Research Article Open Access
Influences of Barriers to Cessation and Reasons for Quitting on Substance Use among Treatment-Seeking Smokers Who Report Heavy Drinking
Dawn W Foster1*, Norman B Schmidt2 and Michael J Zvolensky3,4
1Yale School of Medicine, Department of Psychiatry, New Haven, CT, USA
2Florida State University, Department of Psychology, New Haven, CT, USA
3The University of Texas MD Anderson Cancer Center, Department of Behavioral Science, New Haven, CT, USA
4University of Houston, Department of Psychology, New Haven, CT, USA
- Corresponding Author:
- Dawn W Foster
Psychiatry Department at Yale Schol of Medicine
Yale University, New Haven, CT 06519, USA
Tel: 203 974 7892
E-mail: dawn.foster@yale.edu
Received: September 11, 2015; Accepted: October 09, 2015; Published: October 15, 2015
Citation: Foster DW, Schmidt NB, Zvolensky MJ (2015) Influences of Barriers to Cessation and Reasons for Quitting on Substance Use among Treatment-Seeking Smokers Who Report Heavy Drinking. J Addict Res Ther 6:246. doi:10.4172/2155- 6105.1000246
Copyright: © 2015 Foster DW, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Related article at Pubmed, Scholar Google
Visit for more related articles at Journal of Addiction Research & Therapy
Abstract
Objective: We examined behavioral and cognitively-based quit processes among concurrent alcohol and tobacco users and assessed whether smoking and drinking were differentially influenced.
Method: Participants were 200 treatment-seeking smokers (37.50% female; Mage=30.72; SD=12.68) who reported smoking an average of 10 or more cigarettes daily for at least one year.
Results: Barriers to cessation (BCS) and reasons for quitting (RFQ) were generally correlated with substance use. BCS moderated the relationship between quit methods and cigarette use such that quit methods were negatively associated with smoking, particularly among those with more BCS. RFQ moderated the association between quit methods and cigarette use such that quit methods were negatively linked with smoking among those with fewer RFQ, but positively linked with smoking among those with more RFQ. Two 3-way interactions emerged. The first 3-way indicated that among individuals with fewer RFQ, quit methods was negatively associated with smoking, and this was strongest among those with more BCS. However, among those with more RFQ, smoking and quit methods were positively associated, particularly among those with more BCS. The second 3-way showed that among those with fewer RFQ, quit methods was negatively linked with drinking frequency, and this was strongest among those with more BCS. However, among those with fewer BCS, drinking and quit methods were positively linked.
Conclusion: The relationship between behavioral and cognitively-based quit processes and substance use is not straightforward. There may be concurrent substance-using individuals for whom these processes might be associated with increased substance use.
Keywords
Barriers to cessation; Reasons for quitting; Cigarette; Drinking; Concurrent
Introduction
Influences of barriers to cessation and reasons for quitting on substance use among treatment-seeking smokers who report heavy drinking. Strong associations between tobacco and alcohol use have been documented [1]. Roughly 85% of smokers drink alcohol, and drinkers are 75% more likely to smoke relative to those who abstain from alcohol [2-5]. Smokers with alcohol problems (relative to smokers without alcohol problems) tend to also report lower tobacco quit rates, be more dependent on nicotine [6], and die at higher rates from diseases linked with smoking as opposed to alcohol causes [7]. Concurrent use has reciprocal effects such that use of one substance predicts use of the other [8], and concurrent use also has multiplicative effects greater than the independent risk of either substance [9,10].
Multiple perspectives have emerged with respect to treatment for co-use. One perspective suggests that coping with withdrawal symptoms following treatment for concurrent alcohol and tobacco use may be a barrier to successful cessation [11]. Another perspective suggests one drug may become a conditioned stimulus for the other; and thus, concurrent treatment may improve abstinence rates relative to treating each substance separately. Research has explored efficacy of concurrent treatment [12], and findings largely support targeting cooccurring substance use [11,13,14]. However, further work is needed to understand effects of behaviorally- and cognitively-based quit processes on concurrent substance use. Examination of quit processes among smokers who drink heavily is important in elucidating the extent to which changes in behavioral (the use of quit methods) and cognitive (e.g., quit barriers, reasons for quitting) variables are linked with use, and whether these processes uniquely or differentially influence substance use outcomes.
Methods for quitting
Most current smokers desire to quit [15], and many utilize multiple quit methods. It is likely that the use of multiple quit methods is linked with quit success as the individual “weeds out” ineffective methods either by self-selection or with help from a health professional. Quit success for concurrent substances is predicted in part by motivation to quit one substance [16], and thus, we expect number of quit methods (an indirect indication that an individual is motivated or desires to quit) to be associated with reductions in tobacco and alcohol use.
Barriers to cessation
Barriers to smoking cessation (referred to henceforth as BCS) are broadly described as beliefs about inconveniences, costs, or cons regarding quitting smoking. In other words, BCS are stressors that reflect cognitive appraisal of negative aspects of quitting [17]. Commonly endorsed barriers include missing or craving cigarettes, feeling nervous or irritable following cessation, and losing a source of pleasure [18]. Other barriers include fear of weight gain, difficulty managing negative emotions, and low self-efficacy related to quitting [19]. As BCS has predictive validity with respect to smoking outcomes among concurrent alcohol and tobacco users [20], we expected that BCS would be associated with increased cigarette use. Previous work in co-using samples have not shown significant links between BCS and alcohol [20,21], and thus we did not expect alcohol outcomes to be significantly predicted by BCS. No published research to our knowledge has evaluated the interaction between quit methods and BCS in predicting substance use among cousers, and thus we examined this important relationship. Based on the predicted links between barriers and use, and between quit methods and use, we expected that BCS would moderate the relationship between quit methods and use such that quit methods would be negatively linked with substance use, and that this negative relationship would be stronger among those with fewer BCS relative to more BCS.
