Evidence-Based Medicine: A Study of Signs and Signals of the Person in Coma
Received: 19-Feb-2016 / Accepted Date: 26-Apr-2016 / Published Date: 03-May-2016 DOI: 10.4172/2471-9919.1000106
Abstract
This is an experimental research with quantitative and qualitative approach in order to identify the signifiers of body language in a coma and signs that express the machine connected to it resulting from nursing care. The procedures chosen were the technique of in-bed bath, oral hygiene and intimate hygiene. The study population consisted of 30 subjects. The main significant findings were wrinkles on forehead, close eyes tightly, crying, smiling, tongue protrusion, facial flushing, look toward the person, sweat on forehead. The main signs were shortness of breath and increased heart rate. All variables related to signals presented by the machinery connected to the patient’s body in a coma, respiratory rate, heart rate and diastolic and systolic blood pressure showed significant statistical difference (p<0.0001) between before and after nursing care.
Conclusion: We conclude that the answer to question this study is given when we say that the person in coma is expressed through significant understood as expressions of the body and, through such signs as the records show that the physiology through the machine.
Keywords: Nursing Care; Coma; Body; Non-verbal language
41781Introduction
We have no doubt that this issue is a further complicating the challenge us because this is not the speech that usually used in care. There is an understanding of the professionals, teachers and students of Nursing, which before thinking-how semiotics and semiotics is necessary to think of semiotics to the care science.
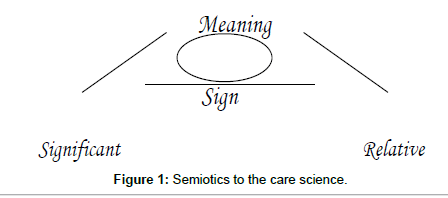
Semiology is a part of linguistics, more precisely, the part that is in charge of large meaningful units of speech. The referent, the signifier and the signified are the components of a sign, which the referent object or simply the referent is that which the sign refers, the plan of significant is the level of expression and the level of significance, the plan content [1]. The meaning is the act that unites the referent, signifier and signified, whose product of this union is the sign as shown in formula (Figure 1) [2]:
In the search for a reading of the body that is expressed through signs, we have held us significant. We are in search of what is for us the significant issued by the subject of our attention.
This subject, silent by the disease. Unable to communicate verbally in an environment with an atmosphere often impersonal within an Intensive Care Unit (ICU). To assist the patient is said to be premised on the need to understand it, to deliver nursing care, and this understanding will be coming from what he expresses verbally and the non-verbal. With this, there will always be communication, recognizing that even silence is a way to communicate. To do so, the nurse will have to stay tuned to different channels where the interaction is occurring [3].
Objectives
• Register the signs and signals identified as the client’s body language in a coma in the ICU resulting nursing care.
• Discuss the implications of the data produced resulting nursing care with the client’s body in a coma
Materials and Methods
Experimental research with quantitative and qualitative approach that does not follow the guidelines of the research under control as it is in the basic sciences. There is research, which while not having random distribution of the subjects or control groups, are developed quite rigorous methodology and approach to be quite basic experimental research [4]. Opting for this type of study it is given by the fact that through an experimental study it is possible to see what happens, when it happens, who is and how it occurs, making it possible to analyze cause-effect relationships; are studies that provide validation of clinical practice and rationale to change specific aspects of practice being useful for the development of nursing knowledge for testing the effects of nursing actions [5]. When we use the quantitative and qualitative approach to research, we allow each method plays its part by avoiding limitations of the unique approach thus leading to the enrichment of the research. Although qualitative data prevail in the field of study, researchers sometimes may include quantitative measures to work to take advantage of a more structured information gathering [6].
The site chosen for data collection was the CTI of two district hospitals of the City of Rio de Janeiro. The collect data started after the approval of the Ethics in Research of the Municipal Health Secretariat of Rio de Janeiro numbering 0054.0.314.000-09 and 0055.0.314.000-09 Committee and thus serve the requirements of Resolution 466/2012 National Health Council.
