Research Article Open Access
Improvements of Muscle Strength and Gait Ability among Chronic Post-Stroke Patients by Gait Training with a Footpad-Type Locomotion Interface
| Naoki Tanaka1,2, Takeshige Kanamori2, Hideyuki Saitou2, Hiroaki Yano3, Junko Okuno1and Hisako Yanagi1* | |
| 1Department of Medical Science and Welfare, Graduate School of Comprehensive Human Sciences, University of Tsukuba, Tsukuba, 305-8577, Japan | |
| 2Department of Rehabilitation, Tsukuba Memorial Hospital, Japan | |
| 3Department of Intelligent Interaction Technologies, Graduate School of Systems and Information Engineering, University of Tsukuba, Japan | |
| Corresponding Author : | Dr. Hisako Yanagi Institute of Medical Science and Welfare Faculty of Medicine, University of Tsukuba Tennoudai 1-1-1, Tsukubashi, Ibaraki-ken 305, Japan Tel: 81-298-53-3496 Fax: 81-298-53-3039 E-mail: hyanagi@md.tsukuba.ac.jp |
| Received July 01, 2012; Accepted September 18, 2012; Published September 21, 2012 | |
| Citation: Tanaka N, Kanamori T, Saitou H, Yano H, Okuno J, et al. (2012) Improvements of Muscle Strength and Gait Ability among Chronic Post-Stroke Patients by Gait Training with a Footpad-Type Locomotion Interface. J Nov Physiother S1:002. doi: | |
| Copyright: © 2012 Tanaka N, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Objective: We examined the effects of gait training using an original footpad-type locomotion interface named GaitMaster for chronic stroke patients.
Method: Ten chronic hemiparetic patients after stroke participated. The subjects were divided randomly into two groups (n=5 each). Group A subjects followed an ‘intervention phase’ and then a ‘non-intervention phase’, and group B subjects followed the ‘non-intervention phase’ and then the ‘intervention phase.’ In the intervention phase, the subjects underwent twelve 20-min sessions of gait training using the Gait Master. In the non-intervention phase, they performed the same typical rehabilitation or exercise they had been doing before beginning their anticipation in the study.
Main Outcome Measures: We measured the subjects’ gait speed and the isometric muscle strength of hip flexion and extension once a week or after every three Gait Master training sessions.
Results: No significant differences were observed in the clinical data at baseline between the groups. The maximum gait speed improved significantly in the intervention phase compared to the non-intervention phase (p<0.05). Muscle strength in paretic hip flexion (p<0.05), non-paretic hip flexion (p<0.05), and paretic hip extension (p<0.05) improved significantly after the intervention phase compared to the non-intervention phase.
Conclusions: These results suggest that gait training using the Gait Master can improve gait ability and the muscle strength of both paretic hip flexion and extension, and that gait rehabilitation using the Gait Master will be effective for chronic stroke patients.
| Keywords |
| Foot-pad type locomotion interface; Gait rehabilitation; Gait speed; Muscle strength |
| Introduction |
| Gait rehabilitation has changed from traditional unaffected sidemuscle strength enhancement, brace therapy, and neurophysiological approaches such as the Bobath approach [1] to a task-specific approach. Body weight-support treadmill training is representative of task-specific approaches to gait rehabilitation. In body weight-support treadmill training, which was developed by Finch et al., the subject is fitted with harness and performs treadmill training [2]. Body weightsupport treadmill training is based on the theoretical concept that a central pattern generator can be facilitated [3,4]. Since Hesse et al. reported improved gait ability by body weight-support treadmill training in stroke patients in 1994 [5], many body weight-support treadmill training-based studies have been conducted, mainly in stroke patients [6-10]. These studies found that repetitive movement and hip extension movement are important aspects of body weightsupport treadmill training [11,12], and therefore, support by physical therapists is indispensable for body weight-support treadmill training, although physical therapists’ adoption of this method increases their burden. |
