Case Report Open Access
Intensive Management of Chronic Bronchorrhea in a Tracheostomized Duchenne Patient with Bronchiectasis
| Michel Toussaint* and Philippe Soudon | |
| Rehabilitation Hospital Inkendaal, Inkendaalstraat 1, B-1602 Vlezenbeek (Brussels), Belgium | |
| Corresponding Author : | Michel Toussaint Rehabilitation Hospital Inkendaal Inkendaalstraat 1, B-1602 Vlezenbeek (Brussels), Belgium Tel: +32 2 531 51 11 Fax: +32 2 531 53 01 E-mail: michel.toussaint@inkendaal.be |
| Received March 12, 2012; Accepted March 31, 2012; Published April 03, 2012 | |
| Citation: Toussaint M, Soudon P (2012) Intensive Management of Chronic Bronchorrhea in a Tracheostomized Duchenne Patient with Bronchiectasis. J Nov Physiother 2:110. doi: 10.4172/2165-7025.1000110 | |
| Copyright: © 2012 Toussaint M, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. | |
Visit for more related articles at Journal of Novel Physiotherapies
Abstract
Duchenne muscular dystrophy (DMD) is a severe X-linked hereditary neuromuscular disease characterized by progressive muscle degeneration and functional tetraplegia. Advances related to the use of mechanical ventilation and techniques of airway clearance have improved the lifespan of these patients until 30-35 years. In a 27 years old home-ventilated tracheostomized DMD patient affected by bronchiectasis and atelectasis with excessive bronchorrhea (>300ml mucus production/24h), endotracheal suctioning act became so frequent that it severely affected his mental health and that of his family. An intensive programme of airway clearance including ventilation via Intrapulmonary Percussive Ventilation (IPV) and suctioning via mechanical insufflation-exsufflation (MI-E) associated with strong manual chest compression improved mean nocturnal SpO2 from 91 to 95% and reduced mucus production and suctioning rate by 50%. The perceived physical and emotional health (SF-36) increased in the patient and in his family. In the patient, the general mental health score increased from 16 to 48%, the vitality from 10 to 40% and the general health perception from 10 to 35%. In the patient’s father, the social functioning improved from 38 to 63%, the general mental health from 36 to 60% and the vitality from 35 to 60%. In this report, intensive respiratory therapy with IPV in combination with MI-E and chest compression was safe and spectacularly improved the quality of ventilation, the mucus production and the perceived mental health in an adult Duchenne patient with bronchorrhea.
| Keywords |
| Chest physiotherapy; Cough-assist; Duchenne; Mechanical insufflation-exsufflation; Tracheostomy; Ventilation |
| Introduction |
| Progressive muscular weakness characterizes Duchenne muscular Dystrophy (DMD). In the second decade of life, lung function decreases to such an extent that spontaneous ventilation needs to be assisted [1]. Nocturnal nasal intermittent positive pressure ventilation (NIPPV) is effective in providing 24 h normocapnia during several years but needs to be extended with disease progression when diurnal dyspnoea is present [2]. Non-invasive interfaces may be used for continuous assisted ventilation [3]. Some DMD patients however may require tracheostomy when bulbar function is severely altered. Other patients may undergo tracheostomy in the emergency room after acute respiratory insufficiency. Long-term intermittent positive pressure ventilation via tracheostomy is reported with good acceptance in 2/3 of the DMD patients [4]. In spite of advantages (i.e. safety and possibility of endotracheal suction), tracheostomy also puts patients in danger of side effects such as excessive mucus production, tracheal stenosis, tracheobronchomalacia, bleeding, chronic bronchitis and bronchiectasis [5,6]. In the present case, a dramatic mucus hyperproduction aggravated by a severely impaired secretion clearance was treated in a 27 yrs old tracheostomized Duchenne patient affected by bronchiectasis, a permanent dilatation of the bronchi with destruction of the elastic and muscular component of the bronchial walls. In the current case, bronchiectasis was probably related to prolonged use of invasive ventilation and recurrent aspirations [7]. In addition, impaired clearance of secretions caused chronic respiratory infection resulting in a vicious cycle of bronchial damage, bronchial dilation, impaired clearance of secretions, recurrent infection, and more bronchial damage. The quality of life of this patient and that of his family had been destroyed with the challenging management of this bronchorrhea. |