Patients chosen for the study includes the following criteria
• To be admitted to the ICU.
• Being in a coma (or unable to speak).
• Over 18 years old.
• Either sex.
• Sedated or not.
• Score in Glasgow Scale of coma greater than or equal to three.
Currently, in the ICU, the team uses scale as an important resource to grade the level of consciousness of patients, providing a quantitative method of assessing and facilitating the visualization of the evolution of the mental level of these patients. The most used is the Glasgow Coma Scale, which scores the patient’s reactions to your perceptual system. It was first published in 1974 by Teasdale and Jennet at the University of Glasgow (Scotland) in order to standardize the clinical observations of patients with head trauma and consciousness changes. Its use has spread both in Neurological Intensive centers as in emergencies, and is now known worldwide. This scale has also been incorporated into instruments designed to capture the severity of disease and multisystem trauma [7-12].
The Glasgow Coma Scale has three markers assessment - eye opening, best verbal response, and best motor response, the total score being provided by the sum of these markers and range of at least 3 and a maximum of 15 points. A score lower than 8 is commonly accepted as critical of changes in the level of consciousness and as the score which defines an individual in a coma [13].
Another clinical situation in the ICU, where there is change in the level of consciousness and the patient’s responsiveness occurs when they are used the sedating therapies, that is, the state of coma becomes induced. Sedation is the pharmacological use of depressants of the central nervous system (CNS) to reduce the fear, anxiety and agitation. The need of sedation is based on the underlying pathological condition, the primary goals of treatment in response to physiological stress disorder and in the presence of agitation and delirium [14].
On the other hand, improper administration of sedatives may increase the morbidity of patients admitted to an ICU. Those insufficiently sedated may have psychomotor agitation that predisposes to potentially dangerous events, such as the inadvertent removal of catheters and endotracheal tubes, or even complications of adrenergic discharge and the occurrence of myocardial infarction.
The scale of Ramsay Sedation is a resource used for assessment of agitation and sedation effectiveness. This sedation protocol consists of a care plan that guides the ICU professionals in achieving sedation goal and efficient control of agitation and delirium; further emphasizing the importance of patient comfort as a matter of quality. Research shows that this protocol, when properly used, can reduce the time of sedation, hospitalization in the ICU, in the hospital and mechanical ventilation [14].
The score of Ramsay scale was used for the sedated patient since it could not be applied to the Glasgow scale because of sedation. Using the Ramsey scale, we can assess the level of consciousness of the patient sedated.
The chosen procedures were the technique of Bath on Bed, Oral Hygiene and Intimate Hygiene to be the moment in which we believe to be in closer contact with the patient, more time, and considered those that invade privacy, rich tones and tactile stimuli that stimulate responses signifying a body that does not speak.
Results
After registering the information of 30 customers and notices on the machine we explore the material produced (data organization) through the construction of three tables: In the 30 clients who composed the sample studied, the 03 proposed procedures were performed (bed bath, personal hygiene and oral hygiene), each client being played 50 times, creating a total sum 1500 touches (Tables 1-3).