| To address this problem, robotic applications such as Lokomat [13,14] and Gait Trainer [15,16] were developed to help patients swing their lower limbs. Werner et al. compared the Gait Trainer with body weight-support treadmill training and reported that patients in both groups improved their gait ability, walking velocity, and other motor functions considerably during the treatment period; they also found that Gait Trainer therapy required less therapeutic assistance than treadmill training [17]. Mayr et al. compared Lokomat with conventional gait rehabilitation, and they found significant improvement in function during a 6-week period of Lokomat training, indicating that functional recovery depends on intensive and longer training periods [18]. A systematic review showed that electromechanically assisted training was effective at improving gait ability after stroke [19]; however, the review also noted some specific questions to be addressed by further research, including the optimal frequency and duration of electromechanically assisted gait training, the initiation timing after stroke, and the high cost of the machines [20]. Other studies showed that conventional gait rehabilitation has additional benefits compared to electromechanically assisted training [21,22]. |
| We have developed a footpad-type, small-sized and low-priced locomotion interface named the Gait Master- which has footpads with two degrees of freedom for each lower limb- as a training system to enable patients to swing their lower limbs efficiently [23]. Gait movement on a Gait Master is a passive movement in which the footpads move the patient’s feet back and forth and up and down independently of the patient’s will. The movements of the Gait Master footpads are realized with chain-drive mechanisms in Gait Master2 [24], ball-screw mechanisms in GaitMaster3 [25], and slider-crank mechanisms in GaitMaster4 (Figure 1) [26]. |
| GaitMaster4 is 1.59 m long and 1.16 m wide, weighs 80 kg, and is going to be commercialized below $60,000 dollars (USD). The Gait Master consists of two slider cranks for moving the footpads back and forth, two ball-screw actuators for moving the footpads up and down, and a computer for controlling their movements. No body weight support devices are needed. The trajectories of the Gait Master footpads are based on a healthy individual’s gait trajectory, which is prerecorded with a motion capture device. The trajectory can be scaled to any size and cycle in accord with the patient’s physical size and condition. As a result, patients can do repetitive exercise and hip extension exercise. Since the Gait Master is controlled by computer, the gait trajectories and gait speed can be easily changed. Moreover, because the Gait Master moves the lower limbs, a physical therapist can support the trunk of the patient easily. |
| We previously reported a feasibility study in which we found that gait ability in chronic patients was improved after twelve 20-min Gait Master sessions [27]. Here, we show improvement pattern of muscle strength and gait ability using the Gait Master4. |
| Methods |
| Subjects |
| As we could not obtain the data of muscle strengths in two subjects among the patients reported previously [27], the present populations were 10 chronic-stroke hemiparetic patients (9 men and 1 woman) with a mean age of 59.9 ± 8.7 years and a mean post-stroke interval of 65.5 ± 51.8 months. Nine patients were right hemiparetic and 1 was left hemiparetic; the causes of stroke were ischemia (4 cases) and hemorrhage (6 cases). The inclusion criteria were (1) first-time stroke, (2) more than 6 months’ passage since stroke onset, (3) slight to moderate motor deficit (Brunnstrom recovery stages III–VI), and (4) ambulatory ability with or without any walking aids. The exclusion criteria were (1) a higher-brain function disorder or cognitive deficit affecting the ability to understand and describe symptoms (<24 on the Mini-Mental State Examination), (2) severe heart disorder affecting gait movement intensity, and (3) severe bone or joint disease affecting gait movement. |