| Case Summary |
| We report here the original experience of aggressive respiratory therapy in a 27 year old patient with Duchenne muscular dystrophy presenting bronchiectasis with chronic bronchorrhea. In this patient, NIPPV was initiated at 15.5 years. Lung function tests at this time were as follows (value (% of predicted value)): vital capacity (VC) was 1330 ml (25%), maximal inspiratory pressure (MIP) was 39 cm H2O (29%) and the peak expiratory flow (PEF) was 136 L/min (19%). NIPPV allowed 24 h normocapnia for five years. During an acute chest infection, tracheostomy was placed in the emergency room to provide permanent ventilation and to offer the possibility for airway clearance by endotracheal suctioning. As a consequence of the tracheostomy the patient had recurrent chest infections and was regularly hospitalized. Hypersecretion, aspiration and prolonged use of intermittent positive pressure ventilation via tracheostomy involved in severe bronchiectasis and bronchorrhea. Bronchiectasis was diagnosed via a computed tomography (CT) scan. This examination showed bronchial wall thickening and luminal dilatation and a complete atelectasis of the right lower lobe with a discrete air bronchogram. A right upper lobe and, to a lesser extent, a right lower lobe bronchiectasis were found with alveolar infiltrates of infectious origin. |
| The patient was primary treated at home by non instrumental chest physiotherapy and two weeks turning antibiotherapy (Amoxycillin + Clavulanic acid; Clarithromycin; Trimethoprim + Sulmamethoxazol). The patient lost 13 kg (from 42 to 29 kg) within 7 years after tracheostomy and SpO2<88% was found within 14% of the time with ventilation. At the age of 27, the family addressed to our Centre a rescue appeal for helping them in the management of the bronchorrhea. At this moment, no ventilator free time was available, VC was 80 ml (1.5%), MIP was 4 cm H2O (3.7%) and PEF was 15 L/ min (2.7%). The impact of permanent hypersecretion and recurrent suctions every hour largely interfered with the social activities of the parents. Mucus production was abnormally elevated, reaching more than 300 ml per 24 h. This largely surpassed the most severe cases we had previously met. We proposed an hospitalisation including a respiratory therapy program to manage this problem, accepted by the patient and his family. |
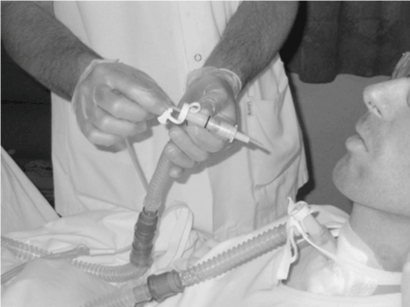
| We started intensive chest physiotherapy during a 5 days program. The program included 9 hours of night-time high frequency percussive ventilation (VDR4®, Percussionaire, Sandpoint, USA). The parameters were as follows: high frequency signal: peak inspiratory pressure = 50 cm H2O (37 torr); peak expiratory pressure = 15 cm H2O (11 torr); rate = 550 min-1; low frequency signal: plateau inspiratory pressure = 50 cm H2O (37 torr); convective peak pressure = 78 cm H2O (57 torr); oscillatory CPAP = 8 cm H2O (6 torr); rate = 21.8 min-1. We started night-time high frequency percussive ventilation after a 2 hour monitoring of transcutaneous CO2 tension (TcCO2) to check that VDR4 did not cause hyperventilation. During the day, airway clearance was achieved by 4 sessions/day, 1 hour each, divided in subsessions of 10 minutes separated by 5 minutes rest. Airway clearance was obtained by the combination of 3 techniques, two non-invasive and one invasive at the same time. Mechanical insufflation-exsufflation (MI-E) display (Cough-Assist®, Emerson, Cambridge, USA) was directly connected on the canula of tracheostomy at an intermittent negative pressure of – 40 cm H2O (-29 torr), with inspiratory and expiratory times of 2 seconds. In addition, invasive suction was achieved by a catheter placed into the canula through the ventilation tubing adapted with a suction hall in front of the canula (Figure 1). Initially controlled by endoscopy, the suction catheter was placed 4 cm above the carina avoiding any mechanical traumatism. Invasive suction by catheter was carried out only to avoid mucus invasion in MI-E tubing. This precaution meant that the therapist did not waste time cleaning out secretions in the tubing. Expiratory manual thoracic compression was achieved during the 10 minute sub-session by two strong hand compressions on the right and on the left ribs (Figure 2). Mucus collection surpassed 300 ml/day during the trial. |
| After 5 days hospitalisation, the patient was discharged home with a Cough-Assist® and was asked to prolong therapy. Intrapulmonary percussive ventilation (IPV) was recommended during the day via a portable device for home use (Impulsator®, Percussionaire, Sandpoint, USA) for 3 periods of 15 minutes. |