| Patient | Age | Gender | Glasgow | Ramsay | Situation Disease |
|---|---|---|---|---|---|
| 01 | 69 | Female | 04 | 05 | Hepatic impairment |
| 02 | 70 | Female | 06 | 01 | Post-OP vascular surgery |
| 03 | 78 | Female | 05 | 01 | Post-OP subdural hematoma |
| 04 | 56 | Female | 07 | 02 | Pancreatitis |
| 05 | 82 | Male | 09 | -- | Septicemia |
| 06 | 44 | Male | 11 | -- | Brain Tumor |
| 07 | 54 | Male | 03 | 06 | Traumatic brain injury |
| 08 | 85 | Male | 08 | -- | Ischemic Stroke |
| 09 | 34 | Male | 03 | 06 | Trauma brain injury |
| 10 | 40 | Female | 09 | -- | Hemorrhagic Stroke |
| 11 | 35 | Male | 03 | 06 | Post-OP of fusion for spinal cord trauma |
| 12 | 80 | Male | 06 | 06 | orthopedic trauma - femur fracture |
| 13 | 78 | Female | 06 | 01 | Acute lung edema |
| 14 | 68 | Male | 07 | -- | Peritonitis |
| 15 | 38 | Male | 09 | 05 | facial trauma - right temporal hematoma |
| 16 | 83 | Female | 08 | -- | Congestive heart failure and chronic atrial fibrillation |
| 17 | 82 | Male | 10 | 05 | Peritonitis - colon tumor |
| 18 | 57 | Female | 09 | 01 | Peritonitis |
| 19 | 28 | Female | 08 | 01 | Vascular Brain hemorrhagic accident |
| 20 | 70 | Male | 05 | -- | chest trauma pelvis + + tibia fracture and right pneumonia |
| 21 | 55 | Male | 08 | 02 | Post-OP vascular surgery |
| 22 | 71 | Male | 06 | -- | Pneumonia + erysipelas |
| 23 | 73 | Male | 09 | -- | Vascular Brain Ischemic accident |
| 24 | 85 | Male | 03 | 06 | femur fracture + pulmonary fibrosis |
| 25 | 38 | Male | 08 | 01 | Fracture C6 and C7 |
| 26 | 51 | Male | 10 | 01 | Post-OP transmetatarsalbilateral |
| 27 | 23 | Male | 05 | 06 | Failure kidney + Congestive Heart Failure + cardiomegaly |
| 28 | 84 | Male | 05 | 06 | urinary sepsis + septic shock |
| 29 | 51 | Male | 10 | 04 | pancreatitis |
| 30 | 84 | Male | 09 | 01 | heart attack |
Table 1: Characterization of patients.
| Customers | Procedures | Touch | Total touches |
|---|---|---|---|
| 30 | Bath in Bed | 30 | 900 |
| 30 | Intimate hygiene | 12 | 360 |
| 30 | Oral hygiene | 08 | 240 |
Table 2: Touch the movements of care.
| Patients | Procedures | Significants |
|---|---|---|
| 01 | Bed bath | Hair of spiky arms |
| 02 | Bed bath | closed his eyes tightly |
| 03 | intimate hygiene | Contraction of the legs |
| 04 | Bed bath | A tear rolled |
| 05 | Bed bath | blinked |
| 06 | Bed bath | smiled |
| 07 | Bed bath | blinked |
| 08 | oral hygiene | tongue protrusion |
| 09 | intimate hygiene | twitching of the legs |
| 10 | Bed bath | Movement with open eyes (Watching us) |
| 11 | Bed bath | Wrinkles on the forehead |
| 12 | Bed bath | Wrinkles on the forehead |
| 13 | oral hygiene | Wrinkles on the forehead |
| 14 | oral hygiene | Smiled |
| 15 | oral hygiene | tongue retraction |
| 16 | oral hygiene | tongue protrusion |
| 17 | oral hygiene | Movement with the fingers |
| 18 | intimate hygiene | twitching of the legs |
| 19 | intimate hygiene | twitching of the legs |
| 20 | intimate hygiene | Movement with your toes |
| 21 | intimate hygiene | Movement with your toes |
| 22 | oral hygiene | opened his mouth |
| Bed bath | closed his eyes tightly and wrinkles on the forehead | |
| 23 | oral hygiene | closed his eyes tightly |
| Bed bath | Facial flushing contraction of the legs and diaphragm muscle | |
| intimate hygiene | Facial flushing and wrinkles on the forehead | |
| 24 | Bed bath | Biting teeth |
| 25 | Bed bath | abundant sweat |
| 26 | Bed bath | Wrinkles on the forehead |
| 27 | intimate hygiene | internal eye movement |
| 28 | Bed bath | internal eye movement |
| 29 | oral hygiene | Shut your mouth |
| 30 | oral hygiene | Shut your mouth |
Table 3: Overall picture of the person's body language in a coma.