| This study was approved by the Tsukuba Memorial Hospital Ethics Committee, and all subjects or their legal representatives gave their written informed consent to participate in the study. |
| Study protocol |
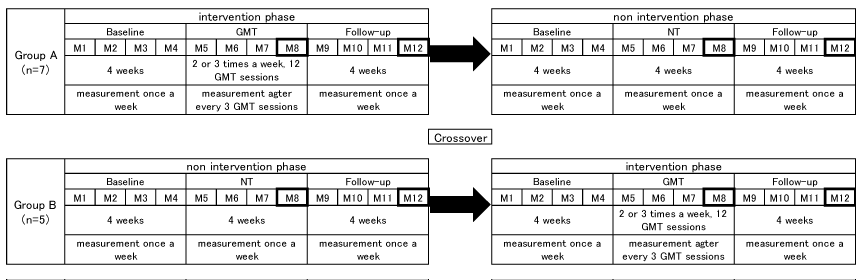
| The subjects were divided randomly by a computer into two groups. The group A subjects followed an ‘intervention phase’ and then a ‘non-intervention phase,’ whereas group B subjects followed the ‘non-intervention phase’ first and then the ‘intervention phase.’ There was no break between the phases. The intervention phase consisted of the baseline, Gait Master training (GMT), and a follow-up, and the non-intervention phase consisted of the baseline, non-training (NT), and a follow-up. In the intervention phase, after a 4-week baseline period, the subject performed gait training using the Gait, Master4 two or three times a week, for a total of 12 GMT sessions, followed by 4 weeks of follow-up. In the non-intervention phase, the subject performed the baseline, NT, and follow-up, with each of these segments lasting 4 weeks (Figure 2). |
| Therapy on the gait master |
| The Gait Master4 was developed by the Department of Intelligent Interaction Technologies, Graduate School of Systems and Information Engineering, University of Tsukuba. The details of this device are described elsewhere [25]. In the present study, the conditions of gait training using the Gait Master4 were as follows: (a) gait training time was 20 min once a day, (b) the gait speed was set as fast as possible, with the target being double the subject’s comfortable gait speed, (c) the subject could use gait orthosis, and (d) the subject was able to grip the Gait Master4 handrail. The gait speed, stride, and foot clearance were controlled in accord with the subject’s condition. |
| During the gait training, the subject’s body movement and lower limb movement were supported by a physical therapist as needed. All subjects were monitored continually with electrocardiography and a sphygmomanometer. During the study period, the subjects continued the same rehabilitation or exercise regimens they were doing before the study began. |
| Assessment |
| The main outcome measures were the isometric muscle strengths of hip flexion and extension and the maximum gait speed. In the intervention phase, we measured each of this parameter once a week at both baseline and follow-up, and after every three GMT sessions. In the non-intervention phase, we measured the same parameters once a week during baseline, non-training, and follow-up. |
| For the assessment of gait speed, the subject walked 10 m on the ground at maximum speed. We measured the gait speed of three attempts by the subject and used the best time as the final measurement. The subjects could use their same walking aids (if any) throughout all measurements. A therapist supported the subjects as necessary. |
| For the assessment of muscle strength, we used a hand-held dynamometer (μtas-MF01, Anima Corp., Tokyo) and measured the isometric contraction muscle strength of hip flexion and extension as lower-limb muscle strength. We measured the hip flexion with the subject in the sitting position and the hip extension in the supine position. We measured the maximum isometric contraction muscle strength for 10-sec periods. We locked a pressure sensor to a belt that each subject wore around the limb to record the maximum power. We used the higher of two strength readings. |
| Statistical analysis |
