Environmental Risk Factors and Social Determinants of Pulmonary Tuberculosis in Pakistan
Received: 08-Sep-2015 / Accepted Date: 25-Sep-2015 / Published Date: 30-Sep-2015 DOI: 10.4172/2161-1165.1000201
Abstract
Objective: To evaluate the role of potential environmental risk factors and social determinants associated with pulmonary tuberculosis in Pakistan.
Methods: Newly diagnosed pulmonary TB patients from August 2011-August 2014 from Gulab Devi Chest Hospital, Lahore, were recruited for this study. Two types of controls, house hold and community healthy controls (n=800 each) were selected. Multivariate analysis was performed to calculate odd ratios (OR) and observe the association of these factors with the disease.
Results: For host-related factors, TB was found to be significantly associated with male gender, married individuals, smoking, drinking, personal and family history of TB, asthma and diabetes (OR: 1.08, 1.96, 1.21, 4.26, 2.07, 3.16, 3.43 and 3.67) respectively with P-value <0.001. For environmental and socio economic factors TB was found to be associated with adult crowding, increased family size, poor ventilation and use of biofuels (OR: 4.60, 1.75, 3.29 and 3.90) illiteracy, unawareness of the disease, migration and presence of animals in the house (OR: 1.74, 0.07, 1.83 and 1.60) respectively with p-values of <0.005.
Conclusion: Information related to environmental and host related risk factors are very important to control the spread of infection and disease. Smoking, exposure to TB infected individuals, crowding ventilation and use of biofuels can be controlled by proper planning which are the risk factors of high potential found in this study. Proper health care facilities and education of people is also very important to control the disease.
Keywords: Tuberculosis; Environmental factors; Social factors; Multivariate analysis; Pakistan
163963Introduction
Tuberculosis (TB), the world’s deadliest communicable disease with an estimated 9.0 million cases of TB and 1.5 million deaths in 2013 throughout the world [1]. TB is a major health issue in resource limited countries. Despite immense progress in medical sciences and improved health care facilities in developed countries, TB remains one of the biggest challenges in resource poor setting and developing countries [2]. One of the obvious reasons for this dilemma is the involvement of multiple factors in increasing the susceptibility of infection and progression of the disease [3]. Pathogenesis of TB in man is a two stage process. In the first stage, the infection is initiated when a person is exposed to an infected individual and inhales the virulent bacterium through sneezing and coughing of an infected individual. Inhalation of droplet nuclei that are smaller enough (1-2 µm) to reach the alveolar surface of the lower respiratory tract can cause the infection. At this stage, a person’s duration to exposure, immune response, innate host resistance and other risk factors (environmental and social) play an important role to determine whether the infection will progress to disease or not. If a person having long duration of exposure and is also immunosuppressed, his chance of developing the disease will increase while in the opposite condition he can successfully overcome the infection [4].
Apart from host related factors, many environmental and social risk factors have been reported to be involved in the increased susceptibility of infection and progression of the disease [5-8]. Host related factors include genetics and gender of host, immune response, co-infection of HIV or other immunosuppressive disease like asthma, diabetes etc., smoking, drinking and malnutrition [9-11]. The environmental and social factors reported include proximity of contact, crowding, indoor pollution and use of biofuels (especially in rural areas), housing conditions, living style, ethnicity, education and socio-economic status. Several studies have reported these host-related, environmental and social risk factors of TB in different settings [12-14].
To our knowledge, no such study has been conducted in Pakistan which is ranked 5th in 22 TB high burden countries (HBC) with the incident rate of 231/100,000 population. The present study was aimed to investigate the host related, environmental and social risk factors of TB in a study conducted on newly diagnosed pulmonary TB patients of Gulab Devi chest hospital (GDH), Lahore, Pakistan from August 2011-August 2014.
Methods
Study area
The present study was conducted on newly diagnosed pulmonary TB patients presented to Out Door department (OPD) of Gulab Devi Chest Hospital (GDH), Lahore which is one of the biggest hospitals specialized for chest and respiratory infectious diseases in Pakistan. Pulmonary TB patients (n=800) of age >15 years were included in the study over a period of 3 years from August 2011-August 2014. The presence M. tb infection was confirmed by two consecutive smears and culture (Cul) on solid LJ media. The laboratory work for smear microscopy and culture was done in the Department of Microbiology, GDH and Department of the Pathology, Allama Iqbal Medical College (AIMC), Lahore, according to standard protocols provided by National TB Control Program, Pakistan (NTP) and the guidelines of World Health organization (WHO). Baseline information of demographic factors was obtained from NTP, Lahore, Pakistan.
