Review Article Open Access
Effects of Acupuncture on Obesity and Adipokines Involved in Body Weight Control
| García-Vivas Jessica1, González-González Roberto2, García-Cardona Ma. Del Carmen3, López-Camarillo César4 and Marchat Laurence A1,3* | |
| 1Doctorate Biotechnology Network, National School of Medicine and Homeopathy, México | |
| 2Especialidad de Acupuntura Humana, Escuela Nacional de Medicina y Homeopatía del IPN, Guillermo Massieu Helguera #239, Fracc. La Escalera, Ticoman, México D.F., C.P. 07320, México | |
| 3Programa Institucional de Biomedicina Molecular, Escuela Nacional de Medicina y Homeopatía del IPN, Guillermo Massieu Helguera #239, Fracc. La Escalera, Ticoman, México D.F., C.P. 07320, México | |
| 4Posgrado en Ciencias Genómicas, Universidad Autónoma de la Ciudad de México, San Lorenzo #290, Col. del Valle, México D.F., C.P. 03110, México | |
| Corresponding Author : | Dr. Laurence A. Marchat Programa Institucional de Biomedicina Molecular Escuela Nacional de Medicina y Homeopatía del IPN Guillermo Massieu Helguera #239, Fracc. La Escalera Ticoman, México D.F., C.P. 07320, México Tel: (52 55) 5729 6300 ext. 55543 E-mail: lmarchat@gmail.com, lmarchat@ipn.mx |
| Received July 04, 2013; Accepted August 17, 2013; Published August 24, 2013 | |
| Citation: Garcia-Vivas J, Gonzalez-Gonzalez R, Garcia-Cardona M, Lopez- Camarillo C, Marchat LA (2013) Effects of Acupuncture on Obesity and Adipokines Involved in Body Weight Control. J Homeop Ayurv Med 2:129. doi: 10.4172/2167-1206.1000129 | |
| Copyright: © 2013 Garcia-Vivas J, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Traditional Medicine & Clinical Naturopathy
Abstract
Obesity is a worldwide disease that results from a deregulation of energy balance and changes in adipokines
and other molecules with metabolic relevance. Pharmacological treatments for obesity are often associated to drug adverse effects. Among alternative and complementary therapeutic methods for obesity treatment, Traditional Chinese Medicine and particularly acupuncture that have been practiced for thousands of years in China, have been increasingly used for the efficient control of body weight without producing negative side effects and weight regain. Several works have suggested that the effects of acupuncture may be related to hypothalamus stimulation, which may regulate the production of some proteins involved in food intake and energy expenditure balance. In this review, we present the main results of English publications obtained from PubMed database as well as data from works published in original Chinese language. These reports describe the clinical effectiveness of acupuncture as a treatment for obesity. They also provide evidence about the regulation of the principal adipokines related to obesity, namely leptin and adiponectin, as well as other relevant biochemical molecules. Although further well-designed and controlled studies are required,
this knowledge contributes to gain some insight in the mechanisms underlying the effect of acupuncture for obesity treatment.
