Case Report Open Access
Endoscopic Submucosal Dissection of Secondary Hypopharyngeal Neoplasia in Trismus Oral Cancer Patients: Case Series Report
Chen-Shuan Chung1,2, Wu-Chia Lo3, Kuan-Chih Chen1 and Li-Jen Liao3*1Department of Internal Medicine, Far Eastern Memorial Hospital, Banciao District, New Taipei City, Taiwan
2College of Medicine, Fu Jen Catholic University, New Taipei City, Taiwan
3Department of Otolaryngology, Far Eastern Memorial Hospital, Banciao District, New Taipei City, Taiwan
- *Corresponding Author:
- Li-Jen Liao
Department of Otolaryngology, Far Eastern Memorial Hospital
No. 21, Nan-Ya South Road, Section 2, Banciao District
New Taipei City, Taiwan, 22060
Tel: 886289667000
E-mail: dtent87@gmail.com
Received date: May 18, 2017; Accepted date: May 26, 2017; Published date: June 02, 2017
Citation: Chung CS, Lo WC, Chen KC, Liao LJ (2017) Endoscopic Submucosal Dissection of Secondary Hypopharyngeal Neoplasia in Trismus Oral Cancer Patients: Case Series Report. J Gastrointest Dig Syst 7:507. doi:10.4172/2161-069X.1000507
Copyright: © 2017 Chung CS, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Visit for more related articles at Journal of Gastrointestinal & Digestive System
Abstract
The incidence of second primary tumor (SPT) in head and neck (H&N) cancer patients is not uncommon [1,2]. When using image-enhanced endoscopy (IEE) screening in patients at risk, especially narrow-band imaging (NBI) endoscopy and chromoendoscopy with Lugol's solution, approximately 20% of H&N cancer patients have synchronous neoplasia in H&N regions of esophagus [1,2]. Unfortunately, some of them have trismus because of oral submucosa fibrosis secondary to long-term betel quit chewing or post-irradiation therapy, and tumor-related airway compromised. These situations make the pharyngeal passages difficult to reach with conventional endoscopes. Traditionally, hypopharyngeal neoplasia in trismus patients are managed with widest field of resection, open partial pharyngectomy and usually in conjunction with partial or total laryngectomy, which are accompanied with poor quality of life (QoL). We present three trismus patients with early hypopharyngeal neoplasia treated by transoral endoscopic submucosal dissection (ESD).
Keywords
Neoplasia; Endoscopy; Pharyngectomy; Laryngectomy
Case Report
Three trismus oral cancer male patients with mean (± SD) age of 56.7 (± 2.1) years old were reported (Table 1). All of them received endoscopic examinations with NBI and magnifying endoscope which has powerful 80 times optical magnification (EVIS LUCERA CLV-260NBI, GIF-H260Z endoscopy, Olympus Medical Systems Corp, Tokyo, Japan), and chromoendoscopy with Lugol’s solution (Sigma- Aldrich, St. Louis, Missouri, USA). One early synchronous esophageal neoplasia (high-grade intraepithelial neoplasia, HGIN) with hypopharyngeal squamous cell carcinoma (SCC, case 1), one stage I hypopharyngeal SCC (case 2), and one hypopharyngeal HGIN (case 3) were reported (Table 1).
| Case | Age (year) | Sex | Primary tumor | cStage | SPT | cStage | SPT size (mm) | Margin free | Adjuvant therapy | Status | Survival (months) |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 59 | Male | Oral cancer | III | EsoHGIN | 0 | 15 | Yes | Nil | LD | 39 |
| HypoSCC | I | 15 | Yes | RT | |||||||
| NSCLC | IIIB | 42 | NA | CCRT | |||||||
| 2 | 56 | Male | Oral cancer | IVB | HypoSCC | I | 6 | No | CCRT | DF | 26 |
| 3 | 55 | Male | Oral cancer | II | HypoHGIN | 0 | 6 | Yes | Nil | DF | 75 |
CCRT: Concurrent chemoradiotherapy; DF: Disease free; EsoHGIN: Esophageal high-grade intraepithelial neoplasia; HypoHGIN: Hypopharyngeal high-grade intraepithelial neoplasia; HypoSCC: Hypopharyngeal squanous cell carcinoma; LD: Live with disease (metachronous lung cancer); NSCLC: Non-small cell lung cancer; NA: Not applicable; SPT: Second primary tumor
Table 1: Demographic and survival data of reported patients.
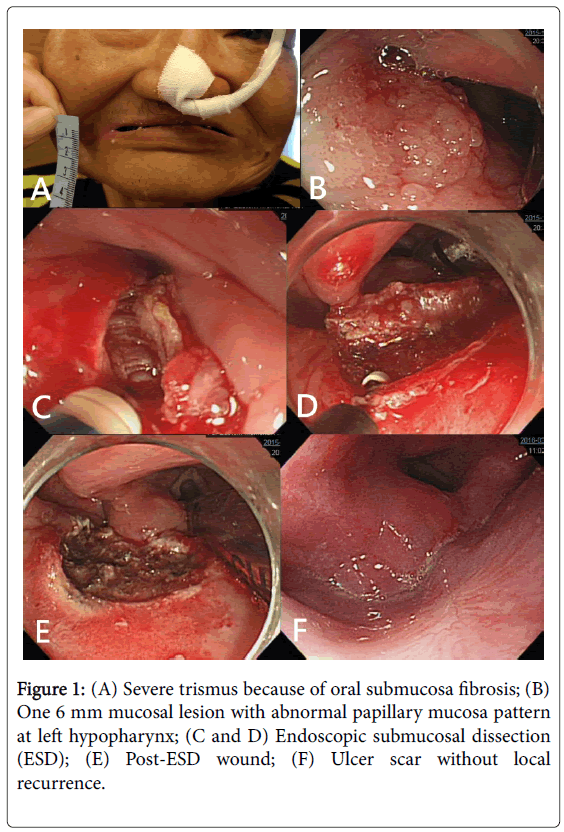
The mean (± SD) size of synchronous neoplasia were 9.0 (± 5.2) mm. After general anesthesia with endotracheal tube and assistance of adult size Lindholm operating laryngoscope (length 15 cm, Karl Storz 8587A), ESD were carried out by endoknives IT-nano (KD-612L, Olympus) and DualKnife (KD-650U, Olympus) with electrosurgial unit ESG-100 (Olympus, Tokyo, Japan; incision pulse-cut slow 25W dissection forced coagulation-2, 25W) without sub-mucosal lifting by solution injection (Figure 1).