Sample characterization
Samples were categorized into different groups after following the routine protocol for TB suspects in GDH according to the guidelines of NTP Pakistan. A person presented with the symptoms of cough for more than 2 weeks, fever, night sweats, cough with productive sputum, weight and appetite loss were considered as true TB suspects. Final selection was made on the basis of ZN microscopy result and culture results. Chest X-ray reports were also considered. Personal and clinical history of each patient was recorded. Two sputum specimens, one early morning and second spot samples are used to determine positivity by AFB microscopy. Based on the smear report patients are categorized into two main categories.
1. Sputum smear positive patients who are categorized as pulmonary TB smear positive cases and their anti-tuberculosis (ATT) treatment is started on the same day.
2. Sputum smear negative patients with chest x-ray suggestive of TB: these patients are considered as smear negative pulmonary TB patients; based on their clinical symptoms and chest x-ray report and are subjected to ATT.
Sample groups
Control group: Blood samples of the healthy individuals were taken from the same geographical area as the TB patients. Two types of controls were randomly selected, a house hold control (n=800) and a community control (n=800). All the controls were age matched within 8-10 years of the case irrespective of gender matching because it was a confounding factor. A house hold was defined as the extended family living in the same house or in neighboring area having frequent exposure with the case. House hold controls were selected to investigate the host related risk factors of the infection while community controls were selected to find out the environmental and social risk factors involved in the increased susceptibility of the infection.
Disease group: Blood and sputum samples were collected from AFB microscopy-positive (AFB+) TB patients and AFB microscopy-negative (AFB-) TB patients.
Sample collection and processing
Blood and sputum samples from TB patients (disease group) and healthy individuals (blood sample only) were obtained under the protocols approved through the institutional review boards (IRBs) at School of Biological Sciences, (SBS), University of the Punjab (PU). Blood samples were processed to separate plasma for antibody profiling (data not included in this study). All Sputum sample were processed for liquification and decontamination by a conventional mycobacterial N-acetyl L-cystein sodium hydroxide (NaOH-NALC) method. Briefly, fresh digestant of 4% NaOH and 2.9% Sodium Citrate+0.05 g NALC/100 ml was made. Equal quantity of digestant and sputum sample was mixed and allowed to settle for 20 minutes. After 20 minutes the volume was made up to 50 ml by adding 1x PBS, pH 6.8, mixed and centrifuged at 3000xg for 15 minutes. Pellet was dissolved in 3 ml of 1x PBS, pH 6.8. Following decontamination, aliquots were collected for M. tb detection by ZN staining, inoculation of MGIT tubes employed by the BACTEC™ MGIT™ 960 system and culturing on solid L J media and for extraction of total DNA.
DNA isolation: DNA isolation from culture samples was done by CTAB method. Briefly, two loops of mycobacteria were transferred into a micro centrifuge tube containing 400 μL of 1X TE. The cells were killed by heating for 20 min at 80°C, and cool at room temperature.50 μL of 10 mg/mL lysozyme was added followed by vortex and incubation at 37°, while shaking, for at least one hour. After lysis 75 μL of 10% SDS/proteinase K solution was added, vortex, and incubated for 10 min at 65°C. After incubation 100 μL of 5 M NaCl and 100 μL of prewarmed CTAB/NaCl solution was added and vortex until the liquid content becomes white ("milky"). It was then followed by incubation for 10 min at 65°C. After that 750 μL of chloroform/isoamyl alcohol was added and vortex for at least 10 seconds. The samples were centrifuged for 8 min at ±11,000xg at 4°C. To the supernatant 0.6 volume (450 μL) of chilled isopropanol was added and placed at -20°C for at least 30 min. After 30 minutes the samples were centrifuge for 15 min at ±11,000xg at 4°C. To the pellet 1 mL of cold 70% ethanol (from the -20°C freezer) was added followed by centrifugation for 5 min at ±11,000xg at 4°C. The pellet was dried for ±15 min at room temperature and dissolved in 50 ul of 1X TE. DNA quantification was done by spectrophotometer. The A260/A280 ratio of 1.8 was considered appropriate.