It is important to inform the normal parameters of vital signs so that the data of the findings can be compared.
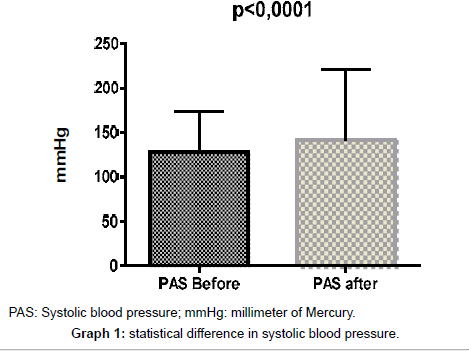
Normal blood pressure: The normal blood pressure in adults is 120 (systolic)/80 (diastolic) (Tables 4-6) (Graph 1-4).
| Mean | Median | Std. Deviation | N. Min | N. Max | ||||||
|---|---|---|---|---|---|---|---|---|---|---|
| Before | after | Before | after | Before | after | Before | after | Before | after | |
| PAS | 127,0 | 142,8 | 128,5 | 141,5 | ± 21,78 | ±28,12 | 80,0 | 88,0 | 174,0 | 221,0 |
| PAD | 73,37 | 82,47 | 71,00 | 84,50 | ± 15,00 | ±18,27 | 43,0 | 48,0 | 110,0 | 137,0 |
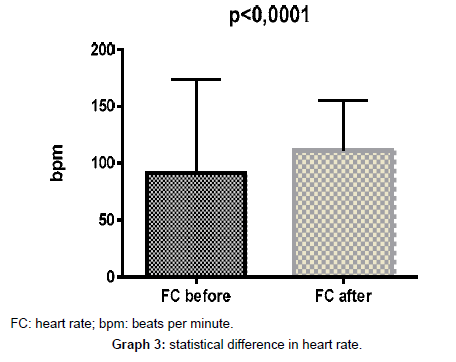
| FC | 91,37 | 107,0 | 91,50 | 111,0 | ± 25,19 | ±23,86 | 56,00 | 65,0 | 173,0 | 155,0 |
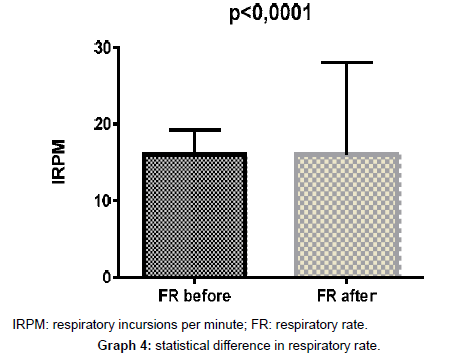
| FR | 17,83 | 21,80 | 16,00 | 16,00 | ± 4,434 | ±8,560 | 9,000 | 12,0 | 28,00 | 51,00 |
FC = heart rate; FR = respiratory rate; PAS = Systolic blood pressure; PAD = diastolic blood pressure; N. Min = minimum number; N. Max = maximum number.
Table 4: Inferential statistics of the person's body signals in a coma.
| Approximate Age Range | Heart Rate |
|---|---|
| Newborn | 100-160 |
| 0-5 months | 90-150 |
| 6-12 months | 80-140 |
| 1-3 years | 80-130 |
| 3-5 years | 80-120 |
| 6-10 years | 70-110 |
| 11-14 years | 60-105 |
| 15-20 years | 60-100 |
| Adults | 50-80 |
Table 5: Normal Heart Rate by Age.
| Approximate Age Range | Respiratory Rate |
|---|---|
| Newborn | 30-50 |
| 0-5 months | 25-40 |
| 6-12 months | 20-30 |
| 1-3 years | 20-30 |
| 3-5 years | 20-30 |
| 6-10 years | 15-30 |
| 11-14 years | Dec-20 |
| 15-20 years | Dec-30 |
| Adults | 16-20 |
Table 6: Normal Respiratory Rate by Age.