| Keywords |
| Acupuncture; Adiponectin; Body weight control; Inflammation; Leptin; Obesity; Traditional Chinese Medicine |
| Abbreviations |
| ACOX: Acyl-CoA Oxidase; AGRP: Agouti-Related Peptide; α-MSH: α-Melanocyte-Stimulating Hormone; BE: Beta Endorphin; BMI: Body Mass Index; CART: Amphetamine-Related Transcript; CNS: Central Nervous System; CSF: Cerebrospinal Fluid; DIO rat: Diet-Induced Obese Rat; EA: Electro Acupuncture; FFA: Free Fatty Acid; HDL: High Density Lipoprotein; Hsp: Heat Shock Protein; LDL: Low Density Lipoprotein; MCP-1: Monocyte Chemoattractant Protein-1; NPY: Neuropeptide Y; NRF 1: Nuclear Respiratory Factor 1; PGC-1α: Peroxisome Proliferator-Actived Receptor Coactivator- 1α; POMC: Pro-Opiomelacortin; PPAR γ: Peroxisome Proliferator- Activated Receptor γ; SIRT1: Skeletal Sirtuin 1 Protein; TCM: Traditional Chinese Medicine; TNF α: Tumor Necrosis Factor α; WAT: White Adipose Tissue |
| Introduction |
| Obesity is a global public health problem that presents the characteristics of a pandemic due to its rapidly increasing incidence [1-3]. Notably obesity promotes hyperglycemia, hyperinsulinemia and hyperleptinemia, as well as glucose intolerance and insulin resistance [4] that are part of the metabolic syndrome [3,5,6]. It also represents a risk for degenerative illnesses, including coronary diseases, heart attack, infertility, erectile dysfunction, arthropathies, neuropathies, as well as colon, prostate, endometrial and breast cancer [7]. These obesity-related diseases cause an excessive economic cost and represent the main causes of death worldwide. Together with a balanced diet and physical exercise, anti-obesity drugs and surgery processes can help patients to lose weight. However, they usually produce adverse effects and weight regain is very common if patients do not strictly follow nutritional recommendations and come back to their sedentary life style. Therefore, there is an increasing interest in alternative and complementary therapeutic methods for obesity treatment. Among these, Traditional Chinese Medicine (TCM) and particularly acupuncture that have been practiced for thousands years in China, represent a suitable therapeutic approach for individuals with obesity, without producing negative side effects and weight regain. This review describes the main metabolic pathways involved in body weight regulation, with an emphasis in leptin and adiponectin adipokines that are essential for the control of food intake and energy expenditure balance. It also describes the clinical effectiveness of acupuncture treatment for obesity and provides evidence about the effects on these adipokines and other relevant biochemical parameters, from extensive analyses of English articles published in PubMed database, as well as works published in original Chinese language in acupuncture and TCM journals. |
| Obesity |
| Obesity is defined as an abnormal increase of fatty acids storage in an expanded adipose tissue mass [3] and accumulation of ectopic fat, which is associated to an increased number and size of adipocytes as a result of passive overconsumption of high-fat and carbohydratesrich diets, and low physical activity. This energy imbalance is due to numerous physiological, psychological, socioeconomic, cultural, emotional, metabolic and genetic factors, whose complex roles are not fully understood yet [8,9]. At cellular level, obesity is also related with activation of immunocompetent cells, such as macrophages, which produce a low-grade chronic inflammation characterized by abnormal cytokine production, increased acute-phase reactants and other mediators, and activation of a network of inflammatory signaling pathways [6]. |
| Involuntary control of energy homeostasis is thought to be crucial to maintain the equilibrium between energy intake and expenditure. In general, body weight is regulated by the central nervous system (CNS), mainly hypothalamus, which controls hunger and satiety in response to a complex network of signals from endocrine tissues, including pancreas (insulin), adipose tissue (leptin, adiponectin) and stomach (ghrelin) [10]. These peripheral signals provide information about the ingested food to the brain, which responds via integrated neuropeptide pathways that are related to energy homeostasis, including neuroendocrine activation from the pituitary gland, motor behavior, and autonomic activity, which is a fundamental metabolic process, including lipolysis, insulin and glucagon secretion from pancreas, and glucose synthesis from liver [11]. |