Reasons for quitting
Having reasons for quitting (RFQ) substance use is an indication of desire to quit. This desire has been described as a dynamic, multidimensional construct comprised of facets including strength of motivation [22], considerations of pros and cons of quitting [23], and readiness to change [24]. RFQ has been operationalized as consisting of four dimensions: health concerns, self-control, social pressure, and immediate reinforcement. The former two correspond to intrinsic motivation and the latter to extrinsic motivation [25]. RFQ has demonstrated predictive validity with respect to quit success [26,27]. Thus, we expected to replicate previous findings with respect to the association between RFQ and reduced smoking. Examinations of RFQ with respect to concurrent substance use are scarce, and as such, relatively little is known about the influence of RFQ and other behavioral (e.g., Quit methods) and psychological (e.g., BCS) phenomena on cessation in co-using populations. We sought to address this gap in empirical knowledge by evaluating links among RFQ, BCS, and quit methods. We expected that in addition to buffering against smoking, RFQ would also predict reductions in drinking outcomes. As noted above, quit methods were expected to negatively associate with substance use, and we further expected that RFQ would moderate this relationship such that the negative association would be stronger among those with more RFQ. Finally, we explored whether RFQ influenced relationships among BCS, quit methods, and substance use. As stated previously, we predicted that BCS would moderate the link between quit methods and use. Further, as RFQ is associated with quit success [26], we expected that RFQ would significantly interact with BCS and quit methods. In other words, we expected a significant three-way interaction to emerge with respect to substance use (RQF X Quit Methods X BCS).
Current study
This study was designed to examine relationships among behavioral and cognitively-based quit processes in a sample of daily smokers who drink heavily. We had three main hypotheses. Our first hypothesis was related to main effects. Specifically, we expected that: H1a) quit methods would be associated with reduced substance use; H1b) BCS would be linked with increased cigarette use; and H1c) RFQ would be linked with reduced substance use. Our second hypothesis was related to moderating relationships. We expected that: H2a) RFQ would moderate the relationship between quit methods and substance use such that quit methods would be negatively linked with use, particularly among those with more RFQ; and H2b) BCS would moderate the relationship between quit methods and use such that quit methods would be negatively linked with use, particularly among those with less BCS. Our third hypothesis (H3) predicted that quit methods, RFQ, and BCS would interact to predict substance use.
Method
Participants
The present sample consisted of 200 treatment-seeking daily smokers (37.50% female; Mage=30.72; SD=12.68). The racial and ethnic distribution of this sample was as follows: 89.50% identified as White/ Caucasian; 3.50% identified as Black/Non-Hispanic; 1.00% identified as Black/Hispanic; 2.50% identified as Hispanic; 0.50% identified as Asian; and 3.00% identified as ‘Other.’ 20.5% of participants completed high school as their highest form of education, 49.50% completed some college, 11.00% obtained a 4-year college degree, 6.00% obtained a 2-year college degree, 6.00% obtained a graduate degree, 5.00% completed some graduate school, and 2.00% completed less than a high school degree. Of the sample, 48.24% met criteria for at least one current (past month) Axis I diagnosis including social anxiety disorder (9.05%), generalized anxiety disorder (5.03%), and alcohol abuse (5.03%).
Inclusion criteria for the larger longitudinal intervention included: (1) 18 years or older; (2) reporting smoking an average of 10 or more cigarettes per day for at least one year; and, (3) providing a Carbon Monoxide breath sample of 10 ppm or higher during the baseline session. Participants were excluded based on the following criteria: (1) current homicidality or suicidality; (2) endorsement of past or current psychotic-spectrum symptoms via structured interview screening; and (3) limited mental competency and inability to provide informed, voluntary, written consent. Additionally, all participants in the present sample met heavy drinking criteria (scoring 8 or higher on the Alcohol Use Disorders Identification Test) [28].
Measures
Demographics: Participants provided demographic information including gender, age, racial background, ethnicity, highest education level, and marital status.
The Quantity/frequency scale structured clinical interview for DSM-IV axis I disorders (SCID-I): The SCID-I-NP (Non-Patient Version) was utilized for diagnostic assessments to assess DSM-IVTR diagnoses for past and current Axis I Disorders [29]. All SCID-I interviews were administered by trained personnel including research assistants or doctoral level staff, and supervised by independent doctoral-level professionals. Interviews were audio-taped. The reliability of a random selection of 12.5% of interviews was reviewed (MJZ) for accuracy; no cases of diagnostic coding disagreement were noted.
Smoking history questionnaire: Smoking rate, years of being a daily smoker, age of onset of initiation, and other characteristics were assessed using the Smoking History Questionnaire (SHQ) [30]. Items included, for example, “Since you started regular daily smoking, what is the average number of cigarettes you smoked per day?” which assessed smoking rate. Additionally, individuals indicated their quit methods by endorsing items (0=No or 1=Yes) including “Cold turkey,” “Behavior modification,” “Nicotine patch,” “Gradual reduction,” and “Telephone counseling.”
