year. In a study performed by Waxman AJ et al. in 2010, they review data obtained from the original 9 registries of the NCI SEER program from 1973-2005 in the United States in which 5,798 black and 28,939 white patients were diagnosed with MM, the age-adjusted MM incidence rates were 11.0 and 4.9 per 100,000 for blacks and whites, respectively [5]. Unlike other haematological malignancies, the incidence of MM is highest in Afro-Caribbean populations followed by Caucasian and Asian populations [5]. The incidence in males is two to three folds higher than in females and increases with increasing age. The average age at diagnosis ranges from 65-70 years in Western countries [5-8].
Patients with myeloma are more commonly anaemic than patients with other haematological malignancies, such as Hodgkin’s and Non- Hodgkin’s Lymphoma [9]. This has been associated with poor quality of life and prognosis [9-11]. Recently myeloma was reported as the fourteenth leading cause of cancer death in the United States [4] and where the number of deaths due to MM was 3.3 per 100,000 per year [4]. Similarly Myeloma was the 15th most common cause of cancer death in the UK during 2014, accounting for 2% of all cancer deaths [12]. The Bermuda National Tumour Registry Annual Report for 2013 stated that cancer was responsible for 30.2% of deaths [13].
This study was undertaken to investigate the incidence of MM in Bermuda compared with other parts of the world and the contribution of MM to cancer morbidity and mortality.
Patients and Methods
A retrospective study was conducted involving consecutive patients with multiple myeloma (MM) seen at King Edward VII Memorial Hospital (KEMH), Bermuda over a 5 year period from January, 2010- December, 2014. The data bases used were KEMH Health Information Management Services, CoPath Software in the Pathology Department and the Bermuda National Tumour Registry database. Demographic and clinical data, on each patient, were obtained from hospital records. A standardized data collection form was used to collect data pertaining to age, gender, ethnicity, initial clinical presentation, haematological and biochemical parameters, final diagnosis and patient mortality status. The diagnosis of MM was made based on International Myeloma Working Group 2003 [14,15].
Results
As shown in Table 1, The Tumour Registry database contained 2009 patients with cancer over the period of study and newly diagnosed haematological malignancies accounted for 7% (144/2009) (Table 1).
| Male | Female | Total (%) | |
|---|---|---|---|
| Non-Hodgkin’s Lymphoma | 26 | 24 | 50 (34) |
| Hodgkin's Lymphoma | 2 | 0 | 3 (2) |
| Multiple Myeloma | 10 | 23 | 33 (23) |
| Acute Leukaemia | 0 | 1 | 1 (1) |
| Chronic Myelomonocytic Leukaemia | 1 | 0 | 1 (1) |
| Myeloproliferative Neoplasm | 9 | 12 | 21 (15) |
| Adult T-Cell Leukaemia | 1 | 1 | 1 (1) |
| Acute Lymphoblastic Leukaemia | 2 | 0 | 2 (1) |
| Acute Myeloid Leukaemia | 3 | 2 | 5 (4) |
| Chronic Lymphocytic Leukaemia | 3 | 2 | 5 (4) |
| Chronic Myeloid Leukaemia | 1 | 2 | 3 (2) |
| Hairy Cell Leukaemia | 2 | 0 | 2 (1) |
| Myelodysplastic Syndrome | 10 | 7 | 17 (11) |
| Total | 70 | 74 | 144 |
Table 1: Newly Diagnosed Haematologic Malignancy between January 1, 2010 to December 31, 2014 in Bermuda.
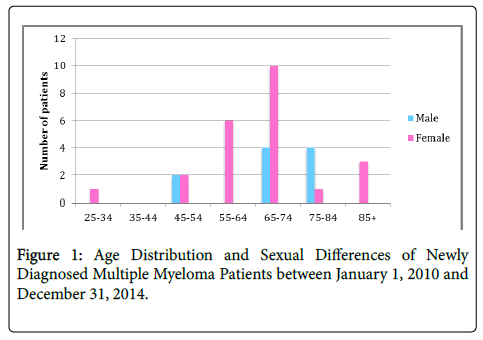
Of the 144 patients with haematological malignancies 33 (23%) were newly diagnosed with MM and the incidence of MM was 10.2/100,000 per year (taking into consideration the total of 64,237 persons in Bermuda in 2010). The 33 newly diagnosed cases of MM included 23 females and 10 males (female: male ratio, 2.3:1); 28 were blacks while only 5 were whites. In Bermuda, the incidence rate in blacks and whites were 16.1 and 5.0/100,000 per year respectively. According to Bermuda census in 2010, out of the total population of 64237, 54% were blacks, 31% were whites while others were 15%). As shown in Table 1 and Figure 1 the average age at diagnosis of MM was 68 years (range 33-89 years) and this was comparable for males and females (71 vs. 67 years). The majority of patients (22/33, 67%) were aged 65 and older at the time of diagnosis (Figure 1).