| Adipose tissue is not only a passive reservoir of energy [12], it also plays a role in energy homeostasis by regulation of whole body free fatty acid (FFA) homeostasis. It stores FFAs in the form of triglycerides through their esterification to glycerol in periods of calorie abundance, and releases them back to the circulation in times of energy shortage [3]. In response to nutrient, neural and hormonal signals, adipose tissue also secretes bioactive peptides, called adipokines, which act at local (autocrine/paracrine) and systemic (endocrine) levels to control feeding, thermogenesis, immunity and neuroendocrine function [13]. In addition to these efferent signals, adipose tissue expresses receptors to respond to afferent signals from hormone systems and CNS [14]. It also has a role in insulin resistance and cardiovascular complications [6]. |
| The predominant type of adipose tissue commonly called “fat” is the white adipose tissue (WAT) located in subcutaneous region and around viscera [13]. It consists of adipocytes surrounded by vascularized and innervated loose connective tissue with macrophages, fibroblasts, adipocytes precursors and other cells. Notably, WAT is responsible for the synthesis of adipokines for body weight control: leptin, adiponectin, acylation stimulating protein and resistin are produced by adipocytes, while TNFα and IL-6 are synthesized by macrophages [15-17]. |
| Main Adipokines Involved in Body Weight Control |
| Leptin |
| The best known adipokine that promotes weight loss is leptin that acts on the hypothalamus (arcuate nucleus), suppressing food intake and stimulating energy expenditure through increased thermogenesis [8,18]. The regulatory feedback includes the following steps: 1) a sensor (leptin production by adipose cells) monitors the level of energy stores (size of adipose tissue mass); 2) hypothalamic centers receive and integrate the leptin signal through leptin receptors; 3) effectors systems (mainly sympathetic nervous system) control energy intake and energy expenditure [8]. Leptin released from WAT enters into the circulating system, binds to a short form of leptin receptor (LRa) and crosses the blood-brain-barrier [19,20]. In the hypothalamus, leptin binds to the long form of leptin receptor (LRb) [21] in two different groups of neurons. One population synthesizes and releases two orexigenic neuropeptides: the neuropeptide Y (NPY) and the agouti-related peptide (AGRP); the other produces two anorexigenic proteins: the anorexigenic peptide α-melanocyte-stimulating hormone (α-MSH), which derived from pro-opiomelacortin (POMC) and the cocaine and amphetamine-related transcript (CART) [22]. |
| Leptin concentration in plasma and mRNA expression level in adipose tissue are related to obesity severity, which means that an increase of fat mass is associated with an increase of leptin, making it an indicator of total fat mass [23,24]. Most obese subjects have a high plasma leptin concentration and present leptin resistance, which may contribute to deregulation of body weight control. This might result from: 1) a limitation of blood-brain-barrier [25,26], in which leptin receptor (LRa) that transports leptin into the cerebrospinal fluid (CSF) is saturated [19]; 2) mutation of LRb leptin receptor in hypothalamus [27] or 3) inhibition of leptin signaling mechanism in hypothalamus, like STAT3 pathway [28]. Therefore leptin can be successfully used as an anti-obesity tool only in the small number of obese patients with leptin deficiency. |
| Adiponectin |
| Exclusively produced by mature adipocytes [29], adiponectin is an abundant plasma protein [30] that exists as low-molecular-weight trimers to high-molecular-weight dodecamers [31]. It is an antiinflammatory adipokine that regulates energy balance and peripheral lipid metabolism [32,33], stimulating fatty acid oxidation and glucose untaken in skeletal muscles and adipose tissue, both dependent on AMPK signals [34-36]. Moreover, its binding to adiponectin receptors (AdipoR1 and AdipoR2), which colocalize with leptin receptor in hypothalamus, regulates energy expenditure through the same signaling pathway than leptin [37]. Adiponectin has anti-diabetic and anti-atherogenic roles, which are negatively correlated with obesity and insulin sensitivity markers, like waist-hip ratio, insulin resistance, dyslipidemia, diabetes and cardiovascular diseases [38]. Therefore a low plasma adiponectin level is considerate as an independent risk factor for type II diabetes [6,24,39,40]. |