Fagerström test for nicotine dependence: The Fagerström Test for Nicotine Dependence (FTND) is a six-item scale that assesses gradations in tobacco dependence [31] and exhibits positive relations with key smoking variables, adequate internal consistency, and high test-retest reliability [31,32]. FTND scores range from 0 to 10, and higher scores indicating greater dependence on nicotine [33]. (Cronbach’s α=0.35).
Alcohol history questionnaire: Alcohol use in terms of quantity and frequency was assessed using the 42-item Alcohol History Questionnaire (AHQ) [34]. Example items include, “How many years have you been drinking regularly?” and “How old were you when you first had an alcoholic drink?”
Alcohol use: Alcohol use was also assessed using the Alcohol Use Disorders Identification Test (AUDIT), which is a 10-item measure that screens for hazardous or harmful drinking [28]. Items assess heavy drinking, quantity and frequency of use, dependence, tolerance, and problems. The AUDIT’s internal consistency alpha was .69 in the present sample, and in past work it has reliably distinguished between hazardous, harmful, and no drinking histories [28,35]. An AUDIT score of 8 produces 85% sensitivity and 89% specificity for harmful or hazardous drinking [36].
Barriers to cessation scale: The Barriers to Cessation Scale (BCS) is a 19-item measure that assesses barriers, or specific stressors, associated with smoking cessation [37]. Participants respond on a four-point Likert-type scale ranging from (0=“not a barrier” to 3=“large barrier”), and indicate the extent to which they identify with each of the identified BCS. The BCS total score has shown good internal consistency [37], and has also shown good internal consistency with respect to the three subscales (Addictive Barriers, External Barriers, and Internal Barriers) [37]. Further, the BCS has evinced good content and predictive validity [37]. Consistent with previous work [17], the total score summary statistic was utilized in the present study. This scale demonstrated high levels of internal consistency in the current sample (Cronbach’s alpha=0.89).
Reasons for quitting scale: The Reasons for Quitting (RFQ) scale is a 20-item measure that assesses motivation for quitting smoking [38]. Respondents indicate the extent to which each reason for quitting applies to them on a 4-point Likert-type scale ranging from (1=Not at all true to 4=Extremely true). The RFQ consists of four dimensions: health concerns (e.g., “I’m concerned about illness”; α=0.79), selfcontrol (e.g., “I’ll prove I can accomplish other things”; α=0.85), social pressure (e.g., “I want people to stop nagging me” α=0.70), and immediate reinforcement (e.g., “I won’t smell”; α=0.69). The former two subscales correspond to intrinsic motivation and the latter two to extrinsic [25]. The RFQ total score took into account all four subscales and was created by summing responses to items. The Cronbach’s alpha for the total RFQ scale was .82. The RFQ has shown good psychometric properties and this has been evident across diverse samples [27,39].
Cannabis use: The Marijuana Smoking History Questionnaire (MSHQ) is comprised of 40-items and assesses history and patterns of cannabis use [40]. Example items include “How many years have you smoked marijuana?” and “Think about your smoking during the last week, how much marijuana did you smoke per occasion in an average day?” Participants rated the latter item on an eight-point Likert scale. Scores correspond to pictures depicting increasing sizes of marijuana joints, with 1 indicating the smallest marijuana joint and 8 indicating the largest marijuana joint. Previous research has used the MSHQ as a successful indicator of cannabis use [41]. In the present study, cannabis use was included in analyses as a covariate given the frequent cooccurrence of cannabis with tobacco use [42,43] and alcohol [44].
Procedure
Participants were adult daily smokers who drink heavily and were recruited from the community via radio announcements, flyers, and newspaper ads to participate in a large dual-site randomized controlled clinical trial evaluating the efficacy of two interventions for smoking cessation. Individuals responding to study-related advertisements were scheduled for an in-person baseline session to evaluate eligibility for study inclusion. Participants provided written informed consent during the baseline assessment and were interviewed using the SCID-I/ NP. Participants also completed a computerized battery of self-report questionnaires. All study procedures and treatment of human subjects were conducted in compliance with ethical standards of the American Psychological Association and the study protocol was approved by the Institutional Review Board at each study site. The present study is based on analyses of baseline (pre-treatment) data for a sub-set of the sample, which was on the basis of available data on all studied variables.
Analysis Plan
Zero-order correlations were obtained to examine relationships between predictor and criterion variables. The incremental validity of covariates (gender, race, education status, marital status, and cannabis use) and independent variables (IV; RFQ, quit methods, and BCS) were examined in relation to the dependent variables (DV; cigarettes smoked per day and drinking frequency) using hiearchical multiple regression [44]. Separate models were constructed for each DV. At Level 1, RFQ, quit methods, and BCS were included in the model, along with gender, race, education status, marital status, and cannabis use included as covariates to ensure any observed effects were not due to these factors. At Level 2, covariates and RFQ, quit methods, and BCS were simulatenously entered to test two-way interactions or product terms. At Level 3, covariates, RFQ, quit methods, and BCS were entered into the model to test three-way interactions (Table 1). Emerging two- and three-way interactions were graphed using parameter estimates from the regression equation where high and low values were specified as one standard deviation above and below their respective means [45].