Discussion
It is essential to tell you how to develop this study was difficult operation due to the complexity, not specifically object, but the question we wanted to answer. Complexity effectively involves the fabric knowledge, actions, interactions, retroactions, determinations, chances are that the phenomenal world [7]. This assertion is the background of this research involved a body “silence” a coma and the attempt of Nursing seek a language that did not involve speech, but signs and signals of a body of a living person.
Semiology is a part of linguistics, more precisely, the part that is in charge of large meaningful units of speech. The referent, the signifier and the signified are the components of a sign which the referent object or simply the referent is that which the sign refers, the plan of significant is the level of expression and the level of significance, the plan content. The meaning is the act that unites the referent, signifier and signified, whose product of this union is the sign [1]. We believe that the analysis of the following categories can enlarge our thoughts and statements.
1st Category
The signs are in body language during care: the emergence of significant visible in the body. The body is alive, no doubt, the disease stopped his voice, but cannot control his expression. The three above data show that life is in the body that we care. A patient in his bed, presents property, not to mention and to be touched procedures: talk through “forehead wrinkles”, “heartbeat”, “jaw movement”, “close and open the mouth” “control has legs” and “cries”, you cannot say that it is the indifferent.
Perhaps the biggest implication of this study, not in the sense of magnitude, but the complexity involved in the clinical view of nursing as a building movement for Semiotics care, is the emergence of significant visible in the body.
The implications with regard to the sign, involve communication when the non-verbal language when captured by the Nurse reverses in meeting some of the needs expressed by customers and effective resolution of their problems [8].
It is amazing to note that patients with scores four on the Glasgow coma scale present significant as, for example, a tear when you hear the voice of the nurse and this informs her that his family is waiting for the end procedure to be able to see it.
Moments like this are what make us realize how important is the perception and awareness on the part of us health professionals that all the time that body “trapped” in a parallel world because of illness may be trying to communicate and for that, using non-verbal communication that we have identified, but we cannot say is that he wants this, then do that...
The mind is not just in the brain but through the body in caravans of hormones and enzymes, engaged in making sense of the wonders that the body catalogs as touch, taste, smell, hearing and vision [9].
An important aspect that emerges from the client’s body language is that 100% of subjects surveyed had some sort of expression in your callsign body significantly ranging from a snap or a movement of lips to the “silence” of the body, once what has been said earlier in this study that even the “silence” may be the unspoken seen the inside of language.
What caught our attention the fact that 80% of individuals surveyed reported some kind of facial expression. This can be clarified because the face is the most exposed part of the human body, and is where the emotions are mostly demonstrated [10]. So we Nurses need to be aware of what occurs on the faces of our customers in order to realize emotions of evidence not expressed verbally, enabling individualized and holistic care.
When the symptomatology consisted of international conferences object, the word was examined seriously and it was proposed to replace it with the word semiotics, and this for a reason that particularly concerns us here: in order to avoid confusion between the semiotics of linguistic origin and the clinical examination.
We understand that the very Semiotics of Nursing Care values the profession in building your knowledge while a Health Science concerned with the interaction between the client and the nurse knowing that nonverbal communication is part of this interaction [11].
It is clear to us, analyzing the results, we can consider the client’s body expressions as indicative of significant interaction for the nursing care, interaction such that when effective, can be called nonverbal communication.
2nd Category
Signs before and after care: changes in heart rate, respiratory rate and blood pressure - the significant technology. All variables related to signals presented by the machinery connected to the patient’s body in a coma, respiratory rate, heart rate and diastolic and systolic blood pressure showed significant statistical difference (p<0.0001) before and after nursing care.
This category is a Nursing look at the machine connected to the client’s body in a coma, unable to speak and that is expressed through signs on the monitor. These signals are the result of care provided - Bath in Bed - as a nursing technique (mandatory for bedridden clients).
Machine care that records signals is a new thinking of the careful way, because it has been part of a body that can not only breathe, eliminating only, feed themselves only. At the same time it has been our concrete and not intersubjective assurance that contribute to the healing of the physical body and interpret for us measurable signals.