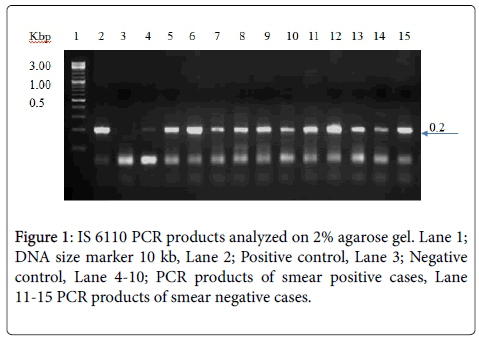
M. tb Infection confirmation through IS6110 PCR: The PCR was performed to amplify the IS6110 sequence of 200 bp. The primer sequences that were used for this target were: IS F 5’CCTGTCCGGGACCACCCGCGGCAA3’ and IS R 5’GGATCCTGCGACGTAGGCGTCGG3'. The optimized PCR conditions used were: 94°C for 5 min (initial denaturation) then 94°C, 30 sec (denaturation); 65°C, 30 sec (annealing); 72°C, 45 sec (extension) (35 cycles), then 72°C, for 10 min. PCR product were analyzed on 2% agarose.
Investigation of risk factors
The host-related factors investigated in this study were: gender, marital status, personal history of TB, family history of TB, smoking, drinking, nutritional status and intervention of other immune compromised diseases like asthma and diabetes. Environmental and socioeconomic factors included: household size, number of people per room, no. of adults in a family, no. of windows/room, structural composition of walls and floor, type of house, hygienic conditions, water supply, and presence of animals in the house, factory nearby house, socioeconomic status, education and awareness about TB.
The study was conducted with a consistent methodology using a standardized questionnaire. The study subjects were completely explained about the objectives of the study. The questionnaires were addressed to the study subjects by field assistants using the appropriate colloquial language. The presence of a BCG scar on the left or right deltoid region of the arm was checked. All the cases were screened for HIV using Rapid anti-HIV (1&2) test (Advanced Quality™) according to manufacturer’s instructions. All the cases were negative for HIV. Information was collected after the written consent from cases and controls on a wide range of potential host and environment-related risk factors for TB.
Statistical analysis
Data of risk factors obtained with the help of questionnaires from patient and control group was entered in Microsoft Excel 2010 version and transferred to SPSS (version 20) for analysis. Statistical analysis was conducted using TB index cases and household controls to assess the effect of host-related factors and TB index cases and community controls to assess the effect of environmental and social risk factors by performing multivariate analysis. Odds ratios (OR) and their 95% confidence intervals (CIs) were estimated using conditional logistic regression, with TB as an outcome. The likelihood ratio test was used to test the association between the explanatory variables and the risk of TB and for linear trend and interaction.
Results
During the study period, a total of 1000 cases of pulmonary TB cases were recruited. Out of 1000, 550 were smear positive and 450 were smear negative. From 550 smear positive cases, 500 were culture positive and from 580 smear negative cases, 300 were culture positive. The cases with culture negative or contaminated results were excluded from study. Finally, 800 cases each for TB index, household controls and community controls were recruited. Baseline information on demographic factors and Tuberculosis Control in Pakistan is given in Table 1.
| Demographic factors | Country: Pakistan |
|---|---|
| Population | 179 million |
| BCG Coverage | 94% |
| TB case detection rate | 65% per 100,000 population |
| SS+ cases cure rate | 92% |
| Defaulter | 11% |
| Relapse | 52% |
| Failure of treatment | 7% |
| Prevalence of TB (inclusive of HIV) | 376 per 100,000 population |
| Incidence of TB (inclusive of HIV) | 231 per 100,000 population |
| Incidence of HIV | 4% |
Table 1: Baseline Information of TB in Pakistan
All PCR products were loaded on 2% agarose gel and the results are shown in Figure 1.