| Predictor | B | SE | t | p | β | Adj R2 | ||
|---|---|---|---|---|---|---|---|---|
| Number of Cigarettes Smoked Per Day | Step 1 | Gender | -0.01 | 0.16 | -0.08 | 0.94 | -0.01 | 0.12 |
| Race | 0.05 | 0.07 | 0.63 | 0.53 | 0.04 | |||
| Education Status | 0.15 | 0.05 | 2.71 | 0.01 | 0.20* | |||
| Marital Status | -0.08 | 0.05 | -1.67 | 0.1 | -0.13 | |||
| Cannabis use | 0.07 | 0.03 | 2.56 | 0.01 | 0.19* | |||
| Reasons for Quitting (RQF) | -0.01 | 0.01 | -1.71 | 0.09 | -0.13† | |||
| Quit Methods (QM) | -0.001 | 0.04 | -0.01 | 0.99 | -0.001 | |||
| Barriers to Cessation (BCS) | 0.001 | 0.01 | 0.09 | 0.93 | 0.01 | |||
| Step 2 | RQF * QM | 0.09 | 0.04 | 2.15 | 0.03 | 1.10* | 0.17 | |
| RQF * BCS | 0 | 0.01 | -0.22 | 0.83 | -0.1 | |||
| QM * BCS | 0.09 | 0.03 | 2.71 | 0.01 | 0.65* | |||
| Step 3 | RQF * QM * BCS | 0.01 | 0 | 3.77 | 0.0002 | 4.52*** | 0.23 | |
| Frequency of Alcohol Use | ||||||||
| Step 1 | Gender | 3.37 | 1.35 | 2.51 | 0.01 | 0.18* | 0.05 | |
| Race | -0.21 | 0.62 | -0.34 | 0.73 | -0.02 | |||
| Education Status | -0.58 | 0.47 | -1.23 | 0.22 | -0.09 | |||
| Marital Status | -0.65 | 0.41 | -1.59 | 0.11 | -0.12 | |||
| Cannabis use | -0.29 | 0.22 | -1.32 | 0.19 | -0.1 | |||
| RQF | 0.17 | 0.07 | 2.44 | 0.02 | 0.17* | |||
| QM | 0.48 | 0.36 | 1.31 | 0.19 | 0.1 | |||
| BCS | 0.15 | 0.06 | 2.35 | 0.02 | 0.17* | |||
| Step 2 | RQF * QM | -0.002 | 0.01 | -0.3 | 0.76 | -0.17 | 0.05 | |
| RQF * BCS | 0.001 | 0.001 | 1.49 | 0.14 | 0.72 | |||
| QM * BCS | -0.003 | 0.004 | -0.88 | 0.38 | -0.23 | |||
| Step 3 | RQF * QM * BCS | 0.001 | 0.0003 | 2.6 | 0.01 | 3.40* | 0.08 |
Note: N=200 *** p<0.001 ** p<0.01 * p<0.05.
Table 1: Hierarchical regression analysis for variables predicting cigarette and alcohol use from the reasons for quitting, number of quit methods, and barriers to cessation.
Results
Descriptive data and correlations among variables
Means, standard deviations, and bivariate correlations for all of the study variables are presented in Table 2. For illustrative purposes, we have provided a table of means at low and high levels of reasons for quitting based on a mean split (Table 3).
Primary analyses
Cigarette use as outcome: Our first model included daily cigarette use as the DV, and predictors included covariates and IVs (RFQ, BCS, and QM). At Level 1, the model accounted for 12% of the variance. Education status (β=0.20, p=0.01) and cannabis use (β=0.19, p=0.01) were significant predictors. At Level 2, the model accounted for 17% of the variance, with two significant two-way interactions emerging.
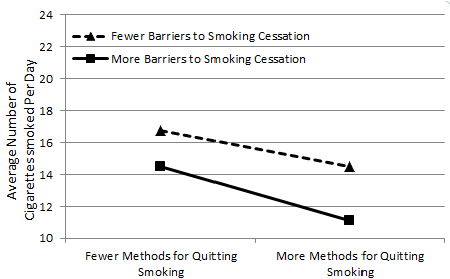
The first two-way interaction was between quit methods and BCS (β=0.65, p=0.01). BCS moderated the relationship between quit methods and number of cigarettes smoked per day. Quit methods were negatively associated with cigarette use, and this negative relationship was stronger among those with more BCS relative to those with fewer BCS (Figure 1). The second two-way interaction was between RFQ (composite score) and quit methods (β=1.10, p=0.03). RFQ moderated the relationship between quit methods and daily cigarette use such that quit methods were negatively linked with smoking, but only among those with fewer RFQ. The opposite emerged among those with more RFQ such that, for these individuals, the quit methods was positively associated with smoking.
The model at Level 3 accounted for 23% of the variance, with a significant three-way interaction between quit methods, BCS, and RFQ (β=4.52, p=0.0002; Table 1). Among individuals with fewer RFQ, quit methods was negatively associated with smoking, and this relationship was strongest among those with more BCS. However, among individuals with more RFQ, quit methods was positively associated with smoking, particularly among those with more BCS (Figure 2).