| For muscle strength, and gait speed, we calculated the change from the mean baseline value. We assumed measurement number 8 in figure 2 (M8) as a representative measurement for ‘after GMT’ or ‘after NT,’ and we used measurement number 12 in figure 2 (M12) as a representative of the follow-up. The Friedman test was used to compare the values within the intervention phase and the nonintervention phase, respectively. The Mann-Whitney U-test was used to compare the measurements at M8 and M12 between the intervention phase and the non-intervention phase and to compare the characteristics between groups A and B. Correlations of muscle strength and gait speed after GMT were calculated using Pearson’s correlation coefficient. All statistical analyses were performed using SPSS (Version 20.0). Significance was set at p<0.05. |
| Results |
| No significant differences were observed in the clinical data, initial muscle strength, and initial gait speed at the study onset between groups A and B (Table 1). |
| On the Gait Master4, three of the subjects required the help of a physical therapist to control the trunk and knee at study onset, and the other seven subjects did not require this help. |
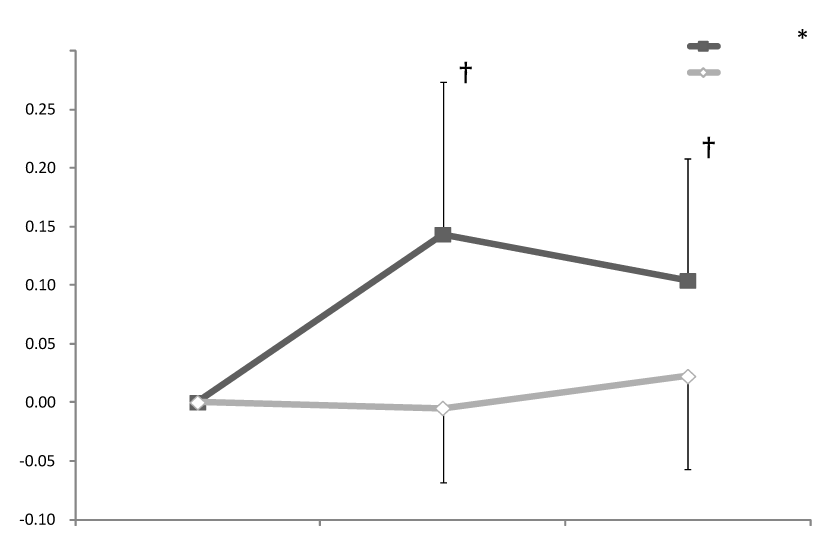
| Figure 3 shows the changes in maximum gait speed. During the intervention phase, there was a significant increase in gait speed (Friedman test, p=0.006), whereas during the non-intervention phase, there was no significant increase in gait speed (Friedman test, p=0.905). We found a significant difference in the change in maximum gait speed at both M8 and M12 between the intervention and non-intervention phases (M8: p=0.002; M12: p=0.035). |
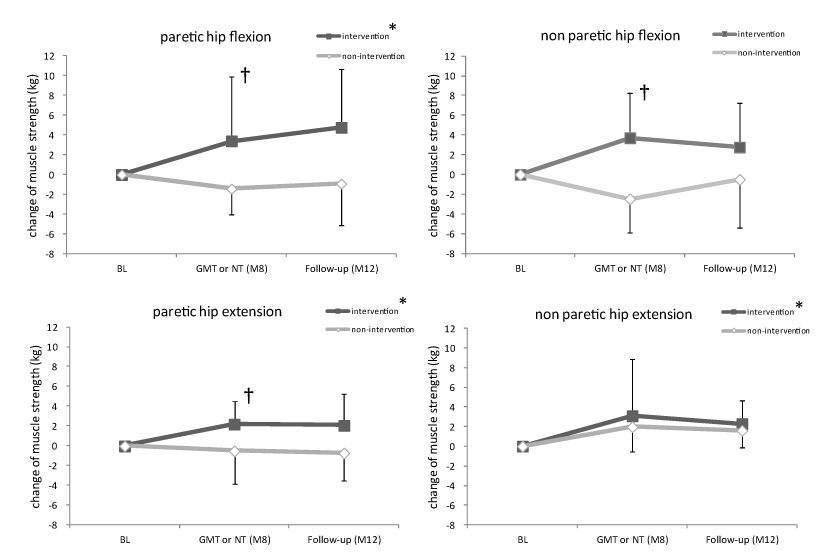
| Figure 4 shows the changes in lower limb muscle strength. During the intervention phase, there were significant changes in paretic hip flexion strength (Friedman test, p=0.045), paretic hip extension (Friedman test, p=0.014) and non-paretic hip extension (Friedman test, p=0.025), but no significant change in the strength of non-paretic hip flexion (Friedman test, p=0.202). During the nonintervention phase, there were no significant changes in the strength of paretic hip flexion (Friedman test, p=0.548), paretic hip extension (Friedman test, p=0.905), non-paretic hip flexion (Friedman test, p=0.150) or non-paretic hip extension (Friedman test, p=0.067). Between the intervention and non-intervention phases, we found significant differences in the change in strength in paretic hip flexion (M8: p=0.035), non-paretic hip flexion (M8: p=0.004), and paretic hip extension (M8: p=0.035). |
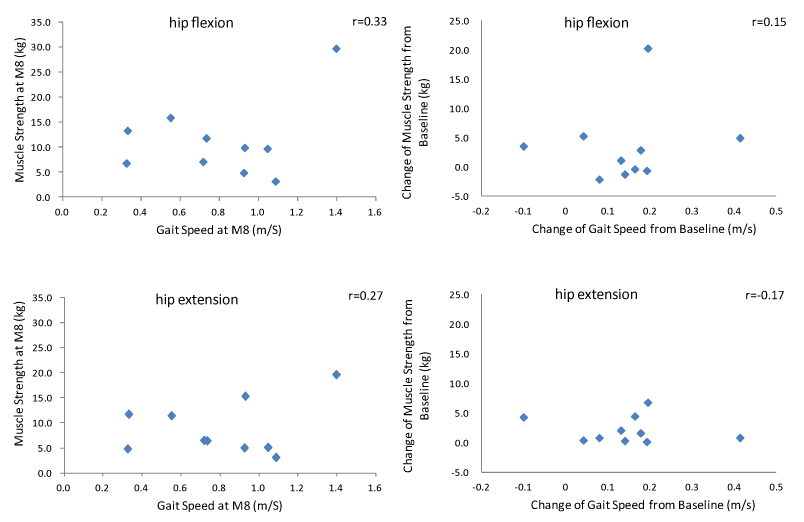
| Figure 5 shows the correlations between muscle strengths and gait speed and between the changes of muscle strength and the change of gait speed; no significant correlations were revealed. |
| Discussion |
| In the present study, improvements in lower-limb muscle strength and gait speed were observed when the Gait Master- a footpad-type, small-sized and inexpensive locomotion interface !—! was used for the gait training of chronic stroke patients. The results suggest that the Gait Master is effective for improving both muscle strength in the paretic limbs and gait ability. |
| Previous studies reported that improvement of gait ability is correlated with improvement of muscle strength of the hip flexion and extension in paretic limbs [28,29]. In the present study, significant improvements of gait speed and muscle strength of hip flexion and extension were observed after GMT, but improvement of gait speed and muscle strength were not significantly correlated. In gait training using gait devices, hip extension seems to be important for the activation of central pattern generator to improve gait ability [30]. Additionally, recent studies reported that improvement of gait ability depended on the high-profile plasticity of the brain caused by repetitive movement, constrained movement, and pelvic assist during gait movement [30-33]. Therefore, the improvement of gait ability by the Gait Master training might be due to reorganization of the neural network and/or to the improvement of muscle strengths. In light of the present results and the findings described above, we propose that the Gait Master may be useful for chronic stroke patients, because uniform repetitive gait movement, constrained gait movement, pelvic rotation, and hip extension and flexion are characteristic gait-like movements achieved with the Gait Master. |