Host related risk factors
Host related factors were investigated on the data obtained from house hold controls and TB index cases. Multivariate analysis was performed to compare the house hold controls and TB cases and the results are summarized in Table 3.
| Category | L J culture | IS 6110 PCR | ||
|---|---|---|---|---|
| Cul + | Cul- | PCR + | PCR- | |
| SS +ve (n=550) | 510(92.7%) | 40 (7.2%) | 500(98%) | 10 (1.9%) |
| SS-ve (n=450) | 290(64.4%) | 160(35.5%) | 278(95.8%) | 12 (4.1%) |
Table 2: Summary of culture and IS 6110 PCR results.
| Variable | Total cases (N=1600) | Controls (N=800) | Cases (N=800) | OR | 95%CI | p-value | |
|---|---|---|---|---|---|---|---|
| Gender | |||||||
| Female | 746 | 414 | 332 | 1 | |||
| Male | 854 | 386 | 468 | 1.087 | 1.24-1.84 | 0.0001 | |
| Marital Status | |||||||
| Unmarried | 1167 | 636 | 531 | 1 | |||
| Married | 433 | 164 | 269 | 1.965 | 1.56-2.46 | 0.0001 | |
| Drinking | |||||||
| No | 1569 | 794 | 775 | 1 | |||
| Yes | 31 | 6 | 25 | 4.269 | 1.74-10.46 | 0.001 | |
| Smoking | |||||||
| No | 811 | 425 | 386 | 1 | |||
| Yes | 789 | 375 | 414 | 1.216 | 0.99-1.47 | 0.051 | |
| Meals per day | |||||||
| Two | 1068 | 658 | 410 | 1 | |||
| Three | 532 | 142 | 390 | 4.408 | 3.50-5.53 | 0.0001 | |
| History of Asthma | |||||||
| No | 1379 | 723 | 77 | 1 | |||
| Yes | 221 | 656 | 144 | 2.061 | 1.53-2.77 | 0.0001 | |
| Treatment of Asthma | |||||||
| No | 1408 | 752 | 656 | 1 | |||
| Yes | 192 | 48 | 144 | 3.43 | 2.44-4.84 | 0.0001 | |
| History of Diabetes | |||||||
| No | 1240 | 705 | 535 | 1 | |||
| Yes | 360 | 95 | 265 | 3.67 | 2.83-4.67 | 0.0001 | |
| Treatment of Diabetes | |||||||
| No | 1235 | 700 | 535 | 1 | |||
| Yes | 365 | 100 | 265 | 3.67 | 2.83-4.67 | 0.0001 | |
| Personal history of TB | |||||||
| No | 979 | 558 | 421 | 1 | |||
| Yes | 621 | 142 | 479 | 2.076 | 1.69-2.54 | 0.0001 | |
| Family History of TB | |||||||
| No | 994 | 602 | 392 | 1 | |||
| Yes | 606 | 198 | 408 | 3.16 | 2.56-3.91 | 0.0001 | |
Table 3: A multivariate analysis of host related factors of TB; a comparison of TB cases and house hold controls. (N=1600).
The analysis showed that male gender was at higher risk of developing the disease as compared to female (OR=1.51). Similarly married individuals and smokers were more infected than single and non-smokers (OR=1.96 and 1.21 respectively). Although a small population was involved in drinking but drinking increased the risk of the disease (OR=4.26). The individuals who were also having asthma and its treatment were also at higher risk (OR=2.06 and 3.43 respectively) as compared to non-asthmatic individuals. Diabetic and its treatment also increased the risk of development of the disease (OR=3.67 and 3.67 respectively). Individuals having previous personal or family history of TB were at much higher risk of the disease. (OR+2.07 and 3.16 respectively). All this host related factors were significantly involved in the increasing risk of developing the disease with p value of 0.0001.
Environmental risk factors
Environmental risk factors investigated in this study were studied at community level. 800 cases each for community controls and TB index cases were compared to collect the data for environmental risk factors. The results are summarized in Table 3.
The multivariate analysis showed that risk of TB was significantly associated with crowding i.e. with increasing number of families living together (OR=4.60), families with larger size (OR=2.90) and having more number of adults (OR=4.60) were at higher risk of getting the infection with a p value of 0.0001 as compared to small size, single families and few young adults. The risk of TB infection transmission was high in setting with increased number of person/room (OR=2.78), having small sized house (OR=4.25) poor ventilation system with less no. of windows per room (OR=8.83) with p value of 0.0001. It was also observed that the risk of TB increased if the wall and floor of the houses were built with mud/brick rather than cement (OR=2.50 and 1.89) with a significant p-value of 0.0001. The risk of TB was significantly high when biofuels were used as cooking source (OR=3.90) as compared to gas or electric source. There was no significant relationship observed between incident cases and controls for the source of water, open/closed house types and the waste disposal inside or outside the house. The risk of TB was increased among the people who were living near some factory area (OR=2.30) with p-value of 0.0001.