Alcohol use frequency as outcome: Our second model was similar to the first except that drinking frequency was the DV. The model accounted for 5% of the variance at Level 1, with gender (β=0.18, p=0.01), RFQ (β=0.17, p=0.02), and BCS (β=0.17, p=0.02) as significant predictors. At Level 2, the model accounted for 5% of the variance. No significant two-way interactions emerged. Level 3 accounted for 8% of the variance, and a significant three-way interaction emerged between quit methods, BCS, and RFQ (β=3.40, p=0.01; Table 1). This threeway interaction showed that among individuals with fewer RFQ, quit methods was negatively associated with drinking frequency, and this relationship was strongest among those with more BCS. However, among those low in both BCS and RFQ, quit methods was positively associated with drinking frequency.
Discussion
The present study examines behavioral and cognitively-based quit processes among daily smokers who drink heavily, and sought to determine whether these processes differentially influence cigarette and alcohol use.
Hypothesis 1: Main effects
Our first hypothesis was partially supported. Quit methods was not significantly associated with substance use, and this is contrary to what was expected (H1a). Further, BCS was associated with increased drinking, which was also unexpected (H1b). Previous work has not shown significant associations between smoking-related BCS and alcohol outcomes [20,21], and thus we had not predicted that this relationship would emerge. This finding may support the perspective that among co-occurring substance users, barriers to quitting one substance (cigarettes) may pose difficulties to quitting a different substance (alcohol). The relationship between RFQ and substance use (H1c) was somewhat complex. RFQ predicted marginal reductions in the number of cigarettes smoked per day, whereas RFQ was associated with increases in drinking frequency. This may imply a parallel recognition of the need to change problematic behavior and may provide support for the notion that individuals who use substances at higher levels may also have more RFQ due to salience of health problems. An alternative explanation for the positive association between RFQ and drinking is that perhaps having many reasons for smoking cessation might increase cognitive load or stress linked with quitting, and individuals may attempt to fill the cigarette “void” by turning to another substance (alcohol). The latter explanation is somewhat troublesome, as it may provide evidence for the perspective that among co-users, quitting one substance may heighten the risk of using the other substance at increased levels. Generally, these findings imply that cognitive-based smoking processes are relevant to concurrent substance using individuals and this warrants further investigation.
Hypothesis 2: Two-way interactions
Results supported our second hypothesis. BCS moderated the relationship between quit methods and cigarette use (Figure 1; H2a). Higher numbers of quit methods (endorsing more items) was negatively linked with the number of cigarettes smoked per day, and this relationship was stronger among those with more versus few BCS. Interestingly, the negative relationship between quit methods and smoking emerged more strongly among those with more BCS relative to fewer BCS. One possible explanation for these findings is that individuals with many barriers might have found ways to overcome them via multiple and varied attempts to quit smoking (e.g., nicotine patch or gum, or quitting with friends or relatives). These individuals might represent “hardier” quitters; those who, despite being buffeted by many barriers, have found ways to reduce their cigarette use. It is worth noting that those with fewer BCS smoked more relative to those with more BCS. Although having more quit methods was linked with decreased smoking overall, it appears that those with fewer BCS might benefit less from varying quit approaches relative to those with more BCS. It could be that these individuals may struggle with ambivalence about their smoking. For example, having fewer BCS is consistent with desire to quit, however, continuing to smoke is consistent with the simultaneous desire not to quit, and this tugging of opposite forces is a hallmark of ambivalence [46,47].
Results also supported our expectation that RFQ would moderate the relationship between quit methods and substance use (Figure 3; H2b). Quit methods were linked with reductions in cigarettes per day. However, this relationship was only evident among those with fewer RFQ. Interestingly, the opposite emerged among those with more RFQ; that is, among individuals with many RFQ, quit methods were linked with increased cigarette use. It seems intuitive to suggest that engaging in a variety of quit methods and having many RFQ is consistent with goals aligned with eventual cessation; however, the data did not support this assertion. It is possible that the discouragement of repeatedly and unsuccessfully trying to quit may lead to the uncomfortable experience of dissonance (awareness that one is continuing to smoke while trying to quit). A large body of literature has explored the theory of cognitive dissonance [48] which suggests that dissonance can be reduced by either modifying behavior (e.g., quit smoking) or modifying cognition (e.g., minimizing risk associated with smoking) [48]. Studies have demonstrated links between dissonance and perceptions of selfexemption from health risks [49]. Further, smokers tend to down-play cigarette-related risk [50,51]. In other words, despite having many RFQ, smokers who have attempted various methods to quit may hold inaccurate assumptions that they are not personally susceptible to health problems. Additional work is needed to better understand relationships among RFQ, quit methods, and cigarette use, particularly to explore characteristics that may increase risk for heavy smoking.
It is interesting to note that although the interaction between quit methods and RFQ emerged when predicting cigarette use, it did not emerge when predicting drinking frequency. This may lend support to the perspective that behavioral and cognitive quit processes differentially affect tobacco and alcohol outcomes among co-users. Perhaps processes that buffer against cigarette use for some individuals (e.g., smokers who do not drink) do not have protective effects against cigarette use for others (e.g., smokers who drink). These findings indicate that behavioral and cognitive processes may not have a straightforward relationship with concurrent substance use, and additional examination of characteristics that might predispose cousers to benefit most from specific quit strategies are needed.
Hypothesis 3: Three-way interactions
We found evidence to support our third hypothesis. Two threeway interactions emerged between RFQ, BCS, and quit methods in predicting substance use. The first three-way interaction (Figure 2) predicted the number of cigarettes smoked per day. Among individuals with fewer RFQ, quit methods were associated with reductions in smoking regardless of how many BCS were reported. However, among those with more RFQ, quit methods were linked with reductions in smoking, but only among individuals with fewer BCS. The opposite emerged among those with more BCS such that quit methods were linked with increased cigarette use.