| Traditional Chinese Medicine and Acupuncture for the Treatment of Obesity |
| Definition |
| Traditional Chinese Medicine (TCM) is a complete medical system that has been used to diagnose, treat, and prevent illnesses for more than 2,000 years. TCM is based on the belief in yin and yang (defined as opposing energies): when they are in balance, there is health; when they are out of balance, it means illness [41]. According to TCM, life force or “Qi” circulates longitudinally throughout the body within 12 energy pathways named “energetic channels” or “meridians” [42] that connect with what Western medicine defined as organs or tissues. Health depends on the proper function and harmony of a system consisting of “organs”, “vital substances” (energy, blood, fluids) and “energetic channels”. When balance is disrupted, vital substances production and distribution throughout the body is altered and disease occurs [43]. Stimulation of specific points in the “channels”, called “acupoints”, using different methods described in Table 1, can normalize Qi to restore health [42]. |
| Molecular mechanisms of acupuncture |
| Recent experimental studies have tried to investigate the molecular mechanisms underlying the effects of acupuncture, one of the most used methods of TCM.Using functional magnetic resonance imaging, Napadow et al. showed that limbic system is central for the acupunctural effect (acupuncture, electroacupuncture or tactile pressure), although different pathways and neurobiological responses are activated depending on stimulated points [44]. In contrast, there was no response in limbic system when no-points were stimulated as control [45]. These molecular mechanisms may explain the effects of acupuncture in obesity control since limbic system includes the hypothalamus region that regulates food intake and energy expenditure balance. Other studies have revealed that endogenous opioid peptides (enkephalin, beta-endorphin, endomorphin, dynorphin) in CNS mediate the analgesic effect of electroacupuncture [46]. However, the exact mechanisms underlying the beneficial effects of acupuncture in many pathologies, including obesity, remain largely unknown. |
| Obesity in TCM |
| The Chinese term for obesity is “fei pang” (è�?¥è�?�?) which means “fat, grease easily generated”. TCM describes obesity as a complex condition involving energy systems of spleen, liver and kidney. The alteration of their energy creates an imbalance in body fluids metabolism, which generates pathological products called “moisture” or “humidity” and “phlegm” that accumulate in different parts of the body as fat. This phlegm-fat turn constitutes a pathological product that triggers a wide variety of disease processes, affecting multiple body systems. TCM also considers that poor eating habits and sedentary lifestyles cause obesity, and recognizes that heredity and congenitally determined constitution are important. According to the characteristics of each patient, obesity can correspond to distinct deficiency syndromes (Table 2) and distinct points should be stimulated. The individual diagnostic also includes clinical manifestations, the radial pulse, and a specialized evaluation of the tongue [43]. |
| Experimental evidence of the effects of acupuncture on adipokines regulating body weight |
| An exhaustive search in PubMed database allows the release of numerous reports about the use of acupuncture for obesity treatment. Because one of the coauthor of the present review is a specialist in acupuncture medicine and has Chinese language knowledge, we were able to analyze both English and Chinese language publications, which is somewhat difficult for most scientists. In addition, thanks to his personal access to works published in acupuncture and Traditional Chinese Medicine journals in original Chinese language, we also have the opportunity to review clinical and experimental reports published by acupuncture experts from China, where acupuncture has been practiced for thousands years. |