| It is notable that the present subjects’ muscle strengths were significantly improved after BMC Nursing of only 12 training sessions, since according to National Strength and Conditioning Association (NSCA) Guidelines, strength training should be implemented for 9 to 20 weeks to produce optimal strength gains. We also found that gait speeds were improved after 12 sessions of Gait Master intervention, whereas previous studies using other gait devices required 6 to 8 weeks for improvement [6,7,9,10,17,18]. Our results suggest that Gait Master4 might be faster at rehabilitating gait in post-stroke patients compared to other devices. |
| In conventional gait rehabilitation for stroke patients, a physical therapist can assist only one stroke patient at a time, and he or she may have difficulty helping a patient move the lower limbs and trunk at the same time, or difficulty assisting with long rehabilitation sessions. Similarly, the simultaneous efforts of two or three physical therapists are appropriate for the safe gait rehabilitation of a single patient using body weight-support treadmill training. In the present study, in contrast, the Gait Master made gait rehabilitation achievable with little or no assistance from a physical therapist. Since the gait-like movement produced with the Gait Master is controlled by a computer, the physical therapist is free to help the patient move his or her trunk and lower limbs, thus enabling long rehabilitation sessions. |
| These findings indicate that gait rehabilitation using the Gait Master can not only provide a more effective gait rehabilitation environment for stroke patients but can also reduce the burden on physical therapists. Because the present subjects’ gait rehabilitation using the Gait Master showed quick improvements, we propose that the Gait Master can provide a new approach for a short-time intensive model for chronic stroke patients. |
| In conclusion, gait rehabilitation using the Gait Master improved gait ability and the strength of both hip extension and flexion in chronic stroke patients. Using the Gait Master, patients can perform gait exercises with little support from a physical therapist. In addition, the Gait Master requires fewer physical therapists than body weightsupport treadmill training. We therefore feel that gait rehabilitation using the Gait Master is effective training for chronic stroke patients. Its main advantages are its characteristic gait-like movement, the reduced effort on the part of physical therapists, its small size and its reasonable cost compared with other electromechanically assisted devices (e.g., the Lokomat is 4,000 dollars). Further studies are warranted to compare gait rehabilitation using the Gait Master with conventional gait rehabilitation and with body weight-support treadmill training and other electromechanically assisted devices. |
| Acknowledgements |
| We thank the volunteers and the hemiparetic patients for their participation in this study, and Dr. Susumu Koseki and the rehabilitation staff of Tsukuba Memorial Hospital for the data collection. |
| The authors have declared no conflicts of interest. |
References
- Hiroaki F, Taizo S (2007) Physical therapy approaches for the central nervous system: from the task-oriented approach to the motor relearning program (in Japanese). Rigakuryoho Kagaku 22: 319-324.