There is no machine that wow before a body that expresses this feeling, but records concrete signs of emotion when it shows a heart stroke that redraws a heart rate increases or decreases. So it is essential to take care of it, which requires technical and rational knowledge, based on protocols and algorithms, and has the “false image” to contribute to the emergence of signs that relate to the behavior, we have called “careless”.
By looking at the camera and say that the heart rate (the body) increased or decreased during the bed bath is to recognize the human running as energy via electricity contained in the machine wire. Life is there, the heart monitor attached to the body that expresses itself in signs.
Conclusion
The answer to the question of this study is given when we say that the body of the comatose person speaks through signs understood and body expressions and points to the semiotics of care, and through signs as the body’s internal physiology of records that shows on the monitors of the machines attached to it at the time of nursing care when we bath in bed, intimate hygiene and oral hygiene.
This discovery should continue to stimulate further research because this is an issue that concerns all those who care for a client who does not speak but is expressed through signs and signals.
References
- Barthes R (1992) Elementos de Semiologia. Traducao Izidoro Blikstein. Sao Paulo: Cultrix.
- Dias Bordenave JE (1998) Alem dos Meios e Mensagens: introducao a comunicacao Como processo, tecnologia, sistema e ciência. 3 ed. Petrópolis: Vozes.
- Gil AC (1999) Métodos e tecnicas de pesquisa social. 5. ed. Sao Paulo: Atlas.
- Dell'Acqua MCQ, Araujo VA de, Silva MJP da (1998) Toque: qual o USO atual pelo enfermeiro? Rev. Latino-Am. Enfermagem v.6 n.2 Ribeirao Preto abr.
- Lobiondo G, Haber J, Pesquisa em enfermagem, Metodos, Avaliaçao e Utilizacao (2001) 4 ed. Rio de Janeiro: Guanabara Koogan.
- Polit DF, Cheryl TB, Hungler BP (2004) Fundamentos de pesquisa em enfermagem: metodos, avaliação e utilização. Tradução Ana Thorell. 5 ed. Porto Alegre: Artmed.
- Morin E (1990) Introdução ao pensamento complexo. Instituto Piaget, 2ª ed. Lisboa.
- Ferreira MA (2006) A comunicação no cuidado: uma questão fundamental da enfermagem. Revista Brasileira de Enfermagem 2006 maio-junho 59: 327-30.
- Ackermam D (1992) Uma história natural dos sentidos. Rio de Janeiro; São Paulo: Bertrand do Brasil.
- Watzlawick PA (1967) Pragmática da Comunicação Humana. São Paulo: Editorial.
- Taets GG De C, Figueiredo NMA de (2009) Silent language of the body that is care: a study in metaanalysis for a semiotic under construction. Rev Enferm UFPE on Line 3: 335-339.
- Koizume MS (2000) Avaliação neurológica utilizando a Escala de Coma de Glasgow: origem e abrangência. Acta Paul Enferm 13: 90-94.
- Muniz ECS, Thomaz MCA, Kubota MY, Cianci L, Souza RMC (1997) Utilização da Escala de Coma de Glasgow e Escala de Coma de Jouvet para avaliação do nÃvel de consciência. Rev Esc Enferm USP 31: 287-303.
- Schell HM, Puntilho KA (2005) Segredos em enfermagem Na terapia intensiva. Trad. de Regina Garcez. Porto Alegre: Artmed.
Citation: Gunnar Glauco DCT (2016) Evidence-Based Medicine: A Study of Signs and Signals of the Person in Coma. Evidence Based Medicine and Practice 1: 106. DOI: 10.4172/2471-9919.1000106
Copyright: ©2016 Gunnar Glauco DCT. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Select your language of interest to view the total content in your interested language
Share This Article
Recommended Journals
Open Access Journals
Article Tools
Article Usage
- Total views: 4930
- [From(publication date): 0-2016 - Aug 20, 2025]
- Breakdown by view type
- HTML page views: 3960
- PDF downloads: 970