| After one month therapy at home, the amount of secretions diminished to 150 ml/day, and mean nocturnal SpO2 improved from 91% to 95% (SpO2 mini from 82 to 94%). Measured at the time of the trial and 4 weeks later, the quality of perceived physical and emotional health was assessed by the short-form health survey questionnaire (SF- 36) for the patient and for his father who mostly looks after him. In the patient, the general mental health score increased from 16 to 48%, the vitality from 10 to 40% and the general health perception from 10 to 35%. In the patient’s father, the social functioning improved from 38 to 63%, the general mental health from 36 to 60% and the vitality from 35 to 60%. The father found that the outcome of the situation had improve very satisfactorily. |
| Discussion |
| We report here an original, safe and effective way of MI-E use in a weak, hypersecretive and tracheostomized ventilated Duchenne patient. The goal of the present trial was to improve the delay between two successive suctions. The need for suction interfered so much with the father’s social activities that he reported having actually no more social life out of the house, as evidenced by his low social functioning score before treatment. |
| Excessive mucus production is reported in neuromuscular patients receiving long-term ventilation with uncuffed tracheostomies [5]. Hypersecretion is considered as a common side effect of the tracheostomy [6] and is generally defined as a mucus production above 30 ml per day. The present case had a singular massive mucus production. In the literature, no case of such a massive hypersecretion was previously reported as surpassing 300 ml/day in neuromuscular disorders. We hypothesized that atelectasis and bronchiectasis, confirmed by CT scan, had probably structured and fed a vicious circle of mucus hypersecretion and stagnation. We logically aimed at breaking this vicious circle by (1) improving the quality of ventilation and (2) achieving intensive and effective mucus clearance. Techniques of intrapulmonary percussive ventilation (IPV) [8], mechanical insufflation-exsufflation (MI-E) [9] or chest compression [10] are reported to help in secretion clearance in neuromuscular disorders. MI-E without chest or abdominal compression was already described in invasive ventilation and MI-E seemed more effective in clearing out secretions than conventional tracheal suction [11]. The three techniques (IPV, MI-E, chest compression), however, were not previously associated. |
| As a result of the present trial, the quality of ventilation improved as assessed by SpO2 improvement. Mucus production diminished by 50%. The general mental health improved both in the patient and in his father. According with a previous report [12], the delay between 2 suctions rose from 1-2 hours to 5-9 hours which was deemed very satisfactory by the patient and his family. After initiation of the therapy, the father told that he could now spend complete nights without suctioning secretions for the first time in 7 years. |
| When airway clearance techniques are mixed, it is difficult to assess which part of the efficiency can be attributed to each technique. In the present case, we assume that the combination of MI-E and the thoracic compression both brought a significant part of the efficiency in clearing out secretions. In patients receiving mechanical ventilation, mechanical rib-cage compression during the expiratory phase is reported effective in airway-secretion removal [10]. Clearly, the efficiency of strong thoracic compression was here visually observed in real time by an immediate higher mucus collection. Moreover, mixing MI-E and chest compression was very well tolerated by the patient who felt it very soft. To our surprise, MI-E was useful in ventilating the patient during the respiratory care sessions. |
| In this report, intensive respiratory therapy achieved by noninvasive suctioning was safe, improved the quality of ventilation and reduced mucus production in a Duchenne patient with bronchorrhea. Moreover, suction frequency substantially diminished. This treatment improved the quality of life of the patient and that of his family. |
References
- Finder JD, Birnkrant D, Carl J, Farber HJ, Gozal D, et al. (2004) Respiratory care of the patient with Duchenne muscular dystrophy: ATS consensus statement. Am J Respir Crit Care Med 170: 456-465.