- Finch L, Barbeau H, Arsenault B (1991) Influence of body weight support on normal human gait: development of a gait retraining strategy. Phys Ther 71: 842-855.
- Grillner S (1985) Neurobiological bases of rhythmic motor acts in vertebrates. Science 228: 143-149.
- Shik ML, Severin FV, Orlovski�?�?�? GN (1966) [Control of walking and running by means of electric stimulation of the midbrain]. Biofizika 11: 659-666.
- Hesse S, Bertelt C, Schaffrin A, Malezic M, Mauritz K (1994) Restoration of gait in nonambulatory hemiparetic patients by treadmill training with partial body-weight support. Arch Phys Med Rehabil 75: 1087-1093.
- Hesse S, Bertelt C, Jahnke MT, Schaffrin A, Baake P, et al. (1995) Treadmill training with partial body weight support compared with physiotherapy in nonambulatory hemiparetic patients. Stroke 26: 976-981.
- Visintin M, Barbeau H, Korner-Bitensky N, Mayo NE (1998) A new approach to retrain gait in stroke patients through body weight support and treadmill stimulation. Stroke 29: 1122-1128.
- Sullivan KJ, Knowlton BJ, Dobkin BH (2002) Step training with body weight support: effect of treadmill speed and practice paradigms on poststroke locomotor recovery. Arch Phys Med Rehabil 83: 683-691.
- Eich HJ, Mach H, Werner C, Hesse S (2004) Aerobic treadmill plus Bobath walking training improves walking in subacute stroke: a randomized controlled trial. Clin Rehabil 18: 640-651.
- Yagura H, Hatakenaka M, Miyai I (2006) Does therapeutic facilitation add to locomotor outcome of body weight--supported treadmill training in nonambulatory patients with stroke? A randomized controlled trial. Arch Phys Med Rehabil 87: 529-535.
- Dobkin BH, Harkema S, Requejo P, Edgerton VR (1995) Modulation of locomotor-like EMG activity in subjects with complete and incomplete spinal cord injury. J Neurol Rehabil 9: 183-190.
- Harkema SJ, Hurley SL, Patel UK, Requejo PS, Dobkin BH, et al. (1997) Human lumbosacral spinal cord interprets loading during stepping. J Neurophysiol 77: 797-811.
- Colombo G, Wirz M, Dietz V (2001) Driven gait orthosis for improvement of locomotor training in paraplegic patients. Spinal Cord 39: 252-255.
- Husemann B, M�?¼ller F, Krewer C, Heller S, Koenig E (2007) Effects of locomotion training with assistance of a robot-driven gait orthosis in hemiparetic patients after stroke: a randomized controlled pilot study. Stroke 38: 349-354.
- Hesse S, Uhlenbrock D, Sarkodie-Gyan T (1999) Gait pattern of severely disabled hemiparetic subjects on a new controlled gait trainer as compared to assisted treadmill walking with partial body weight support. Clin Rehabil 13: 401-410.
- Hesse S, Uhlenbrock D, Werner C, Bardeleben A (2000) A mechanized gait trainer for restoring gait in nonambulatory subjects. Arch Phys Med Rehabil 81: 1158-1161.