| The majority of publication related to acupuncture and obesity, usually analyzed the effects on body mass and anthropometric data, but little is known about the regulation of biochemical parameters and adipokines, mainly leptin and adiponectin that are relevant for body weight control. Here we describe several results of the main reports related to electroacupuncture (EA) that is the most commonly used method for obesity treatment; we also include some interesting data about catgut embedding and other acupuncture protocols. These reports were selected because they used control group (placebo) and present experimental data related to leptin and adiponectin (and other molecules) that might contribute to explain the molecular mechanisms of the beneficial effects of acupuncture. |
| Electroacupuncture |
| Electroacupuncture is the most frequently used acupuncture technique to control body weight, because the stimulation is constant and easily measurable in Hertz (Hz). Therefore, the parameters of EA can be precisely characterized, which allows reproducible results. |
| In 2005, You and Hung showed that 100 Hz EA (bilateral Zusanli (ST36) and Sanyinjiao (SP6) for 30 min during 14 days) significantly inhibits weight gain in Wistar diet-induced obese (DIO) rats, with a decrease in triglycerides and an increase in HDL. Leptin and insulin levels were significantly increased in control group, while they remained unchanged in EA group [47]. In human, a similar reduction in body weight, lipid profile (triglycerides, total cholesterol and LDL), as well as in waist and hip circumference, was observed when patients were treated with EA for six weeks (bilateral Tianshu (ST25), bilateral Weidao (GB28), Zhongwan (CV12), Shuifen (CV9), Guanyuan (CV4), Sanyinjiao (SP6), as well as Quchi (LI11) and Fenlong (ST40) for obese patients with higher energy, or Qihai (CV6) and Yinlingquan (SP9) for patients with lower energy, using 30-40 Hz and dense-disperse wave), followed by a six weeks period without any treatment for six weeks and another six weeks period with a low-calorie diet. These results demonstrated that EA exhibits long-term effects on body homeostasis in obese patients [48]. Body weight and serum leptin reduction (p<0.000) in response to EA (ear points Sanjiao (Hungry) and Shenmen (Stomach), and body points Hegu (LI4), Quchi (LI11), Tianshu (ST25), Zusanli (ST36), Neiting (ST44), Taichong (LV3) and Qihai (CV6), once daily, for 30 minutes, during 20 days) were also associated with an increase in serum beta endorphin (BE) levels (p<0.05). Authors hypothesized that the effect of EA in modulating serum BE level could enhance lipolytic activity, which may induce weight loss by mobilizing energy stores [49]. A randomized, sham-controlled preliminary trial confirmed that the significant reduction of body weight and body mass index (BMI) in obese women treated with EA (Hegu (LI4), Shenmen (HT7), Zusanli (ST36), Neiting (ST44), and Sanyinjiao (SP6) bilaterally, two sessions of 20 minutes/week for five weeks) was related to decreased levels of leptin. They also observed reduced insulin levels, and increased levels of ghrelin and cholecystokinin [50]. Lou et al. also reported that EA can significantly reduce leptin levels and increase adiponectin serum levels in obese [51]. Finally, study of Fan et al. evidenced that EA at lateral Housanli and Neiting (ST44) with 2-15 Hz, 4mA for 49 days, was more effective than the anti-obesity drug, sibutramine, to reduce body mass through the regulation of adiponectin and insulin levels in obese rats [52]. |