Social risk factors
Community controls and TB index cases were compared to determine what type of socio-economic factors are associated with the increased susceptibility of the disease and the results are shown in Table 4.
| Variable | Total cases (N=1600) | Controls (N=800) | Cases (N=800) | OR | 95%CI | p-value | |
|---|---|---|---|---|---|---|---|
| No. of HH in a compound | |||||||
| 1 | 376 | 255 | 122 | 1 | |||
| 2 to 4 | 906 | 466 | 460 | 2.156 | 1.67-2.77 | ||
| >4 | 317 | 99 | 218 | 4.603 | 3.33-6.34 | 0.001 | |
| No. of people in HH | |||||||
| 1 to 5 | 403 | 256 | 147 | 1 | |||
| 6 to 10 | 778 | 387 | 391 | 1.759 | 1.37-2.25 | ||
| >10 | 419 | 157 | 262 | 2.906 | 2.18-3.85 | 0.001 | |
| No. of adults in HH | |||||||
| 1 to 5 | 400 | 277 | 123 | 1 | |||
| 6 to 10 | 786 | 387 | 399 | 2.322 | 1.80-2.99 | ||
| >10 | 414 | 136 | 278 | 4.603 | 3.42-6.18 | 0.001 | |
| Person/room | |||||||
| 1 to 2 | 212 | 138 | 74 | ||||
| 2 to 4 | 643 | 363 | 280 | 1.43 | 1.04-1.98 | ||
| >4 | 745 | 299 | 446 | 2.78 | 2.02-3.82 | 0.0001 | |
| No. of rooms | |||||||
| 1 to 2 | 12 | 4 | 8 | ||||
| 2 to 4 | 1044 | 710 | 334 | 4.251 | 1.27-14.21 | ||
| >4 | 544 | 86 | 458 | 0.376 | 0.11-1.27 | 0.0001 | |
| No. of windows/room | |||||||
| 1 | 543 | 109 | 434 | 1 | |||
| 2 | 898 | 619 | 279 | 8.83 | 6.85-11.37 | ||
| >2 | 159 | 72 | 87 | 3.29 | 2.26-4.80 | 0.0001 | |
| Composition of walls | |||||||
| Cement | 1486 | 720 | 766 | ||||
| Mud and brick | 114 | 80 | 34 | 2.50 | 1.65-3.78 | 0.0001 | |
| Composition of floor | |||||||
| Cement | 1431 | 692 | 739 | ||||
| Mud and brick | 169 | 108 | 61 | 1.89 | 1.35-2.63 | 0.0001 | |
| Source of water | |||||||
| Tap | 1194 | 635 | 559 | 1 | |||
| Well | 103 | 12 | 91 | 0.11 | 0.06-0.21 | ||
| Other | 303 | 153 | 150 | 0.89 | 0.69-1.15 | 0.0001 | |
| Source of cooking | |||||||
| Biofuel | 818 | 540 | 278 | 1 | |||
| Gas/electric | 782 | 260 | 522 | 3.90 | 3.16-4.79 | 0.0001 | |
| Factory near house | |||||||
| No | 508 | 183 | 325 | 1 | |||
| Yes | 1092 | 617 | 475 | 2.307 | 1.85-2.86 | 0.0001 | |
| Housing Condition | |||||||
| Closed | 962 | 571 | 391 | ||||
| Open | 638 | 229 | 409 | 0.38 | 0.31-0.47 | 0.0001 | |
| Waste disposal | |||||||
| Inside | 614 | 215 | 399 | ||||
| Outside | 986 | 585 | 401 | 0.36 | 0.30-0.45 | 0.0001 | |
Table 4: A multivariate analysis of Environmental risk factors of TB: Comparison of TB cases and community controls (N=1600).
Multivariate analysis of community controls and index cases showed that farmers were at higher risk of TB infection as compared to professionals or unemployed (OR=1.73) with p-value of 0.0001. The religion was not found to be associated with the risk of TB. People who migrated were at increased risk of getting the infection (OR=1.83). Education was also observed to be associated significantly with the risk of TB, the risk was high among illiterate people (OR=1.29) with a p-value of 0.007. The risk of TB was not found to be associated with ownership of the house but increased with the presence of animals in the house (OR=1.60) and p-value 0.005. People who were unaware of the symptoms and conditions of and diagnostic procedure of TB were at higher risk of infection as compared to those who had knowledge of the disease.