- Werner C, Von Frankenberg S, Treig T, Konrad M, Hesse S (2002) Treadmill training with partial body weight support and an electromechanical gait trainer for restoration of gait in subacute stroke patients: a randomized crossover study. Stroke 33: 2895-2901.
- Mayr A, Kofler M, Quirbach E, Matzak H, Fr�?¶hlich K, et al. (2007) Prospective, blinded, randomized crossover study of gait rehabilitation in stroke patients using the Lokomat gait orthosis. Neurorehabil Neural Repair 21: 307-314.
- Ada L, Dean CM, Vargas J, Ennis S (2010) Mechanically assisted walking with body weight support results in more independent walking than assisted overground walking in non-ambulatory patients early after stroke: a systematic review. J Physiother 56: 153-161.
- Mehrholz J, Werner C, Kugler J, Pohl M (2007) Electromechanical-assisted training for walking after stroke. Cochrane Database Syst Rev : CD006185.
- Hidler J, Nichols D, Pelliccio M, Brady K, Campbell DD, et al. (2009) Multicenter randomized clinical trial evaluating the effectiveness of the Lokomat in subacute stroke. Neurorehabil Neural Repair 23: 5-13.
- Hornby TG, Campbell DD, Kahn JH, Demott T, Moore JL, et al. (2008) Enhanced gait-related improvements after therapist- versus robotic-assisted locomotor training in subjects with chronic stroke: a randomized controlled study. Stroke 39: 1786-1792.
- Iwata H, Yano H, Nakaizumi F (2001) GaitMaster: a versatile locomotion interface foruneven virtual terrain. Proc of IEEE Virtual Reality Conference, Yokohama, Japan 131-137.
- Yano H, Kasai K, Saitoh H, Iwata H (2003) Development of a gait rehabilitation system using a locomotion interface. Journal of Visualization and Computer Animation 14: 243-252.
- Yano H, Oonuki K, Tai G, Iwata H (2005) Evaluation of shared walking environment with locomotion interfaces. Proceedings of CollabTech 85-90.
- Yano H, Masuda T, Nakajima Y, Tanaka N, Tamefusa S, et al. (2008) Development of a gait rehabilitation system with a spherical immersive projectiondisplay. Journal of Robotics and Mechatronics 12: 836-845.
- Tanaka N, Saitou H, Takao T, Iizuka N, Okuno J, et al. (2012) Effects of gait rehabilitation with a footpad-type locomotion interface in patients with chronic post-stroke hemiparesis: a pilot study. Clin Rehabil 26: 686-695.
- Bohannon RW (1989) Selected determinants of ambulatory capacity in patients with hemiplegia. Clin Rehabil 3: 47-53.
- Teixeira-Salmela LF, Nadeau S, Mcbride I, Olney SJ (2001) Effects of muscle strengthening and physical conditioning training on temporal, kinematic and kinetic variables during gait in chronic stroke survivors. J Rehabil Med 33: 53-60.
- Thompson RF, Berger TW, Madden J 4th (1983) Cellular processes of learning and memory in the mammalian CNS. Annu Rev Neurosci 6: 447-491.
- Nudo RJ, Wise BM, SiFuentes F, Milliken GW (1996) Neural substrates for the effects of rehabilitative training on motor recovery after ischemic infarct. Science 272: 1791-1794.
- Miyai I, Yagura H, Hatakenaka M, Oda I, Konishi I, et al. (2003) Longitudinal optical imaging study for locomotor recovery after stroke. Stroke 34: 2866-2870.
- Miyai I, Suzuki M, Hatakenaka M, Kubota K (2006) Effect of body weight support on cortical activation during gait in patients with stroke. Exp Brain Res 169: 85-91.
Tables and Figures at a glance
| Table 1 |
Figures at a glance
 |
 |
 |
 |
 |
| Figure 1 | Figure 2 | Figure 3 | Figure 4 | Figure 5 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 7086
- [From(publication date):
specialissue-2012 - Jul 16, 2025] - Breakdown by view type
- HTML page views : 2482
- PDF downloads : 4604