| To confirm that EA, and not the stress produced by the manipulation, was responsible for body weight reduction and adipokines modulation, Kim et al. compared three groups of rats: AL (fed ad libitum without any treatment), Holder (fed ad libitum with daily holder restraint) and EA (fed ad libitum with daily holder restraint and 100 Hz EA stimulation) groups. After the four-week experimental period, they evidenced that food intake and body weight reduction in EA group was associated to increased serum leptin levels, as previously reported. Interestingly, the level of stress hormones, such as epinephrine and norepinephrine, and corticosterone, was increased in Holder group, but not in EA group. Altogether, these results suggested that the effect of EA on body weight was through increasing leptin, but was not due to the stress caused by the daily holder restraint [53]. Taken altogether, these studies indicated that EA might help to control obesity owing to its beneficial effects on hormones that participate in pathways regulating body weight, namely leptin and adiponectin, among others. An interesting study showed that the significant reduction in food intake and body weight in DIO rats treated with 2 Hz EA (Zusanli (ST36) and Sanyinjiao (SP6) with intensity increasing stepwise from 0.5-1-1.5 mA daily for 30 minutes), was associated with increased levels of α-MSH peptide and POMC mRNA in hypothalamus, and an elevated α-MSH concentration in CSF. These data suggested that the mechanism by which EA controls body weight in rat involves α-MSH that has an anorexigenic effect [54]. In another study, in addition to the effect on appetite and α-MSH, the application of 2 Hz EA (four weeks, three sessions/week) in DIO rats also induced increase in anorexigenic CART peptide, and a decrease in orexigenic peptide NPY in hypothalamus. The modulation of these neuropeptides could explain the reduction of food intake and body weight in rat. Notably, 2 Hz EA treatment induced a more important reduction in food intake, body weight and ghrelin levels, that 100 Hz EA; while 100 Hz EA was more efficient to reduce cholesterol and triglycerides, and increase plasma leptin [55]. |
| Some of the studies described above showed that EA not only modulates leptin and adiponectin, but also affects insulin levels. This was confirmed in works published by Cabio�?�?lu and colleagues in which EA application (ear points Sanjiao (Hungry) and Shenmen (Stomach), and body points Hegu (LI4), Quchi (LI11), Tianshu (ST25), Zusanli (ST36), Neiting (ST44) and Taichong (LV3), once daily, for 30 minutes, during 20 days) produced a 4.8% weight reduction and a significant decrease (p<0.05) in total cholesterol, triglycerides and LDL in obese women [56], as well as a significant decrease in lipoprotein A and apolipoprotein B (p<0.05), indicating that EA therapy might be a useful approach for both losing weight and reducing risk factors for associated cardiovascular diseases [57]. Interestingly, the effects of EA also included an increase in serum insulin and c-peptide levels (p<0.001) and a decrease in glucose levels (p<0.01), suggesting that EA can help to control serum glucose levels through regulation of serum insulin and c-peptide levels [58]. These results are consistent with those of Lin et al. which reported that EA treatment with 15 Hz at bilateral Zusanli (ST36) was able to significantly reduce HOMA index from 7.29 ± 3.0 to 3.3 ± 1.1 in rats with insulin resistance induced by prednisolone, while HOMA index was 5.1 ± 1 in control. Plasma levels of FFAs were significantly decreased after 60 minutes of prednisolone injection (until 16 ± 20% in EA group, compared with 72 ± 31% in control). Therefore, the positive effect of EA on insulin resistance could be by lowering plasma FFAs levels [59]. Another study also demonstrated that the decrease in FFAs levels in response to 3 Hz EA (Zusanli (ST36) and Guanyuan (CV4), five sessions/week, eight weeks), was associated to up-regulation of skeletal Sirtuin 1 (SIRT1) protein expression, peroxisome proliferator-actived receptor γ coactivator 1α (PGC-1α), nuclear respiratory factor 1 (NRF 1) and acyl-CoA oxidase (ACOX). Authors concluded that low-frequency EA improves insulin sensibility in obese diabetic mice probably through activation of SIRT 1/PGC-1α in skeletal muscle [60]. |
| Obesity is closely associated with a chronic inflammation and a few studies have described the anti-inflammatory actions of acupuncture in the treatment of obesity. For example, results from Yu et al. evidenced that strong EA (20 Hz, 5 V at Zusanli (ST36) and Sanyinjiao (SP6) daily for 14 days) was more effective to regulate body weight, as well as triglycerides, cholesterol, HDL and LDL, than weak EA (20 Hz, 2.5 V) in obese rats. Interestingly, RT-PCR assays using RNA obtained from epididymis adipose tissue revealed a significant reduction of transcripts corresponding to that monocyte chemoattractant protein-1 (MCP-1) and TNFα, both proinflammatory molecules. Then the modulation of inflammation could contribute to the effects of EA in obese patients [61]. |