Discussion
The present study is the first study of its types conducted in a combined fashion in Pakistan to investigate the role of various host, environmental and social risk factors involved in the increasing risk of infection of TB in the population where TB is endemic. Gender was observed to be associated with the increasing risk of the infection which also has been reported previously [15,16]. Different studies from developed and developing countries have reported the gender variation in the prevalence of the TB infection and the disease [17-19]. This difference is more at the reproductive age group because of differential social roles and economic activities of the males at this age and also because of the differential response to delayed hypersensitivity in both the sexes [20-22].
In addition to age and sex differences in susceptibility related to biologic mechanisms, socioeconomic and cultural factors may also play a role in determining age and sex differences in the rates of infection, progression to disease, and treatment outcome. Active smoking was found to significantly increase the risk of infection in this study. It has been reported that active and passive smoking changes the structural and immunological host defense system which increases the risk of the infection [23].
Malnutrition was another profound risk for the TB in this study. As it affects cell-mediated immunity (CMI) which is the principal host defense against TB. The disease progresses rapidly in malnourished and immune compromised individuals. Various studies have shown that risk of progression of primary or latent infection to the active disease increases significantly in malnourished individual [11,24]. In a report on Nutrition and health, the US Surgeon General summarized the potential impact of malnutrition on the global incidence of TB suggesting that malnutrition is an important factor of acquired immune system dysfunction throughout the world [25].
People co-infected with diabetes or other immune compromised/respiratory infectious diseases are at a higher risk of the disease. Several studies have reported the association between diabetes and tuberculosis and found that people with diabetes are 2.5 times more likely to develop TB particularly in developing countries [26]. It has been observed that with increasing the no. of people in the household specially adults in a house doubles the risk of TB increased which has been justified by many studies [12,27-29].
In poorly maintained housing conditions with closed house types, less no. of rooms and windows/room and poor material used in the construction are also significant risk factors of increasing the TB incidence because it results in overcrowding and poor ventilation. These results are supported by various studies that showed that crowding, ventilation and housing conditions are markers of increased susceptibility of getting the infection [30,31].
TB is known as the disease of poverty. Social risk factors for infectious diseases have long been reported to be associated with one another. We found that increased incidence of cases are associated with unemployment, lack of education and migration which are all because of poverty, a marker of socio economic status. Very little data is available for the association of socio-economic status with TB in developing countries [32-37] (Table 5).
| Variable | Total cases (N=1600) | Controls (N=800) | Cases (N=800) | OR | 95%CI | p-value | |
|---|---|---|---|---|---|---|---|
| Occupation | |||||||
| Professional | 303 | 168 | 135 | 1 | |||
| unemployed | 704 | 385 | 319 | 1.03 | 0.78-1.35 | ||
| farmer | 593 | 247 | 346 | 1.74 | 1.31-2.30 | 0.0001 | |
| Religion | |||||||
| Muslim | 1570 | 780 | 790 | 1 | |||
| Christian | 30 | 20 | 10 | 0.46 | 0.18-1.16 | 0.103 | |
| Migration | |||||||
| No | 1520 | 780 | 740 | 1 | |||
| Yes | 80 | 20 | 60 | 1.83 | 1.05-3.18 | 0.31 | |
| Education | |||||||
| none | 362 | 126 | 236 | ||||
| primary | 359 | 116 | 243 | 1.29 | 0.92-1.80 | ||
| >5 years | 879 | 558 | 321 | 0.80 | 0.59-1.09 | 0.007 | |
| Ownership of the House | |||||||
| No | 186 | 92 | 94 | ||||
| Yes | 1414 | 708 | 706 | 0.97 | 0.71-1.32 | 0.876 | |
| Presence of Animals in house | |||||||
| No | 1296 | 710 | 586 | ||||
| Yes | 304 | 90 | 214 | 1.60 | 1.15-2.21 | 0.005 | |
| Awareness about TB | |||||||
| No | 1134 | 394 | 740 | 1 | |||
| Yes | 466 | 406 | 60 | 0.07 | 0.05-0.10 | 0.0001 | |
Table 5: A multivariate analysis of Socio economic risk factors of TB: Comparison of TB cases and community controls. (N=1600).