The second three-way interaction (Figure 4) predicted drinking frequency, and results showed that among those with fewer RFQ, quit methods were associated with reductions in drinking for individuals with many BCS. However, the opposite was true among those with fewer BCS such that quit methods were linked with increased drinking frequency. Further, among those with more RFQ, only marginal changes in drinking frequency emerged, regardless of number of quit methods or BCS.
Taken together, the present data demonstrated that with some exceptions, cigarette and alcohol use dropped among individuals with higher levels of these behavioral and cognitive quit processes. Thus, these findings support previous work exploring benefits of concurrently treating co-occurring substance use [11,14]. However, it is also important to note that the present findings also suggest that there may be a subset of individuals for whom these otherwise protective processes might be associated with increases in substance use. In other words, there may be co-users for whom a reduction in one substance could lead to an increase in the other. One potential reason for this might relate to difficulties coping with withdrawal symptoms from attempts to reduce co-occurring substance use. This perspective has been previously been suggested [11] and warrants additional research. Another potential reason for these findings might stem from the rewarding effects [52,53] and attentional bias towards drug-related reward cues [54]. Further work is needed to understand whether the sub-set of co-users for whom reducing the use of one substance leads to increasing another may benefit from tailored attentional retraining interventions [55,56].
In conclusion, findings from the present study supported our hypotheses that behavioral and cognitive quit processes would evince differential effects on tobacco and alcohol. However, results imply that behavioral and cognitively-based quit processes have a complex relationship with concurrent tobacco and alcohol use, and this needs further elucidation. These examinations have practical utility and may inform development and implementation of interventions and programs targeting comorbid alcohol and tobacco dependence.
Limitations and Future Directions
The strengths of the study must be considered in light of its limitations. First, the present sample is relatively homogenous (e.g., primarily Caucasian) in that it is comprised largely of a group of adult smokers who volunteered to participate in smoking cessation treatment. A large percentage of cigarette smokers attempt to quit on their own [57], and thus, it will be important for researchers to draw from populations other than those included in the present study to address potential self-selection bias among individuals with these characteristics and to increase the generalizability of findings. Further, although nicotine replacement therapy with respect to the use of patches was captured by the variable indicating quit methods; other forms of nicotine replacement therapy (e.g., lozenges, gum) were not. Replications of this work are needed to address whether various forms of nicotine replacement therapy impact outcomes. Second, the present study was cross-sectional and items were assessed via selfreport. Thus, findings cannot shed light on processes over time or isolate causal relations between variables, and the measures are subject to potential biases. Additionally, the study sample did not exclude participants based on drinking criteria, and thus, the sample included light, moderate, and heavy drinkers. Moreover, the data collected were part of a larger trial, and thus, the decision on which participants were included in the present analysis was based on the availability of the necessary data. Third, it is worth noting that the FTND exhibited low internal consistency, which is an issue that can emerge with this scale [58].
Author Disclosure
Role of funding sources
This project was supported by National Institute of Mental Health grant R01 MH076629-01 (Drs. Zvolensky and Schmidt). Additionally, preparation of this manuscript was supported in part by National Institute on Drug Abuse grant K12-DA-000167 (Dr. Foster). NIMH and NIDA had no direct role in the study design, collection, analysis or interpretation of the data, writing the manuscript, or the decision to submit the paper for publication. The contents of this manuscript do not necessarily represent the policy of the NIMH or NIDA, and as such, endorsement by the Federal Government should not be assumed.
Human subjects
This study was approved by the instituational review board at the University of Vermont and Florida State University.
Contributors
Dawn Foster conducted literature searches and statistical analysis, and drafted the manuscript. Michael Zvolensky and Norman Schmidt conceptualized theoretical bases of the grant, oversaw data collection, and provided guidance and feedback to manuscript drafts. All authors contributed to and have approved the final manuscript.
References
- Palfai TP, Monti PM, Ostafin B, Hutchison K (2000) Effects of nicotine deprivation on alcohol-related information processing and drinking behavior. J Abnorm Psychol 109: 96-105.
- Harrison EL, Hinson RE, McKee SA (2009) Experimenting and daily smokers: episodic patterns of alcohol and cigarette use. Addict Behav 34: 484-486.
- Howell A, Leyro T, Hogan J, Buckner J, Zvolensky M (2010) Anxiety sensitivity, distress tolerance, and discomfort intolerance in relation to coping and conformity motives for alcohol use and alcohol use problems among young adult drinkers. Addictive Behaviors 35:1144-1147.
- Krukowski RA, Solomon LJ, Naud S (2005) Triggers of heavier and lighter cigarette smoking in college students. J Behav Med 28: 335-345.
- Reed MB, Wang R, Shillington AM, Clapp JD, Lange JE (2007) The relationship between alcohol use and cigarette smoking in a sample of undergraduate college students. Addictive Behaviors 32: 449-464.
- Hughes JR, Kalman D (2006) Do smokers with alcohol problems has more difficulty quitting? Drug Alcohol Depend 82: 91-102.
- Hurt RD, Offord KP, Croghan IT, Gomez-Dahl L, Kottke TE, et al. (1996) Mortality following inpatient addictions treatment: Role of tobacco use in a community-based cohort. JAMA: Journal of the American Medical Association 275: 1097-1103.