Oral intake was resumed at second day after ESD. Histopathologically, horizontal margin free were achieved in all patients but one patient had vertical margin involvement who received concurrent chemoradiotherapy (CCRT) subsequently. During follow-up endoscopy at one year, there were no local recurrences in all patients. The 2-year overall survival were 100% with mean (± SD) of 46.7 (± 25.4) months.
Discussion and Conclusion
Due to common carcinogen exposure at H&N region and esophagus, SPTs are not uncommon in H&N cancer patients and the treatment strategy could be modified when synchronous neoplasia were detected [1]. Using IEE screening, especially NBI endoscopy and Lugol's chromo-endoscopy, the sensitivity/accuracy could be as high as 97%~100%/86~96% and 97%/82%, respectively, for the detection early neoplasia in H&N region or esophagus [1]. Early SPTs could be treated by minimally-invasive resection techniques with organ preservation and better QoL [3,4]. However, many of H&N cancer patients have trismus because of previous radiotherapy or oral submucosa fibrosis after long-term betel quid chewing, which makes passage of surgical instruments difficult. Transoral robotic surgery (TORS) is another choice for minimal invasive surgical technique for hypopharyngeal neoplasia, but not feasible due to trismus [4]. Under these circumstances, extensive field of resection is always needed to treat early synchronous neoplasia. In recent decade, the introduction of ESD technique using flexible video-endoscope and many kinds of endoknives has been widely applied in the treatment of early gastrointestinal tract neoplasia. The endoscopic resection technique has also been proposed as a minimally invasive treatment option with curative potential for SPTs that invades the subepithelial layer, although with local recurrence rate 13% after a median follow-up period of 71 months [5]. In our case series, one esophageal HGIN and one hypopharyngeal HGIN were treated by ESD alone without adjuvant therapy. One SCC of hypopharynx were resected with tumorfree resected margin followed by adjuvant local radiotherapy, and one hypopharyngeal SCC were resected with vertical margin involvement followed by CCRT. None of three patients had local recurrence during IEE surveillance and no procedure-related complication was noted. All patients tolerated oral intake 2 days after ESD and only mild degree throat pain was found. In conclusion, we believed that ESD of early SPTs in H&N cancer patients with trismus could be performed with curative potentials, reduced complication of treatment and improved QoL.
References
- Chung CS, Liao LJ, Lo WC, Chou YH, Chang YC, et al. (2013) Risk factors for second primary neoplasia of esophagus in newly diagnosed head and neck cancer patients: A case-control study. BMC Gastroenterol 13: 154.
- Muto M, Minashi K, Yano T, Saito Y, Oda I, et al. (2010) Early detection of superficial squamous cell carcinoma in the head and neck region and esophagus by narrow band imaging: a multicenter randomized controlled trial. J Clin Oncol 28: 1566-1572.
- Tateya I, Muto M, Morita S, Miyamoto S, Hayashi T, et al. (2016) Endoscopic laryngo-pharyngeal surgery for superficial laryngo-pharyngeal cancer. Surg Endosc 30: 323-329.
- Tateya I, Shiotani A, Satou Y, Tomifuji M, Morita S, et al. (2016) Transoral surgery for laryngo-pharyngeal cancer -The paradigm shift of the head and cancer treatment. Auris Nasus Larynx 43: 21-32.
- Satake H, Yano T, Muto M, Minashi K, Yoda Y, et al. (2014) Clinical outcome after endoscopic resection for superficial pharyngeal squamous cell carcinoma invading the subepithelial layer. Endoscopy 47: 11-18.
Relevant Topics
- Constipation
- Digestive Enzymes
- Endoscopy
- Epigastric Pain
- Gall Bladder
- Gastric Cancer
- Gastrointestinal Bleeding
- Gastrointestinal Hormones
- Gastrointestinal Infections
- Gastrointestinal Inflammation
- Gastrointestinal Pathology
- Gastrointestinal Pharmacology
- Gastrointestinal Radiology
- Gastrointestinal Surgery
- Gastrointestinal Tuberculosis
- GIST Sarcoma
- Intestinal Blockage
- Pancreas
- Salivary Glands
- Stomach Bloating
- Stomach Cramps
- Stomach Disorders
- Stomach Ulcer
Recommended Journals
Article Tools
Article Usage
- Total views: 3458
- [From(publication date):
June-2017 - Aug 23, 2025] - Breakdown by view type
- HTML page views : 2583
- PDF downloads : 875