Conclusion
In this study, potential environmental, host-related and socio-economic risk factors have been found to be associated with the increased susceptibility of getting TB infection. Most important factors found were smoking, exposure to TB infected patient, co-infection of other diseases, crowding, poor ventilation, and increased family size. Illiteracy, poor health care facilities, low socio economic status are the added factors for increased risk of infection. Hence, this study provides useful information for association of risk factors with infection and disease that can be used to control the infection by reducing or eliminating the potential risk factors. It is also concluded from this study that people should be educated and facilitated with proper health care and medical facility and their living conditions should be improved so that the chance of the infection could be reduced to stop TB.
Acknowledgement
The authors would like to pay thanks to Faiza Arooj Khaliq and Asad Ahmed Khan for their valuable support in collection and management of the data.
Funding
This work was funded by Higher Education Commission (Grant Number 117-5210-BM7-10)
References
- Zumla A, George A, Sharma V, Herbert RH, Baroness M, et al. (2015) The WHO 2014 global tuberculosis report--further to go. Lancet Glob Health 3: e10-12.
- Jassal MS, Bishai WR (2010) Epidemiology and challenges to the elimination of global tuberculosis. Clin Infect Dis 50 Suppl 3: S156-164.
- Smith I (2003) Mycobacterium tuberculosis pathogenesis and molecular determinants of virulence. Clin Microbiol Rev 16: 463-496.
- Bennett S, Lienhardt C, Bah-Sow O, Gustafson P, Manneh K, et al. (2002) Investigation of environmental and host-related risk factors for tuberculosis in Africa. II. Investigation of host genetic factors. Am J Epidemiol 155: 1074-1079.
- Gupta S, Shenoy VP, Mukhopadhyay C, Bairy I, Muralidharan S (2011) Role of risk factors and socio-economic status in pulmonary tuberculosis: a search for the root cause in patients in a tertiary care hospital, South India. Trop Med Int Health 16: 74-78.
- Lönnroth K, Holtz TH, Cobelens F, Chua J, van Leth F, et al. (2009) Inclusion of information on risk factors, socio-economic status and health seeking in a tuberculosis prevalence survey. Int J Tuberc Lung Dis 13: 171-176.
- dos Santos MA, Albuquerque MF, Ximenes RA, Lucena-Silva NL, Braga C, et al. (2005) Risk factors for treatment delay in pulmonary tuberculosis in Recife, Brazil. BMC Public Health 5: 25.
- Diendere EA (2011) [Prevalence and risk factors associated with infection by human immunodeficiency virus, hepatitis B virus, syphilis and bacillary pulmonary tuberculosis in prisons in Burkina Faso]. Med Trop (Mars). 71: 464-467.
- du Preez K, Mandalakas AM, Kirchner HL, Grewal HM, Schaaf HS, et al. (2011) Environmental tobacco smoke exposure increases Mycobacterium tuberculosis infection risk in children. Int J Tuberc Lung Dis 15: 1490-1496, i.
- Byrd RP Jr, Mehta JB, Roy TM (2002) Malnutrition and pulmonary tuberculosis. Clin Infect Dis 35: 634-635.
- Baker M, Das D, Venugopal K, Howden-Chapman P (2008) Tuberculosis associated with household crowding in a developed country. J Epidemiol Community Health 62: 715-721.
- Schoeman JH, Westaway MS, Neethling A (1991) The relationship between socioeconomic factors and pulmonary tuberculosis. Int J Epidemiol 20: 435-440.
- Lienhardt C, Fielding K, Sillah JS, Bah B, Gustafson P, et al. (2005) Investigation of the risk factors for tuberculosis: a case-control study in three countries in West Africa. Int J Epidemiol 34: 914-923.
- Lienhardt C, Bennett S, Del Prete G, Bah-Sow O, Newport M, et al. (2002) Investigation of environmental and host-related risk factors for tuberculosis in Africa. I. Methodological aspects of a combined design. Am J Epidemiol 155: 1066-1073.
- Holmes CB, Hausler H, Nunn P (1998) A review of sex differences in the epidemiology of tuberculosis. Int J Tuberc Lung Dis 2: 96-104.