- Lisha NE, Carmody TP2, Humfleet GL2, Delucchi KL2 (2014) Reciprocal effects of alcohol and nicotine in smoking cessation treatment studies. Addict Behav 39: 637-643.
- Taylor B, Rehm J (2006) When risk factors combine: The interaction between alcohol and smoking for aerodigestive cancer, coronary heart disease, and traffic and fire injury. Addictive Behaviors 31: 1522-1535.
- Jarvis CM, Hayman LL, Braun LT, Schwertz DW, Ferrans CE, et al. (2007) Cardiovascular risk factors and metabolic syndrome in alcohol- and nicotine-dependent men and women. J CardiovascNurs 22: 429-435.
- Joseph AM, Willenbring ML, Nugent SM, Nelson DB (2004) A randomized trial of concurrent versus delayed smoking intervention for patients in alcohol dependence treatment. Journal of Studies on Alcohol, 65: 681-691.
- Kodl M, Fu SS, Joseph AM (2006) Tobacco cessation treatment for alcohol-dependent smokers: when is the best time? Alcohol Res Health 29: 203-207.
- Fu S, Kodl M, Willenbring M, Nelson D, Nugent S, et al. (2008) Ethnic differences in alcohol treatment outcomes and the effect of concurrent smoking cessation treatment. Drug and Alcohol Dependence 92: 61-68.
- Holt LJ, Litt MD, Cooney NL (2012) Prospective analysis of early lapse to drinking and smoking among individuals in concurrent alcohol and tobacco treatment. Psychology of Addictive Behaviors 26:561-572.
- Centers for Disease Control and Prevention (CDC) (2009) Cigarette smoking among adults and trends in smoking cessation - United States, 2008. MMWR Morb Mortal Wkly Rep 58: 1227-1232.
- Irving LM, Seidner AL, Burling TA, Thomas RG, Brenner GF (1994) Drug and alcohol abuse inpatients' attitudes about smoking cessation. J Subst Abuse 6: 267-278.
- Macnee CL, Talsma A (1995) Development and testing of the barriers to cessation scale. Nurs Res 44: 214-219.
- Orleans CT, Rimer BK, Cristinzio S, Keintz MK, Fleisher L (1991) A national survey of older smokers: treatment needs of a growing population. Health Psychol 10: 343-351.
- Kristeller JL (1994) Treatment of hard-core, high-risk smokers using FDA approved pharmaceutical agents: An oral health team perspective. Health Values 18: 25-32.
- Asher MK, Martin RA, Rohsenow DJ, MacKinnon S, Traficante R, et al. (2003) Perceived barriers to quitting smoking among alcohol dependent patients in treatment. Journal of Substance Abuse Treatment 24: 169-174.
- Martin RA, Rohsenow DJ, MacKinnon SV, Abrams DB, Monti PM (2006) Correlates of motivation to quit smoking among alcohol dependent patients in residential treatment. Drug Alcohol Depend 83: 73-78.
- Marlatt GA, Gordon JR (1985) Relapse prevention. New York: Guilford Press.
- Velicer WF, DiClemente CC, Prochaska JO, Brandenburg N (1985) Decisional balance measure for assessing and predicting smoking status. J PersSoc Psychol 48: 1279-1289.
- DiClemente CC, Prochaska JO (1982) Self-change and therapy change of smoking behavior: a comparison of processes of change in cessation and maintenance. Addict Behav 7: 133-142.
- Curry SJ, Grothaus L, McBride C (1997) Reasons for quitting: intrinsic and extrinsic motivation for smoking cessation in a population-based sample of smokers. Addict Behav 22: 727-739.
- Baha M, Le Faou AL (2010) Smokers' reasons for quitting in an anti-smoking social context. Public Health 124: 225-231.
- Curry SJ, McBride C, Grothaus LC, Louie D, Wagner EH (1995) A randomized trial of self-help materials, personalized feedback, and telephone counseling with nonvolunteer smokers. J Consult Clin Psychol 63: 1005-1014.
- Saunders JB, Aasland OG, Babor TF, de la Fuente JR, Grant M (1993) Development of the Alcohol Use Disorders Identification Test (AUDIT): WHO Collaborative Project on Early Detection of Persons with Harmful Alcohol Consumption--II. Addiction 88: 791-804.
- First MB, Williams JB, Spitzer RL, Gibbon M (2002) Structured Clinical Interview for DSM-IV-TR Axis I Disorders, Clinical Trials Version (SCID-CT). New York: Biometrics Research, New York State Psychiatric Institute.
- Brown RA, Lejuez CW, Kahler CW, Strong DR (2002) Distress tolerance and duration of past smoking cessation attempts. J Abnorm Psychol 111: 180-185.
- Heatherton TF, Kozlowski LT, Frecker RC, Fagerström KO (1991) The Fagerström Test for Nicotine Dependence: a revision of the Fagerström Tolerance Questionnaire. Br J Addict 86: 1119-1127.
- Pomerleau CS, Carton SM, Lutzke ML, Flessland KA, Pomerleau OF (1994) Reliability of the Fagerstrom Tolerance Questionnaire and the Fagerstrom Test for Nicotine Dependence. Addict Behav 19: 33-39.
- Fagerstrom KO, Heatherton TF, Kozlowski LT (1990) Nicotine addiction and its assessment. Ear Nose Throat J 69: 763-765.