| Catgut embedding |
| Currently, many clinical studies are evaluating the effect of catgut implantation in obese patients and animal models. This method consists in the protein magnetization line with catgut embedding apparatus implanted in the corresponding acupuncture points to produce a sustained and effective stimulation for about 15 days. All the studies clearly demonstrate the efficiency of catgut embedding to regulate body weight; they also evidence changes in several markers. |
| For example, in the study of Gao et al., rats exhibited a reduced weight compared to control group, an increase in PPARγ-mRNA and a reduction in total cholesterol, LDL, hepatic lipoprotein lipase and triglycerides levels in response to two sessions of catgut implantation at points Housanli (posterior ST36 Zusanli), Tianshu (ST25) and Pishu (BL20) [62]. Another report demonstrated that catgut embedding had a better anti-obesity action than manual acupuncture. Interestingly, change in body weight was associated with a significant reduction of serum leptin, triglycerides and cholesterol levels, as well as a significant increase in hypothalamus leptin after four weeks of treatment in obese rats (p<0.05) [63]. In addition to modify lipid profile, catgut implantation in abdomen points during 90 days produced a decrease in glucose levels and fasting insulin in patients with metabolic syndrome, which indicates that catgut embedding method could be useful in patient with metabolic syndrome, probably through insulin reduction [64]. In a recent report, Yan et al. also reported that a 90 days-treatment (one catgut application every two weeks) caused a significant reduction of insulin and leptin resistance, as well as a diminution in total cholesterol, triglycerides and LDL levels, while HDL increased significantly. Interestingly, after one year, patients did not present insulin resistance anymore. Moreover, leptin receptor mRNA expression, leptin and insulin levels were significantly increased in hypothalamus of obese rats with catgut application, which suggested that catgut embedded can modify gene expression [65]. |
| Other acupuncture techniques for the treatment of obesity |
| As described in Table 1, TCM and acupuncture include a large number of methods. Although EA and catgut embedding seem to be the more efficient for obesity treatment, the other techniques have been also shown to reduce body weight and regulate adipokines. |
| One of the most interesting studies about the effects of traditional acupuncture on adipokines, was performed in a diabetic and obese rat model, stimulating Housanli (ST 36) and Yishuand Neiting (ST 44) points. After four weeks of treatment, the authors reported significative changes in the level of several adipokines in circulating blood, namely adiponectin, as well as resistin and TNFα. This indicated that traditional acupuncture can modulate/regulate various biochemical pathways, including metabolism and inflammation, producing different physiological effects that contribute to the control of obesity. These effects were similar to those observed in the group treated with glibenclamide. However, acupuncture treatment did not produce the secondary effects associated with glibenclamide [66]. Auricular acupressure combined with a low-calorie diet was able to produce a significant reduction in plasma leptin levels (18.57%, p<0.01) and body fat mass (4%, p<0.05) in obese patients compared to control group after six weeks treatment [67]. Ippoliti et al. reported that hypocaloric traditional Chinese and western diets produced the same significant reduction in body weight, BMI and waist circumference and leptin levels, without affecting TNFα nor ghrelin levels. Notably, when traditional Chinese diet was associated to auricular acupuncture (Hunger, Shenmen, Liver, Kidney, Lung, Stomach and Mouth points), patients reported a higher reduction of hunger feeling compared with sham group. Unfortunately, the authors did not describe any