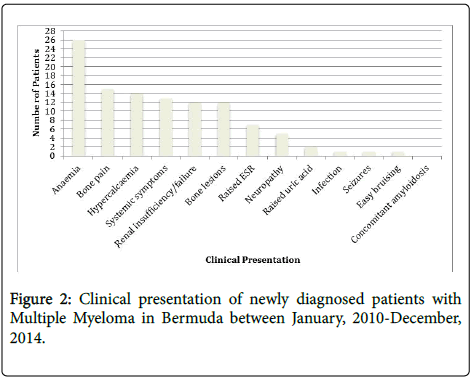
The clinical presentations at the time of diagnosis in the 33 patients with MM are summarized (Figure 2). Anaemia (79%), followed by bone pain involving the lower back and hip (45%), hypocalcaemia (42%), neoplastic systemic symptoms (39%) and renal insufficiency (36%) were the most common manifestations. The neoplastic systemic symptoms included fever, weight loss and night sweats. The majority of patients (15/33, 45%) were diagnosed with stage 2 disease while stage 1 disease was identified in 9 patients (27%) and 8 (24%) had stage 3 disease at diagnosis. Staging was not determined for 1 patient (3%) as albumin and beta2-microglobulin results were unavailable (Figure 2).
Of the 33 cases of MM 18 (55%) were identified as immunoglobulin IgG myeloma (with kappa light chains in 7 and lambda light chains in 11 cases), 7 (21%) cases were IgA myeloma (with kappa light chains in 3 and lambda light chains in 4 cases), while 4 (12%) cases were light chain myeloma (including 2 cases with kappa and 2 cases with lambda light chain myeloma). The pattern was bi-clonal in 1(3%) case (IgG with lambda light chain and IgA with kappa light chains). Immunofixation/immunoelectrophoresis results were not available for the remaining 3 patient (3%).
At the time of the study 21/33 (64%) patients were alive and of these 7 (21%) were negative of cytogenetic abnormalities, 5 (15%) had no identifiable record and 9 (27%) patients were positive for cytogenetic abnormalities. Of the 9 living patients with cytogenetic abnormalities 7 had poor cytogenetic prognostic indices, either singly or in combination, including mutations involving TP53, 1q21, t(14:16), t(4:14) and monosomy 13 (Table 2). The cause of death in the 12 patients was related to MM. The mortality rate of MM in Bermuda is 3.7 per 100,000 per year which is comparable with 3.3 per 100,000 per year found in the United States [4]. The mean age at diagnosis of the deceased patients was 72 years (range 51-89). The deceased patients had more advanced stage (92% had stage 2 or stage 3), compared with the alive patients (60% had stage 2 or stage 3). There was no record of cytogenetic analysis in 5/12 (42%) deceased patients while 6/12 (50%) had monosomy 13 and translocation involving 1q21 either singly or in combination and 1/12 (8%) was negative for cytogenetic abnormalities (Table 2).
| Cytogenetic Abnormality | Alive Patients (%) | Deceased Patients (%) |
|---|---|---|
| t(4:14) | 1 | 1 |
| t(14:16) | 2 | 0 |
| Monosomy 13 | 3 | 4 |
| 1q21 | 4 | 5 |
| TP53 | 2 | 0 |
| 12 | 11 |
Table 2: Poor cytogenetic abnormalities in patients with MM, present singly or in combination (n=9).
Discussion
This is the first study highlighting the demographics, clinical presentation and outcome of patients with MM in Bermuda. The incidence of MM in Bermuda observed in the present study is higher than that reported for the UK and US [3,4]. A gradual increase in the number of cases diagnosed with MM from 2010 to 2014 was observed. This can be due to increased awareness and recognition of the clinical features of the disease by physicians and greater opportunity to perform diagnostic tests easily. The racial disparities in MM have been discussed by several authors. The incidence of MM in blacks in Bermuda was higher compared with that observed in black populations in the United States. The mean age at diagnosis for patients with MM in Bermuda was comparable with that reported from other countries [2-4,8]. Myeloma is predominately a disease of the elderly and very few cases have been diagnosed in patients less than 40 years of age. As mentioned the youngest patient diagnosed with MM in Bermuda was a black female aged 33 years. The female preponderance of MM observed in the present study is in conflict with reports from the US and UK where MM is more commonly diagnosed in male patients [2-4,8].
The frequency of the clinical presenting features of MM including anaemia, bone pain, hypocalcaemia, systemic symptoms and renal insufficiency in this Bermudian cohort was similar to that reported in other countries. The stage of disease at presentation is a recognized significant prognostic factor. Griepp et al. [16] reported that the median survival rates for patients diagnosed with stage 3 disease was 29 months compared with 45 months and 62 months for stages 2 and 1, respectively. In the present study more than two thirds of the patients presented with a moderately severe disease in keeping with stages 2 and 3, and of these, half were deceased at time of initiation of retrospective analyses.
In one study involving the prevalence of tumour genetic marker in patients with MM, immunoglobulin heavy chain (IGH) gene translocations were more common in females compared with males [17]. The cytogenetic abnormalities associated with poor prognosis identified in that study included monosomy 13, mutations involving 1q21, t(4:14), t(14:16) and TP53. In the current series the identified poor cytogenetic abnormalities were observed in just over 10% and might not have contributed substantially to the survival of the patients. On the other hand the advances in treatment strategies employed for all of our patients might have influenced survival rates even in the patients with poor prognostic cytogenetic markers. Also the majority of the deceased patients were black and monosomy [13], and 1q21 mutations might have contributed significantly to the adverse prognosis [17].