- Filbey FM, Claus E, Audette AR, Niculescu M, Banich MT, et al. (2007) Exposure to the taste of alcohol elicits activation of the mesocorticolimbicneurocircuitry. Neuropsychopharmacology 33: 1391-1401.
- Fleming MF, Barry KL, MacDonald R (1991) The alcohol use disorders identification test (AUDIT) in a college sample. Int J Addict 26: 1173-1185.
- Cherpitel CJ (1995) Analysis of cut points for screening instruments for alcohol problems in the emergency room. J Stud Alcohol 56: 695-700.
- Macnee CL, Talsma A (1995) Predictors of progress in smoking cessation. Public Health Nurs 12: 242-248.
- Curry S, Wagner EH, Grothaus LC (1990) Intrinsic and extrinsic motivation for smoking cessation. J Consult Clin Psychol 58: 310-316.
- McBride CM, Pollak KI, Bepler G, Lyna P, Lipkus IM, et al. (2001) Reasons for quitting smoking among low-income African American smokers. Health Psychol 20: 334-340.
- Bonn-Miller MO, Zvolensky MJ (2009) An evaluation of the nature of marijuana use and its motives among young adult active users. Am J Addict 18: 409-416.
- Buckner JD, Zvolensky MJ, Schmidt NB (2012) Cannabis-related impairment and social anxiety: the roles of gender and cannabis use motives. Addict Behav 37: 1294-1297.
- Agrawal A, Budney AJ, Lynskey MT (2012) The co-occurring use and misuse of cannabis and tobacco: a review. Addiction 107: 1221-1233.
- Degenhardt L, Hall W, Lynskey M (2001) The relationship between cannabis use and other substance use in the general population. Drug Alcohol Depend 64: 319-327.
- Cohen J, Cohen P (1983) Applied multiple regression/correlation analysis for the behavioral sciences. Hillsdale, NJ: Lawrence Erlbaum.
- Cohen J, Cohen P, West SG, Aiken LS (2003) Applied multiple regression/correlation analysis for the behavioral sciences (3rd ed.). Mahwah, NJ US: Lawrence Erlbaum Associates Publishers.
- Lipkus IM, Feaganes JR, Green JD, Sedikides C (2001) The Relationship Between Attitudinal Ambivalence and Desire to Quit Smoking Among College Smokers. Journal of Applied Social Psychology, 31: 113-133.
- Wilson SJ, Creswell KG, Sayette MA, Fiez JA (2013) Ambivalence about smoking and cue-elicited neural activity in quitting-motivated smokers faced with an opportunity to smoke. Addict Behav 38: 1541-1549.
- Festinger LA (1957) A theory of cognitive dissonance. Evanston, IL: Row, Peterson.
- Markowitz LJ (2000) Smoker's perceived self-exemption from health risks. Psi Chi Journal of Undergraduate Research 5: 119-124.
- Jamieson P, Romer D (2001)What do young people think they know about the risks of smoking? In P. Slovic (Ed.), Smoking: Risk, perception, and policy (pp. 51-63). Thousand Oaks, CA US: Sage Publications, Inc.
- Schane RE, Glantz SA, Ling PM (2009) Social smoking implications for public health, clinical practice, and intervention research. American Journal of Preventive Medicine 37: 124-131.
- DaniJA, De Biasi M (2001) Cellular mechanisms of nicotine addiction. PharmacolBiochemBehav 70: 439-446.
- Nestler EJ (2005) Is there a common molecular pathway for addiction? Nat Neurosci 8: 1445-1449.
- Ehrman RN, Robbins SJ, Bromwell MA, Lankford ME, Monterosso JR, et al. (2002) Comparing attentional bias to smoking cues in current smokers, former smokers, and non-smokers using a dot-probe task. Drug Alcohol Depend 67: 185-191.
- Kerst WF, Waters AJ (2014)Attentional retraining administered in the field reduces smokers’ attentional bias and craving.
- Wiers RW, Rinck M, Kordts R, Houben K, Strack F (2010) Retraining automatic action-tendencies to approach alcohol in hazardous drinkers. Addiction 105: 279-287.
- Raupach T, West R, Brown J (2013) The most "successful" method for failing to quit smoking is unassisted cessation. Nicotine Tob Res 15: 748-749.
- Korte KJ, Capron DW, Zvolensky M, Schmidt NB (2013) The Fagerström test for nicotine dependence: do revisions in the item scoring enhance the psychometric properties? Addict Behav 38: 1757-1763.
Relevant Topics
- Addiction Recovery
- Alcohol Addiction Treatment
- Alcohol Rehabilitation
- Amphetamine Addiction
- Amphetamine-Related Disorders
- Cocaine Addiction
- Cocaine-Related Disorders
- Computer Addiction Research
- Drug Addiction Treatment
- Drug Rehabilitation
- Facts About Alcoholism
- Food Addiction Research
- Heroin Addiction Treatment
- Holistic Addiction Treatment
- Hospital-Addiction Syndrome
- Morphine Addiction
- Munchausen Syndrome
- Neonatal Abstinence Syndrome
- Nutritional Suitability
- Opioid-Related Disorders
- Relapse prevention
- Substance-Related Disorders
Recommended Journals
Article Tools
Article Usage
- Total views: 58470
- [From(publication date):
December-2015 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 57583
- PDF downloads : 887