- Toussaint M, Soudon P, Kinnear W (2008) Effect of non-invasive ventilation on respiratory muscle loading and endurance in patients with Duchenne muscular dystrophy. Thorax 63: 430-434.
- Toussaint M, Steens M, Wasteels G, Soudon P (2006) Diurnal ventilation via mouthpiece: survival in end-stage Duchenne patients. Eur Respir J 28: 549-555.
- Narayanaswami P, Bertorini TE, Pourmand R, Horner LH (2000) Long-term tracheostomy ventilation in neuromuscular diseases: patient acceptance and quality of life. Neurorehabil Neural Repair 14: 135-139.
- Baydur A, Kanel G (2003) Tracheobronchomalacia and tracheal hemorrhage in patients with Duchenne muscular dystrophy receiving long-term ventilation with uncuffed tracheostomies. Chest 123: 1307-1311.
- Soudon P, Steens M, Toussaint M (2008) A comparison of invasive versus noninvasive full-time mechanical ventilation in Duchenne muscular dystrophy. Chron Respir Dis 5: 87-93.
- Treggiani MM, Romand JA, Martin JB, Suter PM (2002) Air cysts and bronchiectasis prevail in nondependent areas in severe acute respiratory distress syndrome: a computed tomographic study of ventilator-associated changes. Crit Care Med 30: 1747-1752.
- Toussaint M, De Win H, Steens M, Soudon P (2003) Effect of intrapulmonary percussive ventilation on mucus clearance in duchenne muscular dystrophy patients: a preliminary report. Respir Care 48: 940-947.
- Chatwin M, Ross E, Hart N, Nickol AH, Polkey MI, et al. (2003) Cough augmentation with mechanical insufflation/exsufflation in patients with neuromuscular weakness. Eur Respir J 21: 502-508.
- Unoki T, Kawasaki Y, Mizutani T, Fujino Y, Yanagisawa Y, et al. (2005) Effects of expiratory rib-cage compression on oxygenation, ventilation, and airway-secretion removal in patients receiving mechanical ventilation. Respir Care 50: 1430-1437.
- Sancho J, Servera E, Vergara P, Marín J (2003) Mechanical insufflation-exsufflation vs. tracheal suctioning via tracheostomy tubes for patients with amyotrophic lateral sclerosis: a pilot study. Am J Phys Med Rehabil 82: 750-753.
- Fine CK, Driscoll S, Stafierri F (1999) Comparison of utilization of respiratory technology: Cough-Alator vs. suctioning. J Spinal Cord Med 22: 31.
Figures at a glance
 |
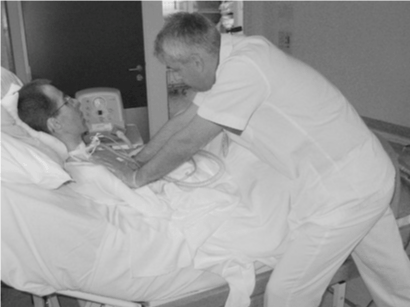 |
| Figure 1 | Figure 2 |
Relevant Topics
- Electrical stimulation
- High Intensity Exercise
- Muscle Movements
- Musculoskeletal Physical Therapy
- Musculoskeletal Physiotherapy
- Neurophysiotherapy
- Neuroplasticity
- Neuropsychiatric drugs
- Physical Activity
- Physical Fitness
- Physical Medicine
- Physical Therapy
- Precision Rehabilitation
- Scapular Mobilization
- Sleep Disorders
- Sports and Physical Activity
- Sports Physical Therapy
Recommended Journals
Article Tools
Article Usage
- Total views: 14466
- [From(publication date):
May-2012 - Aug 29, 2025] - Breakdown by view type
- HTML page views : 9860
- PDF downloads : 4606