- Ogden J (2000) The resurgence of tuberculosis in the tropics. Improving tuberculosis control--social science inputs. Trans R Soc Trop Med Hyg 94: 135-140.
- Leung CC, Lam TH, Yew WW (2007) Smoking and tuberculosis: infection, disease, and mortality. Arch Intern Med 167: 2008-2009.
- Roelsgaard E, Iversen E, Blocher C (1964) Tuberculosis in tropical africa. An epidemiological study. Bull World Health Organ 30: 459-518.
- Borgdorff MW, Nagelkerke NJ, Dye C, Nunn P (2000) Gender and tuberculosis: a comparison of prevalence surveys with notification data to explore sex differences in case detection. Int J Tuberc Lung Dis 4: 123-132.
- Begum V, de Colombani P, Das Gupta S, Salim AH, Hussain H, et al. (2001) Tuberculosis and patient gender in Bangladesh: sex differences in diagnosis and treatment outcome. Int J Tuberc Lung Dis 5: 604-610.
- Diwan VK, Thorson A (1999) Sex, gender, and tuberculosis. Lancet 353: 1000-1001.
- Altet-Gômez MN, Alcaide J, Godoy P, Romero MA, Hernández del Rey I (2005) Clinical and epidemiological aspects of smoking and tuberculosis: a study of 13,038 cases. Int J Tuberc Lung Dis 9: 430-436.
- Chandra RK (1987) Nutrition and immunity: practical applications of research findings. Can Fam Physician 33: 1417-1420.
- McGinnis JM (1988) The Surgeon General's report on nutrition and health. R I Med J 71: 373.
- Jeon CY, Murray MB (2008) Diabetes mellitus increases the risk of active tuberculosis: a systematic review of 13 observational studies. PLoS Med 5: e152.
- Ottmani SE, Murray MB, Jeon CY, Baker MA, Kapur A, et al. (2010) Consultation meeting on tuberculosis and diabetes mellitus: meeting summary and recommendations. Int J Tuberc Lung Dis 14: 1513-1517.
- Wanyeki I, Olson S, Brassard P, Menzies D, Ross N, et al. (2006) Dwellings, crowding, and tuberculosis in Montreal. Soc Sci Med 63: 501-511.
- Clark M, Riben P, Nowgesic E (2002) The association of housing density, isolation and tuberculosis in Canadian First Nations communities. Int J Epidemiol 31: 940-945.
- STEIN L (1952) Tuberculosis and the "social complex" in Glasgow. Br J Soc Med 6: 1-48.
- Mangtani P, Jolley DJ, Watson JM, Rodrigues LC (1995) Socioeconomic deprivation and notification rates for tuberculosis in London during 1982-91. BMJ 310: 963-966.
- Wong MK, Yadav RP, Nishikiori N, Eang MT (2013) The association between household poverty rates and tuberculosis case notification rates in Cambodia, 2010. Western Pac Surveill Response J 4: 25-33.
- Oxlade O, Murray M (2012) Tuberculosis and poverty: why are the poor at greater risk in India? PLoS One 7: e47533.
- Barter DM, Agboola SO, Murray MB, Bärnighausen T (2012) Tuberculosis and poverty: the contribution of patient costs in sub-Saharan Africa--a systematic review. BMC Public Health 12: 980.
- Creswell J, Jaramillo E, Lönnroth K, Weil D, Raviglione M (2011) Tuberculosis and poverty: what is being done. Int J Tuberc Lung Dis 15: 431-432.
- Casali L, Crapa ME (2010) Women, immigration, poverty and tuberculosis. Multidiscip Respir Med 5: 398-400.
- Geraldes Santos Mde L, Figueiredo Vendramini SH, Gazetta CE, Cruz Oliveira SA, Scatena Villa TC (2007) Poverty: socioeconomic characterization at tuberculosis. Rev Lat Am Enfermagem 15 Spec No: 762-767.
Citation: Khaliq A, Khan IH, Akhtar MW, Chaudhry MN (2015) Environmental Risk Factors and Social Determinants of Pulmonary Tuberculosis in Pakistan. Epidemiology (sunnyvale) 5:201. DOI: 10.4172/2161-1165.1000201
Copyright: © 2015 Khaliq A, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 24551
- [From(publication date): 9-2015 - Aug 23, 2025]
- Breakdown by view type
- HTML page views: 19071
- PDF downloads: 5480