results about leptin, TNFα and ghrelin concentrations [68]. Finally, Rahsepar et al. performed a randomized clinical trial to compare the effects of traditional acupuncture versus auricular acupuncture in obese patients. Subjects received treatment in combination with low-calorie diet for six weeks (first period) followed by a low-calorie diet alone in the next six weeks (second period). The authors observed that both treatments significantly reduced anthropometric parameters and anti-Heat shock proteins (Hsp) antibodies in the first period. Interestingly, only patients treated with acupuncture showed anthropometric and lipid profile (excepted for HDL) changes in the second period, demonstrating the more sustained effects of traditional acupuncture in comparison with auricular acupuncture. The authors concluded that although both auricular and acupuncture are effective to control body weight, dyslipidemia and immune system, traditional acupuncture induced the most significant changes [69]. |
| Conclusion |
| Obesity is not only a nutrition disease that results from an imbalance between energy intakes versus calorie consumption; it is a complex metabolic illness that involves disequilibrium in various systems summarized in the psycho-neuro-endocrine-immune axis. As a global effect, the adipocyte far from being an allied cell becomes the enemy of the obese individual, which sometimes can lead to death. Emerging experimental evidence described above shows that acupuncture has multi-faceted effects in obese patients (Figure 1). Consistent with the clinical effects on body weight, acupuncture protocols are able to modify serum levels of leptin and adiponectin adipokines, as well as insulin, α-MSH, POMC, CART, SIRT 1, PPARγ, TNFα and MCP-1, among others. As a result, there is a modulation of various biochemical pathways, including metabolism, inflammation, sympathetic activity and defective insulin signaling pathways, unlike anti-obesity drugs usually limit their action to a specific pathway of body weight control. This clearly shows that acupuncture and its related techniques, in combination with the understanding of etiology, physiology and syndromatic differentiation of TCM offer an attractive alternative therapy for the treatment of obesity. These therapeutic methods do not only improve the state of the psycho-neuro-endocrineimmune axis mentioned above, they also contribute to increase the relationship between the different systems involved in body weight regulation, so that the adipocyte becomes again a friendly cell and not a time bomb. However, additional studies are required to fully understand the molecular basis of acupuncture treatment for obesity. Because of the complexity of its physiopathology, obesity treatment requires the participation of a multidisciplinary team, which means experts in acupuncture working with researchers, to be able to correlate the effect of distinct acupuncture procedures on weight control with modifications of molecular mechanisms and factors involved in energy balance. Such studies will help to determine new strategies for more effective and safer control of this worldwide pandemic illness. |
| Acknowledgements |
| This work was supported by Mexican grants from UACM, CONACyT (113148), COFAA-IPN and SIP-IPN. |
References
|
Tables and Figures at a glance
| Table 1 | Table 2 |
Figures at a glance
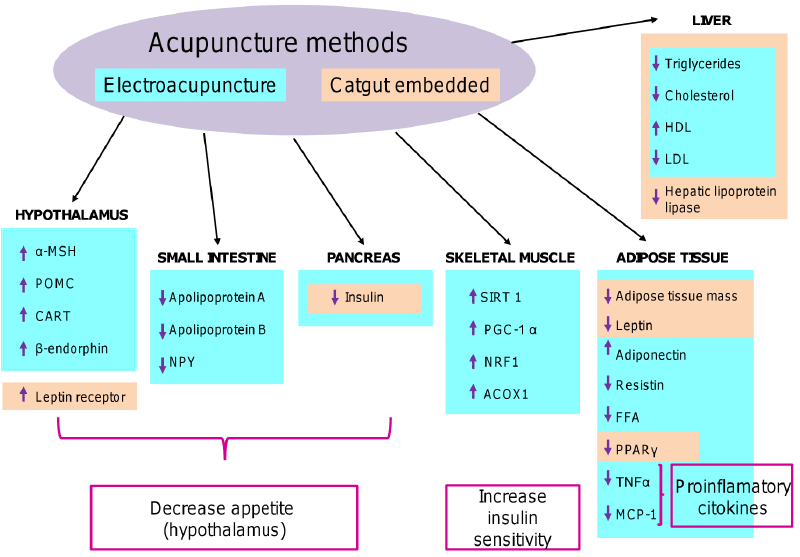 |
| Figure 1 |
Relevant Topics
- Acupuncture Therapy
- Advances in Naturopathic Treatment
- African Traditional Medicine
- Australian Traditional Medicine
- Chinese Acupuncture
- Chinese Medicine
- Clinical Naturopathic Medicine
- Clinical Naturopathy
- Herbal Medicines
- Holistic Cancer Treatment
- Holistic health
- Holistic Nutrition
- Homeopathic Medicine
- Homeopathic Remedies
- Japanese Traditional Medicine
- Korean Traditional Medicine
- Natural Remedies
- Naturopathic Medicine
- Naturopathic Practioner Communications
- Naturopathy
- Naturopathy Clinic Management
- Traditional Asian Medicine
- Traditional medicine
- Traditional Plant Medicine
- UK naturopathy
Recommended Journals
Article Tools
Article Usage
- Total views: 18752
- [From(publication date):
September-2013 - Aug 31, 2025] - Breakdown by view type
- HTML page views : 13726
- PDF downloads : 5026