The limitations of this study are the small sample size, absence of information regarding therapy, response rate, progression free survival and follow-up data.
In conclusion, the incidence of MM in Bermuda is more common in females than in males in contrast to reports from other western countries. The clinical presentations and prognosis of MM in patients in Bermuda are similar to those seen in the Western World. Follow up studies should be considered to understand the correlation between different treatments and outcome of the patients.
Acknowledgements
We would like to extend our gratitude to Bermuda National Tumour Registry, Health Information Management Services, and Daphne Jones (Senior Technologist in Histopathology), for their individual assistance in the collection, interpretation and presentation of the data in this study.
Emma Knight performed the study, collated the data, analysed part of the data and contributed in writing the paper. Eyitayo Fakunle designed the study, assisted in collating the data, analysed part of the data and wrote the paper. Clyde Wilson, Marva Phillips-Williams, Sein Aung and Takawira Mubako contributed in writing the paper and contributed essential tools. Katura Horton-Perinchief and Dy-Juan DeRoza analysed most part of the data.
References
- Becker N (2011) Epidemiology of multiple myeloma. Recent Results Cancer Res 183: 25-35.
- Alexander DD, Mink PJ, Adami HO, Cole P, Mandel JS, et al. (2007) Multiple myeloma: a review of the epidemiologic literature. Int. J. Cancer 120: 40-61.
- Bagguley T, Blase J, Painter D, Roman E, Smith A (2012) Haematological malignancies and cancer registration in England (2004-2008). Leukaemia and Lymphoma Research.
- Howlader N, Noone AM, Krapcho M, Garshell J, Miller D, et al. (2015) SEER Cancer Statistics Review, 1975-2012, National Cancer Institute. Bethesda.
- Waxman AJ, Mink PJ, Devesa SS, Anderson WF, Weiss BM, et al. (2010) Racial disparities in incidence and outcome in multiple myeloma: a population based study. Blood 116: 5501-5506.
- Bird J, Owen R, d’Sa S, Snowden J, Pratt G, et al. (2011) Guidelines for the diagnosis and management of multiple myeloma. Br J Haematol 154: 32-75.
- Landgren O, Gridley G, Turesson I, Caporaso N, Goldin L, et al. (2006) Risk of monoclonal gammopathy of undetermined significance and subsequent multiple myeloma among African Americans and white veterans in the United States. Blood 107: 904-906.
- Moreau P, San Miguel J, Ludwig H, Schouten H, Mohty M, et al. (2013) Multiple myeloma: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow up. Ann Oncol 24: 1-5.
- Birgegard G, Gascón P, Ludwig H (2006) Evaluation of anaemia in patients with multiple myeloma and lymphoma; findings of the European Cancer Anaemia Survey. Eur J Haematol 77: 378-386.
- Auguston BM, Begum G, Dunn JA, Barth NJ, Davies F, et al. (2005) Early Mortality after Diagnosis of Multiple Myeloma: Analysis of Patients Entered Onto the United Kingdom Medical Research Council Trials between 1980 and 2002 - Medical Research Council Adult Leukaemia Working Party. J Clin Oncol 23: 9219-9226.
- Alexanian R, Balcerzak S, Bonnet JD, Gehan EA, Haut A, et al. (1975) Prognostic factors in multiple myeloma. Cancer 36: 1192-1201.
- Data were provided by the Office for National Statistics on request in UK, November 2015.
- Horton-Perinchief K, Landy G (2013) The Bermuda National Tumour Registry Annual Report 2013. Bermuda National Tumour Registry.
- The International Myeloma Working Group (2003) Criteria for the classification of monoclonal gammopathies, multiple myeloma and related disorders: a report of the International Myeloma Working Group. Br J Haematol 121: 749-757.
- Department of Statistics (2010) 2010 Census of Population and Housing. Bermuda Census.
- Griepp P, San Miguel J, Durie BGM, Crowley JJ, Barlogie B, et al. (2005) International Staging System for Multiple Myeloma. J Clin Oncol 23: 3412-3420.
- Boyd KD, Ross FM, Chiecchio L, Dagrada G, Konn ZJ, et al. (2011) Gender Disparities in the Tumour Genetics and Clinical Outcome of Multiple Myeloma. Cancer Epidemiol Biomarkers Prev 20: 1703-1707.
Citation: Knight E, Fakunle EE, Wilson C, Phillips-Williams M, Aung S, et al. (2017) Demographics, Clinical Presentation and Outcome of Multiple Myeloma in Bermuda. J Clin Exp Pathol 7:301. DOI: 10.4172/2161-0681.1000301
Copyright: © 2017 Knight E, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 5236
- [From(publication date): 0-2017 - Aug 29, 2025]
- Breakdown by view type
- HTML page views: 4301
- PDF downloads: 935